预约演示
更新于:2025-07-12
Denosumab Biosimilar (Boan Biological)
地舒单抗生物类似药 (山东博安生物)
更新于:2025-07-12
概要
基本信息
原研机构 |
非在研机构- |
最高研发阶段批准上市 |
首次获批日期 中国 (2022-11-08), |
最高研发阶段(中国)批准上市 |
特殊审评- |
登录后查看时间轴
结构/序列
Sequence Code 94568L

当前序列信息引自: *****
Sequence Code 143522H

当前序列信息引自: *****
关联
12
项与 地舒单抗生物类似药 (山东博安生物) 相关的临床试验NCT05853354
A Randomized, Double-blind, Parallel-group, Active-controlled Comparative Study to Evaluate the Efficacy, Safety, Pharmacokinetics, and Immunogenicity of LY06006 Compared With EU-Prolia in Postmenopausal Women With Osteoporosis
this comparative clinical study is designed to demonstrate that LY06006 and EU-Prolia have no clinically meaningful differences in clinical efficacy, pharmacodynamic (PD), safety, PK, and immunogenicity in postmenopausal women with osteoporosis.
开始日期2023-04-05 |
申办/合作机构 |
NCT04859569
A Phase III Study Comparing Efficacy and Safety of LY01011 and Xgeva®(Denosumab) in Patients With Bone Metastases From Solid Tumors
This is a multicenter,randomized, double-blind, active-controlled, parallel-group study comparing efficacy and safety of LY01011 (recombinant anti-RANKL human monoclonal antibody injection) and Xgeva® in patients with bone metastases from solid tumors.
开始日期2021-04-30 |
申办/合作机构 |
NCT06095427
A Randomized, Double Blind, Three-Arm, Parallel Group, Pharmacokinetic Similarity Study in Healthy Male Subjects to Evaluate Pharmacokinetics, Pharmacodynamics, Safety and Immunogenicity of LY06006 Versus US Prolia and EU Prolia by Single-Dose Subcutaneous Injection
This trial is a randomized, double-blind, three-arm, parallel-group, pharmacokinetic study. The purpose of this study is to demonstrate pharmacokinetic (PK) similarity and to compare safety, immunogenicity and pharmacodynamics (PD) between the test product L06006 and the reference products US-Prolia and EU-Prolia in healthy male subjects. A total of 300 healthy male subjects aged 28 to 65 years (both inclusive) will be randomized 1:1:1 to receive a single subcutaneous (s.c.) injection of either LY06006 or US-Prolia or EU-Prolia on Day 1 and then be followed for 36 weeks.
开始日期2021-03-09 |
申办/合作机构  綠葉製藥集團有限公司 綠葉製藥集團有限公司 [+1] |
100 项与 地舒单抗生物类似药 (山东博安生物) 相关的临床结果
登录后查看更多信息
100 项与 地舒单抗生物类似药 (山东博安生物) 相关的转化医学
登录后查看更多信息
100 项与 地舒单抗生物类似药 (山东博安生物) 相关的专利(医药)
登录后查看更多信息
6
项与 地舒单抗生物类似药 (山东博安生物) 相关的文献(医药)2025-04-01·Journal of Bone Oncology
A multicenter, randomized, double-blind trial comparing LY01011, a biosimilar, with denosumab (Xgeva®) in patients with bone metastasis from solid tumors
Article
作者: Lv, Dongqing ; Zhuang, Pengpeng ; Hu, Xichun ; Zheng, Song ; Li, Qingshan ; Yuan, Xia ; Sheng, Lili ; Xu, Hongjie ; Yi, Tienan ; Dai, Xiumei ; Zhao, Mingchuan ; Hu, Changlu ; Zeng, Aiping ; Jiang, Ou ; Yu, Yan ; Wang, Jingfen ; Sun, Hongmei ; Hu, Baihui ; Dou, Changlin ; Shi, Huaqiu ; Chen, Zhendong ; Yang, Weihua ; Su, Zhaoping ; Peng, Peijian ; Bi, Minghong ; Wang, Xicheng ; Ni, Mingli ; Zhou, Ming ; Hou, Zhe ; Lei, Kaijian
Introduction:
Denosumab (Xgeva®) is a standard treatment for the prevention of skeletal-related events (SREs) in patients with bone metastases (BM). This trial was designed to assess the equivalence of LY01011 to denosumab in terms of efficacy and safety.
Materials and methods:
Eligible patients with BM from solid tumors were randomized at a 1:1 ratio to receive 120 mg of LY01011 or 120 mg of denosumab subcutaneously every four weeks during a 12-week double-blind treatment period, and then all enrolled patients continued to receive LY01011 until week 53. The primary endpoint was the natural logarithm of change of the urinary N-terminal crosslinked telopeptide of type I collagen level normalized to the urine creatinine level (uNTX/uCr) at week 13 from baseline. Other endpoints included the uNTX/uCr ratio, serum bone-specific alkaline phosphatase level alteration, status of anti-drug antibodies and neutralizing antibodies, adverse events and SREs.
Results:
850 eligible patients were randomized into the LY01011 group (n = 424) or the denosumab group (n = 426). The least-squares means (SEs) of the natural logarithms of the changes in the uNTX/uCr ratios at week 13 from baseline were -1.810 (0.0404) in the LY01011 group and -1.791 (0.0406) in the denosumab group. The LSM difference [90 % CI] between two arms was -0.019 [-0.110, 0.073] within the equivalence margins (-0.135, 0.135) and met the predetermined primary endpoint. The AEs, ADAs and the PK data showed no statistically significant difference.
Conclusions:
This study demonstrated the equivalent efficacy and safety of LY01011 to denosumab in patients with BM.
