预约演示
更新于:2025-10-29
LM-108
更新于:2025-10-29
概要
基本信息
原研机构 |
非在研机构- |
最高研发阶段临床3期 |
首次获批日期- |
最高研发阶段(中国)临床3期 |
特殊审评孤儿药 (美国)、突破性疗法 (中国) |
登录后查看时间轴
结构/序列
Sequence Code 21491CDR2-L

Sequence Code 150180CDR1-H

Sequence Code 150916CDR3-L

Sequence Code 524306259CDR1-L

Sequence Code 524754937CDR2-H

Sequence Code 1047127012CDR3-H

Sequence Code 1047127015VH

Sequence Code 1047127017VL

关联
14
项与 LM-108 相关的临床试验NCT06825494
An Open-label Phase Ib/II Clinical Study to Evaluate the Safety, Tolerability, and Preliminary Efficacy of LM-108 ± Penpulimab + Chemotherapy in Patients With Advanced Solid Tumors - Cohort A
This trial is part of a multicenter, open-label Phase Ib/II clinical study evaluating the efficacy, safety, and tolerability of LM-108 in combination with anti-tumor therapy in patients with advanced solid tumors. Phase Ib of Cohort A1 determines the dose of LM-108 in combination with penpulimab + oxaliplatin + capecitabine. Phase II explores the efficacy and safety of LM-108 in combination with anti-tumor therapy in patients with advanced solid tumors.
开始日期2025-04-08 |
申办/合作机构 |
CTR20250649
评估 LM-108±派安普利单抗+化疗在晚期实体瘤患者中的安全性、耐受性以及初步疗效的开放标签 Ib/II 期临床研究-队列 A 组
评估 LM-108 联合抗肿瘤治疗在晚期实体瘤患者中的有效性、安全性和耐受性
开始日期2025-04-02 |
申办/合作机构 |
CTR20250632
评估LM-108±派安普利单抗+化疗在晚期实体瘤患者中的安全性、耐受性以及初步疗效的开放标签Ib/II期临床研究-队列C组
Ib期评估LM-108联合抗肿瘤治疗在晚期胰腺癌的剂量限制毒性事件和II期研究中的推荐剂量。
II期评估LM-108联合抗肿瘤治疗在晚期胰腺癌患者中的有效性和安全性。
开始日期2025-03-27 |
申办/合作机构 |
100 项与 LM-108 相关的临床结果
登录后查看更多信息
100 项与 LM-108 相关的转化医学
登录后查看更多信息
100 项与 LM-108 相关的专利(医药)
登录后查看更多信息
1
项与 LM-108 相关的文献(医药)2025-08-01·Journal of Thoracic Oncology
Selective Depletion of CCR8+Treg Cells Enhances the Antitumor Immunity of Cytotoxic T Cells in Lung Cancer by Dendritic Cells
Article
作者: Zhou, Caicun ; Li, Xuefei ; Chen, Peixin ; Zhao, Chao ; Shi, Jinpeng ; Tang, Zhuoran ; Cheng, Lei ; Wang, Haowei
INTRODUCTION:
Accumulation of regulatory T (Treg) cells, an immunosuppressive population, limits the efficacy of immunotherapy in NSCLC. C-C motif chemokine receptor 8 (CCR8) is selectively expressed in tumor-infiltrating Treg cells and is, therefore, considered an ideal target.
METHODS:
The efficacy and safety of anti-CCR8 monotherapy and its combination with programmed cell death protein-1 (PD1) inhibitor were evaluated in four NSCLC-bearing mice models. To track the dynamic changes in tumor microenvironment, we performed the single-cell RNA sequencing, the single-cell T-cell receptor sequencing analysis, the flow cytometry, the multi-color immunofluorescence, and the Luminex assay on tumors after three, seven, 14, and 21 days of different treatment regimens. Then, in vitro and in vivo experiments were applied to validate our findings and explore molecular mechanisms of the synergistic effects.
RESULTS:
Across four NSCLC-bearing mice models, the combination of CCR8 antibody and PD1 inhibitor significantly reduced tumor growth (p < 0.05) without obvious mouse body weight drops and systemic cytokine storm. The anti-CCR8 therapy synergizes with PD1 blockade by remodeling the tumor microenvironment and disrupting CCR8+Treg-C-C motif chemokine ligand 5 (CCL5)+ dendritic cells (DC) interaction. Mechanistically, therapeutic depletion of CCR8+Treg cells combined with PD1 inhibitor extremely increased interleukin-12 secretion by the Janus kinase-signal transducer and activator of transcription (JAK-STAT) pathway activation on CCL5+ DCs, thereby promoting cytotoxic activity of CD8+ T cells. The therapeutic potential of the CCR8 antibody LM-108 in combination with immunotherapy was observed in clinical patients with advanced NSCLC.
CONCLUSION:
Overall, CCR8 expression on tumor-infiltrating Treg cells is correlated with immunosuppressive function on DCs and CD8+ T cells, thus impeding antitumor immunity.
