预约演示
更新于:2025-09-09
Jeonbuk National University Hospital
更新于:2025-09-09
概览
标签
神经系统疾病
其他疾病
免疫系统疾病
B细胞疗法
小分子化药
疾病领域得分
一眼洞穿机构专注的疾病领域
暂无数据
技术平台
公司药物应用最多的技术
暂无数据
靶点
公司最常开发的靶点
暂无数据
| 排名前五的药物类型 | 数量 |
|---|---|
| B细胞疗法 | 1 |
| 小分子化药 | 1 |
| 排名前五的靶点 | 数量 |
|---|---|
| RIPK1(受体相互作用的丝氨酸/苏氨酸蛋白激酶-1) | 1 |
| IL-27(白细胞介素-27) | 1 |
关联
2
项与 Jeonbuk National University Hospital 相关的药物靶点 |
作用机制 IL-27 agonists |
在研适应症 |
非在研适应症- |
最高研发阶段临床前 |
首次获批国家/地区- |
首次获批日期- |
靶点 |
作用机制 RIPK1抑制剂 |
在研适应症 |
非在研适应症- |
最高研发阶段临床前 |
首次获批国家/地区- |
首次获批日期- |
188
项与 Jeonbuk National University Hospital 相关的临床试验NCT06290271
Correlation Between Changes in Arterial Wall Shear Stress and Prognosis Following Acute Major Intracranial Artery Occlusion and Recanalization
There has been consistent research on the cerebral blood flow features in ischemic stroke patients with acute occlusion of major intracranial arteries. However, studies analyzing the overall features of the major intracranial artery blood flow in the periods of pre and post-recanalization are still lacking. Time-of-flight magnetic resonance angiography (TOF-MRA) is extensively utilized to evaluate the intracranial arteries. The arterial signal intensity from MRA-TOF varies across subjects and arterial subtypes, leading to the development of the Signal Intensity Gradient (SIG) concept. SIG has demonstrated a strong correlation with Computational Fluid Dynamics (CFD), a known method for reflecting wall shear stress. SIG could be associated with the pathophysiology of wall shear stress. We aim to investigate the blood flow patterns and characteristics in the periods of pre and post-recanalization using SIG.
开始日期2023-08-01 |
申办/合作机构 |
NCT06088121
Effects of a ATNC MDD-V1 (TMS With Cognitive Training), for the Treatment of Mild Alzheimer Disease: a Randomized, Double-blinded, Placebo-controlled Study
The study tests the effect of the ATNC MDD-V1 on Alzheimer patients' cognitive function. The ATNC MDD-V1 uses non-invasive stimulation of both magnetic and cognitive training.
开始日期2023-05-15 |
申办/合作机构 |
NCT05324800
This Study Was a 8 Weeks, Randomized, Double-blind, Placebo-controlled Human Trial to Evaluate the Efficacy and Safety of Curcuma Longa Extract Mixture on Immune Enhancement
This study was conducted to investigate the efficacy and safety of Curcuma longa extract mixture on immune enhancement
开始日期2022-02-04 |
100 项与 Jeonbuk National University Hospital 相关的临床结果
登录后查看更多信息
0 项与 Jeonbuk National University Hospital 相关的专利(医药)
登录后查看更多信息
2,678
项与 Jeonbuk National University Hospital 相关的文献(医药)2025-12-31·ANNALS OF MEDICINE
Aetiology of chronic liver disease is a valuable factor for stratifying adverse outcomes of acute decompensation: prospective observational study
Article
作者: Cheon, Gab Jin ; Jang, Jae-Young ; Yoo, Jeong Ju ; Kim, In Hee ; Jeong, Soung Won ; Song, Do Seon ; Kwon, Jung Hyun ; Nam, Seung Woo ; Kim, Hyoungsu ; Kim, Yoon Jun ; Sinn, Dong Hyun ; Kim, Tae Hyung ; Kim, Sang Gyune ; Sohn, Joo Hyun ; Lee, Sung Won ; Kim, Hwi Young ; Chae, Hee Bok ; Kim, Jung Hee ; Kim, Sung-Eun ; Jung, Young-Kul ; Suk, Ki Tae ; Yang, Jin Mo ; Seo, Yeon Seok ; Kim, Moon Young ; Cho, Ju Yeon ; Chung, Woo Jin ; Cho, Hyun Chin ; Kang, Seong Hee ; Kim, Ji Hoon ; Yoon, Eileen L. ; Kim, Won ; Park, Jung Gil ; Park, Ji Won ; Kim, Dong Joon ; Kim, Hee Yeon ; Yim, Hyung Joon ; Lee, Han Ah ; Kim, Byung Seok ; Jin, Young-Joo
BACKGROUND/AIMS:
Acute decompensation (AD) is defined as the development of complications related to portal hypertension and liver dysfunction that affect the progression of chronic liver disease (CLD) or liver cirrhosis (LC). Variations exist in patient demographics and prognostic outcomes of AD based on the aetiology of CLD, encompassing LC. However, limited research has been conducted to analyse these discrepancies across aetiologies.
METHODS:
The prospective Korean Acute-on-Chronic Liver Failure (KACLiF) cohort consisted of 1,501 patients who were hospitalized with AD of CLD from July 2015 to August 2018. In this study, we assess the clinical attributes and prognostic implications of AD with CLD/LC stratified by the aetiology.
RESULTS:
Among 1,501 patients, the mean age was 54.7 years old and 1,118 patients (74.5%) were men. The common events of AD were GI bleeding (35.3%) and jaundice (35.0%). There was a median follow-up of 8.0 months (1.0-16.0 months). The most common aetiology of CLD was alcohol (n = 1021), followed by viral hepatitis (n = 206), viral hepatitis with alcohol-related (n = 129), cryptogenic (n = 108) and autoimmune (n = 37). Viral hepatitis with alcohol-related CLD showed a poor liver function profile and a high frequency of acute-on-chronic liver failure (ACLF) [22.1% vs. 19.6% (alcohol CLD), 8.1% (viral CLD), 5.6% (autoimmune related CLD and 16.0% (cryptogenic CLD)] with worse adverse outcomes (mortality or liver transplantation) than other aetiologies. The difference in aetiology was a significant factor for 28-day adverse outcomes in multivariate analysis even in a high MELD score (≥15), which indicated poor baseline liver function and prognosis (p < 0.001).
