预约演示
更新于:2025-05-07

Kira Pharmaceuticals (Suzhou) Co., Ltd.
科越医药(苏州)有限公司|控股公司|2017|中国江苏省
科越医药(苏州)有限公司|控股公司|2017|中国江苏省
更新于:2025-05-07
概览
标签
免疫系统疾病
血液及淋巴系统疾病
其他疾病
抗体融合蛋白
关联
1
项与 科越医药(苏州)有限公司 相关的药物靶点 |
作用机制 C5抑制剂 [+1] |
在研机构 |
原研机构 |
非在研适应症- |
最高研发阶段临床2期 |
首次获批国家/地区- |
首次获批日期- |
2
项与 科越医药(苏州)有限公司 相关的临床试验CTR20223383
一项评价KP104在IgA肾病(IgAN)和C3肾小球病(C3G)受试者中的有效性、安全性、药代动力学和药效学的开放性II期研究
评价KP104在IgA肾病(IgAN)和C3肾小球病(C3G)受试者中的有效性、安全性、药代动力学和药效学
开始日期- |
申办/合作机构 |
CTR20222784
一项评价KP104在未接受过补体抑制剂治疗的阵发性睡眠性血红蛋白尿症(PNH)受试者中的安全性、耐受性、药代动力学、药效学和有效性的开放性II期研究
评价KP104在未接受过补体抑制剂治疗的阵发性睡眠性血红蛋白尿症(PNH)受试者中的安全性、耐受性、药代动力学、药效学和有效性
开始日期2022-11-21 |
申办/合作机构 |
100 项与 科越医药(苏州)有限公司 相关的临床结果
登录后查看更多信息
0 项与 科越医药(苏州)有限公司 相关的专利(医药)
登录后查看更多信息
3
项与 科越医药(苏州)有限公司 相关的文献(医药)2024-11-05·Blood
KP104, a Bifunctional C5 Mab-Factor H Fusion Protein, Demonstrates Sustained Long-Term Efficacy and Safety in Complement Inhibitor-Naïve PNH Patients: Updated Results from a Phase 2 Study at 36/38 Weeks of Obd Treatment
作者: Han, Bing ; Yue, Changhe ; Zhang, Li ; Tsui, Ping ; Yan, Hui ; Ma, Jay ; Weng, Qing Yu Christina ; Zhang, Fengkui ; Yang, Chen ; He, Chaomei ; Fu, Helen ; Song, Wenru
