预约演示
更新于:2025-05-07
PDE4B
更新于:2025-05-07
基本信息
别名 cAMP-specific 3',5'-cyclic phosphodiesterase 4B、DPDE4、PDE IVB + [7] |
简介 Hydrolyzes the second messenger cAMP, which is a key regulator of many important physiological processes (PubMed:15260978). May be involved in mediating central nervous system effects of therapeutic agents ranging from antidepressants to antiasthmatic and anti-inflammatory agents. |
关联
28
项与 PDE4B 相关的药物靶点 |
作用机制 PDE4B抑制剂 |
在研适应症 |
最高研发阶段批准上市 |
首次获批国家/地区 日本 |
首次获批日期2021-09-27 |
作用机制 A1R拮抗剂 [+2] |
在研机构 |
原研机构 |
在研适应症 |
非在研适应症- |
最高研发阶段批准上市 |
首次获批国家/地区- |
首次获批日期1800-01-20 |
183
项与 PDE4B 相关的临床试验NCT06806592
A Double Blind, Randomised, Placebo-controlled Trial Evaluating the Efficacy and Safety of Nerandomilast Over 26 Weeks in Patients With Systemic Autoimmune Rheumatic Diseases Associated Interstitial Lung Diseases (SARD-ILD)
Adults 18 years of age and older or above legal age with lung fibrosis related to systemic autoimmune rheumatic disease can participate in this study. People can only take part if they show no improvement in lung function after standard treatment with immunosuppressant medicine. The main purpose of this study is to find out how a medicine called nerandomilast affects the lungs in people with systemic autoimmune rheumatic disease.
Participants are put into 2 groups randomly, which means by chance. One group takes nerandomilast tablets and the other group takes placebo tablets. Placebo tablets look like nerandomilast tablets but do not contain any medicine. Participants take a tablet 2 times a day for 26 weeks. Participants continue immunosuppressant treatment for their underlying rheumatic disease.
Participants are in the study for about 7.5 months. During this time, they visit the study site 8 times. At study visits, participants have lung function tests. At select visits, chest imaging is performed. Participants fill in questionnaires about their symptoms and quality of life. The results between the 2 groups are compared to see whether the treatment works. The doctors also regularly check participants' health and take note of any unwanted effects.
Participants are put into 2 groups randomly, which means by chance. One group takes nerandomilast tablets and the other group takes placebo tablets. Placebo tablets look like nerandomilast tablets but do not contain any medicine. Participants take a tablet 2 times a day for 26 weeks. Participants continue immunosuppressant treatment for their underlying rheumatic disease.
Participants are in the study for about 7.5 months. During this time, they visit the study site 8 times. At study visits, participants have lung function tests. At select visits, chest imaging is performed. Participants fill in questionnaires about their symptoms and quality of life. The results between the 2 groups are compared to see whether the treatment works. The doctors also regularly check participants' health and take note of any unwanted effects.
开始日期2025-07-10 |
申办/合作机构 |
NCT06922669
Efficacy and Safety of Glucocorticoids for Acute Drug Induced Liver Injury With Hyperbilirubinemia: A Multicenter Randomized Controlled Trial
Drug-induced liver injury (DILI) can lead to potentially fatal complications, such as acute liver failure and even death. In clinical practice, glucocorticoids have been considered in some cases of DILI, especially patients with hyperbilirubinemia. However, the available evidence remains controversial and its quality is also very limited. Herein, a multicenter randomized controlled trial (RCT) has been designed to explore the efficacy and safety of glucocorticoids in patients with acute DILI and hyperbilirubinemia.
开始日期2025-06-01 |
申办/合作机构 |
NCT06241560
An Open-label, Single-group Trial to Evaluate the Effect of Pirfenidone on the Pharmacokinetics of a Single Oral Dose of BI 1015550
This study is open to adults with idiopathic pulmonary fibrosis (IPF) who are 40 years and older. The purpose of this study is to find out whether a medicine called pirfenidone changes the amount of a medicine called BI 1015550 in the blood. Some people may take more than one medicine at a time. Therefore, it is important to understand how different medicines influence one another.
Participants take one dose of BI 1015550 as a tablet. Participants then take one tablet of pirfenidone 3 times a day for one week. The dose is then increased to 2 tablets 3 times a day for the second week. In the third week the dose is increased further to 3 tablets 3 times a day. Participants then take another dose of BI 1015550 as a tablet.
Participants are in the study for a little over 1 month. During this time, they visit the study site 15 times. Two of the visits include overnight stays at the study site. The study staff also contacts the participants by phone. During the visits, the doctors collect information about participants' health and take blood samples from the participants. They compare the amount of pirfenidone and BI 1015550 in the blood. Doctors also regularly check participants' health and take note of any unwanted effects.