CONCLUSION:
The aetiology of CLD constitutes a pivotal determinant influencing both short- and long-term adverse outcomes of AD in CLD, even among individuals presenting with elevated MELD scores. Notably, patients afflicted with viral hepatitis should exercise caution even in the consumption of modest quantities of alcohol that induced the exacerbations in the adverse outcomes associated with AD.
2025-12-01·LUNG
Impact of Multidrug-Resistant Bacterial Colonization on Clinical Characteristics, Antibiotic Treatment, and Clinical Outcomes of Hospital-Acquired Pneumonia
Article
作者: Park, Hye Kyeong ; Bae, Soohyun ; Shin, Beomsu ; Lee, Hyun-Kyung ; Kim, Changhwan ; Sim, Jae Kyeom ; Yoo, Kwang Ha ; Gil, Hyun-Il ; Baek, Ae-Rin ; Cho, Woo Hyun ; Oh, Jee Youn ; Min, Kyung Hoon ; Lee, Heung Bum ; Jeon, Kyeongman ; Kim, Jin Hyoung ; Moon, Jae Young ; Chang, Youjin ; Hong, Sang-Bum
PURPOSE:
To determine effects of colonization with multidrug-resistant bacteria (MDRB) in general wards on characteristics, treatment, and prognosis of hospital-acquired pneumonia (HAP).
METHODS:
This was a multicenter retrospective cohort study of patients with HAP admitted to 16 tertiary or university hospitals in Korea from July 2019 to December 2019. From the entire cohort, patients who developed pneumonia in general wards with known colonization status before the onset of pneumonia were included in this study. Patients were categorized into a colonization group and a non-colonization group according to MDRB colonization. Patients of the two groups were then compared.
RESULTS:
Among a total of 400 patients, 63 were in the MDRB colonization group. HAP caused by MDR-Staphylococcus aureus or MDR-Pseudomonas aeruginosa was more common in the colonization group than in the non-colonization group (24.4% vs. 8.1%, P = 0.006 or 20.0% vs. 5.4%, P = 0.013, respectively). Colonization with certain bacteria was correlated with subsequent infection with the same bacteria. Carbapenem use (36.5% vs. 24.3%, P = 0.044) and appropriateness of initial antibiotics (50.8% vs. 12.8%) were higher in the colonization group than in the non-colonization group. Although in-hospital mortality was similar in the two groups (34.9% vs. 32.9%, P = 0.759), hospital length of stay was longer (38 days vs. 31 days, P = 0.009) and rate of discharge to home was lower (34.1% vs 59.7%, P = 0.002) in the colonization group.
CONCLUSIONS:
Colonization with MDRB might influence characteristics and treatment of HAP. However, prognosis of HAP was not associated with MDRB colonization.
2025-10-01·BIOMEDICINE & PHARMACOTHERAPY
Taurine suppresses Aβ aggregation and attenuates Alzheimer’s disease pathologies in 5XFAD mice and patient-derived cerebral organoids
Article
作者: Shin, Soo Jung ; Hossain, Muhammad Kamal ; Son, Jeong Gyu ; Lee, Hyewon ; Moon, Minho ; Kim, Byeong-Hyeon ; Park, Hyun Ha ; Kumar, Vijay ; Kim, Hyung-Ryong ; Lee, Hwa-Young
Alzheimer's disease (AD) is marked by amyloid-beta (Aβ) plaque buildup, tau hyperphosphorylation, neuroinflammation, neuronal loss, and impaired adult hippocampal neurogenesis (AHN). Taurine has shown protective effects in various cellular and animal models of AD, though the molecular mechanisms of free taurine and its effects in patient-derived models remain underexplored. This study evaluates taurine's therapeutic potential using integrated in silico, in vitro, in vivo, and ex vivo approaches. In vitro aggregation assays revealed that taurine (10-100 μM) inhibited Aβ42 fibril formation, with transmission electron microscopy showing looser, amorphous fibrils, particularly at higher doses. Computational simulations further supported that taurine binds stably to Aβ peptide fragments and facilitates the dissociation of Aβ dimers. In HT22 cells, taurine protected against Aβ-induced cytotoxicity. In 5XFAD mice, oral administration of taurine (1000 mg/kg, 4 weeks) significantly reduced Aβ accumulation and hyperphosphorylation of tau at Ser202/Thr205 in the dorsal subiculum. Furthermore, taurine attenuated microgliosis, as evidenced by decreased Iba-1 immunoreactivity, protected against neurodegeneration demonstrated by preserving NeuN-positive neurons, and ameliorated deficit of AHN shown by increasing DCX-positive cells in the subgranular zone of the dentate gyrus. Importantly, in cerebral organoids derived from an AD patient carrying the APOE ε4/ε4 genotype, taurine treatment attenuated Aβ accumulation, decreased tau phosphorylation. These findings highlight taurine's multi-target therapeutic potential targeting amyloid aggregation, tau pathology, neuroinflammation and neurogenesis. Our data support taurine emerges as a promising therapeutic candidate for AD.
3
项与 Jeonbuk National University Hospital 相关的新闻(医药)2025-08-08
When added to a regimen of Rituxan and Revlimid (R2), AbbVie and Genmab’s Epkinly reduced the risk of disease progression or death by 79%.
