预约演示
更新于:2025-09-09

Sierra Oncology, Inc.
更新于:2025-09-09
概览
标签
肿瘤
血液及淋巴系统疾病
其他疾病
DNAi疗法
疾病领域得分
一眼洞穿机构专注的疾病领域
暂无数据
技术平台
公司药物应用最多的技术
暂无数据
靶点
公司最常开发的靶点
暂无数据
| 排名前五的药物类型 | 数量 |
|---|---|
| DNAi疗法 | 3 |
| 排名前五的靶点 | 数量 |
|---|---|
| BRD4(溴结构域蛋白-4) | 1 |
| Chk1(检测点激酶1) | 1 |
| PKC(蛋白激酶C) | 1 |
关联
3
项与 Sierra Oncology, Inc. 相关的药物靶点 |
作用机制 Chk1抑制剂 |
在研机构 |
最高研发阶段临床2期 |
首次获批国家/地区- |
首次获批日期- |
靶点 |
作用机制 BRD4抑制剂 [+1] |
原研机构 |
在研适应症 |
最高研发阶段临床1/2期 |
首次获批国家/地区- |
首次获批日期- |
靶点 |
作用机制 PKC抑制剂 |
在研适应症 |
非在研适应症- |
最高研发阶段临床申请 |
首次获批国家/地区- |
首次获批日期- |
19
项与 Sierra Oncology, Inc. 相关的临床试验NCT04173494
A Randomized, Double-blind, Phase 3 Study to Evaluate the Activity of Momelotinib (MMB) Versus Danazol (DAN) in Symptomatic, Anemic Subjects With Primary Myelofibrosis (PMF), Post-polycythemia Vera (PV) Myelofibrosis, or Post-essential Thrombocythemia (ET) Myelofibrosis Who Were Previously Treated With JAK Inhibitor Therapy
MOMENTUM is a randomized, double-blind, active control Phase 3 trial intended to confirm the differentiated clinical benefits of the investigational drug momelotinib (MMB) versus danazol (DAN) in symptomatic and anemic participants who have previously received an approved Janus kinase inhibitor (JAKi) therapy for myelofibrosis (MF). The purpose of this clinical study is to compare the effectiveness and safety of MMB to DAN in treating and reducing: 1) disease related symptoms, 2) the need for blood transfusions and 3) splenomegaly, in adults with primary MF, post-polycythemia vera MF or post-essential thrombocythemia MF. The study is planned in countries including, but not limited to: Australia, Austria, Belgium, Bulgaria, Canada, Czech Republic, Denmark, France, Germany, Hungary, Israel, Italy, New Zealand, Poland, Romania, Singapore, South Korea, Spain, Sweden, Taiwan, United Kingdom (UK) and United States (US).
Participants must be symptomatic with a Myelofibrosis Symptom Assessment Form (MFSAF) version (v) 4.0 Total Symptom Score of >= 10 at screening, and be anemic with hemoglobin (Hgb) < 10 gram/deciliter (g/dL). For participants with ongoing JAKi therapy at screening, JAKi therapy must be tapered over a period of at least 1 week, followed by a 2-week non-treatment washout interval prior to randomization.
Participants will be randomized 2:1 to orally self-administer blinded treatment: MMB plus placebo or DAN plus placebo. Participants randomized to receive MMB who complete the randomized treatment period to the end of Week 24 may continue to receive MMB in the open-label extended treatment period to the end of Week 204 (a total period of treatment of approximately 4 years) if the participants tolerates and continues to benefit from MMB.
Participants randomized to receive DAN may cross-over to MMB open-label treatment in the following circumstances: at the end of Week 24 if they complete the randomized treatment period; or at the end of Week 24 if they discontinue treatment with DAN but continue study assessments and do not receive prohibited medications including alternative active anti-MF therapy; or at any time during the randomized treatment period if they meet the protocol-defined criteria for radiographically confirmed symptomatic splenic progression. Participants randomized to receive DAN who are receiving clinical benefit at the end of Week 24 may choose to continue DAN therapy up to Week 48. The comparator treatment, DAN, is an approved medication in the US and in some other countries and is recommended by national guidelines as a treatment for anemia in MF.
Participants must be symptomatic with a Myelofibrosis Symptom Assessment Form (MFSAF) version (v) 4.0 Total Symptom Score of >= 10 at screening, and be anemic with hemoglobin (Hgb) < 10 gram/deciliter (g/dL). For participants with ongoing JAKi therapy at screening, JAKi therapy must be tapered over a period of at least 1 week, followed by a 2-week non-treatment washout interval prior to randomization.
Participants will be randomized 2:1 to orally self-administer blinded treatment: MMB plus placebo or DAN plus placebo. Participants randomized to receive MMB who complete the randomized treatment period to the end of Week 24 may continue to receive MMB in the open-label extended treatment period to the end of Week 204 (a total period of treatment of approximately 4 years) if the participants tolerates and continues to benefit from MMB.
Participants randomized to receive DAN may cross-over to MMB open-label treatment in the following circumstances: at the end of Week 24 if they complete the randomized treatment period; or at the end of Week 24 if they discontinue treatment with DAN but continue study assessments and do not receive prohibited medications including alternative active anti-MF therapy; or at any time during the randomized treatment period if they meet the protocol-defined criteria for radiographically confirmed symptomatic splenic progression. Participants randomized to receive DAN who are receiving clinical benefit at the end of Week 24 may choose to continue DAN therapy up to Week 48. The comparator treatment, DAN, is an approved medication in the US and in some other countries and is recommended by national guidelines as a treatment for anemia in MF.
开始日期2020-02-07 |
申办/合作机构 |
NCT02797964
A Phase 1/2 Trial of SRA737 (a Chk1 Inhibitor) Administered Orally in Subjects With Advanced Cancer
The purpose of this clinical study is to establish the safety profile, determine the maximum tolerated dose (MTD) and recommend a Phase 2 dose and schedule of SRA737; and to evaluate the efficacy of SRA737 in prospectively-selected subjects with genetically-defined tumors that harbor genomic alterations linked to increased replication stress and that are hypothesized to be more sensitive to checkpoint kinase 1 (Chk1) inhibition via synthetic lethality. Specific cancer indications that frequently harbor these genetic mutations will be studied.