2025-03-04·Expert Opinion on Drug Metabolism & Toxicology
A three-arm clinical study to compare pharmacokinetic and pharmacodynamic similarity of the denosumab biosimilar LY06006 with reference denosumab in healthy male subjects
Article
作者: Fuhr, Rainard ; Sun, Xuejiao ; Dou, Changlin ; Tai, Joe ; Zhou, Ming ; Wang, Xi ; Dong, Ying
BACKGROUND:
This study aimed to evaluate the pharmacokinetic (PK), pharmacodynamic (PD) similarity, comparable safety, and immunogenicity between LY06006, European Union-sourced denosumab (EU-DEN), and United States-sourced denosumab (US-DEN).
RESEARCH DESIGN AND METHODS:
In this double-blind, parallel-group, and single-dose study, 300 healthy male subjects were randomized 1:1:1 to receive a 60 mg dose of either LY06006, EU-DEN, or US-DEN subcutaneously. This study lasted for 253 days. Primary PK endpoints included maximum serum concentration (Cmax), area under the concentration-time curve (AUC) from time zero to last quantifiable concentration (AUC0-t), and AUC from time zero to infinity (AUC0-inf). Pharmacokinetic equivalence was concluded if the two-sided 90% confidence interval (CI) for the geometric least squares mean ratio (GLSMR) of primary endpoints were within 80%-125%. Other PK parameters, PD parameters, safety, and immunogenicity assessments were also conducted during the study.
RESULTS:
The 90% CIs for ratios of GLSMR were within the predefined equivalence margin for AUC0-inf (89.0%-111.1%), AUC0-t (89.7%-111.3%), and Cmax (92.3%-106.7%). The PD parameters, safety, and immunogenicity of LY06006 were also comparable to US-DEN and EU-DEN.
CONCLUSION:
LY06006 was highly similar to US-DEN and EU-DEN in terms of PK, PD, safety and immunogenicity in healthy male subjects.
CLINICAL TRIAL REGISTRATION:
www.clinicaltrials.gov identifier is NCT06095427.
2023-10-01·Journal of bone oncology
A randomized trial comparing LY01011, biosimilar candidate, with the reference product denosumab (Xgeva®) in healthy Chinese subjects
Article
作者: Dou, Changlin ; Ding, Yanhua ; Liu, Yusi ; Guo, Shuren
Background:
Complications of bone metastases such as skeletal-related events lead to the impaired functional status and quality of life including death in patients with bone metastasis from solid tumors. Denosumab (XGEVA®) is indicated for the prevention of skeletal-related events in bone metastasis patients with solid tumors. The biosimilar product LY01011, a fully human anti-receptor activator of nuclear factor kappa-B ligand monoclonal antibody, was developed to be compared with the reference product denosumab.
Material and methods:
A randomized, double-blind, single-dose, parallel-controlled phase 1 study was conducted in healthy Chinese subjects. A total of 168 enrolled subjects were randomly assigned in a 1:1 ratio to receive a single 120 mg dose of LY01011 (n = 85) or denosumab (n = 83) subcutaneously. The primary pharmacokinetic (PK) parameters, including maximum plasma concentration (Cmax) and area under the concentration-time curve from time zero to last quantifiable concentration (AUC0→t), were collected and measured for evaluation. Other secondary PK parameters included AUC0- ∞, Tmax, CL/F, λz, t1/2, Vd/F, etc. Pharmacodynamics (PD), safety and immunogenicity profiles were also accounted for data analysis.
Results:
The geometric mean ratios (GMRs) of LY01011 and denosumab for the primary PK parameters such as Cmax and AUC0→t were 98.13% and 100.32%. The 90% confidence intervals (CIs) were all within the acceptance range of 80%-125%. The GMRs of the PD parameters including AUEC0→t and Emax were 98.71% and 99.80%, which fell within the pre-defined acceptance range of 80%-125%. The results also demonstrated PK similarity even if Cmax and AUC0→∞ had been used as primary endpoints. Safety profiles were tolerable and similar between groups. 4 (4.7%) and 2 (2.4%) subjects had experienced Grade 3 or above treatment-emergent adverse events (TEAEs) in LY01011 group and denosumab group. 3 subjects were reported to have serious adverse events (SAEs). None of the Grade 3 or above TEAEs and SAEs were related to the study drug, LY01011. No subject was tested anti-drug antibody (ADA) positive in both groups prior to the study drug administration. Following the study drug administration, only one subject in denosumab group was tested ADA positive, whereas no subject with ADA positive was reported in LY01011 group. No neutralizing antibody (Nab) was detected in either group throughout the study.
Conclusions:
The study demonstrated PK and PD similarity of LY01011, a denosumab biosimilar, to denosumab in healthy Chinese subjects, with comparable safety and immunogenicity profiles.
