预约演示
更新于:2025-08-29

Keryx Biopharmaceuticals, Inc.
更新于:2025-08-29
概览
标签
血液及淋巴系统疾病
泌尿生殖系统疾病
内分泌与代谢疾病
小分子化药
疾病领域得分
一眼洞穿机构专注的疾病领域
暂无数据
技术平台
公司药物应用最多的技术
暂无数据
靶点
公司最常开发的靶点
暂无数据
| 排名前五的药物类型 | 数量 |
|---|---|
| 小分子化药 | 1 |
| 排名前五的靶点 | 数量 |
|---|---|
| Phosphates(磷酸盐) | 1 |
关联
1
项与 Keryx Biopharmaceuticals, Inc. 相关的药物作用机制 Phosphates 调节剂 |
最高研发阶段批准上市 |
首次获批国家/地区 日本 |
首次获批日期2014-01-17 |
26
项与 Keryx Biopharmaceuticals, Inc. 相关的临床试验NCT04649411
A 24-Week, Open-Label, Randomized, 2-Arm Study to Evaluate the Safety and Tolerability of KRX-0502 (Ferric Citrate) in Children With Iron Deficiency Anemia Associated With Non-Dialysis Dependent Chronic Kidney Disease
This study will be conducted to evaluate the safety and tolerability of ferric citrate in pediatric participants with iron deficiency anemia (IDA) associated with non-dialysis dependent chronic kidney disease (NDD-CKD).
开始日期2025-01-01 |
NCT04523727
A 36-week, Single-Arm, Open-label Study to Evaluate the Safety and Tolerability of Ferric Citrate in Children With Hyperphosphatemia Related to Chronic Kidney Disease
This study will be conducted to assess the safety and tolerability of ferric citrate in pediatric participants with hyperphosphatemia related to chronic kidney disease (CKD).
开始日期2022-06-16 |
NCT03236246
Study of KRX-0502 (Ferric Citrate) Dose Regimens in Subjects With Non-Dialysis Dependent Chronic Kidney Disease and Iron-Deficiency Anemia
The objectives of this study are to assess the long-term efficacy and safety of different dose regimens of KRX-0502 in the treatment of iron deficiency anemia (IDA) in adult subjects with non-dialysis dependent chronic kidney disease (CKD).
开始日期2017-08-15 |
100 项与 Keryx Biopharmaceuticals, Inc. 相关的临床结果
登录后查看更多信息
0 项与 Keryx Biopharmaceuticals, Inc. 相关的专利(医药)
登录后查看更多信息
7
项与 Keryx Biopharmaceuticals, Inc. 相关的文献(医药)2018-08-01·The American journal of cardiology3区 · 医学
Usefulness of Oral Ferric Citrate in Patients With Iron-Deficiency Anemia and Chronic Kidney Disease With or Without Heart Failure
3区 · 医学
Article
作者: McCullough, Peter A ; Fishbane, Steven ; Uhlig, Katrin ; Neylan, John F ; Pergola, Pablo E
Patients with chronic inflammatory conditions including chronic kidney disease (CKD) and heart failure (HF) are undertreated with iron-deficiency anemia (IDA). Progressive inflammation and reduced iron transport associated with CKD and HF may reduce the efficacy of oral iron therapy. Oral ferric citrate improves anemia markers in CKD, but its effects in patients with CKD and concomitant HF have not been described. Patients with CKD not on dialysis and IDA from a phase 2 and 3 trial were treated with ferric citrate (n = 190) or placebo (n = 188); patients with HF were identified from medical histories. Hemoglobin response was defined as a ≥10.0-g/L increase in hemoglobin. Changes in hemoglobin, transferrin saturation, ferritin, and serum phosphate from baseline to week 12 and the incidence of adverse events potentially related to HF were evaluated. HF was reported in 22% (n = 81) of patients. The proportion of patients with hemoglobin response to ferric citrate treatment did not significantly differ in patients with and without HF (43% vs 49%, respectively; p = 0.47); changes from baseline in hemoglobin, iron parameters, and serum phosphate were similar. Adverse events potentially related to HF were noted more frequently in patients with HF (ferric citrate, 23%; placebo, 17%) versus those without HF (ferric citrate, 12%; placebo, 11%). In conclusion, these results indicate a potential role for ferric citrate in the treatment of IDA in patients with CKD not on dialysis and concomitant HF.
2017-06-01·Journal of the American Society of Nephrology : JASN1区 · 医学
Effects of Ferric Citrate in Patients with Nondialysis-Dependent CKD and Iron Deficiency Anemia
1区 · 医学
Article
作者: Chertow, Glenn M ; Uhlig, Katrin ; Neylan, John ; Block, Geoffrey A ; Fishbane, Steven ; Pergola, Pablo E ; Loram, Lisa
Iron deficiency anemia is common and consequential in nondialysis-dependent CKD (NDD-CKD). Efficacy and tolerability of conventional oral iron supplements are mixed; intravenous iron administration associates with finite but important risks. We conducted a randomized double-blind clinical trial in adults with NDD-CKD and iron deficiency anemia to compare the safety and efficacy of oral ferric citrate (n=117) and placebo (n=115). The primary end point was the proportion of patients who achieved a ≥1.0 g/dl increase in hemoglobin at any time during a 16-week randomized period. Patients who completed the 16-week period could also participate in an 8-week open-label extension period. Significantly more patients randomized to ferric citrate achieved the primary end point (61 [52.1%] versus 22 [19.1%] with placebo; P<0.001). All secondary end points reached statistical significance in the ferric citrate group, including the mean relative change in hemoglobin (0.84 g/dl; 95% confidence interval, 0.58 to 1.10 g/dl; P<0.001) and the proportion of patients who achieved a sustained increase in hemoglobin (≥0.75 g/dl over any 4-week period during the randomized trial; 57 [48.7%] versus 17 [14.8%] with placebo; P<0.001). Rates of serious adverse events were similar in the ferric citrate (12.0%) and placebo groups (11.2%). Gastrointestinal disorders were the most common adverse events, with diarrhea reported in 24 (20.5%) and 19 (16.4%) and constipation in 22 (18.8%) and 15 (12.9%) patients treated with ferric citrate and placebo, respectively. Overall, in patients with NDD-CKD, we found oral ferric citrate to be a safe and efficacious treatment for iron deficiency anemia.