Participants take one dose of BI 1015550 as a tablet. Participants then take one tablet of pirfenidone 3 times a day for one week. The dose is then increased to 2 tablets 3 times a day for the second week. In the third week the dose is increased further to 3 tablets 3 times a day. Participants then take another dose of BI 1015550 as a tablet.
Participants are in the study for a little over 1 month. During this time, they visit the study site 15 times. Two of the visits include overnight stays at the study site. The study staff also contacts the participants by phone. During the visits, the doctors collect information about participants' health and take blood samples from the participants. They compare the amount of pirfenidone and BI 1015550 in the blood. Doctors also regularly check participants' health and take note of any unwanted effects.
开始日期2025-04-30 |
申办/合作机构 |
100 项与 PDE4B 相关的临床结果
登录后查看更多信息
100 项与 PDE4B 相关的转化医学
登录后查看更多信息
0 项与 PDE4B 相关的专利(医药)
登录后查看更多信息
663
项与 PDE4B 相关的文献(医药)2025-12-01·Lung
PDE4B Modulates Phosphorylation of p65 (Ser468) via cAMP/PKA in Acute Lung Injury
Article
作者: Dhar, Rana ; Wang, Xuefeng ; Ji, Jie ; Song, Shunde ; Li, Yajun ; Zhang, Zhewen ; Zheng, Xuyang ; Yan, Chunguang ; Li, Zigang ; Hu, Zhengqiang ; Tang, Huifang
2025-06-01·Translational Oncology
Knockdown TNF family prognosis index crucial gene PDE4B promoted PANoptosis of ovarian carcinoma cell:Based in vitro and in vivo experiments
Article
作者: Wang, Yunxiao ; Xu, Yongle ; Han, Dongyu ; Fu, Ting ; Yu, Qianqian ; Zhao, Lin ; Wang, Linlin
2025-05-01·Neurochemistry International
Temporal and spatial expression of Phosphodiesterase-4B after sciatic nerve compression in rats and its mechanism of action on sciatic nerve repair
Article
作者: Wang, Yufei ; Sun, Xuehua ; Zhou, Youfei ; Liu, Jinhao ; Li, Zirui ; Liu, Chen
112
项与 PDE4B 相关的新闻(医药)2025-04-29
·医药笔记
▎Armstrong2025年4月28日,NMPA网站公示信息显示,英矽智能特发性肺纤维化新药INS018-055拟纳入突破性治疗药物程序。INS018-055为英矽智能的核心管线,用于治疗特发性肺纤维化,在中美同步推进临床试验。2024年11月12日,英矽智能公布了ISM001-055治疗特发性肺纤维化患者群体中的IIa期临床数据,在安全性、耐受性,以及多个指标评估的药效方面均表现良好。这项针对ISM001-055开展的IIa期临床研究(NCT05938920)是一项持续12周的随机、双盲、安慰剂对照试验,在中国21个临床研究中心招募了71名IPF患者,分为30mg QD、30mg BID、60mg QD和安慰剂对照共四组,以安全性和耐受性评估为主要终点。根据英矽智能此次公布的顶线数据,ISM001-055在各剂量组均体现出良好的耐受性,与药物相关的不良事件(TEAE)大多为1级或2级,其中以腹泻(14.8%)和肝功能异常(14.8%)最为常见。考虑到上述不良反应常见于现有IPF药物,且患者经常因为副作用降低剂量或者停药,这样的安全性数据足以显示候选药物潜力。