Genmab and AbbVie are taking key steps toward moving their blood cancer drug Epkinly into earlier lines of treatment in follicular lymphoma (FL).On Thursday, Genmab reported results from a phase 3 trial showing that the addition of Epkinly to a regimen of Rituxan and Revlimid (R2) provided statistically significant and clinically meaningful improvements in overall response rate (ORR) and progression-free survival (PFS) in patients with relapsed or refractory FL.When compared to R2 alone, the Epkinly combo reduced the risk of disease progression or death by 79%, according to a pre-planned interim analysis.The detailed results will be presented at the American Society of Hematology (ASH) annual meeting in Orlando in December, Genmab said.In addition, Copenhagen-based Genmab said that the FDA last month accepted the partners' application—based on an earlier interim analysis of the trial—to approve Epkinly plus R2 following at least one prior systemic therapy in patients with relapsed or refractory FL. The U.S. regulator has established a decision date of November 30.With a nod, the combo would become the first bispecific antibody combination regimen available as a second-line option for patients with FL.“These important phase 3 results support our goal to move Epkinly into earlier lines of therapy in order to benefit more cancer patients,” Genmab CEO Jan van de Winkel, Ph.D., said in a quarterly conference call on Thursday. Also on the call, Genmab’s chief medical officer, Tahamtan Ahmadi, M.D., Ph.D., said that the data highlight Epkinly’s “potential to completely transform and disrupt the current treatment paradigm.”Epkinly was originally approved in 2023 to treat diffuse large B-cell lymphoma (DLBCL) after at least two lines of systemic therapy. Then a year ago, the FDA blessed Epkinly in FL after at least two lines of therapy.Epkinly isn’t the only CD20xCD3 T-cell engager to be approved for FL. Roche’s Lunsumio got there first in 2022 as a third-line treatment. Then in 2023, Roche’s Columvi, which is in the same drug class, earned a DLBCL nod. Last month, the FDA rejected the company’s bid to move Columvi into an earlier DLBCL treatment setting.Despite the competition in the class, AbbVie and Genmab's Epkinly boasts one edge as it's the only approved CD20xCD3 T-cell engager to be administered subcutaneously. Genmab reported Epkinly’s first half sales at $211 million for a 74% year-over-year increase. The company’s revenue for the first half came in at $1.64 billion, which was a 19% boost from the first half of 2024.

临床结果临床3期上市批准ASH会议
2025-07-30
In Study 2 of the pivotal Phase 3 UP-AA clinical program, upadacitinib (RINVOQ®) achieved the primary endpoint, demonstrating that 44.6% and 54.3% of patients with severe alopecia areata treated with upadacitinib 15 mg and 30 mg, respectively, reached 80% or more scalp hair coverage at week 24 as defined by the severity of alopecia tool (SALT) score ≤ 201 Key secondary endpoints, including improvements in eyebrows and eyelashes, as well as the percentage of subjects with 90% or more scalp coverage (SALT ≤ 10) and complete scalp hair coverage (SALT=0) at week 24, were also met1 The safety profile in alopecia areata was generally consistent with that in approved indications, and no new safety signals were identified in this study1 Results from the parallel replicate study (Study 1) of the Phase 3 UP-AA clinical program are also expected in the third quarter of 2025
NORTH CHICAGO, Ill., July 30, 2025 /PRNewswire/ -- AbbVie (NYSE: ABBV) today announced positive topline results from the first of two pivotal studies of the Phase 3 UP-AA clinical program evaluating the safety and efficacy of upadacitinib (RINVOQ®; 15 mg and 30 mg, once daily) in adult and adolescent patients with severe alopecia areata (AA) with a mean baseline SALT score of 83.8 (approximately 16% scalp hair coverage).1
In Study 2, both doses of upadacitinib achieved the primary endpoint, with 44.6% and 54.3% of patients treated with upadacitinib 15 mg and 30 mg, respectively, reaching 80% or more scalp hair coverage (SALT score ≤ 20) at week 24, compared to 3.4% of patients receiving placebo (p<0.001).1
"Often misunderstood as a cosmetic issue, AA is a systemic immune-mediated disease that can cause total hair loss, involving the scalp, eyebrows and eyelashes. People living with AA may face difficulties in managing their disease, which can significantly affect their quality of life," said Kori Wallace, M.D., Ph.D., vice president, global head of immunology clinical development, AbbVie. "UP-AA is the first pivotal program to have ranked and met the rigorous standard of SALT=0, indicating complete scalp hair regrowth. These data underscore AbbVie's commitment to advancing novel treatments that have the potential to improve the lives of individuals with immune-mediated diseases."
36.0% and 47.1% of patients treated with upadacitinib 15 mg and 30 mg, respectively, reached 90% or more scalp hair coverage (SALT ≤ 10), compared to 1.4% of patients receiving placebo at week 24 (p<0.001).1 Additional key secondary endpoints that were met included percentage of subjects with improvements in eyebrows and eyelashes, as well as the percentage of subjects with complete scalp hair coverage (SALT=0) with both doses of upadacitinib at week 24.1
"The sudden and often unpredictable hair loss people living with AA experience can profoundly impact their self-esteem and mental well-being," said Arash Mostaghimi, M.D., M.P.A., M.P.H., associate professor of dermatology and vice chair of clinical trials and innovation, Brigham & Women's Hospital, Harvard Medical School. "There is a pressing need for more treatments that help enable regrowth of scalp and non-scalp hair. I am encouraged by these results that demonstrate the potential of upadacitinib to be an important new treatment option."
The safety profile of both doses of upadacitinib in the 24-week, placebo-controlled period (Period A) was generally consistent with that observed in approved indications.1 Treatment-emergent serious adverse events occurred in 1.4% and 2.8% of patients in the upadacitinib 15 mg and 30 mg groups, respectively, and none in the placebo group.1 Discontinuations due to treatment-emergent adverse events (TEAEs) occurred in 0.7% and 1.4% of subjects in the upadacitinib 15 mg and 30 mg groups, respectively, and none in the placebo group.1 The most common TEAEs observed were acne, nasopharyngitis and upper respiratory tract infection.1 Serious infections were reported infrequently with 0.7% in the upadacitinib 15 mg group and 1.0% in the upadacitinib 30 mg group, and none in the placebo group.1 There were no adjudicated MACE, malignancies or deaths reported.1 One adjudicated venous thromboembolism was reported in the upadacitinib 15 mg group in a patient with multiple risk factors.1
Use of upadacitinib in AA is not approved and its safety and efficacy have not been evaluated by regulatory authorities.