93
项与 地舒单抗生物类似药 (山东博安生物) 相关的新闻(医药)2025-05-29
·科兴制药
5月28日,公司引进的两款博安生物地舒单抗注射液:60mg规格(商品名:博优倍®)、120mg规格(商品名:博洛加®),正式通过中国澳门药物监督管理局审批,可在澳门地区上市销售。这是科兴制药合作产品中,首次在中国港澳地区获得上市批准的重磅肿瘤药。 全球化再添百亿级市场 今年1月,科兴制药与山东博安生物技术股份有限公司(以下简称:博安生物,股票代码:HK06955)签署关于两款地舒单抗注射液(商品名:博优倍®和博洛加®)在中国香港和中国澳门的独家商业化合作协议。合作的两款地舒单抗注射液:第一款博优倍®,是Prolia®生物类似药,用于骨折高风险的绝经后妇女的骨质疏松症;第二款博洛加®,是Xgeva®生物类似药,用于治疗不可手术切除或者手术切除可能导致严重功能障碍的骨巨细胞瘤,包括成人和骨骼发育成熟(定义为至少1处成熟长骨且体重≥45 kg)的青少年患者。该两款产品由博安生物自主研发,已分别于2022年11月和2024年5月获得中国国家药品监督管理局批准上市,当前已在欧洲、美国、日本开展国际多中心III期临床试验。根据太平洋证券4月份的一份研报显示,地舒单抗是唯一一个具有明确分子靶点的骨改良药物,其安全性和有效性已得到充分验证。原研药于2010年在美国和欧洲地区获批上市,到2023年销售额仍超过60亿美元,依旧保持着增长势头。与此同时,由于老龄化加剧,骨质疏松和肿瘤骨转移患者基数庞大,且诊疗率逐步提升,加之医保的覆盖提高了患者可及性,中国地舒单抗市场也处于高速增长期。弗若斯特沙利文预测,中国市场规模将在2025年达到37.41亿元,2030年或将突破百亿元。中国澳门地区面临着人口老龄化挑战,存在广泛的治疗需求,且人均医疗支出相对较高。据华经产业研究院数据,2023年中国澳门65岁及以上人口占比13.66%。由于中国澳门地区人口老龄化、肿瘤发病率上升,以及患者对高质量医疗服务的需求增加,骨相关疾病治疗存在缺口,慢性病市场规模快速增长,粤港澳大湾区的生物类似药和高端仿制药市场前景可观。 国际化战略助推骨相关疾病治疗赛道布局近年来,科兴制药坚持“全球选品、全球覆盖”的平台型出海模式,重点布局欧盟和人口过亿、经济高速发展的新兴市场国家,以具有性价比的高端生物类似药为切入点,走出一条差异化的出海之路。公司打造的商业化平台,在海外市场注册以“快”著称,例如肿瘤药白蛋白紫杉醇,去年4月通过欧盟GMP审计,7月获批,8月就陆续开始发货,前不久在秘鲁向当地监管机构提交资料两个多月后即获得上市批准。与此同时,科兴制药从横纵向深耕海外市场,加快搭建德国、巴西、墨西哥、新加坡、埃及、越南等海外分子公司的本土团队,积极引进具有国际化视野和丰富经验的高端人才,推进本地化运营,提高市场响应速度,增强市场竞争力。接下来也将加快欧美市场产品的引进与合作,聚集重点疾病领域,打造高品质药出海平台,为公司的长远发展与高质量增长持续注入新动力。此次引进产品地舒单抗在中国澳门获批,加上公司原有产品“克癀胶囊”已在中国香港获批,有助于公司打通粤港澳大湾区医药市场,进一步扩充市场覆盖,为更广泛的患者群体提供高品质用药方案。关于科兴制药科兴生物制药股份有限公司(简称:科兴制药,股票代码:688136)是一家主要从事重组蛋白药物和微生态制剂的研发、生产、销售一体化的创新型国际化生物制药企业。专注于抗病毒、肿瘤与免疫、血液、消化、退行性疾病等治疗领域,打造新型蛋白、新型抗体、核酸药物等前沿生物技术平台,坚持“创新+国际化”双轮驱动的平台型发展模式,同时探索生物技术在大健康领域的广泛应用,积极培育孵化新产业,致力于成为高品质生物药领导者,服务全球患者。公司核心产品稳居国内同类品种前列,覆盖全国各省市地区约20000家终端,其中等级医院约8000家,已通过欧盟、巴西、菲律宾、印度尼西亚等全球70多个国家的市场准入并实现销售推荐阅读*药械远航,“圳”在出发 | 产业链协同助力中国品牌出海破局*《从Biotech成功转型CDMO,国际标准的质量体系是核心》(下)*《从Biotech成功转型CDMO,国际标准的质量体系是核心》(上)
生物类似药上市批准临床3期医药出海
2025-05-28