在PK-PD方面,ISM001-055在IPF患者中的半衰期为7-12小时,和部分现有药物类似,支持BID和QD给药。药代动力学(PK)曲线与在健康受试者中进行的I期研究结果一致,暴露量随剂量提升。在作为此次临床试验次要终点的药效方面,ISM001-055也有令人惊喜的表现。与基线水平相比,60mg QD组用力肺活量(FVC)平均提升98.4ml,该数据在安慰剂组的水平是-62.3ml,差距明显。再看预测用力肺活量百分比(ppFVC),该指标表征受试者与相同性别、年龄、身高普通人相比的肺活量水平,可以消除部分个体差异,提供更客观的肺功能评估。同样在60mg QD组,ppFVC与基线水平相比,平均提高3.05%,而安慰剂组ppFVC 与基线水平相比,平均下降1.84%。此外,患者生活质量(QoL)和功能性指标的改善也通过莱斯特咳嗽问卷(LCQ)从第0周到第12周的变化进行评估,60mg QD组对比安慰剂组,LCQ总分提高2分,被认为具有临床意义。在30mg QD、30mg BID组则没有显示出有意义的改善。整体而言,ISM001-055在仅12周用药后获得的剂量依赖性药效趋势意味着强大的治疗潜力,不仅有望延缓肺部纤维化发展,甚至提供了逆转病程的可能性,或将带来IPF治疗领域前所未有的突破,后续大规模、长周期的临床试验验证结果值得期待。总结今年2月,勃林格殷格翰宣布PDE4B抑制剂Nerandomilast治疗特发性肺纤维化的第二项三期临床FIBRONEER-ILD达到主要终点,将递交上市申请。尽管如此,IPF领域仍然存在严重的未满足临床需求,亟需更多治疗选择。INS018-055不仅仅是IPF领域的又一颗潜力新星,也代表了AI制药领域的重要进展,期待其后续更多临床进展。Armstrong技术全梳理系列GPRC5D靶点全梳理;CD40靶点全梳理;CD47靶点全梳理;补体靶向药物技术全梳理;补体药物:眼科治疗的重要方向;Claudin 6靶点全梳理;Claudin 18.2靶点全梳理;靶点冷暖,行业自知;中国大分子新药研发格局;被炮轰的“me too”;佐剂百年史;胰岛素百年传奇;CUSBEA:风雨四十载;中国新药研发的焦虑;中国生物医药企业的研发竞争;中国双抗竞争格局;中国ADC竞争格局;中国双抗技术全梳理;中国ADC技术全梳理;Ambrx技术全梳理;Vir Biotech技术全梳理;Immune-Onc技术全梳理;亘喜生物技术全梳理;康哲药业技术全梳理;科济药业技术全梳理;恺佧生物技术全梳理;同宜医药技术全梳理;百奥赛图技术全梳理;腾盛博药技术全梳理;创胜集团技术全梳理;永泰生物技术全梳理;中国抗体技术全梳理;德琪医药技术全梳理;德琪医药技术全梳理2.0;和铂医药技术全梳理;荣昌生物技术全梳理;再鼎医药技术全梳理;药明生物技术全梳理;恒瑞医药技术全梳理;豪森药业技术全梳理;正大天晴技术全梳理;吉凯基因技术全梳理;基石药业技术全梳理;百济神州技术全梳理;百济神州技术全梳理第2版;信达生物技术全梳理;信达生物技术全梳理第2版;中山康方技术全梳理;复宏汉霖技术全梳理;先声药业技术全梳理;君实生物技术全梳理;嘉和生物技术全梳理;志道生物技术全梳理;道尔生物技术全梳理;尚健生物技术全梳理;康宁杰瑞技术全梳理;科望医药技术全梳理;岸迈生物技术全梳理;礼进生物技术全梳理;康桥资本技术全梳理;余国良的抗体药布局;荃信生物技术全梳理;安源医药技术全梳理;三生国健技术全梳理;仁会生物技术全梳理;乐普生物技术全梳理;同润生物技术全梳理;宜明昂科技术全梳理;派格生物技术全梳理;迈威生物技术全梳理;Momenta技术全梳理;NGM技术全梳理;普米斯生物技术全梳理;普米斯生物技术全梳理2.0;三叶草生物技术全梳理;贝达药业抗体药全梳理;泽璟制药抗体药全梳理;恒瑞医药抗体药全梳理;齐鲁制药抗体药全梳理;石药集团抗体药全梳理;豪森药业抗体药全梳理;华海药业抗体药全梳理;科伦药业抗体药全梳理;百奥泰技术全梳理;凡恩世技术全梳理。
临床2期临床结果临床3期临床1期突破性疗法
2025-04-25
·米内网
精彩内容3款1类新药陆续实现商业化后,创新药已然成为海思科业绩新的增长点。2024年公司营收37.2亿元(+10.92%),归母净利润3.95亿元(+34%)。海思科以“创新”为内核,2024年研发投入超过10亿元,目前有24款新药(22款1类新药)处于申请临床及以上阶段,7个品种以新注册分类报产在审。营收净利双增!麻醉新药收入大涨46%海思科成立于2000年,目前拥有40余个品种的生产批文,覆盖麻醉镇痛、神经系统、内分泌系统、肠外营养、肿瘤止吐等多个细分领域,包括环泊酚注射液(1类新药)、苯磺酸克利加巴林胶囊(1类新药)、考格列汀片(1类新药)、甲磺酸多拉司琼注射液、复方氨基酸(18AA)/葡萄糖(15%)电解质注射液等多个独家品种(含独家剂型)。4月12日,海思科公布2024年业绩报告,报告期内公司实现营业收入37.2亿元,同比增长10.92%;归属于上市公司股东的净利润3.95亿元,同比增长34%。此外,公司拟向全体股东每10股派发现金红利1.35元(含税)。从分产品来看,自产产品收入与合作产品相关收入是海思科业绩的两大支柱,2024年营业收入分别达26.29亿元、9.43亿元,占总营收比重分别为70.67%、25.34%。