开始日期2016-07-01 |
申办/合作机构 |
NCT02797977
A Phase 1/2 Trial of Oral SRA737 (a Chk1 Inhibitor) Given in Combination With Gemcitabine Plus Cisplatin or Gemcitabine Alone in Subjects With Advanced Cancer
The purpose of this clinical study is to establish the safety profile, determine the maximum tolerated dose (MTD) and recommend a Phase 2 dose (RP2D) and schedule of SRA737 in combination with low dose gemcitabine; and to evaluate the efficacy of SRA737 in combination with low dose gemcitabine in prospectively-selected subjects with genetically-defined tumors that have predicted sensitivity to Chk1 inhibition based on factors including: genetic profiling of tumor tissue or ctDNA, HPV status, and germline BRCA1 and BRCA2 gene status. Specific cancer indications that frequently feature these factors will be studied.
Preclinical and clinical data support the hypothesis that active doses of SRA737 may be strongly potentiated by sub-therapeutic doses of gemcitabine, which should lead to clinical efficacy. To test this hypothesis, SRA737 in combination with low dose gemcitabine is being explored in this study.
Preclinical and clinical data support the hypothesis that active doses of SRA737 may be strongly potentiated by sub-therapeutic doses of gemcitabine, which should lead to clinical efficacy. To test this hypothesis, SRA737 in combination with low dose gemcitabine is being explored in this study.
开始日期2016-07-01 |
申办/合作机构 |
100 项与 Sierra Oncology, Inc. 相关的临床结果
登录后查看更多信息
0 项与 Sierra Oncology, Inc. 相关的专利(医药)
登录后查看更多信息
13
项与 Sierra Oncology, Inc. 相关的文献(医药)2024-07-01·iScience
CHK1 inhibitor SRA737 is active in PARP inhibitor resistant and CCNE1 amplified ovarian cancer
Article
作者: Kinose, Yasuto ; Shield-Artin, Kristy ; Milutinovic, Snezana ; Hassig, Christian ; Ratnayake, Gayanie ; Strouse, Bryan ; Wang, Xiaolei ; Hansen, Ryan J ; Beard, Sally ; Vandenberg, Cassandra J ; Gitto, Sarah B ; Barker, Holly E ; Medvedev, Sergey ; Hwang, Wei-Ting ; Kim, Hyoung ; Ho, Gwo-Yaw ; Scott, Clare L ; Simpkins, Fiona ; Xu, Haineng ; Wakefield, Matthew J
High-grade serous ovarian cancers (HGSOCs) with homologous recombination deficiency (HRD) are initially responsive to poly (ADP-ribose) polymerase inhibitors (PARPi), but resistance ultimately emerges. HGSOC with CCNE1 amplification (CCNE1 amp) are associated with resistance to PARPi and platinum treatments. High replication stress in HRD and CCNE1 amp HGSOC leads to increased reliance on checkpoint kinase 1 (CHK1), a key regulator of cell cycle progression and the replication stress response. Here, we investigated the anti-tumor activity of the potent, highly selective, orally bioavailable CHK1 inhibitor (CHK1i), SRA737, in both acquired PARPi-resistant BRCA1/2 mutant and CCNE1 amp HGSOC models. We demonstrated that SRA737 increased replication stress and induced subsequent cell death in vitro. SRA737 monotherapy in vivo prolonged survival in CCNE1 amp models, suggesting a potential biomarker for CHK1i therapy. Combination SRA737 and PARPi therapy increased tumor regression in both PARPi-resistant and CCNE1 amp patient-derived xenograft models, warranting further study in these HGSOC subgroups.
2023-07-27·British journal of cancer
A Phase 1/2 trial of SRA737 (a Chk1 inhibitor) administered orally in patients with advanced cancer
Article
作者: Carter, Louise ; Symeonides, Stefan N ; Danson, Sarah ; Banerji, Udai ; Sarker, Debashis ; Kristeleit, Rebecca ; Kowalski, Mark M ; Klencke, Barbara J ; Plummer, Ruth ; Evans, Thomas R Jeffry ; Jones, Robert ; Blagden, Sarah ; Veal, Gareth J ; Arkenau, Tobias
Abstract:
Background:
This was a first-in-human Phase 1/2 open-label dose-escalation study of the novel checkpoint kinase 1 (Chk1) inhibitor SRA737.
Methods:
Patients with advanced solid tumours enrolled in dose-escalation cohorts and received SRA737 monotherapy orally on a continuous daily (QD) dosing schedule in 28-day cycles. Expansion cohorts included up to 20 patients with prospectively selected, pre-specified response predictive biomarkers.
Results:
In total, 107 patients were treated at dose levels from 20–1300 mg. The maximum tolerated dose (MTD) of SRA737 was 1000 mg QD, the recommended Phase 2 dose (RP2D) was 800 mg QD. Common toxicities of diarrhoea, nausea and vomiting were generally mild to moderate. Dose-limiting toxicity at daily doses of 1000 and 1300 mg QD SRA737 included gastrointestinal events, neutropenia and thrombocytopenia. Pharmacokinetic analysis at the 800 mg QD dose showed a mean Cmin of 312 ng/mL (546 nM), exceeding levels required to cause growth delay in xenograft models. No partial or complete responses were seen.
Conclusions:
SRA737 was well tolerated at doses that achieved preclinically relevant drug concentrations but single agent activity did not warrant further development as monotherapy. Given its mechanism of action resulting in abrogating DNA damage repair, further clinical development of SRA737 should be as combination therapy.
Clinical trial registration:
Clinicaltrials.gov NCT02797964.