2017-03-01·Drugs in R&D4区 · 医学
Net Budgetary Impact of Ferric Citrate as a First-Line Phosphate Binder for the Treatment of Hyperphosphatemia: A Markov Microsimulation Model
4区 · 医学
ArticleOA
作者: Sibbel, Scott P ; Hsieh, Andrew ; Sharma, Amit ; Van Wyck, David ; Brunelli, Steven M ; Chertow, Glenn M
Ferric citrate (FC) has demonstrated efficacy as a phosphate binder and reduces the requirements for erythropoiesis-stimulating agents (ESAs) and intravenous (IV) iron in dialysis patients. We developed a net budgetary impact model to evaluate FC vs. other phosphate binders from the vantage of a large dialysis provider. We used a Markov microsimulation model to simulate mutually referential longitudinal effects between serum phosphate and phosphate binder dose; categories of these defined health states. Health states probabilistically determined treatment attendance and utilization of ESA and IV iron. We derived model inputs from a retrospective analysis of incident phosphate binder users from a large dialysis organization (January 2011-June 2013) and incorporated treatment effects of FC from a phase III trial. The model was run over a 1-year time horizon. We considered fixed costs of providing dialysis; costs of administering ESA and IV iron; and payment rates for dialysis, ESAs, and IV iron. In the base-case model, FC had a net budgetary impact (savings) of +US$213,223/year per 100 patients treated vs. standard of care. One-way sensitivity analyses showed a net budgetary impact of up to +US$316,296/year per 100 patients treated when higher hemoglobin levels observed with FC translated into a 30% additional ESA dose reduction, and up to +US$223,281/year per 100 patients treated when effects on missed treatment rates were varied. Two-way sensitivity analyses in which acquisition costs for ESA and IV iron were varied showed a net budgetary impact of +US$104,840 to +US$213,223/year per 100 patients treated. FC as a first-line phosphate binder would likely yield substantive savings vs. standard of care under current reimbursement.
31
项与 Keryx Biopharmaceuticals, Inc. 相关的新闻(医药)2025-07-31
Received U.S. FDA approval for EMPAVELI® (pegcetacoplan) for treatment of patients 12 years and older with C3G and primary IC-MPGN Announced capped royalty purchase agreement with Sobi under which Apellis receives up to $300 million for 90% of ex-U.S. royalties of Aspaveli® (pegcetacoplan) Generated $178 million in 2Q 2025 revenues, including $171 million in U.S. net product sales SYFOVRE® (pegcetacoplan injection) injection demand grew 6% quarter-over-quarter, with U.S. net product revenue of $151 million Cash and cash equivalents of $370 million as of June 30, 2025; existing cash, $275 million payment from Sobi, and future product sales expected to be sufficient to fund business to sustainable profitability. Management to host conference call today at 8:30 a.m. ET
WALTHAM, Mass., July 31, 2025 (GLOBE NEWSWIRE) -- Apellis Pharmaceuticals, Inc. (Nasdaq: APLS), today announced its second quarter 2025 financial results and business highlights.
“We are incredibly proud of the recent FDA approval of EMPAVELI in C3G and primary IC-MPGN and are now focused on bringing this transformational therapy to patients. With two C3-targeting medicines approved across four serious diseases, we have further cemented our position as a leader in complement,” said Cedric Francois, M.D., Ph.D., chief executive officer at Apellis. “On top of our regulatory success, we were encouraged to see SYFOVRE’s continued market leadership in GA.”
Second Quarter 2025 Business Highlights and Upcoming Milestones
Maximizing EMPAVELI’s impact in rare diseases
C3 glomerulopathy (C3G) and primary immune complex glomerulonephritis (IC-MPGN): EMPAVELI was approved by the U.S. Food and Drug Administration (FDA) as the first treatment for C3G and primary IC-MPGN for patients 12 and older. The approval was based on the Phase 3 VALIANT study results, which demonstrated an unprecedented 68% reduction in proteinuria, stabilization of kidney function, and substantial clearance of C3 deposits as measured by C3 staining, compared to placebo. EMPAVELI is the first and only U.S. FDA approved treatment for primary IC-MPGN, adolescent patients with C3G, and post-transplant C3G disease recurrence New 52-week data from the VALIANT study, presented at the European Renal Association (ERA) Congress in June, demonstrated sustained efficacy, including robust proteinuria reduction and stable kidney function across a broad patient population. Safety data remained favorable and continued to show an acceptable profile. Sobi, the Company’s exclusive ex-U.S. commercialization partner, expects an opinion from the European Medicines Agency’s (EMA) Committee for Medicinal Products for Human Use (CHMP) for its indication extension application for Aspaveli (the brand name for EMPAVELI outside the U.S.) before year-end 2025 Paroxysmal nocturnal hemoglobinuria (PNH): Recorded $20.8 million in EMPAVELI U.S. net product revenue for the second quarter 2025 Continued high patient compliance rates of 97% Delayed graft function (DGF) and Focal segmental glomerulosclerosis (FSGS) On track to initiate pivotal studies in 2H 2025, one in DGF and one in FSGS, two rare kidney diseases in which the complement pathway plays a significant role and there are no approved therapies
EMPAVELI was approved by the U.S. Food and Drug Administration (FDA) as the first treatment for C3G and primary IC-MPGN for patients 12 and older. The approval was based on the Phase 3 VALIANT study results, which demonstrated an unprecedented 68% reduction in proteinuria, stabilization of kidney function, and substantial clearance of C3 deposits as measured by C3 staining, compared to placebo. EMPAVELI is the first and only U.S. FDA approved treatment for primary IC-MPGN, adolescent patients with C3G, and post-transplant C3G disease recurrence New 52-week data from the VALIANT study, presented at the European Renal Association (ERA) Congress in June, demonstrated sustained efficacy, including robust proteinuria reduction and stable kidney function across a broad patient population. Safety data remained favorable and continued to show an acceptable profile. Sobi, the Company’s exclusive ex-U.S. commercialization partner, expects an opinion from the European Medicines Agency’s (EMA) Committee for Medicinal Products for Human Use (CHMP) for its indication extension application for Aspaveli (the brand name for EMPAVELI outside the U.S.) before year-end 2025
EMPAVELI is the first and only U.S. FDA approved treatment for primary IC-MPGN, adolescent patients with C3G, and post-transplant C3G disease recurrence New 52-week data from the VALIANT study, presented at the European Renal Association (ERA) Congress in June, demonstrated sustained efficacy, including robust proteinuria reduction and stable kidney function across a broad patient population. Safety data remained favorable and continued to show an acceptable profile. Sobi, the Company’s exclusive ex-U.S. commercialization partner, expects an opinion from the European Medicines Agency’s (EMA) Committee for Medicinal Products for Human Use (CHMP) for its indication extension application for Aspaveli (the brand name for EMPAVELI outside the U.S.) before year-end 2025
Recorded $20.8 million in EMPAVELI U.S. net product revenue for the second quarter 2025 Continued high patient compliance rates of 97%