2024年海思科分产品收入情况来源:公司公告,米内网整理自产产品中,麻醉产品收入12.32亿元,同比增长44.96%,占总营收比重33.1%;肠外营养系产品收入5.12亿元,占总营收比重13.76%;肿瘤止吐产品收入3.05亿元,同比增长44.26%,占总营收比重8.2%。从具体品种看,创新药成为海思科业绩新增长点:1类新药环泊酚注射液收入同比增长45.6%。目前该药已有3个适应症获批上市,且均已通过谈判纳入国家医保目录。此外,苯磺酸克利加巴林胶囊、考格列汀片上市第一年销售收入达数千万元,预计2025年将成为公司业绩增长的主力军。海思科于2012年开始自建创新药团队进行创新转型。近年来,公司以“创新”为内核,持续加大研发投入与研发力度,立志做全球化差异化创新药。2024年海思科研发投入超过10亿元,同比增长14.36%,占营收比重达到26.9%。截至报告期末,海思科在研制剂项目51个,其中创新药26个,改良型新药3个,仿制药22个(上市前19个,上市后3个),主要涉及治疗领域有:电解质、酸碱平衡及营养、扩容药12个、神经系统疾病药物5个、抗肿瘤药物7个、肾脏/泌尿系统疾病药物3个、呼吸系统疾病及抗过敏药物10个、皮肤及五官科药物6个、镇痛药及麻醉科药物2个、消化系统疾病药物3个、其它系统3个。22款1类新药出击,猛攻2大千亿市场2025年以来,海思科新药研发进展不断:HSK41959片、HSK39004吸入粉雾剂、HSK44459片获批临床,其中HSK41959片、HSK39004吸入粉雾剂均为首次获批,且前者已启动I期临床,后者已启动II期临床。据不完全统计,目前海思科在国内有24款新药(22款1类新药)处于申请临床及以上阶段,均为小分子化学药,涉及THR-β、BTK、EGFR、DDP1、PDE4B、USP1等疾病靶点,聚焦抗肿瘤和免疫调节剂、呼吸系统用药、神经系统药物三大治疗领域。海思科国内在研新药来源:米内网综合数据库米内网数据显示,2023年中国三大终端六大市场(统计范围详见本文末),抗肿瘤和免疫调节剂(化学药+生物药)、神经系统药物(化学药+生物药)市场规模分别超过2200亿元、1000亿元。抗肿瘤和免疫调节剂聚焦前列腺癌、非小细胞肺癌等细分病种,其中高选择性USP1抑制剂HSK39775片已步入I/II期临床,目前全球暂无同靶点药物获批,海思科处于研发第一梯队;处于I期临床的HSK40118片、HSK29116散均为口服Protac小分子药物,分别靶向EGFR、BTK,目前国内外均尚无同类产品进入临床,有望成为“first-in-class”药物。在呼吸系统领域,2类改良型新药HL231吸入溶液、1类新药HSK31858片均步入III期临床,上市可期。其中,HSK31858是一款口服、强效和高选择性的二肽基肽酶1(DPP1)抑制剂,目前全球尚无同靶点药物获批上市,在研药物中,海思科的HSK31858国内进展最快。神经系统药物聚焦麻醉镇痛细分领域,环泊酚注射液、苯磺酸克利加巴林胶囊已获批上市,HSK21542注射液已提交NDA,适应症包括术后镇痛、尿毒症瘙痒等。31个品种过评,3个品种备战第11批集采在仿制药方面,海思科立足于高端技术平台开发高壁垒仿制药,如多腔袋、口服缓控释、吸入剂等。目前公司有31个品种过评(14个为首家/独家),涵盖9个治疗大类,集中在血液和造血系统药物(9个)、全身用抗感染药物(6个)、消化系统及代谢药(5个)、神经系统药物(5个)等治疗领域。海思科已过评品种来源:米内网一致性评价进度数据库14个过评品种暂未纳入国采,中/长链脂肪乳注射液(C6~24)、利丙双卡因乳膏、富马酸卢帕他定片已满足入围门槛,符合申报资格企业数均达7家以上。其中,中/长链脂肪乳注射液(C6~24)在2023年中国公立医疗机构终端的销售额超过6亿元。品种申报方面,2023年至今,海思科有7个新分类报产品种在审,涵盖血液和造血系统药物、消化系统及代谢药两大治疗领域。2023年以来海思科新分类报产且在审的品种来源:米内网中国申报进度(MED)数据库目前国内有3家企业拥有注射用多种维生素(12)生产批文,该产品2023年在中国三大终端六大市场的销售额超过20亿元;中长链脂肪乳/氨基酸(16)/葡萄糖(36%)注射液目前仅1家企业拥有生产批文,2024上半年在中国三大终端六大市场的销售额增速超过700%。资料来源:米内网数据库、公司公告等注:米内网《中国三大终端六大市场药品竞争格局》,统计范围是:城市公立医院和县级公立医院、城市社区中心和乡镇卫生院、城市实体药店和网上药店,不含民营医院、私人诊所、村卫生室,不含县乡村药店;上述销售额以产品在终端的平均零售价计算。数据统计截至4月24日,如有疏漏,欢迎指正!免责声明:本文仅作医药信息传播分享,并不构成投资或决策建议。本文为原创稿件,转载文章或引用数据请注明来源和作者,否则将追究侵权责任。投稿及报料请发邮件到872470254@qq.com稿件要求详询米内微信首页菜单栏商务及内容合作可联系QQ:412539092【分享、点赞、在看】点一点不失联哦
财报申请上市医药出海
2025-04-13
·药明康德