2023-11-02·Blood
KP104, a Bifunctional C5 Antibody/Factor H Fusion Protein, Effectively Controls Both Intravascular and Extravascular Hemolysis: Interim Results from a Phase 2 Study in Complement Inhibitor-Naïve PNH Patients
作者: Tsui, Ping ; He, Chaomei ; Song, Wenru ; Yang, Chen ; Han, Bing ; Ma, Jay ; Wu, Jingtao ; Yue, Changhe ; Zhang, Li ; Fu, Helen ; Zhang, Fengkui ; Wang, Chunrong ; Yan, Hui ; Lee, Richard
2022-11-15·Blood
Trial in Progress: An Open-Label, Phase 2 Study to Evaluate the Safety, Tolerability, Pharmacokinetics, Pharmacodynamics, and Efficacy of KP104 in Complement Inhibitor-Naïve Subjects with Paroxysmal Nocturnal Hemoglobinuria
作者: Han, Bing ; Tsui, Ping ; He, Chaomei ; Rabe, Martin ; Beddingfield, Frederick ; Yue, Changhe ; Ma, Jay ; Wang, Chunrong ; He, Guangsheng ; Song, Wenru ; Wu, Jingtao ; Zhou, Hu ; Lee, Richard ; Zhang, Fengkui ; Fu, Helen
23
项与 科越医药(苏州)有限公司 相关的新闻(医药)2024-08-18
·医药笔记
▎Armstrong