On track to initiate pivotal studies in 2H 2025, one in DGF and one in FSGS, two rare kidney diseases in which the complement pathway plays a significant role and there are no approved therapies
Transforming the treatment of geographic atrophy (GA) secondary to age-related macular degeneration (AMD)
SYFOVRE: Generated $150.6 million in SYFOVRE U.S. net product revenue in the second quarter of 2025 Total injections grew 6% quarter-over-quarter SYFOVRE remains the clear market leader in GA with 55% of new patient starts and total market share exceeding 60% during the quarter Utilization of SYFOVRE free goods remained high during the quarter and impacted revenue by approximately $13 million Delivered approximately 95K SYFOVRE doses to physician offices, including ~82K commercial doses and ~13K free goods doses Initiated the Phase 2 study of APL-3007 + SYFOVRE; potential next generation treatment aimed at comprehensively blocking complement activity in the retina and choroid
Generated $150.6 million in SYFOVRE U.S. net product revenue in the second quarter of 2025 Total injections grew 6% quarter-over-quarter SYFOVRE remains the clear market leader in GA with 55% of new patient starts and total market share exceeding 60% during the quarter Utilization of SYFOVRE free goods remained high during the quarter and impacted revenue by approximately $13 million Delivered approximately 95K SYFOVRE doses to physician offices, including ~82K commercial doses and ~13K free goods doses Initiated the Phase 2 study of APL-3007 + SYFOVRE; potential next generation treatment aimed at comprehensively blocking complement activity in the retina and choroid
Advancing our innovative pipeline and leveraging our complement expertise
Advancing investigational pre-clinical research for one-time neonatal Fc receptor (FcRn) treatment using gene editing technology from Beam Therapeutics
Business Update
Apellis and Sobi announced a capped royalty purchase agreement in July in which Apellis will receive up to $300 million in exchange for 90% of Apellis’ future ex-U.S. royalties for Aspaveli. Per the companies’ 2020 collaboration agreement, Apellis is eligible for tiered royalties on ex-U.S. sales of Aspaveli ranging from high teens to high twenties. Under the terms of the newly announced royalty purchase agreement, Sobi acquired 90% of Apellis’ ex-U.S. royalties for Aspaveli for $275 million in cash. Apellis is also eligible for up to $25 million in milestone payments upon EMA approval of Aspaveli for C3G and IC-MPGN. The agreement is subject to defined caps tied to Aspaveli’s performance. Sobi retains 90% of ex-U.S. royalties until these caps are achieved, after which 100% of all ex-U.S. royalties revert to Apellis.
Per the companies’ 2020 collaboration agreement, Apellis is eligible for tiered royalties on ex-U.S. sales of Aspaveli ranging from high teens to high twenties. Under the terms of the newly announced royalty purchase agreement, Sobi acquired 90% of Apellis’ ex-U.S. royalties for Aspaveli for $275 million in cash. Apellis is also eligible for up to $25 million in milestone payments upon EMA approval of Aspaveli for C3G and IC-MPGN. The agreement is subject to defined caps tied to Aspaveli’s performance. Sobi retains 90% of ex-U.S. royalties until these caps are achieved, after which 100% of all ex-U.S. royalties revert to Apellis.
Organizational Updates
Leslie Meltzer, Ph.D., has been named chief research and development officer, effective August 25. An experienced biopharmaceutical leader, she brings a proven track record of advancing programs from discovery through global approvals and commercialization. Most recently, Leslie served as chief medical officer at Orchard Therapeutics, where she led the company’s development functions and was instrumental in securing global regulatory approvals. She previously held senior roles at Keryx, Biogen, and Actelion Pharmaceuticals. Leslie holds a Ph.D. in neuroscience from Stanford University and a bachelor’s degree in biology and neuroscience from Brandeis University. Kelley Boucher recently joined Apellis as chief people officer, bringing more than 20 years of human resources experience across the biotechnology and medical device industries. Most recently, she served as chief human resources officer at Alnylam Pharmaceuticals, where she led the global HR organization during a period of significant growth and industry recognition. She previously held senior HR roles at Abiomed and Shire. Kelley holds a bachelor’s degree in government relations from Cornell University.
Second Quarter 2025 Financial Results
Total Revenue
Total revenue was $178.5 million for the second quarter of 2025, which consisted of $150.6 million of SYFOVRE U.S. net product revenue, $20.8 million of EMPAVELI U.S. net product revenue, and $7.1 million in licensing and other revenue associated with the Sobi collaboration. Total revenue was $199.7 million for the second quarter of 2024, which consisted of $154.6 million of SYFOVRE U.S. net product revenue, $24.5 million in EMPAVELI U.S. net product revenue, and $20.5 million in licensing and other revenue associated with the Sobi collaboration.
Cost of Sales
Cost of sales was $13.6 million for the second quarter 2025, compared to $23.1 million for the same period in 2024. The decrease in cost of sales was primarily driven by lower volumes of product supplied to Sobi and a decrease in expenses incurred related to excess, obsolete or scrapped inventory. The decreases were partially offset by higher volume from commercial sales and product provided under our patient assistance programs, as well as increased costs incurred in connection with cancellable purchase commitments.
R&D Expenses
R&D expenses were $67.0 million for the second quarter of 2025, compared to $78.0 million for the same period in 2024. The decrease in R&D expenses was primarily driven by lower program-specific and non-program-specific external costs, reduced compensation and related personnel costs, and lower other expenses.
Selling, General and Administrative (SG&A) Expenses
SG&A expenses were $131.1 million for the second quarter of 2025, compared to $128.1 million for the same period in 2024. The increase in SG&A was primarily driven by higher office and travel expenses, professional and consulting fees, factoring fees, and insurance expenses, partially offset by lower personnel costs.
Net Loss
Apellis reported a net loss of $42.2 million for the second quarter 2025, compared to a net loss of $37.7 million for the same period in 2024.
Cash
As of June 30, 2025, Apellis had $370.0 million in cash and cash equivalents, compared to $411.3 million in cash and cash equivalents as of December 31, 2024. Apellis anticipates its cash, combined with expected product revenues and funds from the Sobi royalty purchase agreement, will fund the business to profitability.
Conference Call and WebcastApellis will host a conference call and webcast to discuss its second quarter 2025 financial results and business highlights today, July 31, 2025, at 8:30 a.m. ET. To access the live call by phone, please pre-register for the call here. A live audio webcast of the event and accompanying slides may also be accessed through the “Events and Presentations” page of the “Investors and Media” section of the Company’s website. A replay of the webcast will be available for 90 days following the event.
