更新于:2024-12-04
Chongqing Medical University /The First Affiliated Hospital/
中国
中国
更新于:2024-12-04
概览
标签
肿瘤
泌尿生殖系统疾病
诊断用放射药物
小分子化药
核素偶联药物
疾病领域得分
一眼洞穿机构专注的疾病领域
暂无数据
技术平台
公司药物应用最多的技术
暂无数据
靶点
公司最常开发的靶点
暂无数据
| 排名前五的药物类型 | 数量 |
|---|---|
| 诊断用放射药物 | 3 |
| 小分子化药 | 1 |
| 核素偶联药物 | 1 |
| 排名前五的靶点 | 数量 |
|---|---|
| PSMA(前列腺癌特异性膜抗原) | 1 |
| FAP x PSMA | 1 |
关联
4
项与 Chongqing Medical University /The First Affiliated Hospital/ 相关的药物靶点- |
作用机制- |
在研机构 |
非在研适应症- |
最高研发阶段批准上市 |
首次获批国家/地区 美国 |
首次获批日期1987-05-05 |
作用机制 FAP调节剂 [+1] |
在研适应症 |
非在研适应症- |
最高研发阶段早期临床1期 |
首次获批国家/地区- |
首次获批日期- |
靶点- |
作用机制 PET imaging |
在研适应症 |
非在研适应症- |
最高研发阶段早期临床1期 |
首次获批国家/地区- |
首次获批日期- |
207
项与 Chongqing Medical University /The First Affiliated Hospital/ 相关的临床试验Research on Intraoperative Hypothermia Risk Prediction and Temperature Management Strategies in Elderly Patients: Construction of Intraoperative Hypothermia Prediction Model Based on Dynamic Incremental Training and Evaluation of Clinical Application Effectiveness
With the support of partial dual temperature monitoring (comparing the specific difference between standardized axillary temperature monitoring and esophageal temperature), this trial is divided into the following three parts:
1. Multi center observational study: Establish and validate a dynamic incremental training intraoperative hypothermia prediction model - Intelligent Care for the Elderly (ICE) - Intraoperative hypothermia warning system, and provide ICE Offline for use by healthcare professionals and ICE Online for further model updates when needed for clinical or research purposes.
2. Multi center non randomized controlled clinical trial: Conduct a multi center stratified temperature management clinical trial based on ICE Offline after dynamic incremental training to verify the clinical and economic benefits of the model and active warming.
3. Pre and post comparative study: Collect data before ICE application and compare it with data after ICE promotion.
1. Multi center observational study: Establish and validate a dynamic incremental training intraoperative hypothermia prediction model - Intelligent Care for the Elderly (ICE) - Intraoperative hypothermia warning system, and provide ICE Offline for use by healthcare professionals and ICE Online for further model updates when needed for clinical or research purposes.
2. Multi center non randomized controlled clinical trial: Conduct a multi center stratified temperature management clinical trial based on ICE Offline after dynamic incremental training to verify the clinical and economic benefits of the model and active warming.
3. Pre and post comparative study: Collect data before ICE application and compare it with data after ICE promotion.
开始日期2024-12-01 |
A Single-blind Randomized Controlled Trial to Evaluate Efficacy and Safety of Immersive Virtual Reality for Post-stroke Cognitive Impairment
This is a single-blind randomized controlled trial to evaluate the efficacy and safety of immersive virtual reality for post-stroke cognitive impairment.
开始日期2024-12-01 |
Effectiveness of Real Home Settings Via Virtual Reality Task Oriented Training on Upper Limb Function in Patients with Stroke
Stroke rank second among the top causes of death, affecting millions of people in the worldwide. It has been reported that hemiplegia is the most common sequelae after stroke, accounting for about 50%-70% of all sequelae of the disease. About 75% of stroke patients are accompanied by different degrees of upper limb dysfunction, which seriously affects the activities of daily life and cause serious physical and mental burden to patients and their families. Early recovery of upper limb motor function is a great significance for the overall recovery of stroke patients. Task-oriented training (TOT) is reported to improve the motor coordination and ADL. However, lack varies of tasks limited the treatment ability for patients with stroke hemiplegia during hospital admission. Virtual reality (VR) offers advantages of providing virtual scenes that is difficult in the real world, such as the scene of garden, camara, and plaza etc. And the familiar circumstances for patients may have the potential to increase the motivation of rehabilitation training, and improve the efficacy of occupational therapy (OT).
The goal of this study is to observe the effectiveness of real home settings via virtual reality assisted TOT on upper limb function in patients with stroke. Functional near-infrared spectroscopy (fNIRS) and electroencephalography (EEG) were used to observe the changes in brain function under VR-TOT training.