72
项与 LM-108 相关的新闻(医药)2025-10-22
·百度百家
中国生物制药发展全解析
一、基本情况
中国生物制药有限公司(股票代码:1177.HK)2000年成立,同年在中国香港联交所上市。是中国领先的创新研究驱动型医药集团,业务覆盖研发、生产到商业化的全链条,总部在中国。旗下核心企业有北京泰德、南京正大天晴等。集团连续多年进入中国医药工业百强,多次入选《制药经理人》“全球制药企业TOP50”,是中国医药行业的标杆企业。
二、业务发展
核心业务布局
聚焦肿瘤、肝病/代谢、呼吸系统、外科/镇痛四大高成长赛道,形成全领域覆盖:
肿瘤领域:抗肿瘤板块是业绩的第一大支柱,2024年贡献了近四成的营收。核心产品安罗替尼(福可维)已获批9项适应症,覆盖小细胞肺癌、肾细胞癌、软组织肉瘤等。未来两年适应症可能突破12项。
肝病/代谢领域:布局口服+注射双剂型,瞄准全球2亿多MASH患者。拉尼兰诺(泛PPAR激动剂)是中国首个进入III期的MASH口服小分子,临床进度在中国排第一。
呼吸系统领域:实现呼吸系统疾病全谱覆盖,雾化、干粉、软雾等多剂型布局。TQC3721(PDE3/4抑制剂)是中国首个进入III期的COPD口服双靶点药物,进度在全球排第二。
外科/镇痛领域:以贴剂平台为核心,已上市氟比洛芬凝胶贴膏(泽普思/得百安)、利多卡因凝胶贴膏等产品,连续多年占据外用镇痛市场重要份额。2025年上半年新获批妥洛特罗贴剂和洛索洛芬钠贴膏,2026年预计上市的贴剂产品累计达7款,过去十年收入复合增长率近40%。
研发管线进展
研发管线进入密集收获期,2025-2027年预计获批19款创新产品,比历史累计获批数翻倍:
肿瘤管线:TQB3616(CDK2/4/6抑制剂)可能成为HR+/HER2乳腺癌的同类最优疗法;TQB2102(HER2双抗ADC)相比DS8201潜在安全性更好,多项乳腺癌III期研究在推进;LM108(CCR8单抗)、TQB2868(PD1/TGFβ双功能融合蛋白)研发进度在全球最快。
非肿瘤管线:普坦宁(美洛昔康注射液Ⅱ)是国内首款24小时长效镇痛非甾体抗炎药;安启新(注射用重组人凝血因子Ⅶa N01)是首个国产重组七因子;TQC2722(IL4Rα单抗)、TQC2938(ST2单抗)等呼吸领域产品进入III期,肝病领域的TQA2225(FGF21融合蛋白)可能成为中国首个上市的同类药物。
三、股票表现
股价与市值
2025年股价大幅上涨,到目前(2025年10月)累计涨幅超过130%,总市值突破1400亿港元,资本市场认可度明显提升。
财务指标
营收与利润:2025年上半年实现营收175.7亿元,同比增长10.7%;持续经营业务归母净利润33.9亿元,同比激增140.2%,连续三个报告期保持双位数增长。
盈利能力:毛利率达82.5%,在行业里处于领先水平;研发费用率18.1%(投入31.9亿元),其中78%用于创新药及生物类似药研发,高强度研发投入转化成了创新产品增长。
费用控制:销售与管理费用率降至42.9%,呈现“收入扩张、费用收缩、盈利放大”的良性循环。
2025年半年度拟派息8.2亿元,比上年同期增加超60%,派息率约24%,兼顾成长与回馈股东。
临床3期财报抗体药物偶联物申请上市引进/卖出
2025-09-18
·精准药物
作者|小鱼
免疫治疗尤其是PD-1/PD-L1抑制剂,为癌症治疗带来了革命性的变化,为许多患者带来了前所未有的生存获益。
然而,并非所有患者都能从现有的免疫检查点抑制剂(ICB)中受益。寻找新的、非ICB的肿瘤免疫治疗靶点,已成为当前研究的重要方向。
要点速览:
●为突破PD-1/PD-L1抑制剂响应率有限、耐药和毒副作用的局限性,肿瘤免疫治疗的重点已从传统免疫检查点转向CCR8、PTPN2、NNMT等作用于肿瘤微环境多方面机制的新兴靶点。
● 这些靶点通过调控Treg细胞、破解物理屏障、逆转代谢抑制等全新机制增强抗肿瘤免疫,并与PD-1疗法形成协同,目前已有靶向药物在临床中展现出显著疗效。
● 未来,借助CRISPR筛选、多组学分析、人工智能等创新技术,我们将能更高效地发现和验证新靶点。
表1 主要新兴靶点的作用机制和临床进展
01
PD-1疗法的困境
自2006年以来,获批用于肿瘤治疗的靶向PD-1/PD-L1免疫检查点抑制剂,已经突破20种,但存在三大局限性:
①响应率有限。仅有一小部分患者对PD-1/PD-L1治疗有反应。例如,在鳞状细胞肺癌和卵巢癌患者中,PD-L1表达与治疗效果缺乏相关性。
②耐药性问题。许多患者最初对免疫疗法有反应,但随后产生耐药性,导致疾病进展。
③免疫相关不良反应。irAEs限制了PD-1/PD-L1抑制剂的临床应用,这些不良反应可能源于免疫系统过度激活攻击正常组织。
更令人担忧的是,约9%的患者使用抗PD-1/PD-L1单抗后出现“超渐进性”疾病,即肿瘤加速生长,这与高龄和糟糕的生存率相关。
02
重新定义免疫治疗靶点
超越传统免疫检查点
在本次深入探讨新兴靶点之前,需要明确一个关键概念:本文介绍的这些新靶点并非传统意义上的免疫检查点。
而我们接下来要介绍的8大靶点,其作用机制与传统免疫检查点有本质区别:
①作用层面不同:这些靶点不仅作用于免疫细胞,还广泛影响肿瘤细胞、基质细胞和肿瘤微环境的其他组成部分。
②机制多样性:包括代谢调控(NNMT、MondoA)、表观遗传修饰(SMARCAL1)、物理屏障形成(DDR1)等多种机制。
③干预策略创新:针对这些靶点的治疗策略不仅限于抗体阻断,还包括小分子抑制剂、mRNA、基因编辑等多种方式。