▎药明康德内容团队编辑本期看点1. Solu Therapeutics公司创新细胞毒性靶向嵌合体(CyTAC)药物STX-0712的1期临床试验已完成首例患者给药。该类疗法能够靶向传统疗法难以作用的细胞表面蛋白。2. 用于治疗复发性生殖器疱疹的长效解旋酶-引物酶抑制剂ABI-5366的1a期临床试验数据积极,约20天的半衰期有望实现每周一次或每月一次的口服给药方案。药明康德内容团队整理STX-0712:1期临床试验完成首例患者给药Solu Therapeutics公司宣布完成4100万美元的A轮融资,所得资金将用于推进其核心项目STX-0712的临床评估、拓展其他管线,以及探索其细胞毒性靶向嵌合体和治疗指数控制靶向嵌合体(TicTAC)平台的新应用。该公司还宣布启动了STX-0712用于治疗耐药/难治性慢性粒单核细胞白血病(CMML)和其他血液系统恶性肿瘤的1期临床试验,首位患者已开始给药。Solu Therapeutics公司通过以独特的方式将强效、选择性小分子与效应抗体连接起来,能够靶向传统疗法难以作用的细胞表面蛋白(如G蛋白偶联受体和离子通道)。其双功能小分子的一只臂可特异性进入细胞表面蛋白中的深结合口袋,另一臂通过专有连接子技术与其专有的抗体连接,可增强效应抗体的疗效。STX-0712是一种CyTAC药物,通过靶向G蛋白偶联受体CCR2(在恶性单核细胞中高表达),能够清除CCR2阳性细胞,同时减少对正常细胞的影响,有望为耐药/难治性血液肿瘤提供更精准、有效的治疗选择。临床前数据显示,STX-0712对CMML患者样本中的CCR2阳性单核细胞具有强大的离体活性。ABI-5366:公布1a期临床试验的中期数据Assembly Biosciences公司公布了一种用于复发性生殖器疱疹的长效解旋酶-引物酶抑制剂ABI-5366的1a期临床试验数据。该候选疗法通过靶向病毒解旋酶-引物酶复合体发挥作用。这是一种在HSV-1和HSV-2中都保守的重要病毒酶复合体,并且宿主细胞中没有类似的酶复合体。在短期临床研究中,HSV解旋酶-引物酶抑制剂显示出比核苷类似物更佳的疗效潜力。此次公布的结果显示,ABI-5366在口服剂量高达350毫克时耐受性良好,未报告3级或4级治疗相关实验室异常或严重不良事件。此外,在所有剂量组中观察到ABI-5366的半衰期约为20天,有望实现每周一次或每月一次的口服给药方案。CVN293:公布1期临床试验数据Cerevance公司公布了其钾双孔结构域通道亚家族K成员13(KCNK13)抑制剂CVN293的积极1期临床试验结果。CVN293是一种高选择性口服KCNK13抑制剂,旨在通过抑制神经炎症减缓神经退行性疾病进展。KCNK13是一种潜在的NLRP3炎性小体激活的新型调节因子,该靶点由Cerevance公司专有的NETSseq平台发现。此次公布的研究结果显示,接受CVN293单次和14天内多次给药的健康成人对该药物的耐受性良好,100%的受试者完成了试验,未出现剂量限制性毒性、治疗相关停药或具临床意义的生命体征异常,所有不良事件均为轻度。CVN293还显示出强大的脑渗透性,支持KCNK13抑制剂对以神经炎症为特征的神经退行性疾病的效用。PALI-2108:1a期临床试验完成受试者给药Palisade Bio公司宣布,其用于治疗溃疡性结肠炎(UC)的在研药物PALI-2108已完成1a期临床试验,预计将于2025年5月底公布顶线数据。在UC和纤维狭窄型克罗恩病(FSCD)中,较高的PDE4B表达与局部炎症活动有关。PALI-2108是一种PDE4抑制剂前药,能在UC和FSCD等疾病部位局部活化,显著提升病变组织内PDE4抑制剂浓度,同时减少全身暴露,从而降低腹泻等传统PDE4抑制剂的副作用。初步结果显示,迄今为止未观察到与实验室检查或心电图相关的严重不良事件或治疗伴发不良事件。在临床前研究中,与其他PDE4抑制剂相比,PALI-2108对PDE4 B和D有很强的抑制作用。这些结果表明,在剂量相当的情况下,PALI-2108具有极佳的耐受性。ALX2004:IND申请获得FDA许可ALX Oncology公司宣布,其针对EGFR表达实体瘤的潜在“best-in-class”及“first-in-class”抗体偶联药物(ADC)ALX2004的IND申请已获FDA批准,计划于2025年中期启动单剂量递增及扩展的1期临床试验。ALX2004是通过该公司专有的拓扑异构酶I抑制剂有效载荷平台设计的,由三部分组成,分别是经优化的抗EGFR抗体骨架、稳定性增强的连接子,以及能产生强旁观者效应的专有拓扑异构酶I载荷,旨在克服早期EGFR靶向ADC因药物设计、脱靶毒性及传统载荷局限性导致的临床瓶颈。CVHNLC:IND申请获得FDA许可CureVac公司宣布,美国FDA已批准其基于mRNA的精准免疫疗法CVHNLC的IND申请,可启动针对鳞状非小细胞肺癌(sqNSCLC)患者的1期研究。CVHNLC由两种编码8种在sqNSCLC中常见的肿瘤相关抗原(TAA)的mRNA构建体组成,其中4种为已知的实体瘤相关抗原,另4种为CureVac专有发现平台鉴定的新TAA。该疗法采用第二代mRNA骨架,使用未修饰的mRNA封装于脂质纳米颗粒(LNP)中。该公司计划将CVHNLC与免疫检查点抑制剂pembrolizumab联用进行临床试验,旨在放大靶向抗肿瘤免疫反应。