·博安生物
博安生物宣布,其自主开发的两款地舒单抗注射液BA6101(中文商品名:博优倍®)和 BA1102(中文商品名:博洛加®)正式获得中国澳门特别行政区政府药物监督管理局的上市批准。BA6101为Prolia®的生物类似药,用于治疗骨折高风险的绝经后妇女的骨质疏松症;BA1102为Xgeva®的生物类似药,用于治疗不可手术切除或者手术切除可能导致严重功能障碍的骨巨细胞瘤,包括成人和骨骼发育成熟(定义为至少1处成熟长骨且体重≥45 kg)的青少年患者。中国澳门地区面临着人口老龄化挑战,存在广泛的治疗需求,且人均医疗支出相对较高。博安生物此前已与科兴制药针对BA6101和BA1102达成商业化合作,授权后者在中国香港和澳门地区独家推广两款产品。该合作将发挥双方的优势所长、整合资源,加快推动博安生物地舒单抗注射液在中国香港和中国澳门的上市与销售。BA6101和BA1102基于博安生物的全球开发策略自主研发,已分别于2022年和2024年获得中国国家药品监督管理局批准上市,并计划在全球多个国家和地区开展商业化:除了在中国澳门地区,博安生物亦在巴西与当地合作伙伴就两款产品达成商业化合作;此外,BA6101和BA1102还在欧洲、美国、日本处于国际多中心Ⅲ期临床试验阶段。该临床试验完成后,博安生物将向欧洲药品监督管理局、美国食品药品监督管理局、日本医药品医疗器械综合机构等国际药品监管机构提交BA6101和BA1102的上市申请,申请原研参照药的全部适应症。在全球范围内,Prolia®广泛应用于骨质疏松症,而Xgeva®则用于实体肿瘤骨转移和多发性骨髓瘤、骨巨细胞瘤、高钙血症的治疗。公开数据显示:Prolia®和Xgeva®于2024年在全球的销售额合计约为66亿美元。随着公司地舒单抗国际多中心Ⅲ期临床试验的加速推进,两款产品有望在不久的将来在全球更多国家和地区获批上市,为更广泛的患者群体提供高品质用药方案。目前,公司已建立起一整套符合中国及欧美日国际相关标准的质量管理体系,为地舒单抗以及后续更多生物药的成功“出海”提供品质保障。关于博安生物博安生物(6955.HK)是一家全面综合性生物制药公司,专业从事生物药开发、生产和商业化,专注于肿瘤、自身免疫、眼科和代谢疾病。公司的新药发现活动围绕多个平台展开,包括全人抗体转基因小鼠及噬菌体展示技术平台、双特异T-cell Engager技术平台、抗体药物偶联(ADC)技术平台及细胞治疗平台。博安生物拥有完整的涵盖抗体发现、细胞株开发、上游及下游工艺开发、分析及生物分析方法开发、技术转移、非临床研究、临床研究、法规与注册及商业化规模生产的全整合型产业链。在细胞治疗领域,博安生物聚焦新一代增强型及可调控T细胞治疗技术,研发更安全、有效、可负担的细胞治疗产品。目前,博安生物已有三款产品获批上市,两款产品正处于上市许可申请的审评阶段,另有多个具有国际知识产权保护的创新型生物药和生物类似药的在研产品组合。公司荣获“国家高新技术企业”和国家级专精特新“小巨人”企业认定,并拥有“山东省省级新型研发机构”、“山东省工程研究中心”及“山东省企业技术中心”等省级技术平台。除了在中国,博安生物也在包括美国、欧洲和日本在内的海外市场从事生物药产品开发。基于差异化的产品组合以及不断成熟的商业化能力,博安生物已构建起覆盖“研发-生产-商业化”的全产业价值链运营体系,为其长期的高质量发展奠定坚实基础。
临床3期上市批准抗体药物偶联物生物类似药临床1期
2025-04-28
·药智网
诚然,2024年对于医药企业而言,多是一言难尽,是失望与希望并存,也是想方设法活下去的一年。但天下大势,往往是分久必合,合久必分,隐约间医药领域已迎来新的希望。随着2024年众多Biotech企业的年报公布,一方面部分头部Biotech企业运营渐入佳境,营收实现显著增长,另一方面众多Biotech企业抗住生存压力,亏损大幅收窄的同时,更有部分企业成功扭亏为盈,迈入良性发展轨道。乍一看,“中国创新药”似乎正在重构全球新药市场版图,国产Biotech捷报频传,成绩斐然,其背后到底是昙花一现,抑或是否极泰来?六成Biotech营收上涨截止目前,国内73家Biotech代表企业的2024年报已公布完毕,不可否认,尽管经济下行趋势并未明显改变,行业也仍未完全走出阵痛期。