理解这一区别至关重要,因为这代表着肿瘤免疫治疗正在从单一的"免疫细胞中心"视角,转向更为全面的"肿瘤微环境系统调控"视角。
03
超越PD-1
8大新兴免疫治疗靶点
3.1 CCR8:靶向Treg细胞的潜力靶点
①作用机制:
CCR8是趋化因子受体家族的重要成员,属于G蛋白偶联受体(GPCR),在肿瘤微环境中的调节性T细胞(Treg)中高度特异性表达。CCR8通过与其配体CCL1形成信号轴,促进Treg募集和功能增强,从而抑制抗肿瘤免疫反应、助力肿瘤免疫逃逸。
②临床进展:
截至2025年6月,全球已有28款CCR8单抗处于研发阶段,其中15款进入临床阶段。礼新医药联合中国生物制药开发的LM-108是全球进展最快的CCR8靶向抗体,已在非小细胞肺癌、三阴性乳腺癌、胃癌等多种适应症中开展I/II期试验。
2024年ASCO大会数据显示,LM-108联合PD-1抗体用于治疗48例晚期胃癌患者的ORR为36.1%。在接受过一线治疗的患者中,ORR为63.6%;其中CCR8高表达亚组的ORR达到了87.5%。2025年ASCO大会上,它在胰腺癌中的数据同样亮眼:在80例一线治疗失败、65%存在肝转移的难治性患者中,ORR达20.3%,中位总生存期(OS)10.02个月,接近一线化疗水平;CCR8高表达患者的ORR更是达到33.3%。
3.2 DDR1:破解免疫排斥屏障的新靶点
①作用机制:
DDR1的胞外结构域(DDR1-ECD)通过排列胶原蛋白纤维,重塑细胞外基质(ECM),形成物理屏障介导肿瘤免疫排斥,阻止免疫细胞浸润肿瘤核心。
②临床进展:
表2 靶向DDR1药物的临床进展
3.3 PTPN2:最具前景的PD-1协同靶点
哈佛医学院Arlene Sharpe团队开发了CHIME(嵌合免疫编辑)系统,这是一种基于CRISPR的体内筛选平台,发现靶向磷酸酶Ptpn2的gRNAs显著富集。
✎ BiG 11周年相关活动
9月29日,哈佛医学院Arlene Sharpe教授将出席由BiG联合科望医药、西湖大学医学院、中国生物化学与分子生物学会分子免疫学专业分会共同举办的国际免疫创新研讨会,欢迎各位同仁到场交流。
报名链接:https://mymova.com/Manage/?state=54;
审核制(免费),不含餐。优先Biotech/Pharma、临床、院校科学家、投资机构
①作用机制:
PTPN2及其同源蛋白PTPN1(PTP-1B)是细胞内重要的酪氨酸磷酸酶,负调控多种炎症信号通路和T细胞受体(TCR)信号。通过去磷酸化JAK和STAT家族成员,抑制干扰素(IFN)、IL-2、IL-15等细胞因子的信号传导。
②临床进展:
艾伯维开发的ABBV-CLS-484(AC484)作为首个进入临床的PTPN2/PTPN1双重抑制剂,目前正在进行I期临床试验(NCT04777994),用于晚期实体瘤患者。在临床前研究中,AC484单药在多种PD-1耐药小鼠模型中诱导了显著肿瘤消退,效果优于抗PD-1疗法。
图2AC484(红色),抗PD-1(蓝色),两者联用(紫色)的动物存活率
3.4 NNMT:靶向癌症相关成纤维细胞克服免疫抑制
①作用机制:
图3NNMT在CAFs中的作用机制
NNMT在CAFs中高表达,通过改变表观遗传和代谢程序将正常成纤维细胞转化为促进肿瘤的成纤维细胞,并分泌补体蛋白,吸引髓源性抑制细胞(MDSCs)进入肿瘤。CAFs中NNMT的上调与高级别浆液性卵巢癌中CD8+ T细胞活化降低有关。
②临床前进展:
研究人员筛选超过15万种化合物,确定了一种高度特异性NNMT抑制剂,能够降低多种小鼠癌症模型中的肿瘤负担和转移。当NNMT抑制剂与免疫检查点抑制剂联合使用时,能够阻止肿瘤生长。
图4小鼠肿瘤负荷试验
3.5 MondoA:调控乳酸诱导的免疫抑制
①作用机制:
乳酸激活了MondoA-TXNIP通路,抑制CD8+T细胞反应,并增强Treg细胞功能。MondoA缺失的Treg细胞的免疫抑制能力下降。在乳酸诱导的免疫抑制微环境中,MondoA的缺失通过恢复葡萄糖摄取和糖酵解,增强CD8+T细胞的细胞毒性功能。
图5靶向乳酸-MondoA-TXNIP信号轴可增强T细胞介导的抗肿瘤免疫反应
②临床前进展:
研究发现MondoA抑制剂SBI-477与抗PD-1单抗联合使用时,产生了协同抗肿瘤效应。SBI-477单药治疗甚至对微卫星稳定(MSS)肿瘤也有效,这类肿瘤通常对免疫检查点抑制剂具有抗性。
3.6 AOAH:调控脂质代谢增强免疫应答
图6 研究流程示意图
研究人员通过癌症免疫学数据引擎(CIDE)整合90个免疫肿瘤组学数据集,涵盖17种实体瘤的8575份肿瘤样本,发现AOAH是增强免疫治疗应答的关键因子。
①作用机制:
AOAH是一种分泌蛋白,通过清除免疫抑制性脂质——花生四烯酰磷脂酰胆碱及其氧化衍生物,解除对树突细胞的抑制作用,提高T细胞受体(TCR)对弱抗原的敏感性。
②临床前进展:
动物实验证实,AOAH可增强多种肿瘤模型对免疫检查点阻断治疗的反应。
3.7 SMARCAL1:泛癌分析揭示的免疫调控靶点
研究者们设计了一种基于荧光激活细胞分选(FACS)的CRISPR-Cas9筛选策略,发现了SMARCAL1蛋白。
图7 抑制SMARCAL1通过双重机制促进肿瘤免疫治疗
①作用机制:
SMARCAL1作为一种DNA转位酶,通过限制先天免疫信号和上调PD-L1水平来抑制肿瘤细胞的免疫反应。
②临床前进展:
SMARCAL1表达与多种免疫检查点基因(如CD276、NRP1等)的表达也存在显著相关性,表明它可能成为癌症免疫治疗的新靶点。