参考资料(可上下滑动查看)[1] IDEAYA Biosciences Announces Phase 1/2 Expansion for IDE397 and Trodelvy® Combination in MTAP-Deletion Urothelial Cancer. Retrieved April 12, 2025, from https://www.prnewswire.com/news-releases/ideaya-biosciences-announces-phase-12-expansion-for-ide397-and-trodelvy-combination-in-mtap-deletion-urothelial-cancer-302425193.html[2] ALX Oncology Receives IND Clearance from U.S. FDA for ALX2004, a Novel EGFR-targeted Antibody-drug Conjugate. Retrieved April 12, 2025, from https://ir.alxoncology.com/news-releases/news-release-details/alx-oncology-receives-ind-clearance-us-fda-alx2004-novel-egfr[3] CureVac Receives U.S. FDA IND Clearance to Initiate Phase 1 Clinical Trial for Novel mRNA-Based Precision Immunotherapy in Squamous Non-Small Cell Lung Cancer. Retrieved April 12, 2025, from https://www.curevac.com/en/curevac-receives-u-s-fda-ind-clearance-to-initiate-phase-1-clinical-trial-for-novel-mrna-based-precision-immunotherapy-in-squamous-non-small-cell-lung-cancer/[4] NKGen Biotech Presents Data from Phase 1/2a Clinical Trial of Troculeucel in Moderate Alzheimer’s Disease at the International Conference on Alzheimer’s and Parkinson’s Diseases (AD/PD™ 2025). Retrieved April 12, 2025, from https://nkgenbiotech.com/nkgen-biotech-presents-data-from-phase-1-2a-clinical-trial-of-troculeucel-in-moderate-alzheimers-disease-at-the-international-conference-on-alzheimers-and-parkinsons-disease/[5] Lexeo Therapeutics Announces Positive Interim Phase 1/2 Data for LX2006 in Friedreich Ataxia Cardiomyopathy Supporting Advancement to Registrational Study. Retrieved April 12, 2025, from https://www.globenewswire.com/news-release/2025/04/07/3056510/0/en/Lexeo-Therapeutics-Announces-Positive-Interim-Phase-1-2-Data-for-LX2006-in-Friedreich-Ataxia-Cardiomyopathy-Supporting-Advancement-to-Registrational-Study.html[6] Palisade Bio Completes Dosing in Phase 1a Portion of Ongoing Phase 1a/b Study of PALI-2108. Retrieved April 12, 2025, from https://palisadebio.com/palisade-bio-completes-dosing-in-phase-1a-portion-of-ongoing-phase-1a-b-study-of-pali-2108/[7] SciTech Development Announces 2nd FDA Approval of a Phase 1 a/b IND For ST-001. New IND Targets the Treatment of Relapsed/Refractory Small Cell Lung Cancer Following Its Previous Approval in the Treatment of T-Cell NHL. Retrieved April 12, 2025, from https://www.prnewswire.com/news-releases/scitech-development-announces-2nd-fda-approval-of-a-phase-1-ab-ind-for-st-001-new-ind-targets-the-treatment-of-relapsedrefractory-small-cell-lung-cancer-following-its-previous-approval-in-the-treatment-of-t-cell-nhl-302421487.html[8] Cerevance