2024年上半年,补体药物市场规模达到39亿美元,其中阿斯利康两款C5抗体合计销售32亿美元。值得注意的是,补体药物呈现百花齐放的局面,近两年来多款创新药获批,药物形式上从小分子,到抗体,到环肽,再到Aptamer,适应症也扩展到眼科,包括GA这样的常见病。
阿斯利康C5抗体获批gMG、NMOSD神经学适应症后,销售额增长迅速,两款C5抗体全年有望接近70亿美元。
Apellis的C3环肽Syfovre率先获批GA适应症,在经历视网膜血管炎副作用的调查事件后,已经重回增长轨道,2024年上半年实现2.93亿美元销售额。
安斯泰来的C5靶向Aptamer也获批治疗GA适应症,2024年上半年实现1.29亿美元销售额,环比上周73%,放量迅速。
诺华的CFB小分子抑制剂Fabhalta已经获批,2024年上半年销售额2800万美元。
总结
随着神经学、眼科等新适应症的突破,补体药物进入加速发展的新时代。补体C5、C3血浆放量极高,常规的大分子、小分子成药壁垒都很高,新药物形式如环肽、Aptamer等带来新的工具,siRNA也是临床在研的主要技术路径之一。此外,旁路途径新靶点的选择,也是重要的探索方向。国内方面,天辰生物、科越医药、领诺医药等都在开发双靶点或新靶点的补体通路创新药。
Armstrong技术全梳理系列
GPRC5D靶点全梳理;
CD40靶点全梳理;
CD47靶点全梳理;
补体靶向药物技术全梳理;
补体药物:眼科治疗的重要方向;
Claudin 6靶点全梳理;
Claudin 18.2靶点全梳理;
靶点冷暖,行业自知;
中国大分子新药研发格局;
被炮轰的“me too”;
佐剂百年史;
胰岛素百年传奇;
CUSBEA:风雨四十载;
中国新药研发的焦虑;
中国生物医药企业的研发竞争;
中国双抗竞争格局;
中国ADC竞争格局;
中国双抗技术全梳理;
中国ADC技术全梳理;
Ambrx技术全梳理;
Vir Biotech技术全梳理;
Immune-Onc技术全梳理;
亘喜生物技术全梳理;
康哲药业技术全梳理;
科济药业技术全梳理;
恺佧生物技术全梳理;
同宜医药技术全梳理;
百奥赛图技术全梳理;
腾盛博药技术全梳理;
创胜集团技术全梳理;
永泰生物技术全梳理;
中国抗体技术全梳理;
德琪医药技术全梳理;
德琪医药技术全梳理2.0;
和铂医药技术全梳理;
荣昌生物技术全梳理;
再鼎医药技术全梳理;
药明生物技术全梳理;
恒瑞医药技术全梳理;
豪森药业技术全梳理;
正大天晴技术全梳理;
吉凯基因技术全梳理;
基石药业技术全梳理;
百济神州技术全梳理;
百济神州技术全梳理第2版;
信达生物技术全梳理;