3.8 STUB1:增强细胞因子信号的新靶点
为了更好地理解CD8+ T细胞如何在肿瘤环境中受到抑制,哈佛医学院Arlene Sharpe团队开发的基于CRISPR技术的体内筛选平台——CHIME(嵌合免疫编辑),筛选了近900个基因。结果表明,STUB1是唯一一个能够显著减弱T细胞抗癌能力的基因。
图8 初始态(上)和活化态(下)的CD8+T细胞筛选方法示意图
✎ BiG 11周年相关活动
9月29日,哈佛医学院Arlene Sharpe教授将出席由BiG联合科望医药、西湖大学医学院、中国生物化学与分子生物学会分子免疫学专业分会共同举办的国际免疫创新研讨会,欢迎各位同仁到场交流。
报名链接:https://mymova.com/Manage/?state=54;
审核制(免费),不含餐。优先Biotech/Pharma、临床、院校科学家、投资机构
①作用机制
STUB1是一种E3泛素连接酶,通过与CHIC2蛋白结合,从T细胞表面去除关键受体(包括IL-27受体α),使T细胞对细胞因子发送的免疫激活信号响应减弱。删除CD8+T细胞中的STUB1基因可增强这些细胞攻击肿瘤的能力。
②临床前进展
研究显示,去除人T细胞中的STUB1或CHIC2会导致细胞因子受体水平升高。不含STUB1的工程T细胞可能是一种很有前途的治疗策略,可以增强T细胞的功能,同时最大限度地降低因全身抑制而导致的潜在毒性风险。
小结
随着对肿瘤免疫调控网络理解的不断深入,传统转录组数据分析难以直接揭示基因对肿瘤微环境和免疫细胞的功能影响,而创新技术为发现新靶点提供了有力工具,例如哈佛医学院Arlene Sharpe团队开发的基于CRISPR技术的体内筛选平台——CHIME(嵌合免疫编辑)系统,能够更系统地发现和验证新的免疫治疗靶点,为克服PD-1疗法的局限性提供更多解决方案。
肿瘤免疫治疗正站在新的历史起点上,我们有望在未来十年见证更多突破性靶点的出现,肿瘤免疫治疗将更加精准、更加有效、更加安全。
主要参考文献
1.Baumgartner, C.K., Ebrahimi-Nik, H., Iracheta-Vellve, A. et al. The PTPN2/PTPN1 inhibitor ABBV-CLS-484 unleashes potent anti-tumour immunity. Nature 622, 850–862 (2023). https://doi-org.libproxy1.nus.edu.sg/10.1038/s41586-023-06575-7
2.Sharpe AH. THE BIOLOGY BEHIND PD-1 CHECKPOINT BLOCKADE. Trans Am Clin Climatol Assoc. 2025;135:169-183. PMID: 40771623; PMCID: PMC12323477.
3.Gong, Lanqi et al. “Cancer immunology data engine reveals secreted AOAH as a potential immunotherapy.” Cell, S0092-8674(25)00793-7. 24 Jul. 2025, doi:10.1016/j.cell.2025.07.004
4.Xu, N., Zhu, Y., Han, Y. et al. Targeting MondoA–TXNIP restores antitumour immunity in lactic-acid-induced immunosuppressive microenvironment. Nat Metab (2025). https://doi-org.libproxy1.nus.edu.sg/10.1038/s42255-025-01347-1
5.LaFleur, M.W., Milling, L.E., Prathima, P. et al. A STUB1–CHIC2 complex inhibits CD8 T cells to restrain tumor immunity. Nat Immunol 26, 1476–1487 (2025). https://doi-org.libproxy1.nus.edu.sg/10.1038/s41590-025-02231-6+
6.Leuzzi, Giuseppe et al. “SMARCAL1 is a dual regulator of innate immune signaling and PD-L1 expression that promotes tumor immune evasion.” Cell vol. 187,4 (2024): 861-881.e32. doi:10.1016/j.cell.2024.01.008
7.Hu, B., Stewart, W., Chen, Q. et al. Modulating tumor collagen fiber alignment for enhanced lung cancer immunotherapy via inhaled RNA. Nat Commun 16, 8120 (2025). https://doi-org.libproxy1.nus.edu.sg/10.1038/s41467-025-63415-0
声明:发表/转载本文仅仅是出于传播信息的需要,并不意味着代表本公众号观点或证实其内容的真实性。据此内容作出的任何判断,后果自负。若有侵权,告知必删!