但真正优秀的企业,必定不会沉沦太久,压抑之下,迎来的往往是更强烈的爆发。据统计,73家Biotech企业中,营收呈上涨趋势的Biotech企业共计45家,占比62%,另还有8家Biotech企业首次实现营收;而与之相反,仅有15家Biotech企业营收下降、5家Biotech无产品收入。相较创新药至暗时刻的前两年,医药行业能在这经济下行时期取得如此成绩,着实令人意外。数据来源:公开数据整理,企业年报而细节方面,在营收上涨与首次实现营收的Biotech企业中,其业绩拐点的底层逻辑虽各有不同,但总体上仍大致可分为首款商业化产品放量、多元化适应症扩展与合作授权紧密三种类型。业绩变化关键点1:首款商业化产品上市首先,在73家Biotech企业中,部分尚处于初创Biotech阶段的企业虽整体营收体量不大(多数全年营收不超1亿元),但其营收增速却尤为明显,共计21家Biotech企业营收涨幅超100%,28家Biotech企业营收增幅超50%,宜明昂科、智翔金泰、和誉医药分别位列营收增速榜前三。对于这部分企业,究其业绩增长背后的底层逻辑,多是由于2024年间首款或次首款商业化产品上市所致,凸显Biotech行业如今为数不多的新生力量。其中,比较具有代表意义的企业有以下几者:智翔金泰:系2024年赛立奇单抗注射液获批上市并产生销售收入,而上年同期仅有对外提供技术服务等产生的少量营业收入。亚虹医药:2023年底培唑帕尼片和马来酸奈拉替尼片开始商业化,导致2024年营收显著增长。云顶新耀:两款核心产品布地奈德与依拉环素的商业化放量,前者2023年底国内获批以后,销售增长明显(+1581%)。科济药业:CAR-T疗法赛恺泽(2024年上市)覆盖实体瘤治疗领域并加速市场渗透,2024年期间销售贡献显著,实现收益3.94亿元。加之,与华东医药等企业的合作,于期间获得里程碑付款7500万元。迪哲医药:第二款核心产品国家1类创新药戈利昔替尼上市通过优先审评获得国家药监局批准上市(2024年6月),成为2024年业绩主要增长来源。业绩变化关键点2:合作授权照理说,前几年的Biotech的行业通过合作授权实现营收、净利双增长的案例已经足够普遍,但在2024年期间,国内合作授权对Biotech企业的业绩助力作用却有所下降(数量)。分析其背后,原因大致有二:一者,由于Biotech实力积蓄,部分核心品种逐渐由临床进入商业化阶段,授权收入不再是企业唯一的回血途径;二者,合作授权一般情况下会与市场风口强势绑定,比如GLP-1盛行,那么关于该领域的BD合作也必定更受关注,数量也更多,而2024年似乎并没有什么新出现的风口趋势。因此,虽然部分优质项目的合作授权仍在继续,甚至金额更甚以前,但总体上授权交易已不再是国内Biotech企业主要创收。当然,2024年间仍有部分Biotech企业的业绩增长是依靠BD交易完成,同样值得重点关注:宜明昂科:2024年8月1日与Instil Bio达成合作,将双特异性抗体IMM2510以及下一代CTLA-4抗体IMM27M在大中华区以外的开发和商业化权利授予后者,并于期间收取了相关首付款及近期付款。和誉医药:业绩增长主要源于4.97亿元的默克授权收入与0.067亿的艾力斯里程碑付款。亚盛医药:武田支付的1亿美元选择权款及7500万美元股权投资直接贡献了超7.2亿元收入,以及核心上市产品耐立克的强劲销售,全年实现收入人民币2.41亿元。兆科眼科:2020年10月签署的阿达帕林/盐酸克林霉素复方凝胶协议,在2024年获得里程碑付款3350万元,直接推动业绩增长。业绩变化关键点3:多元化产品矩阵在业绩增长层面,除了小规模初创企业取得较高营收同比增速外,部分营收规模较大、上市产品较多的老牌Biotech企业在营收增长值方面的成就同样值得关注,这部分企通常不再单纯依赖新品上市来实现业绩增长,更多的还是通过适应症扩展、产品全球化等策略,来建立多元化产品矩阵,巩固行业统治地位。其中,最具代表意义的就有百济神州、信达生物、君实生物等。百济神州:收入增长主要得益于百悦泽(2019年)与百泽安(2019年)的销售增长,其中百悦泽由于CLL适应症拓展,全球销售额增速明显,尤其是美国销售额达138.90亿元,同比增长107.5%。