We intended to recruit 120 participants, and allocate to three groups: VR-TOT, TOT, and traditional OT. Each of them completed the Fugl-Meyer-UE, Wolf motor function test (WMFT), hand gripping power, modified Ashworth、Purdue Pegboard test (PPT)、modified Barthel index (MBI)、mini mental state examination (MMSE)、NIH stroke scale (NIHSS)、Virtual reality sickness questionnaire (VRSQ), Intrinsic Motivation Inventory Inventory (IMI), satisfaction VAS, body representation, sense of ownership, Proprioceptive Drift scale before and after the treatment. Additionally, we conducted fNIRS and EEG at baseline and during the follow up to understand the changes in brain function.
The goal of this study is to observe the effectiveness of real home settings via virtual reality assisted TOT on upper limb function in patients with stroke. Functional near-infrared spectroscopy (fNIRS) and electroencephalography (EEG) were used to observe the changes in brain function under VR-TOT training.
We intended to recruit 120 participants, and allocate to three groups: VR-TOT, TOT, and traditional OT. Each of them completed the Fugl-Meyer-UE, Wolf motor function test (WMFT), hand gripping power, modified Ashworth、Purdue Pegboard test (PPT)、modified Barthel index (MBI)、mini mental state examination (MMSE)、NIH stroke scale (NIHSS)、Virtual reality sickness questionnaire (VRSQ), Intrinsic Motivation Inventory Inventory (IMI), satisfaction VAS, body representation, sense of ownership, Proprioceptive Drift scale before and after the treatment. Additionally, we conducted fNIRS and EEG at baseline and during the follow up to understand the changes in brain function.
开始日期2024-11-01 |
申办/合作机构  山东大学齐鲁医院 山东大学齐鲁医院 [+2] |
100 项与 Chongqing Medical University /The First Affiliated Hospital/ 相关的临床结果
登录后查看更多信息
0 项与 Chongqing Medical University /The First Affiliated Hospital/ 相关的专利(医药)
登录后查看更多信息
100 项与 Chongqing Medical University /The First Affiliated Hospital/ 相关的药物交易
登录后查看更多信息
100 项与 Chongqing Medical University /The First Affiliated Hospital/ 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2024年12月23日管线快照