2023-01-17·Clinical cancer research : an official journal of the American Association for Cancer Research
A Phase I/II Trial of Oral SRA737 (a Chk1 Inhibitor) Given in Combination with Low-Dose Gemcitabine in Patients with Advanced Cancer
Article
作者: Carter, Louise ; Garralda, Elena ; Walter, Harriet S. ; Sarker, Debashis ; Anthoney, Alan ; Banerji, Udai ; Moreno, Victor ; Roxburgh, Patricia ; Kowalski, Mark M. ; Roda, Desamparados ; Kristeleit, Rebecca ; Plummer, Ruth ; Blagden, Sarah ; Klencke, Barbara J. ; Jones, Robert ; Arkenau, Tobias
Abstract:
Purpose::
This was a Phase I/II trial of the novel checkpoint kinase 1 (Chk1) inhibitor SRA737 given in combination with gemcitabine. Its objectives were to establish the safety profile, recommended Phase 2 dose (RP2D), pharmacokinetics profile, and clinical activity of SRA737.
Patients and Methods::
Patients with advanced solid tumors were enrolled into dose-escalation cohorts and treated in 28-day cycles with oral SRA737 on days 2, 3, 9, 10, 16, and 17, and intravenous gemcitabine on days 1, 8, and 15. Treatment was continued until progression. Each expansion cohort included up to 20 patients with specific genetically defined tumors.
Results::
The RP2D was determined to be 500 mg SRA737 combined with low-dose (250 mg/m2) gemcitabine. Of 143 enrolled patients, 77 were treated at doses of at least 500 mg SRA737 combined with 250 mg/m2 gemcitabine. Common toxicities of nausea, vomiting, fatigue, and diarrhea were primarily mild to moderate, and rarely led to treatment discontinuation. Anemia, neutropenia, and thrombocytopenia were grade ≥3 in 11.7%, 16.7%, and 10% of patients treated at the RP2D, respectively. The objective response rate (ORR) was 10.8% overall and notably the ORR in anogenital cancer was 25%. Partial tumor responses were observed in anogenital cancer, cervical cancer, high-grade serous ovarian cancer, rectal cancer, and small cell lung cancer.
Conclusions::
SRA737 in combination with low-dose gemcitabine was well tolerated with lower myelotoxicity than has been seen at standard doses of gemcitabine or with other combinations of Chk1 inhibitors with gemcitabine. Tumor responses were observed in anogenital and other solid tumors.
151
项与 Sierra Oncology, Inc. 相关的新闻(医药)2025-09-03
The launch of emerging therapies like BESREMi (PharmaEssentia and AOP Orphan Pharmaceuticals), INCB057643 (Incyte), XPOVIO (Karyopharm Therapeutics), RYTELO (Geron), REBLOZYL (Bristol Myers Squibb), Navtemadlin (Kartos Therapeutics), Pelabresib (Novartis), and others is going to shift the myelofibrosis market.
LAS VEGAS, Sept. 3, 2025 /PRNewswire/ -- DelveInsight's
Myelofibrosis Market Insights report includes a comprehensive understanding of current treatment practices, emerging myelofibrosis drugs, market share of individual therapies, and current and forecasted myelofibrosis market size from 2020 to 2034, segmented into leading markets (the US, EU4, UK, and Japan).
Myelofibrosis Market Summary
The total myelofibrosis treatment market size in the leading markets (the US, EU4, UK, and Japan) was
USD 2.2 billion in 2024.
The United States accounts for the largest market size of myelofibrosis, in comparison to EU4 (Germany, Italy, France, and Spain) and the UK, and Japan.
Based on DelveInsight's assessment in 2024, the 7MM had approximately
56K patient pool (prevalent cases) of myelofibrosis.
Key myelofibrosis companies, including
PharmaEssentia, AOP Orphan Pharmaceuticals, Incyte, Karyopharm Therapeutics, Geron, Bristol Myers Squibb, Kartos Therapeutics, Novartis, Merck, Telios Pharma, Ryvu Therapeutics, Sumitomo Pharma, Syntara, Disc Medicine, Menarini Group, and others, are actively working on innovative myelofibrosis drugs.
Some of the key myelofibrosis therapies in clinical trials include
BESREMi (ropeginterferon alfa-2b-njft/P-1101), INCB057643, XPOVIO (NEXPOVIO/selinexor/KPT-330), RYTELO (imetelstat), REBLOZYL (luspatercept/ACE-536), Navtemadlin (KRT-232), Pelabresib (DAK539), Bomedemstat (IMG-7289/MK-3543), TL-895, RVU120 ( SEL-120), TP-3654 (nuvisertib), SNT-5505 (PXS-5505), DISC-0974, ELZONRIS (tagraxofusp/SL-401), and others. These novel myelofibrosis therapies are anticipated to enter the myelofibrosis market in the forecast period and are expected to change the market.
By 2034, among all the therapies, the highest revenue is expected to be generated by
OJJAARA/OMJJARA.
Discover which myelofibrosis therapies are expected to grab the largest market share @
Myelofibrosis Market Report
Key Factors Driving the Growth of the Myelofibrosis Market
Novel Therapies Drive Myelofibrosis Treatment Advancements
Currently, four JAK inhibitors have been approved by the US FDA for the treatment of myelofibrosis, including JAKAFI (ruxolitinib), INREBIC (fedratinib), VONJO (pacritinib), and OJJAARA (momelotinib). No drug therapy can cure myelofibrosis. As myelofibrosis primarily affects older adults, stem cell transplantation is not a treatment option for most myelofibrosis patients. The launch of another JAK inhibitor, BESREMi, will further change the dynamics of the myelofibrosis market.
Rich clinical pipeline and emerging non-JAK approaches driving the myelofibrosis landscape
Beyond JAK inhibitors, active clinical development includes
BET inhibitors (Incyte's INCB057643; Novartis' Pelabresib),
XPO1 inhibitor (Karyopharm Therapeutics' XPOVIO),
Telomerase inhibitor (Geron's RYTELO),
MDM2 protein inhibitor (Kartos Therapeutics' Navtemadlin),
Tyrosine kinase inhibitors (Telios Pharma's TL-895),
PIM1 kinase inhibitor (Sumitomo Pharma's TP-3654),
LOX inhibitor (Syntara's SNT-5505), and others, raising market potential by promising new label expansions, second-line options, and higher-value therapies should any prove to be disease-modifying.