About UP-AA Clinical Trial
UP-AA M23-716 was conducted as a single protocol that includes two replicate pivotal studies (Study 1 and Study 2) with randomization, investigative sites, data collection, analysis and reporting independent for each study. The Phase 3 randomized, placebo-controlled, double-blind studies evaluate efficacy and safety of upadacitinib in adult and adolescent subjects with severe alopecia areata. In Study 1 and Study 2 Period A, participants are randomized to one of three groups to receive upadacitinib 15 mg, upadacitinib 30 mg or placebo for 24 weeks. In Study 1 and Study 2 Period B, participants originally randomized to upadacitinib dose groups in Period A will continue their same treatment in Period B for 28 weeks. Participants originally randomized to placebo in Period A will either remain on placebo in Period B, or be randomized in one of two groups, based off of their SALT score at week 24. In total, Study 1 and Study 2 Periods A and B span 52 weeks. Participants who complete Study 1 or Study 2, can join Study 3 and may be re-randomized to receive 1 of 2 doses of upadacitinib for up to 108 weeks. The two trials randomized 1,399 participants with severe AA ages 12 to 64 across 248 sites worldwide. More information on this trial can be found at www.clinicaltrials.gov (NCT06012240).
About RINVOQ
Discovered and developed by AbbVie scientists, RINVOQ is a JAK inhibitor that is being studied in several immune-mediated inflammatory diseases. In human leukocyte cellular assays, RINVOQ inhibited cytokine-induced STAT phosphorylation mediated by JAK1 and JAK1/JAK3 more potently than JAK2/JAK2 mediated STAT phosphorylation.2 The relevance of inhibition of specific JAK enzymes to therapeutic effectiveness and safety is not currently known.
Upadacitinib (RINVOQ) is being studied in Phase 3 clinical trials for alopecia areata, hidradenitis suppurativa, Takayasu arteritis, systemic lupus erythematosus and vitiligo.3,4,5,6,7
RINVOQ (upadacitinib) U.S. Uses and Important Safety Information1
RINVOQ is a prescription medicine used to treat:
Adults with moderate to severe rheumatoid arthritis (RA) when 1 or more medicines called tumor necrosis factor (TNF) blockers have been used, and did not work well or could not be tolerated. Adults with active psoriatic arthritis (PsA) when 1 or more medicines called TNF blockers have been used, and did not work well or could not be tolerated. Adults with active ankylosing spondylitis (AS) when 1 or more medicines called TNF blockers have been used, and did not work well or could not be tolerated. Adults with active non-radiographic axial spondyloarthritis (nr-axSpA) with objective signs of inflammation when a TNF blocker medicine has been used, and did not work well or could not be tolerated. Adults with giant cell arteritis (GCA). Adults with moderate to severe ulcerative colitis (UC) when 1 or more medicines called TNF blockers have been used, and did not work well or could not be tolerated. Adults with moderate to severe Crohn's disease (CD) when 1 or more medicines called TNF blockers have been used, and did not work well or could not be tolerated.
It is not known if RINVOQ is safe and effective in children with ankylosing spondylitis, non-radiographic axial spondyloarthritis, ulcerative colitis, or Crohn's disease.
Adults and children 12 years of age and older with moderate to severe eczema (atopic dermatitis [AD]) that did not respond to previous treatment and their eczema is not well controlled with other pills or injections, including biologic medicines, or the use of other pills or injections is not recommended.
It is not known if RINVOQ is safe and effective in children under 12 years of age with atopic dermatitis.
It is not known if RINVOQ LQ is safe and effective in children with atopic dermatitis.
RINVOQ/RINVOQ LQ is a prescription medicine used to treat:
Children 2 years of age and older with active polyarticular juvenile idiopathic arthritis (pJIA) when 1 or more medicines called TNF blockers have been used, and did not work well or could not be tolerated. Children 2 to less than 18 years of age with active psoriatic arthritis (PsA) when 1 or more medicines called TNF blockers have been used, and did not work well or could not be tolerated.
It is not known if RINVOQ/RINVOQ LQ is safe and effective in children under 2 years of age with polyarticular juvenile idiopathic arthritis or psoriatic arthritis.
IMPORTANT SAFETY INFORMATION FOR RINVOQ/RINVOQ LQ (upadacitinib)
What is the most important information I should know about RINVOQ<*>?
RINVOQ may cause serious side effects, including:
Serious infections. RINVOQ can lower your ability to fight infections. Serious infections have happened while taking RINVOQ, including tuberculosis (TB) and infections caused by bacteria, fungi, or viruses that can spread throughout the body. Some people have died from these infections. Your healthcare provider (HCP) should test you for TB before starting RINVOQ and check you closely for signs and symptoms of TB during treatment with RINVOQ. You should not start taking RINVOQ if you have any kind of infection unless your HCP tells you it is okay. If you get a serious infection, your HCP may stop your treatment until your infection is controlled. You may be at higher risk of developing shingles (herpes zoster). Increased risk of death in people 50 years and older who have at least 1 heart disease (cardiovascular) risk factor. Cancer and immune system problems. RINVOQ may increase your risk of certain cancers. Lymphoma and other cancers, including skin cancers, can happen. Current or past smokers are at higher risk of certain cancers, including lymphoma and lung cancer. Follow your HCP's advice about having your skin checked for skin cancer during treatment with RINVOQ. Limit the amount of time you spend in sunlight. Wear protective clothing when you are in the sun and use sunscreen. Increased risk of major cardiovascular (CV) events, such as heart attack, stroke, or death, in people 50 years and older who have at least 1 heart disease (CV) risk factor, especially if you are a current or past smoker. Blood clots. Blood clots in the veins of the legs or lungs and arteries can happen with RINVOQ. This may be life-threatening and cause death. Blood clots in the veins of the legs and lungs have happened more often in people who are 50 years and older and with at least 1 heart disease (CV) risk factor. Allergic reactions. Symptoms such as rash (hives), trouble breathing, feeling faint or dizzy, or swelling of your lips, tongue, or throat, that may mean you are having an allergic reaction have been seen in people taking RINVOQ. Some of these reactions were serious. If any of these symptoms occur during treatment with RINVOQ, stop taking RINVOQ and get emergency medical help right away. Tears in the stomach or intestines. This happens most often in people who take nonsteroidal anti-inflammatory drugs (NSAIDs) or corticosteroids. Get medical help right away if you get stomach-area pain, fever, chills, nausea, or vomiting. Changes in certain laboratory tests. Your HCP should do blood tests before you start taking RINVOQ and while you take it. Your HCP may stop your RINVOQ treatment for a period of time if needed because of changes in these blood test results.