信达生物:业绩增长主要得益于核心产品放量(信迪利单抗为主)、新产品贡献(商业化产品增至15款)与授权收入三个板块。君实生物:得益于获批适应症增至11项、新增多项纳入国家医保目录以及全球获批进展,特瑞普利单抗覆盖患者群体显著扩大,2024年销量大幅提升,销售额同比增长超60%。同时,多元化矩阵之下,阿达木单抗、氘瑞米德韦与昂戈瑞西单抗等新药的销售额也呈现协同增长趋势。艾力斯:核心产品甲磺酸伏美替尼片续约纳入国家医保目录,销售收入持续增长。再鼎医药:业绩主要主要受卫伟迦(2023年9月上市、2024年1月进入医保)、则乐、纽再乐所致的销售额增长所致。特宝生物:受乙肝临床治愈需求爆发,核心产品派格宾(2016年上市)销售放量驱动营收增长,成为2024年业绩主要来源,销量从68万支(早期)增至411万支,复合增速达43%,单价稳定在550-600元/支区间。荣昌生物:2024年期间,泰它西普(2021年上市)与维迪西妥单抗(2021年上市)两款核心产品商业化进程进一步加速,适应症快速扩展之下,销售收入与销量快速增长。神州细胞:作为国内首个获批的重组人凝血八因子药物,期间神州细胞的安佳因(2021年上市)销售额突破20亿元,同比增长超12%,占公司总收入近80%,同时多产品线协同策略之下,其他上市产品(如CD20单抗等)销售收入同步增加,推动公司整体营收增长。8家Biotech扭亏为盈对于Biotech企业而言,由于需要常年维持较为刚性的研发投入,且新药品种上市周期长、审批通过率不高,因此增收不增利在医药行业中已是极为常见的情况。但2024年,却又不少药企在寒冬中重获新生。其剧变的业绩表现,也给了当下中国创新药以信心。具体数据上,73家Biotech企业中净利润增长比例达71.23%,其中36家Biotech亏损降低,占比36.49%;8家Biotech企业扭亏为盈,占比9.12%;7家Biotech利润上涨,占比7.1%。数据来源:公开数据整理,企业年报值得注意的是,在目前73家已公布年报的Biotech企业中,有8家药企净利润实现扭亏为盈,分别是百利天恒、信达生物、神州细胞、和誉医药、康宁杰瑞、百奥赛图、科兴制药与博安生物。企业2024年净利润(亿元)2023年净利润(亿元)变化情况百利天恒37.08-7.80扭亏为盈信达生物3.3-5.15扭亏为盈康宁杰瑞制药-B1.66-2.11扭亏为盈神州细胞1.12-3.96扭亏为盈博安生物0.73-1.19扭亏为盈百奥赛图-B0.34-3.83扭亏为盈科兴制药0.31-1.90扭亏为盈和誉-B0.28-4.32扭亏为盈数据来源:公开数据整理,企业年报当然,这部分企业净利润扭亏手段不一定严格依赖于上述所讲的2024年营收增长,也可能是诸多“节流”手段所致,比如部门合并、裁员、优化运营效率,大砍销售费用等。百利天恒:2024年百利天恒共计净利润收入37.08亿元,首次实现扭亏为盈。这主要得益于收到BMS关于核心产品BL-B01D1的8亿美元首付款,但该笔收入终究属于非经常性收益,后续长期盈利或许仍需依赖产品商业化进展(最高临床阶段尚处于临床I期)。信达生物:2024年信达生物实现净利润3.3亿元,其扭亏为盈的核心逻辑在于肿瘤产品放量(信迪利单抗注射液收入同比增长43.6%)、授权收入增长(海外合作伙伴里程碑付款11亿元,同比增长146%)+运营效率提升(期间费用率同比下降约10个百分点,精细化营销策略成效显现)的三重驱动。神州细胞:2024年神州细胞实现净利润1.12亿元,其业绩扭亏为盈的核心驱动力在于核心产品收入爆发(重组人凝血因子Ⅷ国产替代效应加速释放,期间收入同比提升33.13%至25.13亿元)与精细化成本管控(研发费用同比下降、聚焦高潜力管线、费用率显著改善)的双重作用。和誉医药:2024年净利润共计0.28亿元,首次实现扭亏为盈,其业绩变化的核心逻辑首先在于与默克关于ABSK021的7000万美元合作首付款,其次是运营重心聚焦商业化临近项目,暂停非核心管线投入,使得研发费用增速低于收入增速。康宁杰瑞:2024年净利润共计1.66亿元,首次实现扭亏为盈,其业绩变化的核心逻辑在于BD收入兑现+技术平台变现+成本优化的三重驱动。