信达生物技术全梳理第2版;
中山康方技术全梳理;
复宏汉霖技术全梳理;
先声药业技术全梳理;
君实生物技术全梳理;
嘉和生物技术全梳理;
志道生物技术全梳理;
道尔生物技术全梳理;
尚健生物技术全梳理;
康宁杰瑞技术全梳理;
科望医药技术全梳理;
科望医药技术全梳理2.0;
岸迈生物技术全梳理;
礼进生物技术全梳理;
康桥资本技术全梳理;
余国良的抗体药布局;
荃信生物技术全梳理;
安源医药技术全梳理;
三生国健技术全梳理;
仁会生物技术全梳理;
乐普生物技术全梳理;
同润生物技术全梳理;
宜明昂科技术全梳理;
派格生物技术全梳理;
迈威生物技术全梳理;
Momenta技术全梳理;
NGM技术全梳理;
普米斯生物技术全梳理;
普米斯生物技术全梳理2.0;
三叶草生物技术全梳理;
贝达药业抗体药全梳理;
泽璟制药抗体药全梳理;
恒瑞医药抗体药全梳理;
齐鲁制药抗体药全梳理;
石药集团抗体药全梳理;
豪森药业抗体药全梳理;
华海药业抗体药全梳理;
科伦药业抗体药全梳理;
百奥泰技术全梳理;
凡恩世技术全梳理。
抗体药物偶联物siRNA
2024-06-19
·医药观澜
6月18日,科越医药宣布,在2024年欧洲血液学协会(EHA)会议上以口头报告形式公布了KP104治疗阵发性睡眠性血红蛋白尿症2期临床研究的长期安全性和有效性结果。KP104是一种在研双功能C5抗体/H因子融合蛋白。
阵发性睡眠性血红蛋白尿症(PNH)是一种罕见的、危及生命的血液疾病,由属于先天免疫系统的补体系统的过度活动引起。PNH以红细胞破坏、血栓形成和骨髓功能受损为特征。由于补体生物学的复杂性和PNH致病病理学的多种途径,该疾病仍然存在巨大未被满足的临床需求,急需具有比当前疗法更好的疗效和给药便利性的下一代药物。据介绍,当前的疗法尚无法解决与替代途径相关的血管外溶血(EVH),或是存在不能充分阻断下游C5的问题,导致危及生命的突破性溶血。
KP104是一种具有独特作用机制的双功能补体生物药。该产品旨在同时选择性抑制补体旁路(H因子)和末端途径(C5),提供一种协同机制且可能更加有选择性的精准治疗补体介导的疾病。KP104还被设计成具有延长的半衰期和效力,其配方可用于静脉注射和皮下给药。
本次在EHA年会口头报告的是一项2期临床研究的长期结果,该研究针对的是未接受补体抑制剂治疗的PNH患者。研究要点包括了18名患者长达65周的治疗结果,以及所有患者均从剂量递增阶段的3个队列(每个队列n=6)转换到最佳生物剂量(OBD)后,继续长达24~26周的治疗结果。