Presents Positive Results from Phase 1 Study of CVN293 at American Academy of Neurology 2025 Annual Meeting. Retrieved April 12, 2025, from https://www.cerevance.com/media/cerevance-presents-positive-results-from-phase-1-study-of-cvn293-at-american-academy-of-neurology-2025-annual-meeting[9] LifeMine Announces First Participant Dosed in First-in-human Phase 1 Clinical Trial of LIFE-001, Designed De Novo to Become a Field Dominating Immunosuppressive for Immune-mediated Disorders and Transplantation. Retrieved April 12, 2025, from https://www.businesswire.com/news/home/20250407523884/en/LifeMine-Announces-First-Participant-Dosed-in-First-in-human-Phase-1-Clinical-Trial-of-LIFE-001-Designed-De-Novo-to-Become-a-Field-Dominating-Immunosuppressive-for-Immune-mediated-Disorders-and-Transplantation[10] Neurona Therapeutics Presents Positive Clinical Data Update from NRTX-1001 Cell Therapy Trial in Drug-resistant Epilepsy at American Academy of Neurology Annual Meeting. Retrieved April 12, 2025, from https://www.neuronatherapeutics.com/news/press-releases/040825/[11] Opus Genetics Announces One-Month Clinical Data from Pediatric Patient in Phase 1/2 Trial of OPGx-LCA5 Gene Therapy in Inherited Retinal Diseases. Retrieved April 12, 2025, from https://ir.opusgtx.com/press-releases/detail/483/opus-genetics-announces-one-month-clinical-data-from-pediatric-patient-in-phase-12-trial-of-opgx-lca5-gene-therapy-in-inherited-retinal-diseases[12] Cytora Reports Successful Results of Phase 1/2a Trial of Stem Cell Treatment for Diabetic Foot Ulcers. Retrieved April 12, 2025, from https://www.prnewswire.com/news-releases/cytora-reports-successful-results-of-phase-12a-trial-of-stem-cell-treatment-for-diabetic-foot-ulcers-302424359.html[13] KSQ Therapeutics Announces First Patient Dosed in Phase 1/2 Study for KSQ-004EX, a CRISPR/Cas9-Engineered Tumor Infiltrating Lymphocyte (eTIL®) Therapy. Retrieved April 12, 2025, from https://www.globenewswire.com/news-release/2025/04/09/3058270/0/en/KSQ-Therapeutics-Announces-First-Patient-Dosed-in-Phase-1-2-Study-for-KSQ-004EX-a-CRISPR-Cas9-Engineered-Tumor-Infiltrating-Lymphocyte-eTIL-Therapy.html[14] KSQ Therapeutics Announces First Patient Dosed in Phase 1/2 Study for KSQ-004EX, a CRISPR/Cas9-Engineered Tumor Infiltrating Lymphocyte (eTIL®) Therapy. Retrieved