Do not take RINVOQ if you are allergic to upadacitinib or any of the ingredients in RINVOQ. See the Medication Guide or Consumer Brief Summary for a complete list of ingredients.
What should I tell my HCP BEFORE starting RINVOQ?
Tell your HCP if you:
Are being treated for an infection, have an infection that won't go away or keeps coming back, or have symptoms of an infection, such as:
̶ Fever, sweating, or chills
̶ Shortness of breath
̶ Warm, red, or painful skin or sores on your body
̶ Muscle aches
̶ Feeling tired
̶ Blood in phlegm
̶ Diarrhea or stomach pain
̶ Cough
̶ Weight loss
̶ Burning when urinating or urinating more often than normal
Have TB or have been in close contact with someone with TB. Are a current or past smoker. Have had a heart attack, other heart problems, or stroke. Have or have had any type of cancer, hepatitis B or C, shingles (herpes zoster), blood clots in the veins of your legs or lungs, diverticulitis (inflammation in parts of the large intestine), or ulcers in your stomach or intestines. Have other medical conditions, including liver problems, low blood cell counts, diabetes, chronic lung disease, HIV, or a weak immune system. Live, have lived, or have traveled to parts of the country, such as the Ohio and Mississippi River valleys and the Southwest, that increase your risk of getting certain kinds of fungal infections. If you are unsure if you've been to these types of areas, ask your HCP. Have recently received or are scheduled to receive a vaccine. People who take RINVOQ should not receive live vaccines. Are pregnant or plan to become pregnant. Based on animal studies, RINVOQ may harm your unborn baby. Your HCP will check whether or not you are pregnant before you start RINVOQ. You should use effective birth control (contraception) to avoid becoming pregnant during treatment with RINVOQ and for 4 weeks after your last dose. There is a pregnancy surveillance program for RINVOQ. The purpose of the program is to collect information about the health of you and your baby. If you become pregnant while taking RINVOQ, you are encouraged to report the pregnancy by calling 1-800-633-9110. Are breastfeeding or plan to breastfeed. RINVOQ may pass into your breast milk. Do not breastfeed during treatment with RINVOQ and for 6 days after your last dose.
Tell your HCP about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. RINVOQ and other medicines may affect each other, causing side effects.
Especially tell your HCP if you take:
Medicines for fungal or bacterial infections Rifampicin or phenytoin Medicines that affect your immune system
If you are not sure if you are taking any of these medicines, ask your HCP or pharmacist.
What should I avoid while taking RINVOQ?
Avoid food or drink containing grapefruit during treatment with RINVOQ as it may increase the risk of side effects.
What should I do or tell my HCP AFTER starting RINVOQ?
Tell your HCP right away if you have any symptoms of an infection. RINVOQ can make you more likely to get infections or make any infections you have worse. Get emergency help right away if you have any symptoms of a heart attack or stroke while taking RINVOQ, including: Discomfort in the center of your chest that lasts for more than a few minutes or that goes away and comes back Severe tightness, pain, pressure, or heaviness in your chest, throat, neck, or jaw Pain or discomfort in your arms, back, neck, jaw, or stomach Shortness of breath with or without chest discomfort Breaking out in a cold sweat Nausea or vomiting Feeling lightheaded Weakness in one part or on one side of your body Slurred speech Tell your HCP right away if you have any signs or symptoms of blood clots during treatment with RINVOQ, including:
Discomfort in the center of your chest that lasts for more than a few minutes or that goes away and comes back Severe tightness, pain, pressure, or heaviness in your chest, throat, neck, or jaw Pain or discomfort in your arms, back, neck, jaw, or stomach Shortness of breath with or without chest discomfort Breaking out in a cold sweat Nausea or vomiting Feeling lightheaded Weakness in one part or on one side of your body Slurred speech
̶ Swelling
̶ Pain or tenderness in one or both legs
̶ Sudden unexplained chest or upper back pain
̶ Shortness of breath or difficulty breathing
Tell your HCP right away if you have a fever or stomach-area pain that does not go away, and a change in your bowel habits.
What are other possible side effects of RINVOQ?
Common side effects include upper respiratory tract infections (common cold, sinus infections), shingles (herpes zoster), herpes simplex virus infections (including cold sores), bronchitis, nausea, cough, fever, acne, headache, swelling of the feet and hands (peripheral edema), increased blood levels of creatine phosphokinase, allergic reactions, inflammation of hair follicles, stomach-area (abdominal) pain, increased weight, flu, tiredness, lower number of certain types of white blood cells (neutropenia, lymphopenia, leukopenia), muscle pain, flu-like illness, rash, increased blood cholesterol levels, increased liver enzyme levels, pneumonia, low number of red blood cells (anemia), and infection of the stomach and intestine (gastroenteritis).
A separation or tear to the lining of the back part of the eye (retinal detachment) has happened in people with atopic dermatitis treated with RINVOQ. Call your HCP right away if you have any sudden changes in your vision during treatment with RINVOQ.
Some people taking RINVOQ may see medicine residue (a whole tablet or tablet pieces) in their stool. If this happens, call your HCP.
These are not all the possible side effects of RINVOQ.
How should I take RINVOQ/RINVOQ LQ?
RINVOQ is taken once a day with or without food. Do not split, crush, or chew the tablet. Take RINVOQ exactly as your HCP tells you to use it. RINVOQ is available in 15 mg, 30 mg, and 45 mg extended-release tablets. RINVOQ LQ is taken twice a day with or without food. RINVOQ LQ is available in a 1 mg/mL oral solution. RINVOQ LQ is not the same as RINVOQ tablets. Do not switch between RINVOQ LQ and RINVOQ tablets unless the change has been made by your HCP.
<*>Unless otherwise stated, "RINVOQ" in the IMPORTANT SAFETY INFORMATION refers to RINVOQ and RINVOQ LQ.