An aging population & increasing incidence with better survival
Myelofibrosis primarily affects older adults; population aging increases the absolute number of patients. As treatments improve symptoms and (in some cases) survival, prevalent patient pools grow, supporting longer-term market demand. In the US in 2024, the 70+ years of age group had the highest number of cases, accounting for approximately
60% of the total prevalent cases, while the ≤39 years of age group accounted for just
~2%.
Diagnostic & genomic testing improvements are driving myelofibrosis patient pool, leading to the growth of myelofibrosis market
Wider use of molecular profiling (JAK2, CALR, MPL, and others) enables earlier and more accurate MF diagnosis and better patient stratification for targeted therapies. This both expands the diagnosed population and helps match patients to appropriate, often higher-value, treatments.
Myelofibrosis Market Analysis
JAK inhibitors have become the cornerstone of treatment for patients with myelofibrosis, offering significant benefits such as spleen reduction, symptom relief, and improved quality of life, which can also extend survival in those with advanced disease. All approved JAK inhibitors primarily target JAK2, particularly the wild-type form, but they differ in their activity against other JAK family members.
For instance, JAKAFI myelofibrosis inhibits both JAK1 and JAK2; INREBIC selectively inhibits JAK2 while sparing JAK1 and also affects FLT3 and other targets; VONJO myelofibrosis inhibits JAK2 while sparing JAK1 but additionally impacts FLT3, IRAK, and ACVR1; and OJJAARA, approved through a different pathway, targets JAK1/JAK2 and ACVR1, mainly for myelofibrosis patients with anemia. These varying mechanisms lead to distinct patient outcomes.
JAKAFI myelofibrosis continues to see strong demand and is expected to grow further, maintaining its position as the standard of care in myelofibrosis. Myelofibrosis will remain the largest segment of JAKAFI's patient population until polycythemia vera cases eventually increase. However, market growth may be limited due to patent expirations of key therapies, with JAKAFI patents set to expire in 2027 for Novartis and 2028 for Incyte, presenting potential opportunities for competitors. In response, Incyte is exploring combination trials with novel drugs to extend JAKAFI's therapeutic lifespan.
Learn more about the treatment options for myelofibrosis @
Myelofibrosis Therapy
The myelofibrosis treatment landscape offers significant opportunities for innovation, focusing on several key areas:
Treating Lower-Risk Patients: Developing safe and effective therapies for patients with lower-risk myelofibrosis, allowing for earlier and more favorable interventions.
Enhancing First-Line Treatments: Improving existing first-line therapies for intermediate- to high-risk patients through novel drugs or combination strategies.
Managing Cytopenia: Developing targeted therapies to address cytopenia, a significant unmet need in patient care.
Myelofibrosis Competitive Landscape
The myelofibrosis clinical trial pipeline includes several drugs in mid- and late-stage development that are expected to enter the market during the forecast period. The emerging landscape offers a diverse range of therapeutic alternatives for treatment, including
XPOVIO (Karyopharm Therapeutics),
Elitracet (Takeda/Keros Therapeutics),
Navtemadlin (Kartos Therapeutics),
Pelabresib (Novartis),
INCB057643 (Incyte),
Bomedemstat (Merck), and others, all of which are used in various lines of treatment. The expected launch of these therapies is expected to have a further positive impact on the market.
INCB57643 is an orally administered small molecule. Bromodomain and extra-terminal (BET) proteins act as epigenetic readers that control the expression of key oncoproteins implicated in the development of myelofibrosis and other hematologic malignancies, including B-lymphoma-2, nuclear factor kappa, and c-Myc. In a prior Phase I/II clinical trial, the oral BET inhibitor INCB057643, tested both as a monotherapy and in combination with ruxolitinib, demonstrated favorable tolerability and promising clinical activity in patients with advanced cancers. In its Q2 2025 financial report, the company announced that the combination of INCB057643 with ruxolitinib and INCB57643 (a JAK1/JAK2 and BET inhibitor) is currently being evaluated in a Phase II trial for myelofibrosis.
RYTELO (imetelstat) is an investigational telomerase inhibitor that targets telomerase, selectively eliminating malignant stem and progenitor cells in the bone marrow, which drive diseases like myelodysplastic syndromes (MDS) and myelofibrosis. By blocking the proliferation of these malignant cells, imetelstat supports the recovery of healthy bone marrow and blood cell production and has shown disease-modifying effects and clinical benefits in Phase III trials for myelofibrosis. This mechanism sets imetelstat apart from other approved or investigational therapies for these blood cancers. In January 2025, Geron reported achieving 75% enrollment in the Phase III IMpactMF trial, which is comparing imetelstat to Best Available Therapy (BAT) in intermediate-2 or high-risk myelofibrosis patients who have relapsed or are refractory to JAK inhibitor treatment.
Elritercept is a late-stage investigational activin inhibitor aimed at treating anemia associated with hematologic malignancies, including MDS and myelofibrosis. It is currently undergoing Phase II evaluation in patients with myelofibrosis. In December 2024, Keros Therapeutics presented updated data from this ongoing Phase II trial at ASH 2024. Additionally, in December 2024, Takeda announced an exclusive licensing agreement with Keros to further develop, manufacture, and commercialize elritercept globally, excluding mainland China, Hong Kong, and Macau.
The anticipated launch of these emerging myelofibrosis therapies are poised to transform the myelofibrosis market landscape in the coming years. As these cutting-edge myelofibrosis therapies continue to mature and gain regulatory approval, they are expected to reshape the myelofibrosis market landscape, offering new standards of care and unlocking opportunities for medical innovation and economic growth.
To know more about new myelofibrosis treatment, visit @
Myelofibrosis Treatment Market
Recent Developments in the Myelofibrosis Market
In
July 2025, Incyte announced that the Phase I data in patients with myelofibrosis as monotherapy and in combination with ruxolitinib are anticipated in the second half of 2025.