About SYFOVRE® (pegcetacoplan injection)SYFOVRE® (pegcetacoplan injection) is the first-ever approved therapy for geographic atrophy (GA). By targeting C3, SYFOVRE is designed to provide comprehensive control of the complement cascade, part of the body’s immune system. SYFOVRE is approved in the United States and Australia.
About EMPAVELI®/Aspaveli® (pegcetacoplan)EMPAVELI®/Aspaveli® (pegcetacoplan) is a targeted C3 therapy designed to regulate excessive activation of the complement cascade, part of the body’s immune system, which can lead to the onset and progression of many serious diseases. It is approved for the treatment of C3 glomerulopathy (C3G) and primary immune complex membranoproliferative glomerulonephritis (IC-MPGN) in the United States and paroxysmal nocturnal hemoglobinuria (PNH) in the United States, European Union, and other countries globally. The therapy is also under investigation for other rare diseases.
About the Apellis and Sobi CollaborationApellis and Sobi have global co-development rights for systemic pegcetacoplan. Sobi has exclusive ex-U.S. commercialization rights for systemic pegcetacoplan, and its opt-in rights for future development programs are unchanged, exercisable at any time prior to commercialization. Apellis has exclusive U.S. commercialization rights for systemic pegcetacoplan and worldwide commercial rights for ophthalmological pegcetacoplan, including for geographic atrophy.
U.S. Important Safety Information for SYFOVRE® (pegcetacoplan injection)CONTRAINDICATIONS
SYFOVRE is contraindicated in patients with ocular or periocular infections, in patients with active intraocular inflammation, and in patients with hypersensitivity to pegcetacoplan or any of the excipients in SYFOVRE. Systemic hypersensitivity reactions (e.g., anaphylaxis, rash, urticaria) have occurred.
WARNINGS AND PRECAUTIONS
Endophthalmitis and Retinal Detachments Intravitreal injections, including those with SYFOVRE, may be associated with endophthalmitis and retinal detachments. Proper aseptic injection technique must always be used when administering SYFOVRE to minimize the risk of endophthalmitis. Patients should be instructed to report any symptoms suggestive of endophthalmitis or retinal detachment without delay and should be managed appropriately. Retinal Vasculitis and/or Retinal Vascular Occlusion Retinal vasculitis and/or retinal vascular occlusion, typically in the presence of intraocular inflammation, have been reported with the use of SYFOVRE. Cases may occur with the first dose of SYFOVRE and may result in severe vision loss. Discontinue treatment with SYFOVRE in patients who develop these events. Patients should be instructed to report any change in vision without delay. Neovascular AMD In clinical trials, use of SYFOVRE was associated with increased rates of neovascular (wet) AMD or choroidal neovascularization (12% when administered monthly, 7% when administered every other month and 3% in the control group) by Month 24. Patients receiving SYFOVRE should be monitored for signs of neovascular AMD. In case anti-Vascular Endothelial Growth Factor (anti-VEGF) is required, it should be given separately from SYFOVRE administration. Intraocular Inflammation In clinical trials, use of SYFOVRE was associated with episodes of intraocular inflammation including: vitritis, vitreal cells, iridocyclitis, uveitis, anterior chamber cells, iritis, and anterior chamber flare. After inflammation resolves, patients may resume treatment with SYFOVRE. Increased Intraocular Pressure Acute increase in IOP may occur within minutes of any intravitreal injection, including with SYFOVRE. Perfusion of the optic nerve head should be monitored following the injection and managed as needed.
Intravitreal injections, including those with SYFOVRE, may be associated with endophthalmitis and retinal detachments. Proper aseptic injection technique must always be used when administering SYFOVRE to minimize the risk of endophthalmitis. Patients should be instructed to report any symptoms suggestive of endophthalmitis or retinal detachment without delay and should be managed appropriately.
Retinal vasculitis and/or retinal vascular occlusion, typically in the presence of intraocular inflammation, have been reported with the use of SYFOVRE. Cases may occur with the first dose of SYFOVRE and may result in severe vision loss. Discontinue treatment with SYFOVRE in patients who develop these events. Patients should be instructed to report any change in vision without delay.
In clinical trials, use of SYFOVRE was associated with increased rates of neovascular (wet) AMD or choroidal neovascularization (12% when administered monthly, 7% when administered every other month and 3% in the control group) by Month 24. Patients receiving SYFOVRE should be monitored for signs of neovascular AMD. In case anti-Vascular Endothelial Growth Factor (anti-VEGF) is required, it should be given separately from SYFOVRE administration.
In clinical trials, use of SYFOVRE was associated with episodes of intraocular inflammation including: vitritis, vitreal cells, iridocyclitis, uveitis, anterior chamber cells, iritis, and anterior chamber flare. After inflammation resolves, patients may resume treatment with SYFOVRE.
Acute increase in IOP may occur within minutes of any intravitreal injection, including with SYFOVRE. Perfusion of the optic nerve head should be monitored following the injection and managed as needed.
ADVERSE REACTIONS
Most common adverse reactions (incidence ≥5%) are ocular discomfort, neovascular age-related macular degeneration, vitreous floaters, conjunctival hemorrhage.
Please see full Prescribing Information for more information.
U.S. Important Safety Information for EMPAVELI® (pegcetacoplan)
BOXED WARNING: SERIOUS INFECTIONS CAUSED BY ENCAPSULATED BACTERIAEMPAVELI, a complement inhibitor, increases the risk of serious infections, especially those caused by encapsulated bacteria, such as Streptococcus pneumoniae, Neisseria meningitidis, and Haemophilus influenzae type B. Life-threatening and fatal infections with encapsulated bacteria have occurred in patients treated with complement inhibitors. These infections may become rapidly life-threatening or fatal if not recognized and treated early.
Complete or update vaccination for encapsulated bacteria at least 2 weeks prior to the first dose of EMPAVELI, unless the risks of delaying therapy with EMPAVELI outweigh the risks of developing a serious infection. Comply with the most current Advisory Committee on Immunization Practices (ACIP) recommendations for vaccinations against encapsulated bacteria in patients receiving a complement inhibitor. Patients receiving EMPAVELI are at increased risk for invasive disease caused by encapsulated bacteria, even if they develop antibodies following vaccination. Monitor patients for early signs and symptoms of serious infections and evaluate immediately if infection is suspected.
Because of the risk of serious infections caused by encapsulated bacteria, EMPAVELI is available only through a restricted program under a Risk Evaluation and Mitigation Strategy (REMS) called the EMPAVELI REMS.