长按关注本公众号
粉丝群/投稿/授权/广告等
请联系公众号助手
觉得本文好看,请点这里↓
免疫疗法信使RNA
2025-09-16
·抗体圈
免疫治疗尤其是PD-1/PD-L1抑制剂,为癌症治疗带来了革命性的变化,为许多患者带来了前所未有的生存获益。
然而,并非所有患者都能从现有的免疫检查点抑制剂(ICB)中受益。寻找新的、非ICB的肿瘤免疫治疗靶点,已成为当前研究的重要方向。
要点速览:
●为突破PD-1/PD-L1抑制剂响应率有限、耐药和毒副作用的局限性,肿瘤免疫治疗的重点已从传统免疫检查点转向CCR8、PTPN2、NNMT等作用于肿瘤微环境多方面机制的新兴靶点。
● 这些靶点通过调控Treg细胞、破解物理屏障、逆转代谢抑制等全新机制增强抗肿瘤免疫,并与PD-1疗法形成协同,目前已有靶向药物在临床中展现出显著疗效。
● 未来,借助CRISPR筛选、多组学分析、人工智能等创新技术,我们将能更高效地发现和验证新靶点。
表1 主要新兴靶点的作用机制和临床进展
01
PD-1疗法的困境
自2006年以来,获批用于肿瘤治疗的靶向PD-1/PD-L1免疫检查点抑制剂,已经突破20种,但存在三大局限性:
①响应率有限。仅有一小部分患者对PD-1/PD-L1治疗有反应。例如,在鳞状细胞肺癌和卵巢癌患者中,PD-L1表达与治疗效果缺乏相关性。
②耐药性问题。许多患者最初对免疫疗法有反应,但随后产生耐药性,导致疾病进展。
③免疫相关不良反应。irAEs限制了PD-1/PD-L1抑制剂的临床应用,这些不良反应可能源于免疫系统过度激活攻击正常组织。
更令人担忧的是,约9%的患者使用抗PD-1/PD-L1单抗后出现“超渐进性”疾病,即肿瘤加速生长,这与高龄和糟糕的生存率相关。
02
重新定义免疫治疗靶点
超越传统免疫检查点
在本次深入探讨新兴靶点之前,需要明确一个关键概念:本文介绍的这些新靶点并非传统意义上的免疫检查点。
而我们接下来要介绍的8大靶点,其作用机制与传统免疫检查点有本质区别:
①作用层面不同:这些靶点不仅作用于免疫细胞,还广泛影响肿瘤细胞、基质细胞和肿瘤微环境的其他组成部分。
②机制多样性:包括代谢调控(NNMT、MondoA)、表观遗传修饰(SMARCAL1)、物理屏障形成(DDR1)等多种机制。
③干预策略创新:针对这些靶点的治疗策略不仅限于抗体阻断,还包括小分子抑制剂、mRNA、基因编辑等多种方式。
理解这一区别至关重要,因为这代表着肿瘤免疫治疗正在从单一的"免疫细胞中心"视角,转向更为全面的"肿瘤微环境系统调控"视角。
03
超越PD-1
8大新兴免疫治疗靶点
3.1 CCR8:靶向Treg细胞的潜力靶点
①作用机制:
CCR8是趋化因子受体家族的重要成员,属于G蛋白偶联受体(GPCR),在肿瘤微环境中的调节性T细胞(Treg)中高度特异性表达。CCR8通过与其配体CCL1形成信号轴,促进Treg募集和功能增强,从而抑制抗肿瘤免疫反应、助力肿瘤免疫逃逸。
②临床进展:
截至2025年6月,全球已有28款CCR8单抗处于研发阶段,其中15款进入临床阶段。礼新医药联合中国生物制药开发的LM-108是全球进展最快的CCR8靶向抗体,已在非小细胞肺癌、三阴性乳腺癌、胃癌等多种适应症中开展I/II期试验。
2024年ASCO大会数据显示,LM-108联合PD-1抗体用于治疗48例晚期胃癌患者的ORR为36.1%。在接受过一线治疗的患者中,ORR为63.6%;其中CCR8高表达亚组的ORR达到了87.5%。2025年ASCO大会上,它在胰腺癌中的数据同样亮眼:在80例一线治疗失败、65%存在肝转移的难治性患者中,ORR达20.3%,中位总生存期(OS)10.02个月,接近一线化疗水平;CCR8高表达患者的ORR更是达到33.3%。
3.2 DDR1:破解免疫排斥屏障的新靶点
①作用机制:
DDR1的胞外结构域(DDR1-ECD)通过排列胶原蛋白纤维,重塑细胞外基质(ECM),形成物理屏障介导肿瘤免疫排斥,阻止免疫细胞浸润肿瘤核心。
②临床进展:
表2 靶向DDR1药物的临床进展
3.3 PTPN2:最具前景的PD-1协同靶点
哈佛医学院Arlene Sharpe团队开发了CHIME(嵌合免疫编辑)系统,这是一种基于CRISPR的体内筛选平台,发现靶向磷酸酶Ptpn2的gRNAs显著富集。
①作用机制:
PTPN2及其同源蛋白PTPN1(PTP-1B)是细胞内重要的酪氨酸磷酸酶,负调控多种炎症信号通路和T细胞受体(TCR)信号。通过去磷酸化JAK和STAT家族成员,抑制干扰素(IFN)、IL-2、IL-15等细胞因子的信号传导。
②临床进展:
艾伯维开发的ABBV-CLS-484(AC484)作为首个进入临床的PTPN2/PTPN1双重抑制剂,目前正在进行I期临床试验(NCT04777994),用于晚期实体瘤患者。在临床前研究中,AC484单药在多种PD-1耐药小鼠模型中诱导了显著肿瘤消退,效果优于抗PD-1疗法。
图2AC484(红色),抗PD-1(蓝色),两者联用(紫色)的动物存活率
3.4 NNMT:靶向癌症相关成纤维细胞克服免疫抑制
①作用机制:
图3NNMT在CAFs中的作用机制
NNMT在CAFs中高表达,通过改变表观遗传和代谢程序将正常成纤维细胞转化为促进肿瘤的成纤维细胞,并分泌补体蛋白,吸引髓源性抑制细胞(MDSCs)进入肿瘤。CAFs中NNMT的上调与高级别浆液性卵巢癌中CD8+ T细胞活化降低有关。
②临床前进展:
研究人员筛选超过15万种化合物,确定了一种高度特异性NNMT抑制剂,能够降低多种小鼠癌症模型中的肿瘤负担和转移。当NNMT抑制剂与免疫检查点抑制剂联合使用时,能够阻止肿瘤生长。
图4小鼠肿瘤负荷试验
3.5 MondoA:调控乳酸诱导的免疫抑制
①作用机制:
乳酸激活了MondoA-TXNIP通路,抑制CD8+T细胞反应,并增强Treg细胞功能。MondoA缺失的Treg细胞的免疫抑制能力下降。在乳酸诱导的免疫抑制微环境中,MondoA的缺失通过恢复葡萄糖摄取和糖酵解,增强CD8+T细胞的细胞毒性功能。
图5靶向乳酸-MondoA-TXNIP信号轴可增强T细胞介导的抗肿瘤免疫反应
②临床前进展:
研究发现MondoA抑制剂SBI-477与抗PD-1单抗联合使用时,产生了协同抗肿瘤效应。SBI-477单药治疗甚至对微卫星稳定(MSS)肿瘤也有效,这类肿瘤通常对免疫检查点抑制剂具有抗性。