In
June 2025, QIAGEN and Incyte announced a new global collaboration to develop a novel diagnostic panel to support Incyte's extensive portfolio of investigational therapies for patients with myeloproliferative neoplasms (MPNs), including Incyte's monoclonal antibody INCA033989.
In
January 2025, Karyopharm Therapeutics stated that it expects to report top-line results from the Phase III SENTRY trial in the second half of 2025, which could represent a potentially transformative opportunity to establish a new treatment paradigm in myelofibrosis.
What is
Myelofibrosis?
Myelofibrosis is a rare blood cancer marked by the accumulation of scar tissue, or 'fibrosis', in the bone marrow. This excess scar tissue prevents the bone marrow from producing enough healthy blood cells. It belongs to a group of blood cancers called 'myeloproliferative neoplasms (MPNs)', in which the blood cells produced by the bone marrow grow and function abnormally. When myelofibrosis arises independently, without being caused by another bone marrow disorder, it is referred to as primary myelofibrosis. In other cases, it can develop from another MPN, such as polycythemia vera or essential thrombocythemia. When this occurs, it is called secondary myelofibrosis, sometimes specifically termed post-polycythemia vera myelofibrosis or post-essential thrombocythemia myelofibrosis.
Myelofibrosis Epidemiology Segmentation
The myelofibrosis epidemiology section provides insights into the historical and current myelofibrosis patient pool and forecasted trends for the leading markets (the US, EU4, UK, and Japan). It helps recognize the causes of current and forecasted patient trends by exploring numerous studies and views of key opinion leaders.
The myelofibrosis market report proffers epidemiological analysis for the study period 2020–2034 in the leading markets (the US, EU4, UK, and Japan) segmented into:
Total Prevalent Cases of Myelofibrosis
Type-specific Cases of Myelofibrosis
Myelofibrosis Cases Based on Risk Stratification
Age-specific Prevalent Cases of Myelofibrosis
Myelofibrosis Cases Based on Molecular Alterations
Download the report to understand which factors are driving myelofibrosis epidemiology trends @
Myelofibrosis Treatment Drugs
Scope of the
Myelofibrosis
Market Report
Myelofibrosis Therapeutic Assessment: Myelofibrosis current marketed and emerging therapies
Myelofibrosis
Market Dynamics: Conjoint Analysis of Emerging Myelofibrosis Drugs
Competitive Intelligence Analysis: SWOT analysis and Market entry strategies
Myelofibrosis Market Unmet Needs, KOL's views, Analyst's views, Myelofibrosis Market Access and Reimbursement
Discover more about myelofibrosis drugs in development @
Myelofibrosis Clinical Trials
Table of Contents
Related Reports
JAK Inhibitors Market
JAK Inhibitors Market Size, Target Population, Competitive Landscape, and Market Forecast – 2034 report delivers an in-depth understanding of the market trends, market drivers, market barriers, and key JAK inhibitors companies, including
Pfizer, AbbVie, Galapagos, Sierra Oncology, Theravance Biopharma, Dizal Pharmaceutical, Aclaris Therapeutics, Celon Pharma, Incyte Corporation, Gilead Sciences, Reistone Biopharma, Jiangsu Hengrui Medicine Co., MaxiNovel Pharmaceuticals, among others.
Myelofibrosis Clinical Trial Analysis
Myelofibrosis Pipeline Insight
– 2025 report provides comprehensive insights about the pipeline landscape, pipeline drug profiles, including clinical and non-clinical stage products, and the key myelofibrosis companies, including
Geron Corporation, Merck, Ryvu Therapeutics SA, Morphic Therapeutic, iOnctura, Pharmaxis, Nippon Shinyaku, Active Biotech, Incyte Corporation, Sumitomo Pharma America, Inc., Cellenkos, Disc Medicine, among others.
Polycythemia Vera Market
Polycythemia Vera Market Insights, Epidemiology, and Market Forecast – 2034 report delivers an in-depth understanding of the disease, historical and forecasted epidemiology, as well as the market trends, market drivers, market barriers, and key polycythemia vera companies, including
Incyte, Novartis, PharmaEssentia, AOP Orphan Pharmaceuticals, Protagonist Therapeutics, Merck (Imago BioSciences), Italfarmaco, Ionis Pharmaceutical, Silence Therapeutics, Perseus Proteomics, AbbVie, Johnson & Johnson Innovative Medicine, Mabwell (Shanghai) Bioscience, Disc Medicine, GluBio Therapeutics, among others.
Multiple Myeloma Market
Multiple Myeloma Market Insights, Epidemiology, and Market Forecast – 2034 report delivers an in-depth understanding of the disease, historical and forecasted epidemiology, as well as the market trends, market drivers, market barriers, and key multiple myeloma companies, including
Sanofi, Karyopharm Therapeutics, AbbVie, Takeda Pharmaceutical, Celgene, Bristol-Myers Squibb, RAPA Therapeutics, Pfizer, Array Biopharma, Cellectar Biosciences, BioLineRx, Celgene, Aduro Biotech, ExCellThera, Janssen Pharmaceutical, Precision BioSciences, Takeda, Glenmark (Ichnos Sciences SA), Poseida Therapeutics, Molecular Partners AG, Chipscreen Biosciences, AbbVie, Genentech (Roche), Janssen Biotech, Nanjing Legend Biotech, Merck Sharp & Dohme Corp., among others.
About DelveInsight
DelveInsight is a leading Business Consultant and Market Research firm focused exclusively on life sciences. It supports pharma companies by providing comprehensive end-to-end solutions to improve their performance. Get hassle-free access to all the healthcare and pharma market research reports through our subscription-based platform PharmDelve
.
Connect with us on LinkedIn
| Facebook | Twitter
Contact Us
Shruti Thakur
[email protected]
+14699457679
Logo:
SOURCE DelveInsight Business Research, LLP
WANT YOUR COMPANY'S NEWS FEATURED ON PRNEWSWIRE.COM?