CONTRAINDICATIONS
Hypersensitivity to pegcetacoplan or to any of the excipients For initiation in patients with unresolved serious infection caused by encapsulated bacteria including Streptococcus pneumoniae, Neisseria meningitidis, and Haemophilus influenzae type B
WARNINGS AND PRECAUTIONS
Serious Infections Caused by Encapsulated Bacteria
EMPAVELI, a complement inhibitor, increases a patient’s susceptibility to serious, life-threatening, or fatal infections caused by encapsulated bacteria including Streptococcus pneumoniae, Neisseria meningitidis (caused by any serogroup, including non-groupable strains), and Haemophilus influenzae type B. Life-threatening and fatal infections with encapsulated bacteria have occurred in both vaccinated and unvaccinated patients treated with complement inhibitors. The initiation of EMPAVELI treatment is contraindicated in patients with unresolved serious infection caused by encapsulated bacteria.
Complete or update vaccination against encapsulated bacteria at least 2 weeks prior to administration of the first dose of EMPAVELI, according to the most current ACIP recommendations for patients receiving a complement inhibitor. Revaccinate patients in accordance with ACIP recommendations considering the duration of therapy with EMPAVELI. Note that ACIP recommends an administration schedule in patients receiving complement inhibitors that differs from the administration schedule in the vaccine prescribing information. If urgent EMPAVELI therapy is indicated in a patient who is not up to date with vaccines against encapsulated bacteria according to ACIP recommendations, provide the patient with antibacterial drug prophylaxis and administer these vaccines as soon as possible. The benefits and risks of treatment with EMPAVELI, as well as the benefits and risks of antibacterial drug prophylaxis in unvaccinated or vaccinated patients, must be considered against the known risks for serious infections caused by encapsulated bacteria.
Vaccination does not eliminate the risk of serious encapsulated bacterial infections, despite development of antibodies following vaccination. Closely monitor patients for early signs and symptoms of serious infection and evaluate patients immediately if an infection is suspected. Inform patients of these signs and symptoms and instruct patients to seek immediate medical care if these signs and symptoms occur. Promptly treat known infections. Serious infection may become rapidly life-threatening or fatal if not recognized and treated early. Consider interruption of EMPAVELI in patients who are undergoing treatment for serious infections.
EMPAVELI is available only through a restricted program under a REMS. EMPAVELI REMS
EMPAVELI is available only through a restricted program under a REMS called EMPAVELI REMS, because of the risk of serious infections caused by encapsulated bacteria. Notable requirements of the EMPAVELI REMS include the following:
Under the EMPAVELI REMS, prescribers must enroll in the program. Prescribers must counsel patients about the risks, signs, and symptoms of serious infections caused by encapsulated bacteria, provide patients with the REMS educational materials, ensure patients are vaccinated against encapsulated bacteria at least 2 weeks prior to the first dose of EMPAVELI, prescribe antibacterial drug prophylaxis if patients’ vaccine status is not up to date and treatment must be started urgently, and provide instructions to always carry the Patient Safety Card both during treatment, as well as for 2 months following last dose of EMPAVELI. Pharmacies that dispense EMPAVELI must be certified in the EMPAVELI REMS and must verify prescribers are certified.
Further information is available at www.empavelirems.com or 1-888-343-7073.
Infusion-Related Reactions
Systemic hypersensitivity reactions (eg, facial swelling, rash, urticaria, pyrexia) have occurred in patients treated with EMPAVELI, which may resolve after treatment with antihistamines. Cases of anaphylaxis leading to treatment discontinuation have been reported. If a severe hypersensitivity reaction (including anaphylaxis) occurs, discontinue EMPAVELI infusion immediately, institute appropriate treatment, per standard of care, and monitor until signs and symptoms are resolved.
Monitoring Paroxysmal Nocturnal Hemoglobinuria (PNH) Manifestations after Discontinuation of EMPAVELI
After discontinuing treatment with EMPAVELI, closely monitor for signs and symptoms of hemolysis, identified by elevated LDH levels along with sudden decrease in PNH clone size or hemoglobin, or reappearance of symptoms such as fatigue, hemoglobinuria, abdominal pain, dyspnea, major adverse vascular events (including thrombosis), dysphagia, or erectile dysfunction. Monitor any patient who discontinues EMPAVELI for at least 8 weeks to detect hemolysis and other reactions. If hemolysis, including elevated LDH, occurs after discontinuation of EMPAVELI, consider restarting treatment with EMPAVELI.
Interference with Laboratory Tests
There may be interference between silica reagents in coagulation panels and EMPAVELI that results in artificially prolonged activated partial thromboplastin time (aPTT); therefore, avoid the use of silica reagents in coagulation panels.
ADVERSE REACTIONS
Most common adverse reactions in adult patients with PNH (incidence ≥10%) were injection-site reactions, infections, diarrhea, abdominal pain, respiratory tract infection, pain in extremity, hypokalemia, fatigue, viral infection, cough, arthralgia, dizziness, headache, and rash.
Most common adverse reactions in adult and pediatric patients 12 years of age and older with C3 glomerulopathy (C3G) or primary immune-complex membranoproliferative glomerulonephritis (IC-MPGN) (incidence ≥10%) were injection-site reactions, pyrexia, nasopharyngitis, influenza, cough, and nausea.
USE IN SPECIFIC POPULATIONS
Females of Reproductive Potential
EMPAVELI may cause embryo-fetal harm when administered to pregnant women. Pregnancy testing is recommended for females of reproductive potential prior to treatment with EMPAVELI. Advise female patients of reproductive potential to use effective contraception during treatment with EMPAVELI and for 40 days after the last dose.
Please see full Prescribing Information, including Boxed WARNING regarding serious infections caused by encapsulated bacteria, and Medication Guide.
About Apellis Apellis Pharmaceuticals, Inc. is a global biopharmaceutical company leading the way in complement science to develop life-changing therapies for some of the most challenging diseases patients face. We ushered in the first new class of complement medicine in 15 years and now have two C3-targeting medicines approved to treat four serious diseases. Breakthroughs for patients include the first-ever therapy for geographic atrophy, a leading cause of blindness, and the first treatment for patients 12 and older with C3G or primary IC-MPGN, two severe, rare kidney diseases. We believe we have only begun to unlock the potential of targeting C3 across many serious diseases. For more information, please visit http://apellis.com or follow us on LinkedIn and X.