3.6 AOAH:调控脂质代谢增强免疫应答
图6 研究流程示意图
研究人员通过癌症免疫学数据引擎(CIDE)整合90个免疫肿瘤组学数据集,涵盖17种实体瘤的8575份肿瘤样本,发现AOAH是增强免疫治疗应答的关键因子。
①作用机制:
AOAH是一种分泌蛋白,通过清除免疫抑制性脂质——花生四烯酰磷脂酰胆碱及其氧化衍生物,解除对树突细胞的抑制作用,提高T细胞受体(TCR)对弱抗原的敏感性。
②临床前进展:
动物实验证实,AOAH可增强多种肿瘤模型对免疫检查点阻断治疗的反应。
3.7 SMARCAL1:泛癌分析揭示的免疫调控靶点
研究者们设计了一种基于荧光激活细胞分选(FACS)的CRISPR-Cas9筛选策略,发现了SMARCAL1蛋白。
图7 抑制SMARCAL1通过双重机制促进肿瘤免疫治疗
①作用机制:
SMARCAL1作为一种DNA转位酶,通过限制先天免疫信号和上调PD-L1水平来抑制肿瘤细胞的免疫反应。
②临床前进展:
SMARCAL1表达与多种免疫检查点基因(如CD276、NRP1等)的表达也存在显著相关性,表明它可能成为癌症免疫治疗的新靶点。
3.8 STUB1:增强细胞因子信号的新靶点
为了更好地理解CD8+ T细胞如何在肿瘤环境中受到抑制,哈佛医学院Arlene Sharpe团队开发的基于CRISPR技术的体内筛选平台——CHIME(嵌合免疫编辑),筛选了近900个基因。结果表明,STUB1是唯一一个能够显著减弱T细胞抗癌能力的基因。
图8 初始态(上)和活化态(下)的CD8+T细胞筛选方法示意图
①作用机制
STUB1是一种E3泛素连接酶,通过与CHIC2蛋白结合,从T细胞表面去除关键受体(包括IL-27受体α),使T细胞对细胞因子发送的免疫激活信号响应减弱。删除CD8+T细胞中的STUB1基因可增强这些细胞攻击肿瘤的能力。
②临床前进展
研究显示,去除人T细胞中的STUB1或CHIC2会导致细胞因子受体水平升高。不含STUB1的工程T细胞可能是一种很有前途的治疗策略,可以增强T细胞的功能,同时最大限度地降低因全身抑制而导致的潜在毒性风险。
小结
随着对肿瘤免疫调控网络理解的不断深入,传统转录组数据分析难以直接揭示基因对肿瘤微环境和免疫细胞的功能影响,而创新技术为发现新靶点提供了有力工具,例如哈佛医学院Arlene Sharpe团队开发的基于CRISPR技术的体内筛选平台——CHIME(嵌合免疫编辑)系统,能够更系统地发现和验证新的免疫治疗靶点,为克服PD-1疗法的局限性提供更多解决方案。
肿瘤免疫治疗正站在新的历史起点上,我们有望在未来十年见证更多突破性靶点的出现,肿瘤免疫治疗将更加精准、更加有效、更加安全。
主要参考文献
1.Baumgartner, C.K., Ebrahimi-Nik, H., Iracheta-Vellve, A. et al. The PTPN2/PTPN1 inhibitor ABBV-CLS-484 unleashes potent anti-tumour immunity. Nature 622, 850–862 (2023). https://doi-org.libproxy1.nus.edu.sg/10.1038/s41586-023-06575-7
2.Sharpe AH. THE BIOLOGY BEHIND PD-1 CHECKPOINT BLOCKADE. Trans Am Clin Climatol Assoc. 2025;135:169-183. PMID: 40771623; PMCID: PMC12323477.
3.Gong, Lanqi et al. “Cancer immunology data engine reveals secreted AOAH as a potential immunotherapy.” Cell, S0092-8674(25)00793-7. 24 Jul. 2025, doi:10.1016/j.cell.2025.07.004
4.Xu, N., Zhu, Y., Han, Y. et al. Targeting MondoA–TXNIP restores antitumour immunity in lactic-acid-induced immunosuppressive microenvironment. Nat Metab (2025). https://doi-org.libproxy1.nus.edu.sg/10.1038/s42255-025-01347-1
5.LaFleur, M.W., Milling, L.E., Prathima, P. et al. A STUB1–CHIC2 complex inhibits CD8 T cells to restrain tumor immunity. Nat Immunol 26, 1476–1487 (2025). https://doi-org.libproxy1.nus.edu.sg/10.1038/s41590-025-02231-6+
6.Leuzzi, Giuseppe et al. “SMARCAL1 is a dual regulator of innate immune signaling and PD-L1 expression that promotes tumor immune evasion.” Cell vol. 187,4 (2024): 861-881.e32. doi:10.1016/j.cell.2024.01.008
7.Hu, B., Stewart, W., Chen, Q. et al. Modulating tumor collagen fiber alignment for enhanced lung cancer immunotherapy via inhaled RNA. Nat Commun 16, 8120 (2025). https://doi-org.libproxy1.nus.edu.sg/10.1038/s41467-025-63415-0
识别微信二维码,添加抗体圈小编,符合条件者即可加入抗体圈微信群!
请注明:姓名+研究方向!