440k+
Newsrooms &
Influencers
9k+
Digital Media
Outlets
270k+
Journalists
Opted In
GET STARTED
临床2期引进/卖出临床1期上市批准临床结果
2025-08-08
·贝壳社
▲点击图片,了解详情
近日,贝壳社澳洲创新中心合伙人/总经理曾军博士正式当选为澳大利亚皇家化学会院士(FRACI)。这不仅是对曾博个人学术与产业化成就的高度肯定,更为贝壳社澳洲创新中心按下了“院士级”升级键。
(曾军博士)
曾军博士深耕药物研发领域二十余年,先后在顶尖学术机构与多家生物医药企业任职,拥有10余项具有显著商业价值的发现专利。其中一项名为“选择性激酶抑制剂”的专利,推动Cytopia于2006年与诺华达成商业合作,里程碑付款高达2.65亿美元。他发明的JAK抑制剂药物Ojjaara,被GSK于2022年以19亿美元从Sierra Oncology收购,该药物于2023年获FDA批准用于治疗骨髓纤维化伴贫血。自2009年起,曾博创立或联合创立了多家新药研发企业,并兼任四川大学客座教授及澳大利亚墨尔本大学荣誉副教授。
从靶点发现、专利布局、重磅交易到上市药物,曾博以“科学家+企业家”的双重身份,持续推动全球创新药在澳洲的临床加速。
全球医健产业加速变革的当下,临床研究与转化正成为企业破局国际市场的核心引擎。澳洲用不到世界0.3%的人口,贡献了超过2.5%的医学研究成果,并凭借其前瞻性的政策支持、严谨的临床研究体系和开放的创新生态成为全球临床研究高地。
从享誉全球的医疗科研实力到28天审批的临床跑道,从43.5%现金退税到临床数据互认,澳州把“科研深度”与“产业速度”熔于一炉,成为跨国药企与Biotech抢占全球市场的必争之地。
作为中国医健国际化服务的先行者,贝壳社早在2016年着手布局澳洲,成立贝壳社澳洲创新中心。在澳洲联邦政府、澳洲贸易委员会、维州政府、南澳州政府的共同支持下,多年来一直持续推动中澳在生物医药领域的双向创新成果转化合作,并依托成熟的跨境服务体系,为国内医健企业提供临床落地到市场准入的一站式解决方案。促进中澳两地的学术与产业交流合作,人才项目引进,实现医健行业全球优秀技术成果转化,推动和提升中澳医健市场的协同发展和产业生态的建立。
目前,贝壳社澳洲创新中心可全方位链接澳洲政府、协会、科研机构、医院、临床CRO等生态资源,后续可根据企业实际需求提供定制化的的海外药物临床研发全产业链落地服务。如一站式澳洲药物临床管理服务,专注于医药企业赴澳开展临床试验过程中境外公司落地,税务申报,临床试验咨询,临床试验监查等在澳全套临床管理服务。产品进入澳洲市场注册准入服务,代理申报澳洲TGA认证,服务包括医疗器械、保健品、防护用品等医疗产品的澳洲注册和市场准入。
此外,通过构建“技术引进来、成果走出去”的双向通道,帮助中国医健企业高效打通澳洲乃至全球市场。
2019年5月,杭州高新区(滨江)积极响应科技部火炬中心“一带一路”创新中心建设和国际科技合作号召,与科技部火炬中心联合共建的中澳生物医药产业科技园在杭州正式开园,委托贝壳社独家运营,承担对接中澳产业园和中澳健康产业创新桥梁职责,解决海外技术研究与全球最大健康产业市场之间的鸿沟,实现海内外双向转化。
贝壳社澳洲创新中心以澳洲顶尖科研为起点,以中国产业为放大器,以全球资本为加速器,帮助医健创新项目在最短路径完成“科学发现—临床验证—产业落地—全球市场”的闭环。当“快临床、低成本、全球通”成为生物医药竞争的新赛点,曾军的院士身份,不仅是个人荣誉的加冕,亦是贝壳社澳洲创新中心的新起点,更是医健企业通往全球市场的一张“院士级”通行证。
未来我们将继续加深与澳洲当地医疗健康学术和产业交流合作,人才项目引进,为实现全球化优秀成果转移和产业化,推动和提升中澳医疗健康市场的共同融合与发展贡献自己的力量。
往
期
推
荐
1
医健企业前沿动态
2
医健行业BD/出海/投融资洞察
_
_
_
*声明:本文仅用于分享
关于贝壳社
贝壳社是国内领先的医健创新创业服务平台,构建了"产业空间+创业教育+投资孵化+资本运作"四位一体服务体系,为医健领域创业企业提供全周期赋能。通过深度挖掘高成长项目、精准匹配产业资源及全球化生态网络,覆盖企业从孵化培育到加速发展的全链路,重点提供包括空间落地、创业培训、资本运作及跨境资源链接服务。贝壳社以加速科学技术成果转化与产业升级为目标,致力于成为医健领域的孵化器、加速器、连接器。
并购专利到期
2025-07-22
NEW YORK, July 22, 2025 /PRNewswire/ -- OrbiMed, a leading global healthcare investment firm, today announced the promotion of Mona Ashiya, Ph.D., to general partner. Ashiya joins the company's eight existing general partners as a management company owner and leader of the firm.
"Mona is a recognized leader in biotechnology investing," OrbiMed Managing Partner Carl Gordon said. "She has made significant contributions to the industry and to OrbiMed. We look forward to continuing to work with her to start and grow the next generation of exciting biotechnology companies."
Since joining OrbiMed in 2010, Ashiya has focused on venture capital and special situations opportunities. She has established herself as a leading, consistently successful investor in the life sciences venture capital ecosystem. Ashiya led OrbiMed's investments in many industry-leading companies, including Sierra Oncology, Disc Medicine and ProfoundBio. She has also advanced the growth of OrbiMed's special situations investment practice, leading numerous PIPE investments during her tenure.
About OrbiMed
OrbiMed is a leading healthcare investment firm, with over $17 billion in assets under management. OrbiMed invests globally across the healthcare industry, from start-ups to large multinational corporations, through private equity funds, public equity funds, and royalty/credit funds. OrbiMed seeks to be a capital provider of choice, providing tailored financing solutions and extensive global team resources to help build world-class healthcare companies. OrbiMed's team of over 130 professionals is based in New York City, London, San Francisco, Shanghai, Hong Kong, Mumbai, Herzliya, and other key global markets. For more information, please visit or follow us on X @OrbiMed.