This is the most important information to know about RINVOQ. For more information, talk to your HCP.
You are encouraged to report negative side effects of prescription drugs to the FDA. Visit www.fda.gov/medwatch or call 1-800-FDA-1088.
If you are having difficulty paying for your medicine, AbbVie may be able to help. Visit AbbVie.com/PatientAccessSupport to learn more.
Please click here for the Full Prescribing Information and Medication Guide.
Globally, prescribing information varies; refer to the individual country product label for complete information.
About AbbVieAbbVie's mission is to discover and deliver innovative medicines and solutions that solve serious health issues today and address the medical challenges of tomorrow. We strive to have a remarkable impact on people's lives across several key therapeutic areas including immunology, oncology, neuroscience and eye care – and products and services in our Allergan Aesthetics portfolio. For more information about AbbVie, please visit us at www.abbvie.com. Follow @abbvie on LinkedIn, Facebook, Instagram, X (formerly Twitter) and YouTube.
Forward-Looking Statements Some statements in this news release are, or may be considered, forward-looking statements for purposes of the Private Securities Litigation Reform Act of 1995. The words "believe," "expect," "anticipate," "project" and similar expressions and uses of future or conditional verbs, generally identify forward-looking statements. AbbVie cautions that these forward-looking statements are subject to risks and uncertainties that may cause actual results to differ materially from those expressed or implied in the forward-looking statements. Such risks and uncertainties include, but are not limited to, challenges to intellectual property, competition from other products, difficulties inherent in the research and development process, adverse litigation or government action, changes to laws and regulations applicable to our industry, the impact of global macroeconomic factors, such as economic downturns or uncertainty, international conflict, trade disputes and tariffs, and other uncertainties and risks associated with global business operations. Additional information about the economic, competitive, governmental, technological and other factors that may affect AbbVie's operations is set forth in Item 1A, "Risk Factors," of AbbVie's 2024 Annual Report on Form 10-K, which has been filed with the Securities and Exchange Commission, as updated by its Quarterly Reports on Form 10-Q and in other documents that AbbVie subsequently files with the Securities and Exchange Commission that update, supplement or supersede such information. AbbVie undertakes no obligation, and specifically declines, to release publicly any revisions to forward-looking statements as a result of subsequent events or developments, except as required by law.
Media:
Lindsay Cangemi
lindsay.cangemi@abbvie.com
Investors:
Liz Shea
liz.shea@abbvie.com
______________________________
1 AbbVie. Data on file ABVRRTI81456.
2 RINVOQ [Package Insert]. North Chicago, IL: AbbVie Inc.; 2025.
3 A Study to Evaluate the Efficacy and Safety of Upadacitinib in Participants with Takaysu Arteritis (TAK) (SELECT-TAK). ClinicalTrials.gov. Available at: https://clinicaltrials.gov/study/NCT04161898. Accessed January 15, 2025.
4 Program to Assess Adverse Events and Change in Disease Activity of Oral Upadacitinib in Adult Participants With Moderate to Severe Systemic Lupus Erythematosus (SELECT-SLE). ClinicalTrials.gov. Available at: https://clinicaltrials.gov/study/NCT05843643. Accessed January 15, 2025.
5 A Study to Assess Change in Disease Activity and Adverse Events of Oral Upadacitinib in Adult and Adolescent Participants With Moderate to Severe Hidradenitis Suppurativa Who Have Failed Anti-TNF Therapy (Step-Up HS). ClinicalTrials.gov. Available at: https://clinicaltrials.gov/study/NCT05889182. Accessed January 15, 2025.
6 A Study To Assess Adverse Events and Effectiveness of Upadacitinib Oral Tablets in Adult and Adolescent Participants With Vitiligo (Viti-Up). ClinicalTrials.gov. Available at: https://clinicaltrials.gov/study/NCT06118411. Accessed January 15, 2025.
7 A Study to Evaluate the Safety and Effectiveness of Upadacitinib Tablets in Adult and Adolescent Participants With Severe Alopecia Areata (Up-AA). ClinicalTrials.gov. Available at: https://clinicaltrials.gov/study/NCT06012240. Accessed January 15, 2025.
SOURCE AbbVie
临床结果临床3期临床2期
2025-05-02
COPENHAGEN, Denmark--(BUSINESS WIRE)--Genmab A/S (Nasdaq: GMAB) announced today its intention to submit in the first half of 2025 a supplemental Biologics License Application (sBLA) to the U.S. Food and Drug Administration (FDA) for subcutaneous epcoritamab, a bispecific antibody being investigated in combination with rituximab and lenalidomide (R2) for the treatment of adult patients with relapsed or refractory (R/R) follicular lymphoma (FL), following at least one prior systemic therapy.
The decision to submit the sBLA is supported by positive topline results from the Phase 3 EPCORE FL-1 trial evaluating epcoritamab plus R2 versus R2 alone in adult patients with R/R FL. Based on an interim analysis conducted by an Independent Data Monitoring Committee (IDMC) review, the study met one of its dual primary endpoints of ORR (Complete Response plus Partial Response, p-value < 0.0001). The safety profile of epcoritamab plus R2 in adult patients with R/R FL was consistent with the known safety profiles of the individual regimens (epcoritamab and R2) and as presented in the U.S. prescribing information for epcoritamab. No new safety signals were observed. The full results will be submitted later this year for presentation at an upcoming medical congress and discussed with global regulatory authorities.
“We are pleased with the strength of the data that allows us to submit a supplemental Biologics License Application in accordance with the U.S. FDA’s Project Frontrunner, which supports our commitment to advance novel medicines to patients who need them. The interim topline results demonstrate the potential of this investigational epcoritamab combination regimen to treat relapsed or refractory follicular lymphoma patients,” said Jan van de Winkel, Ph.D., Chief Executive Officer, Genmab. “This milestone represents our commitment to the ongoing development of epcoritamab, with our partner AbbVie, and we look forward to seeing the full results from the study.”