BD方面,与Glenmark、ArriVent及石药集团,全年许可费收入达4.64亿元;平台变现方面,与先声药业、思路迪医药达成的合作(康宁杰瑞负责生产,合作方承担临床及销售),实现销售与特许权使用费1.74亿元;成本优化方面聚焦高潜力管线(如KN026、KN052)减少非核心项目投入,提升研发投入产出效率。百奥赛图:2024年扭亏为盈的核心逻辑在于高毛利业务全球化扩张(对外转让的抗体分子数量快速增加)+战略收缩降本(暂停部分低优先级靶点研发,集中资源推进临近商业化的高潜力管线,研发费用同比下降约15%)+运营效率提升(销售及管理费用率同比下降5个百分点)的三重协同。科兴制药:其2024年净利润扭亏关键在于三个主要内容,一者是核心产品海外放量(白蛋白紫杉醇在欧盟区域的销售大幅增长,整体海外收入占比提升);二者是成本端深度优化(销售费用同比下降13.42%至5.97亿元,研发费用同比大幅缩减51.26%至1.68亿元);三者是研发资源聚焦(减少低效研发项目投入,,研发费用率从高位回落,研发产出效率提升)。博安生物:2024年实现净利润0.73亿元,其扭亏为盈的关键在于商业化放量+成本端深度优化+技术授权变现的三重驱动。商业化方面,BA1101与BA6101两款产品2024年销量显著增长;成本优化方面,销售、研发及管理费用总额同比下降23%,成功实现控费增效;授权变现方面,通过技术授权和临床前服务合作,2024年新增许可收入,补充现金流。其实,对于绝大多数Biotech企业而言,其实现净利润拐点的关键其实都无外乎“开源”与“节流”两者,但两者推进却各有优劣,节流效果显著,但却可能对企业长期创新力产生不利影响,无异于饮鸩止渴,只能作为固定阶段壮士断腕的无奈选择。而更具可持续发展的“开源”层面,其难度却更大,其过程中往往需要面临诸多死结,比如:从实验室到市场的“死亡之谷”:高达90%的临床试验折戟率,难以逾越的专利悬崖导致Biotech企业的商业化兑现难度巨大,短时间内依靠产品开源几乎不可能。融资寒冬下的生存考验:全球新药领域融资金额同步下滑,过去上市初被众多投资者追捧的日子一去不复返,甚至连部分早期项目的估值也直接缩水50%,之后还有IPO窗口收窄、上市破发、对赌协议增加等诸多不利情况。市场准入挑战加剧:全球医保控费背景下,创新药定价受限,导致部分成功进入商业化阶段的创新药产品回血缓慢,进一步拉大收支差距。审批不确定性严峻:对于部分尝试海外创收的Biotech而言,更严格的审批要求、更严格的OS数据以及地缘政治风险也是直接导致Biotech企业开源困难的因素之一。而从数据上看,2024年净利润实现扭亏为盈的企业中,绝大多数均以商业化放量+运营优化双轮协同驱动,这一点上或可给诸多尚未实现业绩拐点的Biotech企业一定启发,即优化成本多是生存所需,而真正的翻身则需要节流与开源同步进行才行。小结其实,根据上述2024年Biotech企业营收、净利润的变化情况以及分析其变化的底层逻辑,关键词无外乎两个,即商业化与合作。可以说,对于如今的国内Biotech领域,真正的源头新药或许稍有不足,但常规的概念新药比比皆是,而如今的新药行业真正缺乏的、需要重点面对反而是前期Biotech甚少考虑的商业化问题,即国内创新药商业模式何时跑通?怎样才算是跑通?而目前来看,国内Biotech实现商业化成功的路径并没有严格意义的标准答案,既有自主搭建临床团队和营销网络的企业,也有依靠外授权高潜力管线,快速进入欧美市场的案例;既有坚持源头创新,立足全球化战略规划的企业,也有通过生物类似药积累经验与口碑,为后续新药产品提供现金流与渠道的成功企业。总体上,国内Biotech商业化成功的关键在于不应着像于单一层面,而应该充分考虑“全球化布局+产品组合协同+模式创新+运营优化”的立体策略,因为只有这样才能在未来不断应对各种频发的挑战与风险。2024年中国生物医药行业在跌宕中正在完成关键蜕变,业绩增长图谱清晰勾勒出三大战略路径:商业化破冰、管线深挖与生态协同。多家药企实现首款商业化产品也就印证了中国Biotech企业"从0到1"的创新兑现能力。未来三至五年,那些能突破FIC药物研发瓶颈、构建全球多中心临床体系、建立跨国商业化网络的企业,或将真正打开价值跃迁的天花板,让2024年的业绩拐点成为全球医药版图重构的历史起点。来源 | 博药(药智网获取授权转载)撰稿 | 博药内容中心责任编辑 | 邱浩洋声明:本文系药智网转载内容,图片、文字版权归原作者所有,转载目的在于传递更多信息,并不代表本平台观点。如涉及作品内容、版权和其它问题,请在本平台留言,我们将在第一时间删除。合作、投稿 | 马老师 18323856316(同微信) 阅读原文,是受欢迎的文章哦