SOURCE OrbiMed
WANT YOUR COMPANY'S NEWS FEATURED ON PRNEWSWIRE.COM?
440k+
Newsrooms &
Influencers
9k+
Digital Media
Outlets
270k+
Journalists
Opted In
GET STARTED
高管变更
100 项与 Sierra Oncology, Inc. 相关的药物交易
登录后查看更多信息
100 项与 Sierra Oncology, Inc. 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2025年11月12日管线快照
管线布局中药物为当前组织机构及其子机构作为药物机构进行统计,早期临床1期并入临床1期,临床1/2期并入临床2期,临床2/3期并入临床3期
临床申请
1
1
临床1期
临床2期
1
13
其他
登录后查看更多信息
当前项目
登录后查看更多信息
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
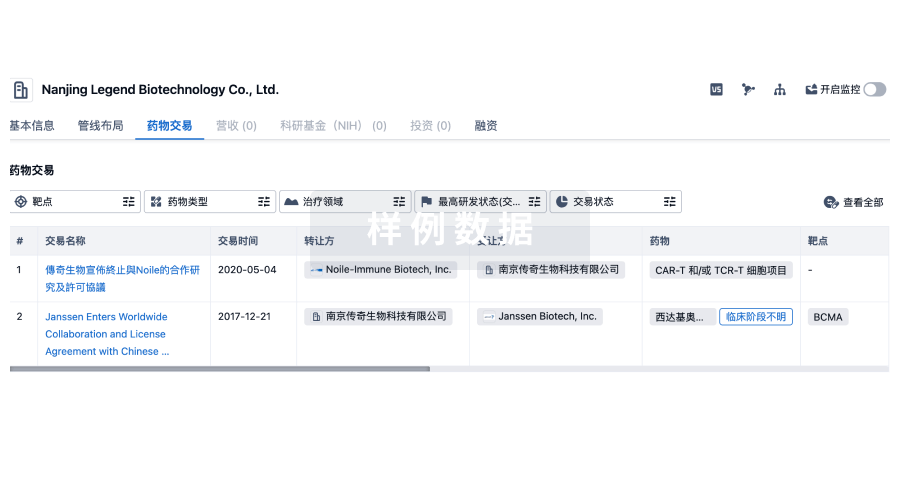
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
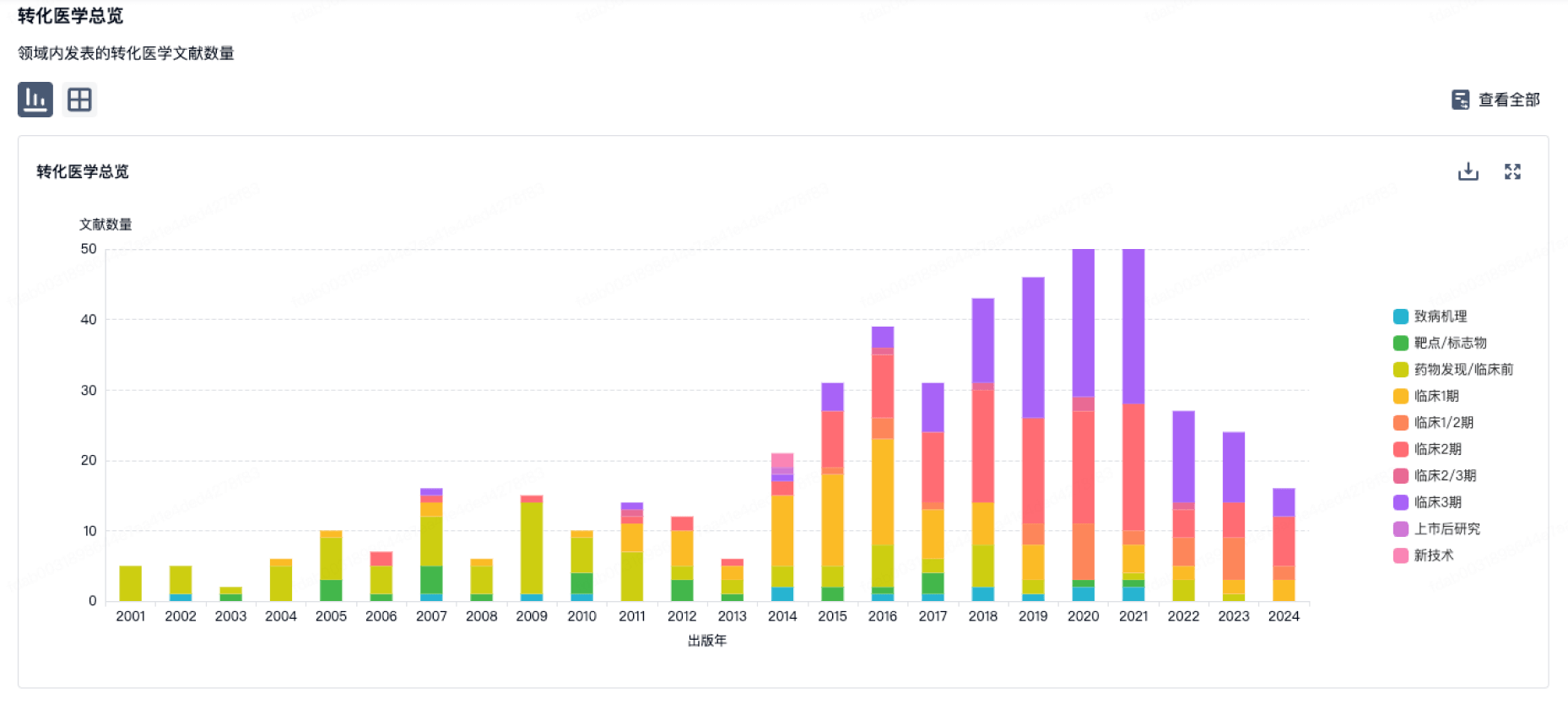
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
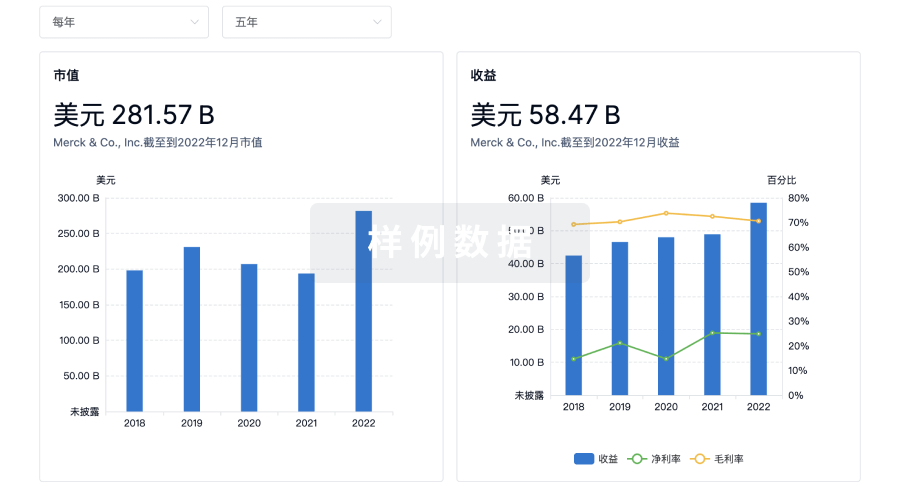
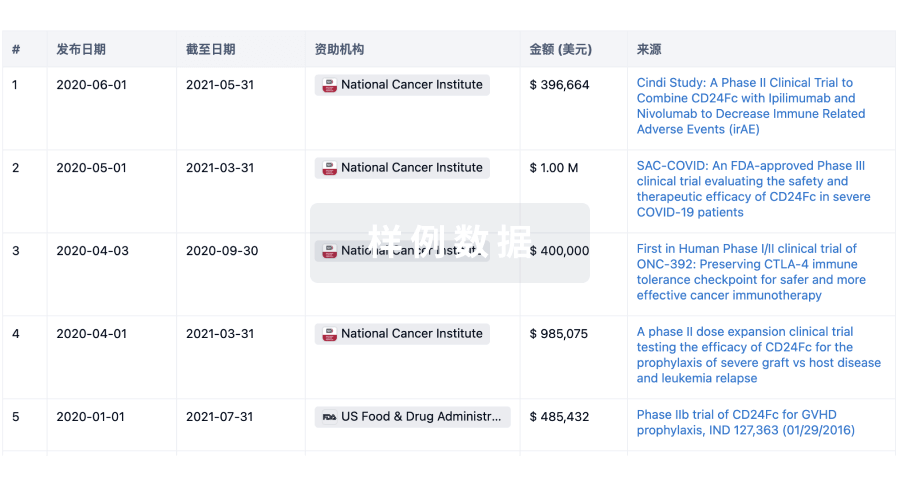
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
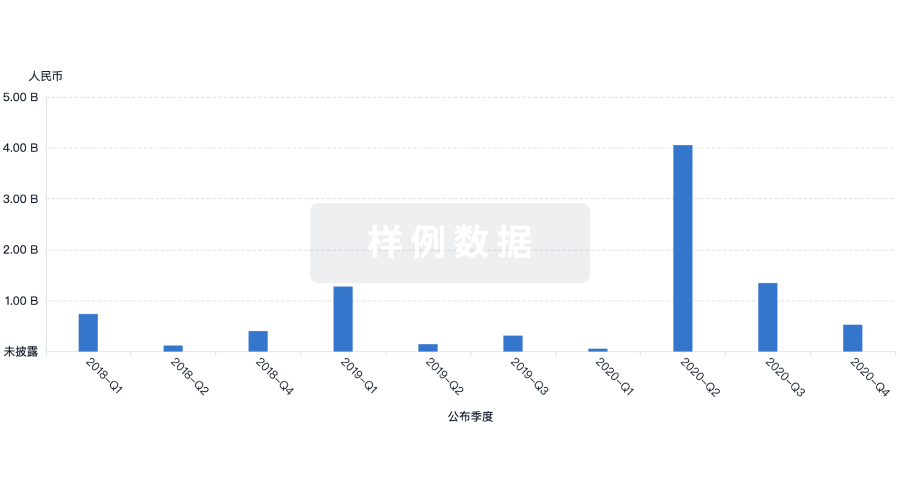
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
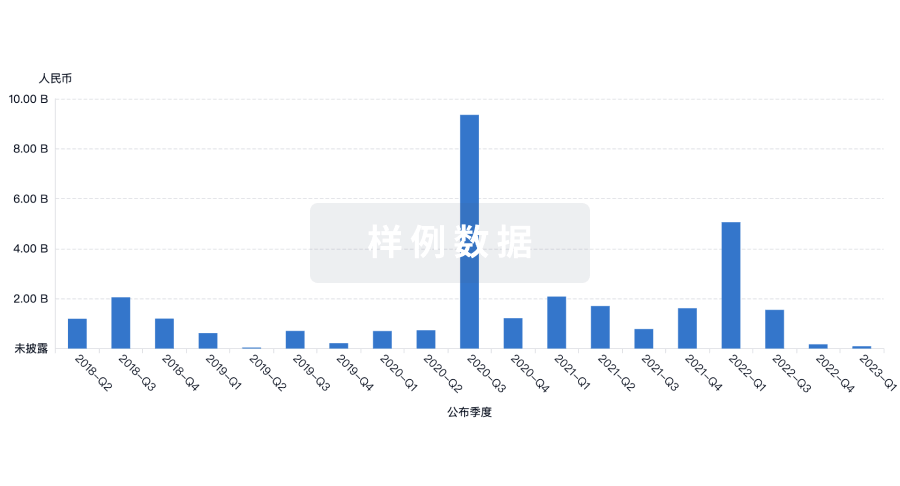
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用