Apellis Forward-Looking StatementStatements in this press release about future expectations, plans and prospects, as well as any other statements regarding matters that are not historical facts, may constitute “forward-looking statements” within the meaning of The Private Securities Litigation Reform Act of 1995. The words “anticipate,” “believe,” “continue,” “could,” “estimate,” “expect,” “intend,” “may,” “plan,” “potential,” “predict,” “project,” “should,” “target,” “will,” “would” and similar expressions are intended to identify forward-looking statements, although not all forward-looking statements contain these identifying words. Actual results may differ materially from those indicated by such forward-looking statements as a result of various important factors, including whether the results of the Company’s clinical trials for EMPAVELI, SYFOVRE, or any of its future products will warrant regulatory submissions to the FDA or equivalent foreign regulatory agencies; whether systemic pegcetacoplan will receive approval from foreign regulatory agencies for C3G and primary IC-MPGN; rate and degree of market acceptance and clinical utility of EMPAVELI, SYFOVRE and any future products for which we receive marketing approval will impact our commercialization efforts; whether SYFOVRE will receive approval from foreign regulatory agencies for GA when expected or at all; whether the Company’s clinical trials will be completed when anticipated; whether results obtained in clinical trials will be indicative of results that will be generated in future clinical trials or in the real world setting; whether the period for which the Company believes that its cash resources will be sufficient to fund its operations; and other factors discussed in the “Risk Factors” section of Apellis’ Annual Report on Form 10-K with the Securities and Exchange Commission on February 28, 2025 and the risks described in other filings that Apellis may make with the Securities and Exchange Commission. Any forward-looking statements contained in this press release speak only as of the date hereof, and Apellis specifically disclaims any obligation to update any forward-looking statement, whether as a result of new information, future events or otherwise.
Media Contact:Tracy Vineismedia@apellis.com617.420.4839
Investor Contact:Neil Carnahan, CFAneil.carnahan@apellis.com617.977.5703
上市批准临床结果临床3期高管变更引进/卖出
2024-04-02
Mike Gray appointed as CFO and COO, Lisa Fiering joins as SVP, People & Culture
WALTHAM, Mass.--(BUSINESS WIRE)-- Upstream Bio, a clinical-stage biotech company advancing verekitug (UPB-101) for respiratory disorders, today announced strategic leadership changes including the appointment of Rand Sutherland, MD, as Chief Executive Officer. Upstream has also appointed Mike Gray as Chief Financial Officer and Chief Operating Officer, and Lisa Fiering as Senior Vice President of People & Culture. These leadership changes will support the growth and evolution of Upstream as the company works to advance verekitug, a recombinant fully human immunoglobulin G1 monoclonal antibody which blocks the thymic stromal lymphopoietin receptor (TLSPR), in ongoing Phase 2 clinical trials for severe asthma and chronic rhinosinusitis with nasal polyps (CRSwNP).
“I am thrilled to join Upstream Bio as CEO. I am committed to the company’s work to conquer inflammation at its source and intend to bring our team into the next stage of business and clinical operations,” said Dr. Sutherland. “Having dedicated much of my career to improving care for people living with asthma, I understand the substantial impact of severe respiratory diseases and I believe that verekitug could further improve standard of care for these patients. I am honored to lead this company at such an exciting time.”
“Upstream Bio is at a critical period as the company advances verekitug, a potentially best-in-class therapeutic in the field of TSLP biology,” said Ron Renaud, Chair of the Board of Directors for Upstream Bio. “I want to thank Samantha Truex for serving as Upstream Bio’s CEO from launch through the initiation of our Phase 2 studies and leading the company to this juncture. By evolving and building our leadership team with these additions, we are further positioning Upstream Bio to become a leader in the immunotherapy landscape. I am pleased to welcome Rand, Mike and Lisa to the Upstream Bio team.”
Dr. Sutherland joins Upstream Bio with more than 25 years of business and clinical experience, having most recently served as CEO of Seeker Biologics, and before that as President of Translate Bio prior to its acquisition by Sanofi. Previously, Dr. Sutherland held a number of R&D and medical affairs roles at Sanofi, providing leadership for the development of novel medicines in Immunology and Rare Diseases, and leading medical affairs globally for the Specialty Care business unit. Dr. Sutherland also serves as an independent director of Allakos, Krystal Biotech and Vanqua Bio. Before joining the biopharma industry, Dr. Sutherland was Professor of Medicine at the University of Colorado and Chief of Pulmonary and Critical Care Medicine at National Jewish Health in Denver. He earned an MD from the University of Chicago, after which he trained in Internal Medicine at UCSF and in Pulmonary and Critical Care Medicine at the University of Colorado.
Mr. Gray has more than 25 years of public-private leadership experience and was most recently the CFO and COO of Carmot Therapeutics, where he helped to secure the company’s acquisition by Roche in 2024. Before this, he was CFO and COO of Imara and Arsanis, working with the leadership teams of each company in completing initial public offerings and building leading organizations. Mr. Gray previously held a number of leadership positions at Curis. Mr. Gray served on the Board of Directors of Therapeutics Acquisition Corporation, a special purpose acquisition corporation, through its merger with POINT Biopharma, which was subsequently acquired by Eli Lilly and Company in March 2024. He received his BS in business administration (accounting) from Bryant College and an MBA in corporate finance and entrepreneurial management from the F.W. Olin Graduate School of Business at Babson College.
Ms. Fiering brings to Upstream 30 years of experience, having spent the past 20 years in various people and culture roles at life sciences companies including Genzyme, Ironwood Pharmaceuticals, Keryx and Trillium, where she developed a pragmatic approach to drive team effectiveness through talent and organizational development. Since 2022, she has provided strategic consulting to early-stage biotech companies, developing strategy and building the foundation for the people and culture function for these growing companies. Ms. Fiering earned her BA in Sociology from Ithaca College.
About Upstream Bio
Upstream Bio strives to reach the source of inflammation and conquer it, leveraging its team’s diverse industry experience to develop verekitug (UPB-101) to ease the burden of respiratory diseases. Verekitug is a clinical-stage monoclonal antibody that inhibits the TSLP receptor. TSLP is a validated target positioned upstream of multiple signaling cascades that affect a variety of immune cells pivotal to common and rare diseases. Upstream has completed a clinical trial in asthma with 32 weeks of observation which demonstrated compelling and sustained reductions in disease-related biomarkers and enabled the investigation of UPB-101 in ongoing Phase 2 trials of asthma and of CRSwNP that include extended dosing regimens of up to every 24 weeks.