April 12, 2025, from https://www.globenewswire.com/news-release/2025/04/09/3058270/0/en/KSQ-Therapeutics-Announces-First-Patient-Dosed-in-Phase-1-2-Study-for-KSQ-004EX-a-CRISPR-Cas9-Engineered-Tumor-Infiltrating-Lymphocyte-eTIL-Therapy.html[15] Solu Therapeutics Closes $41M Series A Financing and Announces First Patient Dosed in Phase 1 Clinical Trial of STX-0712 in Patients with CMML and Other Advanced Hematologic Malignancies. Retrieved April 12, 2025, from https://cdn.prod.website-files.com/669551ccc7908830b842dc2b/67f55ddc890a926ab1f047c9_Final%20Solu%20press%20release_4.9.pdf[16] Context Therapeutics Doses First Patient in Phase 1 Clinical Trial of CT-95. Retrieved April 12, 2025, from https://www.globenewswire.com/news-release/2025/04/09/3058314/0/en/index.html[17] Amylyx Pharmaceuticals Announces First Participant Dosed in Phase 1, Multiple Ascending Dose LUMINA Trial of AMX0114 in People Living with Amyotrophic Lateral Sclerosis. Retrieved April 12, 2025, from https://www.amylyx.com/news/amylyx-pharmaceuticals-announces-first-participant-dosed-in-phase-1-multiple-ascending-dose-lumina-trial-of-amx0114-in-people-living-with-amyotrophic-lateral-sclerosis[18] Assembly Biosciences Presents New Data Highlighting Long-Acting Herpes Simplex Virus Candidate ABI-5366 and Genital Herpes Prevalence and Treatment Patterns at the 2025 ESCMID Congress. Retrieved April 12, 2025, from https://investor.assemblybio.com/news-releases/news-release-details/assembly-biosciences-presents-new-data-highlighting-long-acting[19] Seismic Therapeutic Doses First Cohort in Phase 1 Clinical Trial of S-4321, a Novel Bifunctional Antibody that Agonizes PD-1 and FcγRIIb Inhibitory Receptors for the Treatment of Autoimmune Disease. Retrieved April 12, 2025, from https://seismictx.com/seismic-therapeutic-doses-first-cohort-in-phase-1-clinical-trial-of-s-4321-a-novel-bifunctional-antibody-that-agonizes-pd-1-and-fc%ce%b3riib-inhibitory-receptors-for-the-treatment-of-autoimmune-disea/免责声明:药明康德内容团队专注介绍全球生物医药健康研究进展。本文仅作信息交流之目的,文中观点不代表药明康德立场,亦不代表药明康德支持或反对文中观点。本文也不是治疗方案推荐。如需获得治疗方案指导,请前往正规医院就诊。版权说明:本文来自药明康德内容团队,欢迎个人转发至朋友圈,谢绝媒体或机构未经授权以任何形式转载至其他平台。转载授权请在「药明康德」微信公众号回复“转载”,获取转载须知。分享,点赞,在看,聚焦全球生物医药健康创新
临床1期临床2期
分析
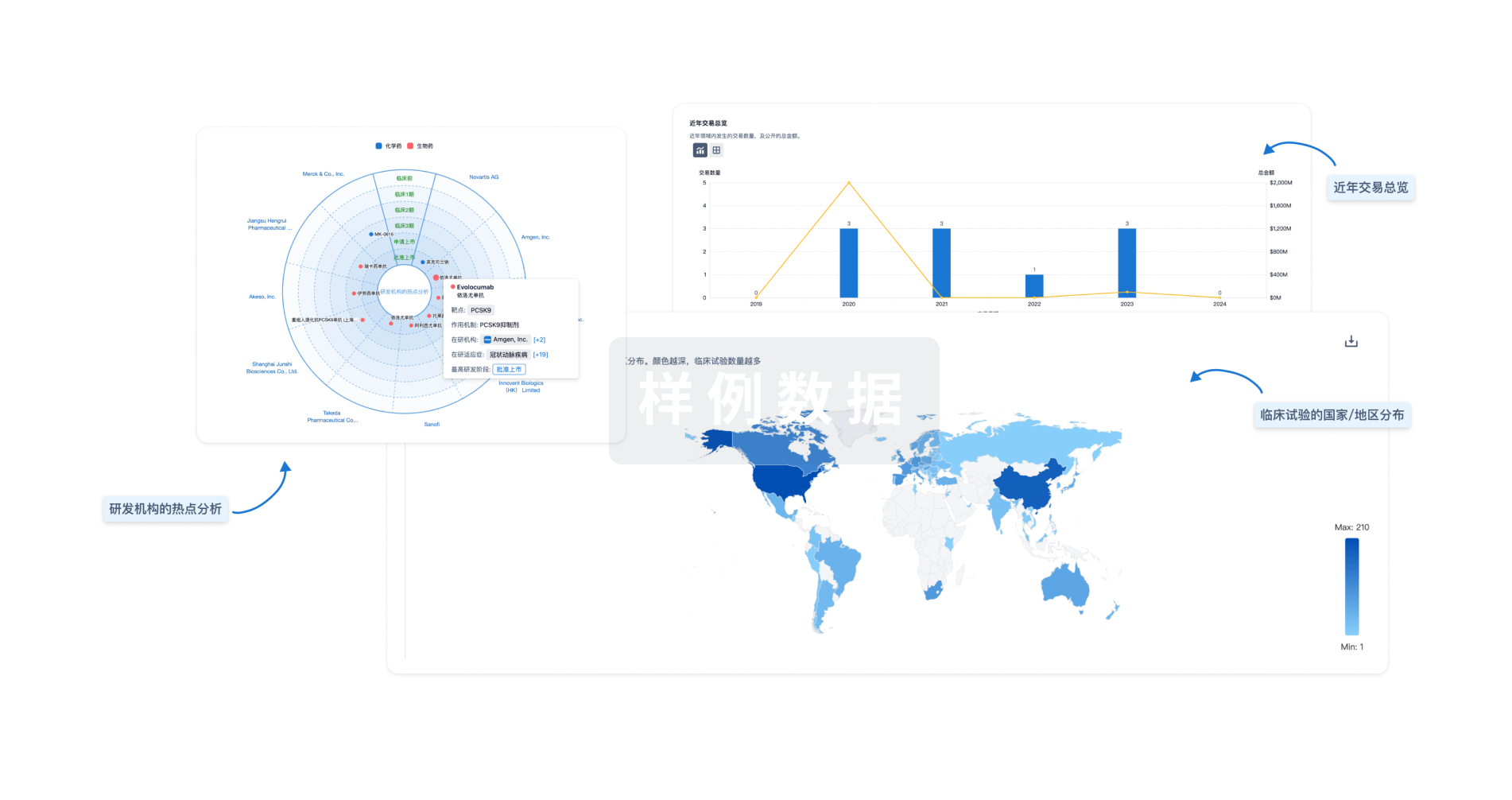
对领域进行一次全面的分析。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用