Use of epcoritamab plus R2 in R/R FL is not approved in the U.S., in the EU or in any other territory. The safety and efficacy of epcoritamab for use as a combination therapy in FL have not been established. Epcoritamab is currently approved by the FDA under Accelerated Approval as a monotherapy for the treatment of adults with R/R FL after two or more lines of systemic therapy.
About Follicular Lymphoma (FL)
FL is typically an indolent (or slow-growing) form of non-Hodgkin's lymphoma (NHL) that arises from B-lymphocytes and is the second most common form of NHL accounting for 20-30 percent of all cases.i About 15,000 people develop FL each year in the U.S.ii and it is considered incurable with current standard of care therapies.iii Patients often relapse and, with each relapse the remission and time to next treatment is shorter.iv Over time, transformation to diffuse large B-cell lymphoma (DLBCL), an aggressive form of NHL associated with poor survival outcomes, can occur in more than 25 percent of FL patients.v
About the EPCORE FL-1 Trial
EPCORE FL-1 (NCT05409066) is a Phase 3 open-label interventional trial to evaluate the safety and efficacy of epcoritamab plus rituximab and lenalidomide (R2) versus R2 alone in patients with relapsed/refractory (R/R) follicular lymphoma (FL). The dual primary endpoints are ORR and progression-free survival assessed by independent review committee (IRC) per Lugano criteria.
About Epcoritamab
Epcoritamab is an IgG1-bispecific antibody created using Genmab's proprietary DuoBody® technology and administered subcutaneously. Genmab's DuoBody-CD3 technology is designed to direct cytotoxic T cells selectively to elicit an immune response toward target cell types. Epcoritamab is designed to simultaneously bind to CD3 on T cells and CD20 on B cells and induces T-cell-mediated killing of CD20+ cells.vi
Epcoritamab (approved under the brand name EPKINLY® in the U.S. and Japan, and TEPKINLY® in the EU) has received regulatory approval in certain lymphoma indications in several territories. Epcoritamab is being co-developed by Genmab and AbbVie as part of the companies' oncology collaboration. The companies will share commercial responsibilities in the U.S. and Japan, with AbbVie responsible for further global commercialization. Both companies will pursue additional international regulatory approvals for the investigational R/R FL indication and additional approvals for the R/R DLBCL indication.
Genmab and AbbVie continue to evaluate the use of epcoritamab as a monotherapy, and in combination, across lines of therapy in a range of hematologic malignancies. This includes five ongoing Phase 3, open-label, randomized trials including a trial evaluating epcoritamab as a monotherapy in patients with R/R DLBCL compared to investigators choice chemotherapy (NCT04628494), a trial evaluating epcoritamab in combination with R-CHOP in adult patients with newly diagnosed DLBCL (NCT05578976), a trial evaluating epcoritamab in combination with rituximab and lenalidomide (R2) in patients with R/R FL (NCT05409066), a trial evaluating epcoritamab in combination with rituximab and lenalidomide (R2) compared to chemoimmunotherapy in patients with previously untreated FL (NCT06191744), and a trial evaluating epcoritamab in combination with lenalidomide compared to chemotherapy infusion in patients with R/R DLBCL (NCT06508658). The safety and efficacy of epcoritamab has not been established for these investigational uses. Please visit www.clinicaltrials.gov for more information.
EPKINLY™ (epcoritamab-bysp) U.S. INDICATIONS & IMPORTANT SAFETY INFORMATION
What is EPKINLY?
EPKINLY is a prescription medicine used to treat adults with certain types of diffuse large B-cell lymphoma (DLBCL), high-grade B-cell lymphoma, or follicular lymphoma (FL) that has come back or that did not respond to previous treatment after receiving 2 or more treatments. EPKINLY is approved based on patient response data. Studies are ongoing to confirm the clinical benefit of EPKINLY. It is not known if EPKINLY is safe and effective in children.
IMPORTANT SAFETY INFORMATION
Important Warnings—EPKINLY can cause serious side effects, including:
Cytokine release syndrome (CRS) , which is common during treatment with EPKINLY and can be serious or life threatening. To help reduce your risk of CRS, you will receive EPKINLY on a step-up dosing schedule (when you receive 2 or 3 smaller step-up doses of EPKINLY before your first full dose during your first cycle of treatment), and you may also receive other medicines before and for 3 days after receiving EPKINLY. If your dose of EPKINLY is delayed for any reason, you may need to repeat the step-up dosing schedule.
Neurologic problems that can be life-threatening and lead to death. Neurologic problems may happen days or weeks after you receive EPKINLY.
People with DLBCL or high-grade B-cell lymphoma should be hospitalized for 24 hours after receiving their first full dose of EPKINLY on day 15 of cycle 1 due to the risk of CRS and neurologic problems.
Tell your healthcare provider or get medical help right away if you develop a fever of 100.4°F (38°C) or higher; dizziness or lightheadedness; trouble breathing; chills; fast heartbeat; feeling anxious; headache; confusion; shaking (tremors); problems with balance and movement, such as trouble walking; trouble speaking or writing; confusion and disorientation; drowsiness, tiredness or lack of energy; muscle weakness; seizures; or memory loss. These may be symptoms of CRS or neurologic problems. If you have any symptoms that impair consciousness, do not drive or use heavy machinery or do other dangerous activities until your symptoms go away.
EPKINLY can cause other serious side effects, including:
Infections that may lead to death. Your healthcare provider will check you for signs and symptoms of infection before and during treatment and treat you as needed if you develop an infection. You should receive medicines from your healthcare provider before you start treatment to help prevent infection. Tell your healthcare provider right away if you develop any symptoms of infection during treatment, including fever of 100.4°F (38°C) or higher, cough, chest pain, tiredness, shortness of breath, painful rash, sore throat, pain during urination, or feeling weak or generally unwell.
Low blood cell counts , which can be serious or severe. Your healthcare provider will check your blood cell counts during treatment. EPKINLY may cause low blood cell counts, including low white blood cells (neutropenia), which can increase your risk for infection; low red blood cells (anemia), which can cause tiredness and shortness of breath; and low platelets (thrombocytopenia), which can cause bruising or bleeding problems. Your healthcare provider will monitor you for symptoms of CRS, neurologic problems, infections, and low blood cell counts during treatment with EPKINLY.