View source version on businesswire.com:
Contacts
Source: Upstream Bio
View this news release online at:
临床2期高管变更IPO临床结果并购
2024-02-04
·赛柏蓝
作者 | 骎丹翼来源 | 药智网2024年,美国将有34款药物的关键专利到期,其中强生的重磅炸弹药物Xarelto(rivaroxaban)最值得关注。以下为笔者盘点的关键专利到期的药物信息,包含销售商、获批时间、适应症、销售额等数据。1.Auryxia(ferric citrate)销售商:Keryx Biopharmaceuticals,Inc.获批时间:2014年9月5日适应症和用途:控制透析患者的血清磷水平、未接受透析的成年慢性肾病患者的缺铁性贫血。关键专利到期时间:2024年2月18日药物专利数量:14销售额:预计2023年净产品收入1.75-1.8亿美元2.Spravato(esketamine hydrochloride)销售商:Janssen获批时间:2019年3月5日适应症和用途:患有难治性抑郁症(TRD)的成人、具有自杀想法或行为的重度抑郁症(MDD)成人的抑郁症状。关键专利到期时间:2024年3月5日药物专利数量:6销售额:2023年前三季度4.83亿美元3.Phexxi(citric acid;lactic acid;potassium bitartrate)销售商:Evofem获批时间:2020年5月22日适应症和用途:女性避孕。关键专利到期时间:2024年3月6日药物专利数量:4销售额:2022年1.68亿美元4.Exparel(bupivacaine)销售商:Pacira Pharms获批时间:2011年10月28日适应症和用途:长效酰胺类局麻药,用于术后镇痛。关键专利到期时间:2024年3月22日药物专利数量:9销售额:2023年净产品收入5.38亿美元5.Ionsys(fentanyl hydrochloride)销售商:The Medicines Co获批时间:2015年5月22日适应症和用途:芬太尼离子电渗透皮系统,用于对需要阿片类镇痛的住院成人进行急性术后疼痛的短期管理。关键专利到期时间:2024年4月1日药物专利数量:86.Contrave(bupropion hydrochloride;naltrexone hydrochloride)销售商:Nalpropion获批时间:2014年9月10日适应症和用途:一种氨基酮类抗抑郁药和阿片类拮抗剂的组合,可作为低热量饮食和增加体力活动的辅助手段,以实现长期体重管理。关键专利到期时间:2024年4月21日药物专利数量:207.Natroba(spinosad)销售商:Parapro获批时间:2011年1月18日适应症和用途:多种体外寄生虫适应症。关键专利到期时间:2024年4月28日药物专利数量:28.Rydapt(midostaurin)销售商:诺华获批时间:2017年4月28日适应症和用途:FLT3突变的急性髓系白血病和系统性肥大细胞增多症。关键专利到期时间:2024年4月28日药物专利数量:2销售额:2022年4.2亿美元9.Tralement(cupric sulfate;manganese sulfate;selenious acid;zinc sulfate)销售商:Am Regent获批时间:2020年7月2日适应症和用途:口服或肠内营养不可能、不足或禁忌时,作为肠外营养的锌、铜、锰和硒的来源。关键专利到期时间:2024年4月30日药物专利数量:110.Radicava(edaravone)销售商:Mitsubishi Tanabe获批时间:2017年5月5日适应症和用途:肌萎缩侧索硬化症(ALS)。关键专利到期时间:2024年5月5日药物专利数量:4销售额:2021财年1.9亿美元11.Omontys(peginesatide acetate)销售商:Takeda获批时间:2012年3月27日(已退市)适应症和用途:成人透析患者慢性肾病(CKD)所致贫血的治疗。关键专利到期时间:2024年5月12日药物专利数量:612.Ulesfia(benzyl alcohol)销售商:Shionogi获批时间:2009年4月13日适应症和用途:非神经毒性头虱。关键专利到期时间:2024年5月12日药物专利数量:613.Adasuve(loxapine)销售商:Alexza Pharmaceuticals获批时间:2012年12月21日适应症和用途:与精神分裂症或躁郁症相关的躁动。关键专利到期时间:2024年5月20日药物专利数量:514.Children's Advil Allergy Sinus销售商:葛兰素史克获批时间:2004年2月24日适应症和用途:由过敏或普通感冒引起的打喷嚏、瘙痒、流泪、流鼻涕、鼻塞、鼻窦充血、头痛、疼痛或发烧。关键专利到期时间:2024年5月25日药物专利数量:115.Gleolan(aminolevulinic acid hydrochloride)销售商:NX Development Corp.获批时间:2017年6月6日适应症和用途:神经胶质瘤手术期间的光学成像。关键专利到期时间:2024年6月6日16.Ilevro(nepafenac)销售商:Harrow Eye获批时间:2012年10月16日适应症和用途:缓解白内障眼部手术后的眼睛疼痛、刺激和发红。关键专利到期时间:2024年6月8日药物专利数量:317.Vyleesi(Autoinjector)(bremelanotide acetate)销售商:Palatin Technologies获批时间:2019年7月8日适应症和用途:性欲减退症。关键专利到期时间:2024年6月21日药物专利数量:518.Triptodur kit(triptorelin pamoate)销售商:Azurity获批时间:2017年6月30日适应症和用途:性早熟。关键专利到期时间:2024年7月29日药物专利数量:119.Endari(L-glutamine)销售商:Emmaus Medical获批时间:2017年7月7日适应症和用途:镰状细胞性贫血症。关键专利到期时间:2024年7月7日药物专利数量:1销售额:2023年前三季度2250万美元20.Dalvance(dalbavancin hydrochloride)销售商:艾伯维获批时间:2014年5月23日适应症和用途:由敏感革兰氏阳性菌(包括耐甲氧西林金黄色葡萄球菌(MRSA))引起的急性细菌性皮肤和皮肤结构感染(ABSSSI)的成人患者。