在转换到OBD后,患者的血红蛋白水平持续改善:在没有输血的情况下,100% (18/18)患者的血红蛋白水平从基线水平增加≥2g/dL,89%(16/18)达到血红蛋白正常化(≥12g/dL),平均(SD)为13.5(1.4)g/dL。其中两例分别患有再生障碍性贫血和骨髓增殖性肿瘤的患者也显示出血红蛋白的改善接近正常水平。
患者在整个治疗期间持续控制乳酸脱氢酶(LDH)水平至接近正常水平,表明KP104非常有效的控制血管内溶血(IVH)。在OBD转换后24/26周结束时,94%(17/18)的患者实现了LDH <1.5x正常值上限(ULN)。
所有患者在KP104治疗期间(从第1天到第65周)之间均不需要输血。
所有其他临床次要终点也观察到显著的改善:转换到OBD后,网织红细胞绝对计数、胆红素水平和FACIT-疲劳评分均恢复正常化。
KP104是安全的,耐受性良好,没有3级或以上的治疗期间不良事件(TEAEs)。
科越医药新闻稿表示,这些来自于2期临床研究的确定性长期结果进一步表明:在安全有效地控制PNH的血管内和血管外溶血方面,KP104具有作为一线单药疗法并且同时靶向补体旁路途径和末端途径的“best-in-class"潜力。这一长期临床试验结果支持KP104推进到全球3期临床试验,科越医药正在计划全球3期临床研究,旨在确定KP104作为PNH治疗的新标准。
参考资料:[1]科越医药在2024年欧洲血液学协会会议上公布了KP104关于阵发性睡眠性血红蛋白尿症II期临床研究的积极的长期安全性和有效性结果. Retrieved June 17,2024, From https://mp.weixin.qq.com/s/EeSWY1Qy8XscTuz-3-idYg
内容来源于网络,如有侵权,请联系删除。
临床结果
2024-04-02
·医药笔记
2024年4月2日,辉瑞PF-07264660注射液、PF-07275315注射液的临床试验申请获得NMPA受理。
PF-07275315为IL-4/IL-13/TSLP三抗,PD-07264660为IL-4/IL-13/IL-33三抗,两款自免三抗均处于二期临床阶段,适应症均为特应性皮炎。