管线布局中药物为当前组织机构及其子机构作为药物机构进行统计,早期临床1期并入临床1期,临床1/2期并入临床2期,临床2/3期并入临床3期
临床前
1
3
早期临床1期
登录后查看更多信息
当前项目
| 药物(靶点) | 适应症 | 全球最高研发状态 |
|---|---|---|
[68Ga]Ga-Sa-DABI-4 | 肿瘤 更多 | 早期临床1期 |
99mTc-QULIC-5-P1 ( PSMA ) | PSMA阳性前列腺癌 更多 | 早期临床1期 |
68Ga-PSFA ( FAP x PSMA ) | PSMA阳性肿瘤 更多 | 早期临床1期 |
登录后查看更多信息
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
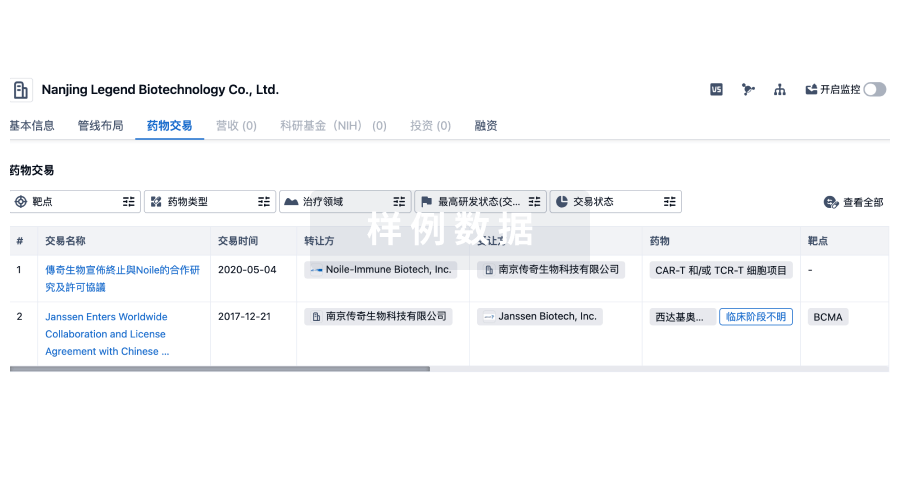
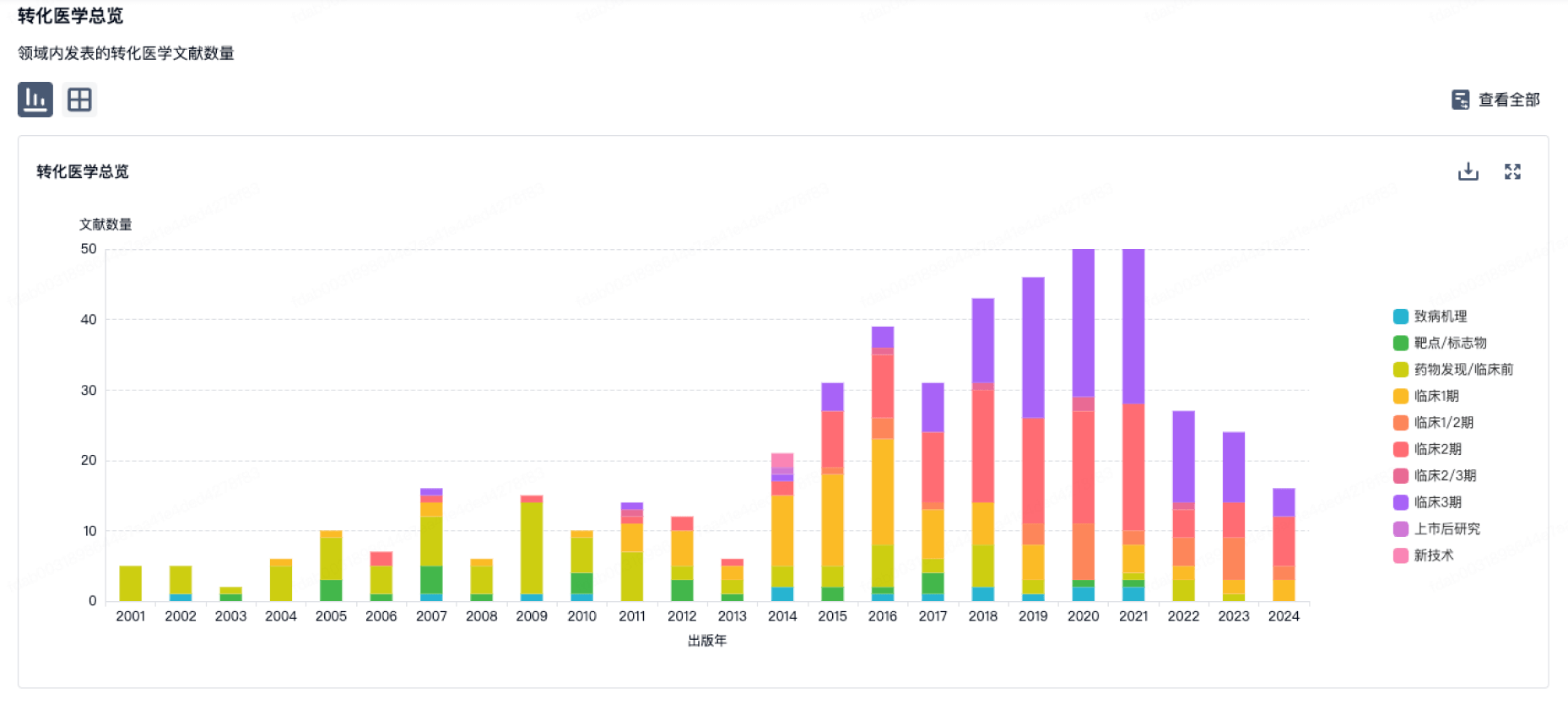
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
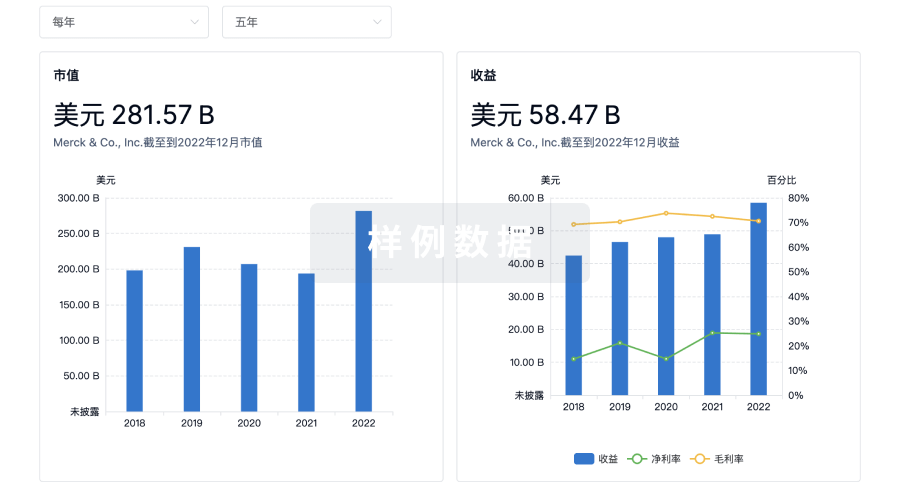
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
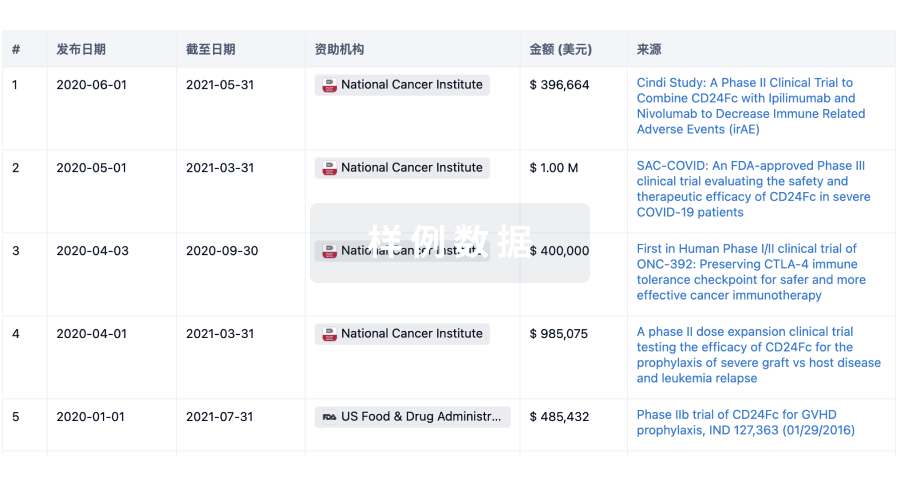
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
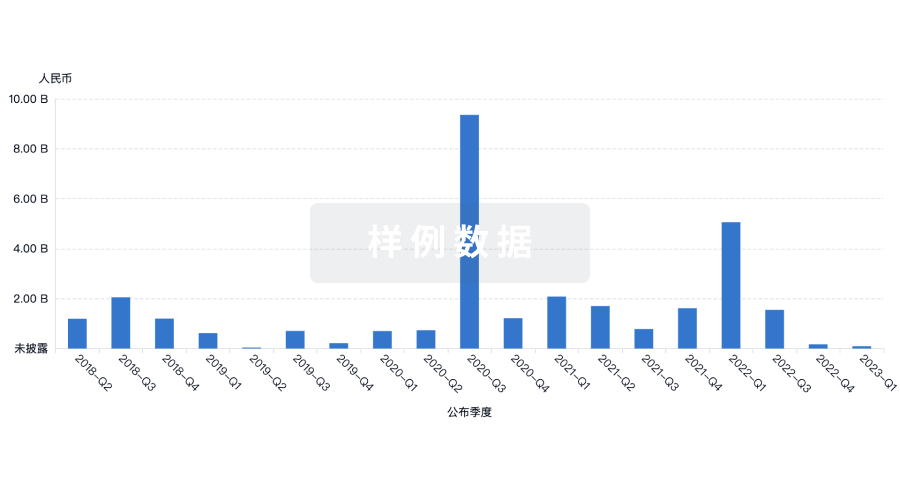
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
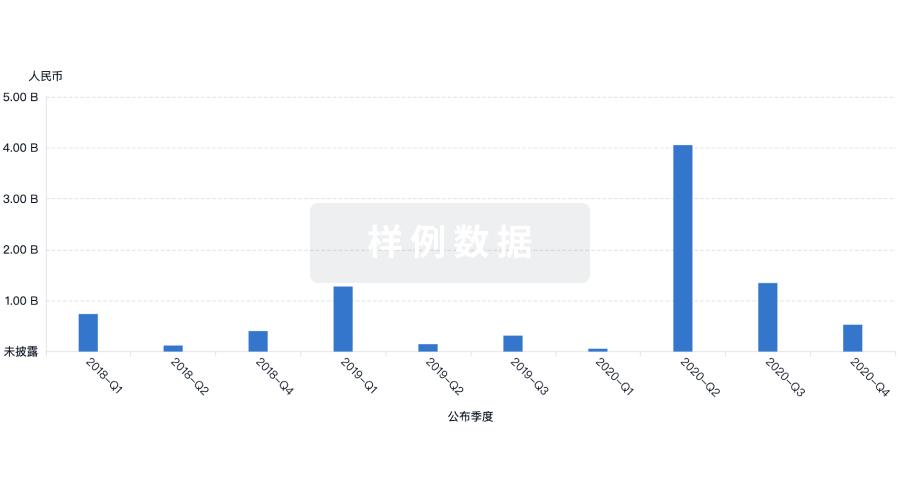
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
标准版
¥16800
元/账号/年
新药情报库 | 省钱又好用!
立即使用
来和芽仔聊天吧
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