关键专利到期时间:2024年7月22日药物专利数量:421.Kimyrsa(oritavancin diphosphate)销售商:艾伯维获批时间:2021年3月15日适应症和用途:成人急性细菌性皮肤和皮肤结构感染(ABSSSI)。关键专利到期时间:2024年8月6日药物专利数量:322.Orbactiv(oritavancin diphosphate)销售商:Melinta Therapeutics获批时间:2014年8月6日适应症和用途:急性细菌性皮肤和皮肤结构感染(ABSSSI)。关键专利到期时间:2024年8月6日药物专利数量:323.Oriahnn(Copackaged)销售商:艾伯维获批时间:2020年5月29日适应症和用途:绝经前妇女与子宫肌瘤(纤维瘤)相关的大量月经出血。关键专利到期时间:2024年9月10日药物专利数量:724.Orilissa(elagolix sodium)销售商:艾伯维获批时间:2018年7月24日适应症和用途:与子宫内膜异位症相关的中度至重度疼痛。关键专利到期时间:2024年9月10日药物专利数量:1025.Somatuline Depot(lanreotide acetate)销售商:Ipsen获批时间:2014年12月16日适应症和用途:胃肠胰神经内分泌肿瘤。关键专利到期时间:2024年9月15日26.Sustol(granisetron)销售商:Heron Therapeutics获批时间:2016年8月9日适应症和用途:化疗引起的恶心/呕吐。关键专利到期时间:2024年9月28日药物专利数量:5销售额:2023年前三季度净产品销售额930万美元27.Prialt(ziconotide acetate)销售商:TerSera获批时间:2004年12月28日适应症和用途:治疗需要鞘内治疗以及对其他治疗(例如全身镇痛药、辅助治疗或IT吗啡)不耐受或无效的患者的严重慢性疼痛。关键专利到期时间:2024年10月1日药物专利数量:328.Ascor(ascorbic acid)销售商:Mcguff获批时间:2017年13月3日适应症和用途:坏血病。关键专利到期时间:2024年10月2日29.Fluorodopa F18(fluorodopa f-18)销售商:Feinstein获批时间:2019年10月10日适应症和用途:对疑似帕金森综合症的成年患者的某些神经细胞进行视觉检测。关键专利到期时间:2024年10月10日30.Byetta(exenatide synthetic)销售商:Amylin Pharmaceuticals/Eli Lilly&Co.获批时间:2005年4月28日适应症和用途:2型糖尿病。关键专利到期时间:2024年11月4日销售额:2019年1.8亿美元31.Exem Foam Kit(air polymer-type a)销售商:ExEm Foam Inc.获批时间:2019年11月7日适应症和用途:检测已知或疑似不孕女性的输卵管通畅性。关键专利到期时间:2024年11月7日32.Nourianz(istradefylline)销售商:Kyowa Hakko Kirin Inc.获批时间:2019年8月27日适应症和用途:帕金森病。关键专利到期时间:2024年11月13日药物专利数量:4销售额:2021年1亿美元33.Macrilen(macimorelin acetate)销售商:诺和诺德获批时间:2017年12月20日适应症和用途:成人生长激素缺乏症的诊断。关键专利到期时间:2024年12月20日药物专利数量:134.Xarelto(rivaroxaban)销售商:Janssen获批时间:2011年7月1日适应症和用途:抗血栓。关键专利到期时间:2024年12月20日药物专利数量:5销售额:2022年24.7亿美元Ref.1.Constantino,A.K.Big pharma is at a crossroads,as J&J,Merck and others prepare to lose heaps of revenue from blockbuster drugs.CNBC.28.01.2024.2.Friedman,Y.United States:These 47 Drugs Face Patent Expirations and Generic Entry From 2024–2025.DrugPatentWatch.com.Retrieved on 31.01.2024.END医药代表交流群扫描下方二维码加入医药代理商转型交流群扫描下方二维码加入
专利到期
100 项与 Keryx Biopharmaceuticals, Inc. 相关的药物交易
登录后查看更多信息
100 项与 Keryx Biopharmaceuticals, Inc. 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2025年09月30日管线快照
管线布局中药物为当前组织机构及其子机构作为药物机构进行统计,早期临床1期并入临床1期,临床1/2期并入临床2期,临床2/3期并入临床3期
批准上市
1
18
其他
登录后查看更多信息
当前项目
| 药物(靶点) | 适应症 | 全球最高研发状态 |
|---|---|---|
枸橼酸铁 ( Phosphates ) | 缺铁性贫血 更多 | 批准上市 |
Erucylphosphocholine | 肿瘤 更多 | 终止 |
Anhydrovinblastine ( Tubulin ) | 肿瘤 更多 | 终止 |
舒洛地特 ( AT III ) | 2型糖尿病 更多 | 无进展 |
苄基鸟嘌呤 ( MGMT ) | 多形性胶质母细胞瘤 更多 | 无进展 |
登录后查看更多信息
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
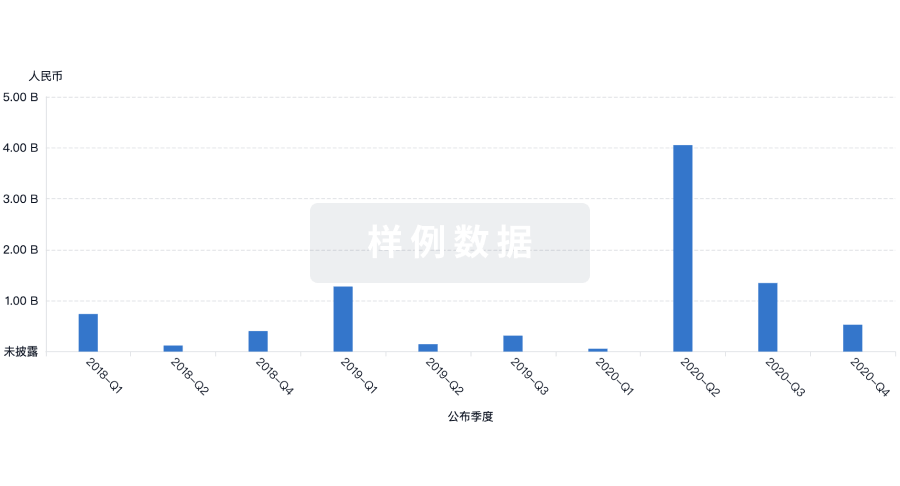
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
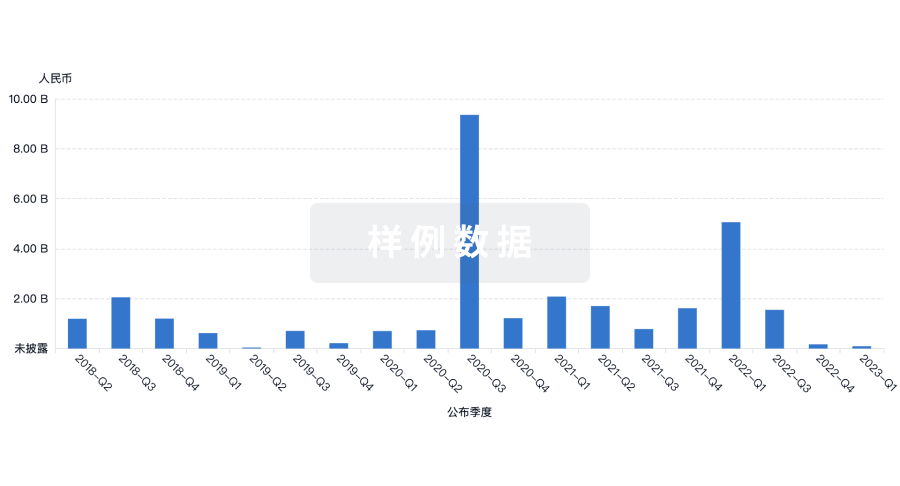
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
Eureka LS:
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用