在肿瘤领域,双抗、多抗的研发布局非常活跃,既有EGFR/cMET这样的TAA组合,也有PD-1/CTLA-4这样免疫检验点的组合,以及TAA/CD3这样的T cell engager,或者PD-1/VEGF这样免疫检验点与血管增生抑制的机制组合等,并陆续取得临床突破。而在自免领域,双抗/多抗的布局少了很多,根源仍在于如何达到机制协同的效果,并且满足慢病药物更高安全性门槛的要求。国内方面,进入临床阶段的自免双抗只有少数几款,包括智翔金泰的TSLP双表位双抗,融捷康生物的IL-4R/IL-5双抗,以及天辰生物、科越医药的补体双功能抗体等。
内容来源于网络,如有侵权,请联系删除。

抗体药物偶联物申请上市
100 项与 科越医药(苏州)有限公司 相关的药物交易
登录后查看更多信息
100 项与 科越医药(苏州)有限公司 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2025年11月06日管线快照
管线布局中药物为当前组织机构及其子机构作为药物机构进行统计,早期临床1期并入临床1期,临床1/2期并入临床2期,临床2/3期并入临床3期
临床2期
1
登录后查看更多信息
当前项目
| 药物(靶点) | 适应症 | 全球最高研发状态 |
|---|---|---|
KP-104 ( C5 x CFH ) | C3肾小球病 更多 | 临床2期 |
登录后查看更多信息
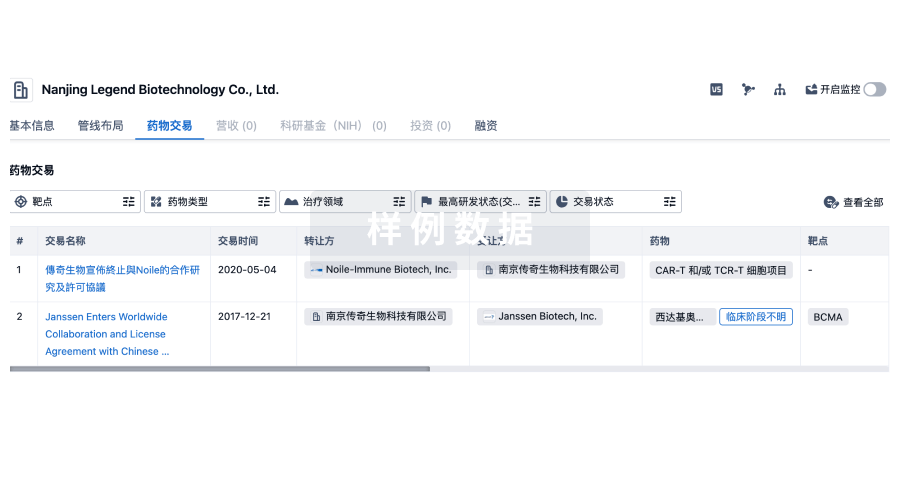
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
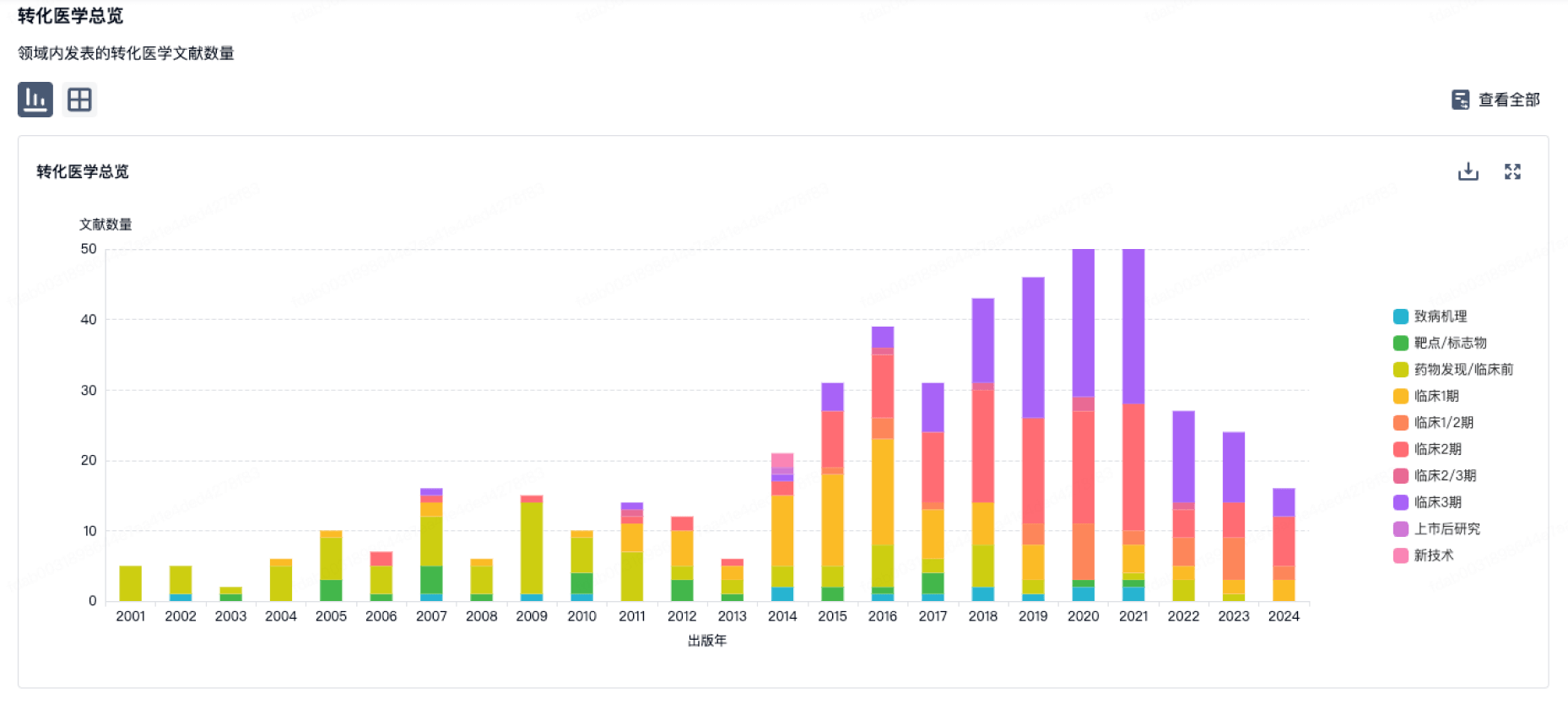
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
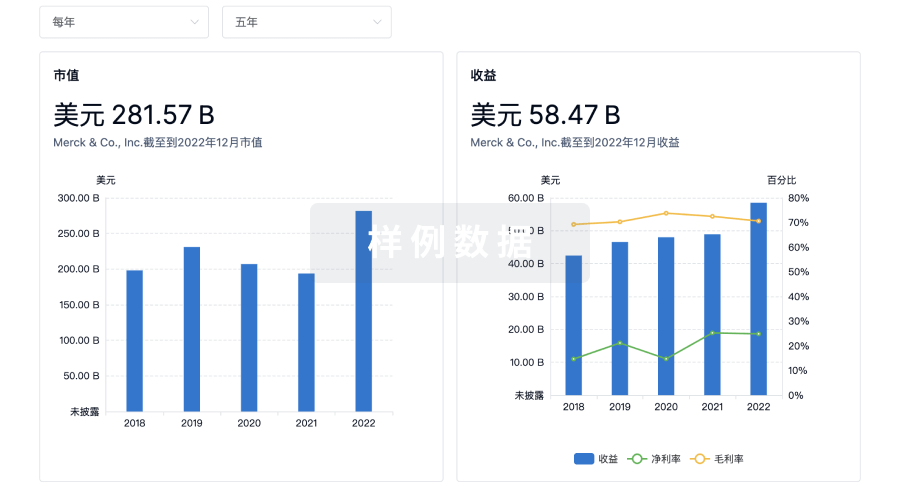
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
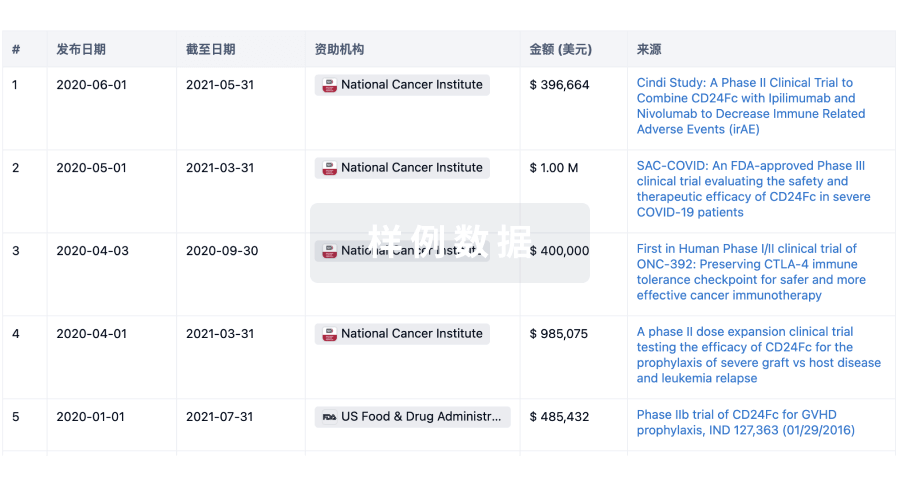
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
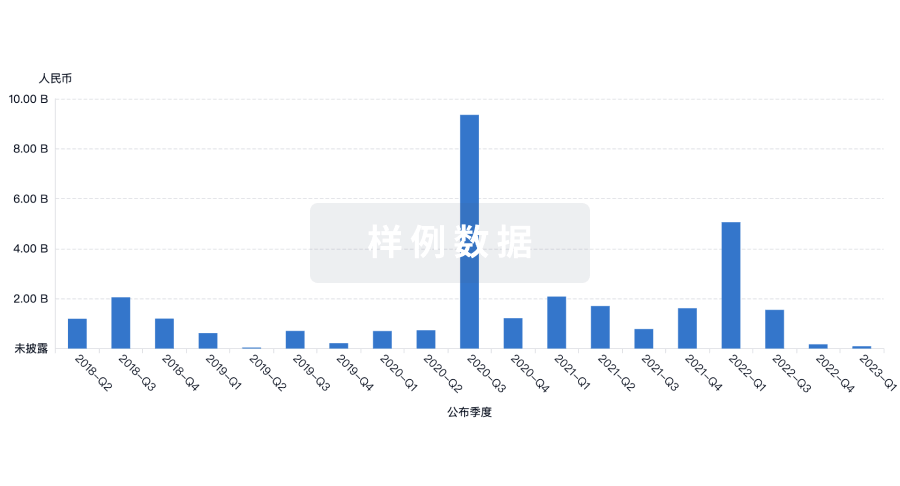
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
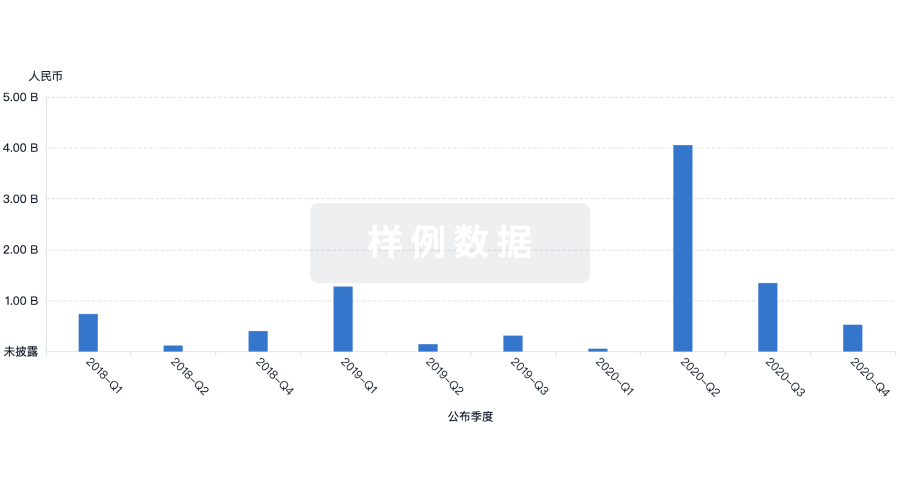
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