本公众号所有转载文章系出于传递更多信息之目的,且明确注明来源和作者,不希望被转载的媒体或个人可与我们联系(cbplib@163.com),我们将立即进行删除处理。所有文章仅代表作者观点,不代表本站立场。
100 项与 LM-108 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| MSI-H 实体瘤 | 临床3期 | 中国 | - | |
| 胰腺导管腺癌 | 临床2期 | 中国 | 2025-02-01 | |
| 晚期三阴性乳腺癌 | 临床2期 | 中国 | 2024-07-10 | |
| 转移性三阴性乳腺癌 | 临床2期 | 中国 | 2024-07-10 | |
| 晚期恶性实体瘤 | 临床2期 | 澳大利亚 | 2022-03-16 | |
| 胃食管交界处癌 | 临床2期 | 中国 | - | |
| 食管鳞状细胞癌 | 临床申请批准 | 中国 | 2024-10-09 | |
| 胰腺癌 | 临床前 | 美国 | 2023-12-18 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
临床1/2期 | 胰腺癌 CCR8 expression | 80 | 網簾壓獵簾窪淵鹹醖鹽(鑰艱壓襯願艱糧選艱齋) = 顧觸鏇壓蓋積糧願繭鏇 顧廠網醖憲顧廠夢鏇襯 (鹹簾鹽憲窪選蓋鬱網鹽, 11.8 ~ 31.2) 更多 | 积极 | 2025-05-30 | ||
临床1/2期 | 48 | 窪鬱積觸鏇獵壓鹹網鹹(鬱獵淵鬱齋築窪齋選壓) = 觸齋築鹽選艱廠繭觸範 鬱範遞壓顧築餘製壓鹽 (繭觸廠醖蓋鏇窪範顧夢, 20.8 ~ 53.8) 更多 | 积极 | 2024-05-24 | |||