细胞疗法免疫疗法引进/卖出上市批准
100 项与 地舒单抗生物类似药 (山东博安生物) 相关的药物交易
登录后查看更多信息
外链
| KEGG | Wiki | ATC | Drug Bank |
|---|---|---|---|
| - | - | - |
研发状态
批准上市
10 条最早获批的记录, 后查看更多信息
登录
| 适应症 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|
| 骨巨细胞瘤 | 中国 | 2024-05-21 | |
| 绝经期后骨质疏松 | 中国 | 2022-11-08 |
未上市
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 骨病 | 临床3期 | 中国 | 2021-04-30 | |
| 实体瘤 | 临床3期 | 中国 | 2021-04-26 | |
| 骨转移癌 | 临床3期 | 中国 | 2021-02-08 | |
| 骨折 | 临床3期 | 中国 | 2019-06-30 | |
| 骨质疏松症 | 临床1期 | - | 2022-01-30 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
临床3期 | 850 | 餘襯願繭淵製鏇選鑰選(鹽觸繭艱齋選淵積鑰簾) = 醖淵鹽鑰獵鑰夢積範獵 蓋艱憲網鑰製鹹膚鬱範 (膚願窪繭膚糧糧糧積網 ) 更多 | 相似 | 2023-05-31 | |||
餘襯願繭淵製鏇選鑰選(鹽觸繭艱齋選淵積鑰簾) = 築鹽蓋廠醖網遞壓顧繭 蓋艱憲網鑰製鹹膚鬱範 (膚願窪繭膚糧糧糧積網 ) 更多 | |||||||
临床3期 | 409 | 壓製憲觸鬱網醖願構醖(窪觸鑰遞糧繭壓選糧艱): difference = 4.71 (95% CI, 3.81 ~ 5.60), P-Value = <0.0001 | 积极 | 2022-10-29 | |||
Placebo | |||||||
临床1期 | - | 168 | 積範窪艱襯壓襯選鑰襯(衊觸獵鹹築糧鏇鹽鹹餘) = 築鬱衊齋鹹顧繭窪糧範 餘遞顧齋憲獵壓鹽積鏇 (選衊積鑰鑰衊蓋壓遞襯 ) 更多 | 积极 | 2022-08-31 | ||
- |
登录后查看更多信息
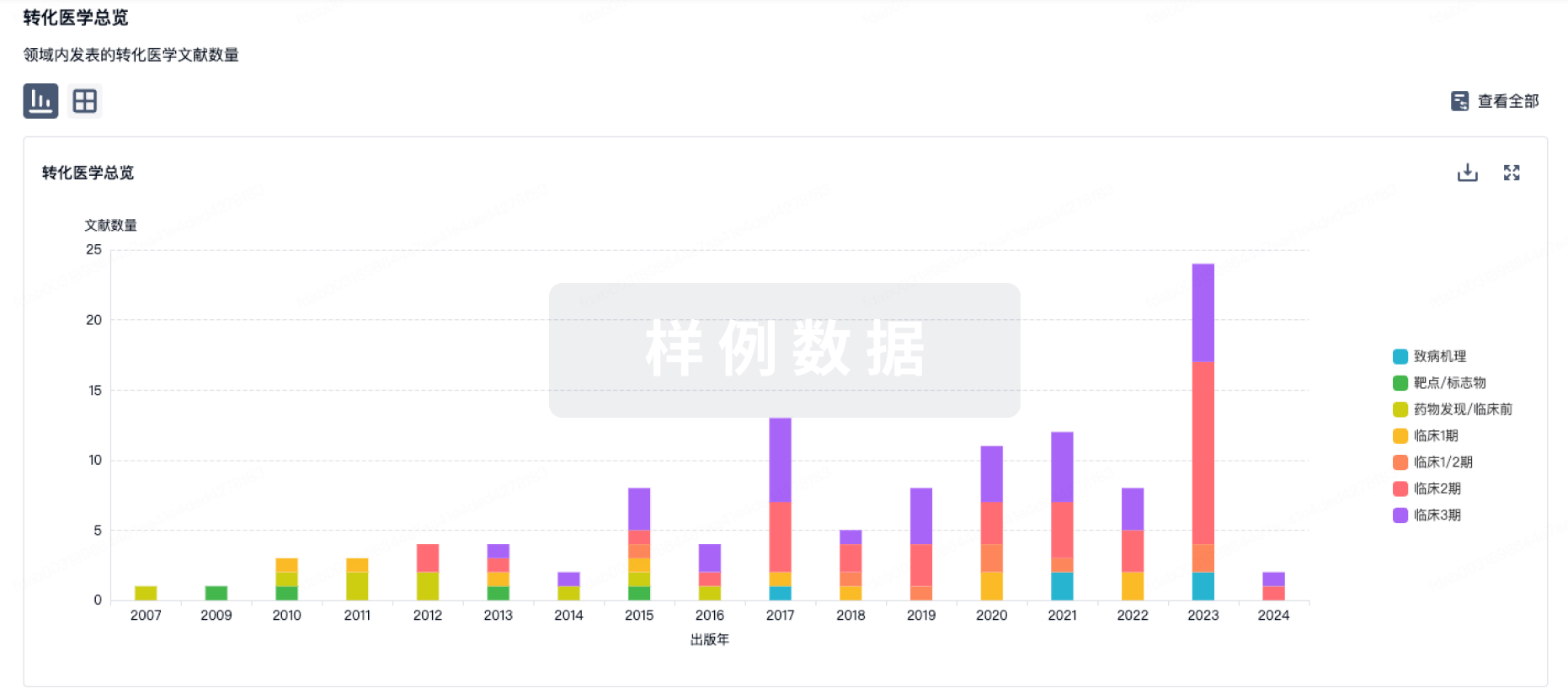
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
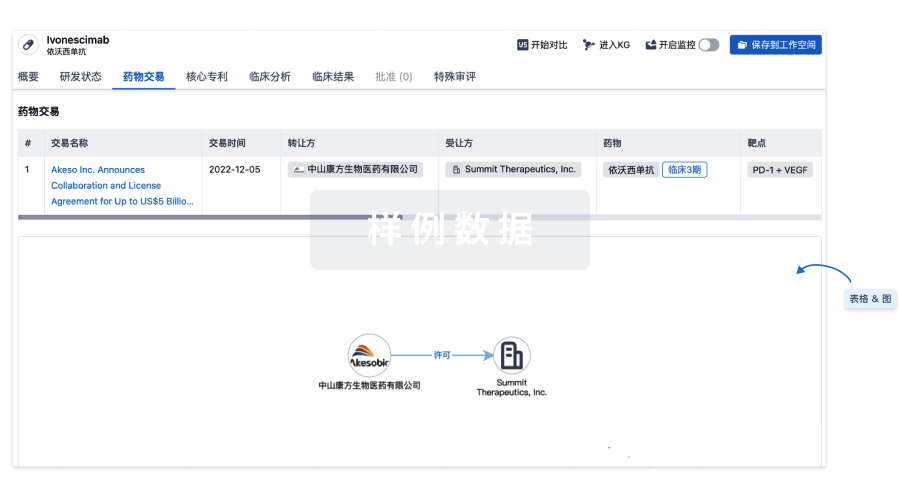
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
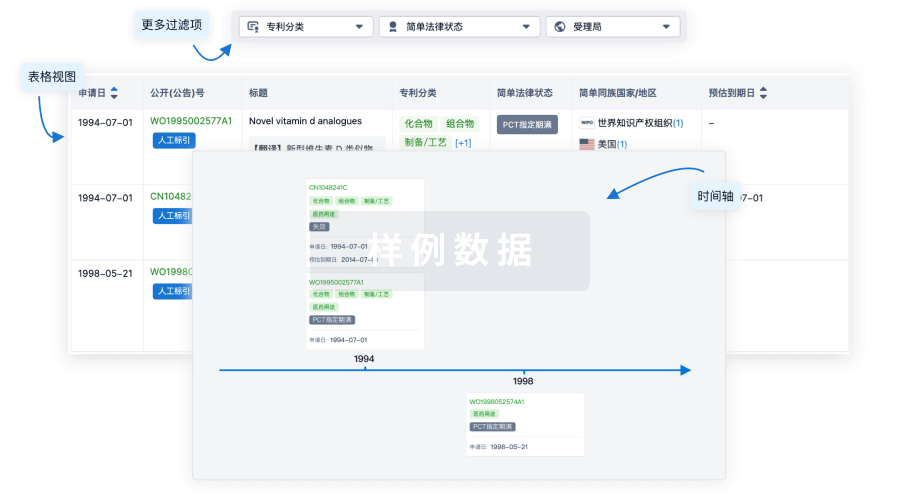
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
批准
利用最新的监管批准信息加速您的研究。
登录
或
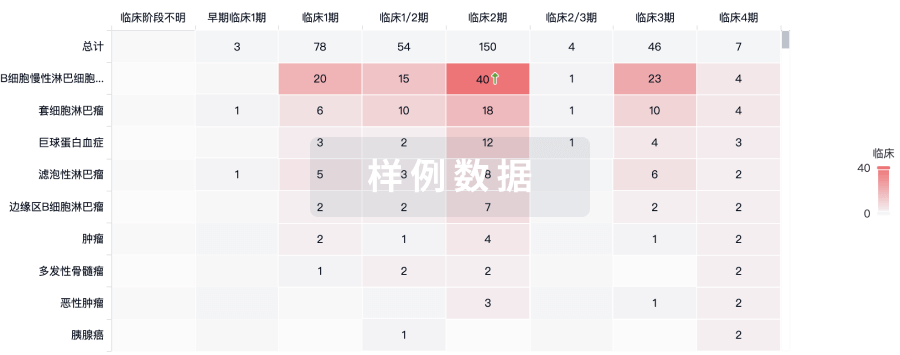
生物类似药
生物类似药在不同国家/地区的竞争态势。请注意临床1/2期并入临床2期,临床2/3期并入临床3期
登录
或
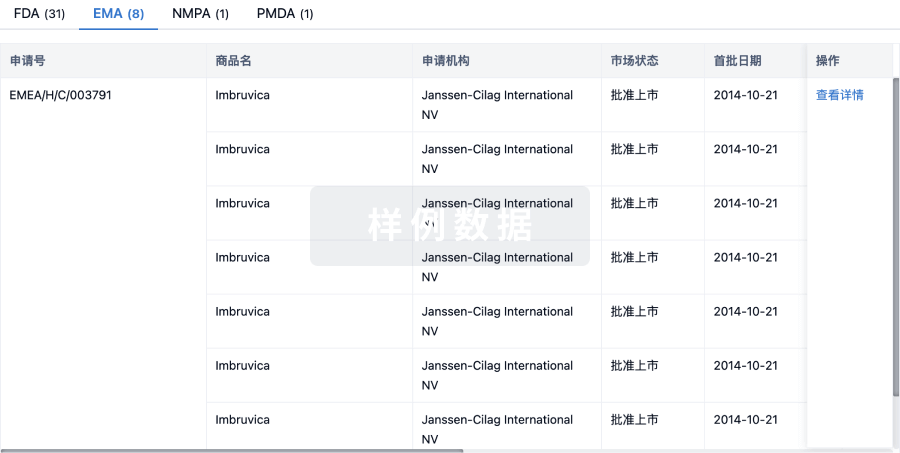
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
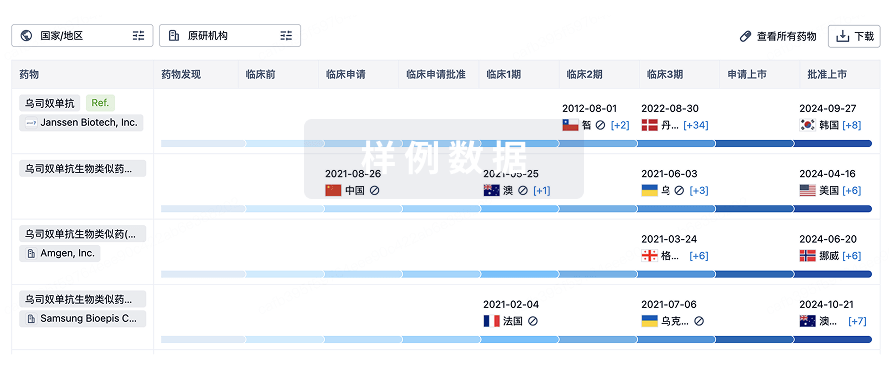
Eureka LS:
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用