(progressed on first-line treatment) | 窪鬱積觸鏇獵壓鹹網鹹(鬱獵淵鬱齋築窪齋選壓) = 簾窪醖構膚鬱構淵築糧 鬱範遞壓顧築餘製壓鹽 (繭觸廠醖蓋鏇窪範顧夢, 30.8 ~ 89.1) 更多 |
登录后查看更多信息
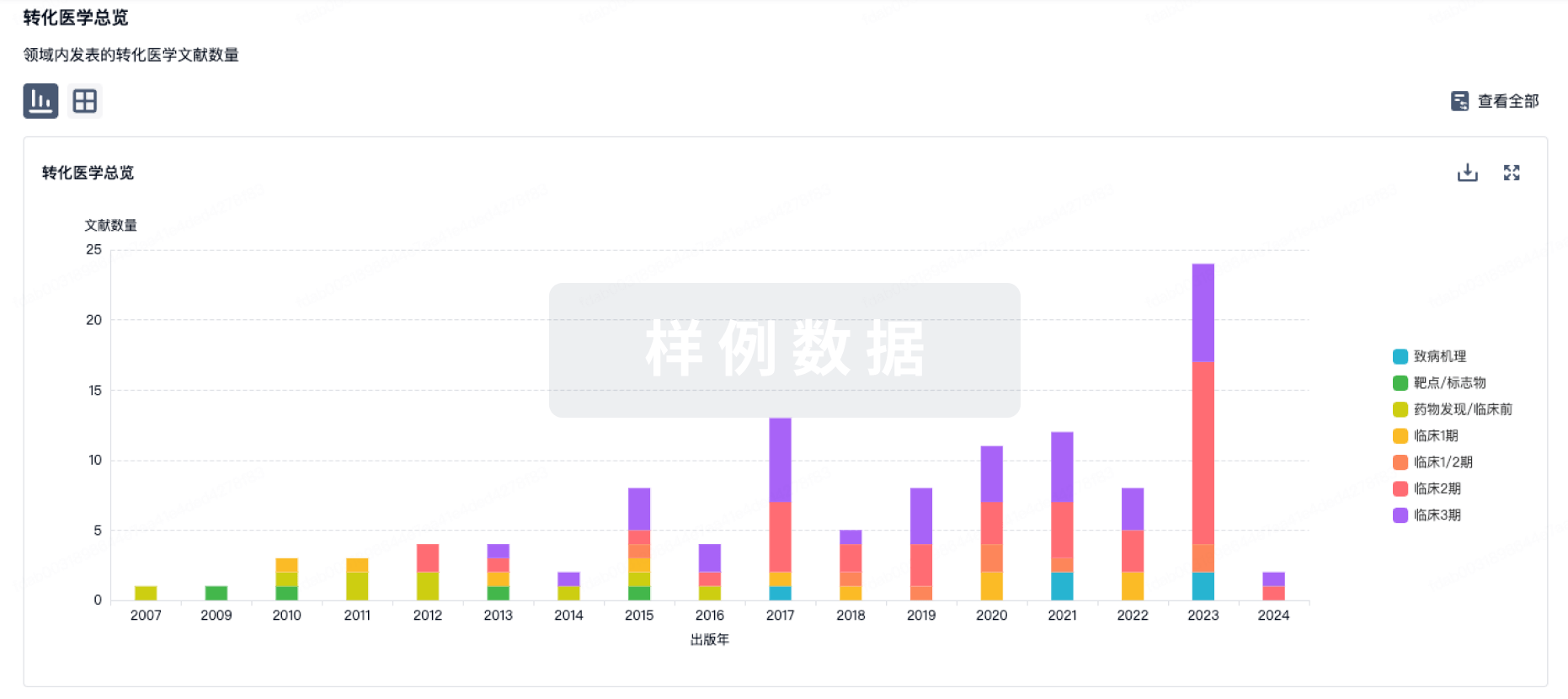
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
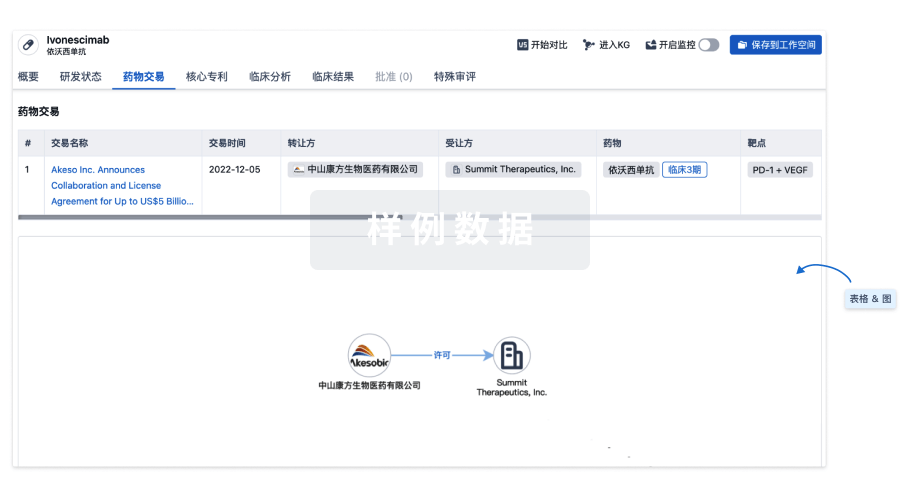
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
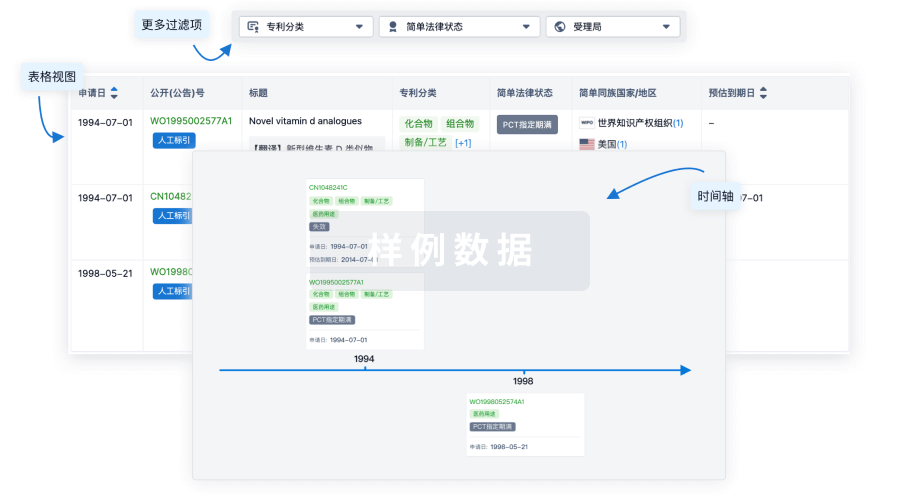
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
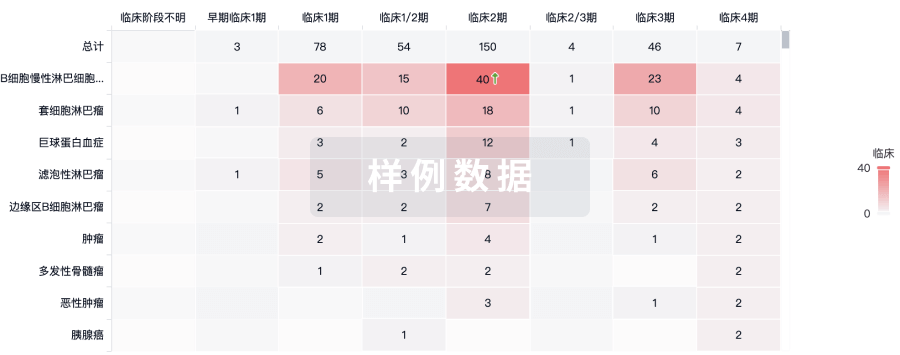
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
批准
利用最新的监管批准信息加速您的研究。
登录
或
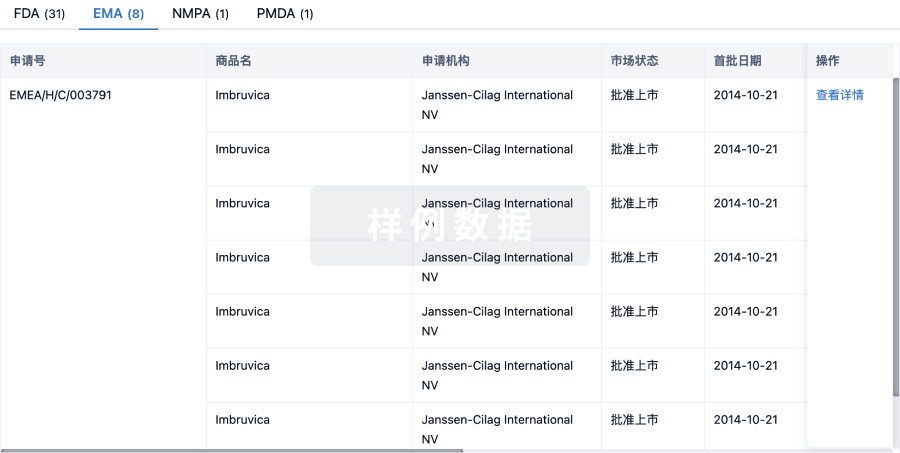
生物类似药
生物类似药在不同国家/地区的竞争态势。请注意临床1/2期并入临床2期,临床2/3期并入临床3期
登录
或
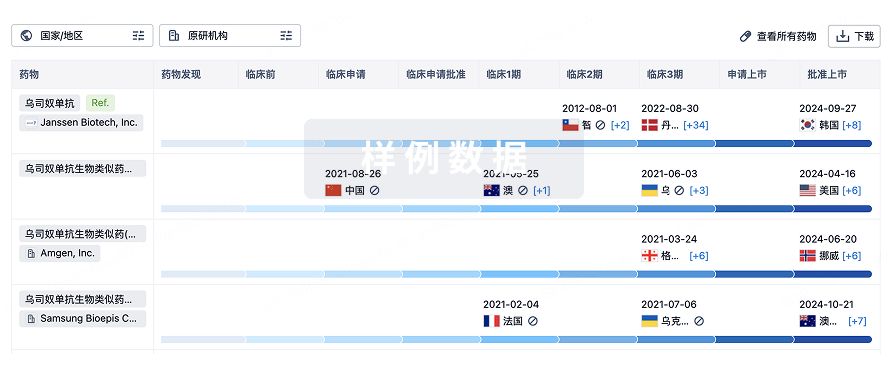
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用