Your healthcare provider may temporarily stop or completely stop treatment with EPKINLY if you develop certain side effects.
Before you receive EPKINLY, tell your healthcare provider about all your medical conditions, including if you have an infection, are pregnant or plan to become pregnant, or are breastfeeding or plan to breastfeed. If you receive EPKINLY while pregnant, it may harm your unborn baby. If you are a female who can become pregnant, your healthcare provider should do a pregnancy test before you start treatment with EPKINLY and you should use effective birth control (contraception) during treatment and for 4 months after your last dose of EPKINLY. Tell your healthcare provider if you become pregnant or think that you may be pregnant during treatment with EPKINLY. Do not breastfeed during treatment with EPKINLY and for 4 months after your last dose of EPKINLY.
In DLBCL or high-grade B-cell lymphoma, the most common side effects of EPKINLY include CRS, tiredness, muscle and bone pain, injection site reactions, fever, stomach-area (abdominal) pain, nausea, and diarrhea. The most common severe abnormal laboratory test results include decreased white blood cells, decreased red blood cells, and decreased platelets.
In follicular lymphoma the most common side effects of EPKINLY include injection site reactions, CRS, COVID-19, tiredness, upper respiratory tract infections, muscle and bone pain, rash, diarrhea, fever, cough, and headache. The most common severe abnormal laboratory test results include decreased white blood cells and decreased red blood cells.
These are not all of the possible side effects of EPKINLY. Call your doctor for medical advice about side effects. You are encouraged to report side effects to the FDA at (800) FDA-1088 or www.fda.gov/medwatch or to Genmab US, Inc. at 1-855-4GENMAB (1-855-443-6622).
Please see Medication Guide, including Important Warnings.
Globally, prescribing information varies; refer to the individual country product label for complete information.
About Genmab
Genmab is an international biotechnology company with a core purpose of guiding its unstoppable team to strive toward improving the lives of patients with innovative and differentiated antibody therapeutics. For more than 25 years, its passionate, innovative and collaborative team has invented next-generation antibody technology platforms and leveraged translational, quantitative and data sciences, resulting in a proprietary pipeline including bispecific T-cell engagers, antibody-drug conjugates, next-generation immune checkpoint modulators and effector function-enhanced antibodies. By 2030, Genmab’s vision is to transform the lives of people with cancer and other serious diseases with knock-your-socks-off (KYSO) antibody medicines®.
Established in 1999, Genmab is headquartered in Copenhagen, Denmark, with international presence across North America, Europe and Asia Pacific. For more information, please visit Genmab.com and follow us on LinkedIn and X.
This Company Announcement contains forward looking statements. The words “believe,” “expect,” “anticipate,” “intend” and “plan” and similar expressions identify forward looking statements. Actual results or performance may differ materially from any future results or performance expressed or implied by such statements. The important factors that could cause our actual results or performance to differ materially include, among others, risks associated with preclinical and clinical development of products, uncertainties related to the outcome and conduct of clinical trials including unforeseen safety issues, uncertainties related to product manufacturing, the lack of market acceptance of our products, our inability to manage growth, the competitive environment in relation to our business area and markets, our inability to attract and retain suitably qualified personnel, the unenforceability or lack of protection of our patents and proprietary rights, our relationships with affiliated entities, changes and developments in technology which may render our products or technologies obsolete, and other factors. For a further discussion of these risks, please refer to the risk management sections in Genmab’s most recent financial reports, which are available on www.genmab.com and the risk factors included in Genmab’s most recent Annual Report on Form 20-F and other filings with the U.S. Securities and Exchange Commission (SEC), which are available at www.sec.gov. Genmab does not undertake any obligation to update or revise forward looking statements in this Company Announcement nor to confirm such statements to reflect subsequent events or circumstances after the date made or in relation to actual results, unless required by law.
Genmab A/S and/or its subsidiaries own the following trademarks: Genmab®; the Y-shaped Genmab logo®; Genmab in combination with the Y-shaped Genmab logo®; HuMax®; DuoBody®; HexaBody®; DuoHexaBody®, HexElect® and KYSO®. EPCORE®, EPKINLY®, TEPKINLY® and their designs are trademarks of AbbVie Biotechnology Ltd.
i Lymphoma Research Foundation official website. https://lymphoma.org/aboutlymphoma/nhl/fl/. Accessed November 2024.
ii Leukemia & Lymphoma Society. https://www.lls.org/research/follicular-lymphoma-fl. Accessed November 2024.
iii Ghione P, Palomba ML, Ghesquieres H, et al. Treatment patterns and outcomes in relapsed/refractory follicular lymphoma: results from the international SCHOLAR-5 study. Haematologica. 2023;108(3):822-832. doi: 10.3324/haematol.2022.281421.
iv Rivas-Delgado A, Magnano L, Moreno-Velázquez M, et al. Response duration and survival shorten after each relapse in patients with follicular lymphoma treated in the rituximab era. Br J Haematol. 2018;184(5):753-759. doi:10.1111/bjh.15708.
v Al-Tourah AJ, Gill KK, Chhanabhai M, et al. Population-based analysis of incidence and outcome of transformed non-Hodgkin's lymphoma. J Clin Oncol. 2008 Nov 10;26(32):5165-9. doi: 10.1200/JCO.2008.16.0283. Epub 2008 Oct 6. PMID: 18838711.
vi Engelberts PJ, et al. DuoBody-CD3xCD20 Induces Potent T-Cell-Mediated Killing of Malignant B Cells in Preclinical Models and Provides Opportunities for Subcutaneous Dosing. EBioMedicine. 2020;52:102625. doi: 10.1016/j.ebiom.2019.102625.
临床3期临床结果上市批准免疫疗法
100 项与 Jeonbuk National University Hospital 相关的药物交易
登录后查看更多信息
100 项与 Jeonbuk National University Hospital 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2025年09月28日管线快照
管线布局中药物为当前组织机构及其子机构作为药物机构进行统计,早期临床1期并入临床1期,临床1/2期并入临床2期,临床2/3期并入临床3期
临床前
2
4
其他
登录后查看更多信息
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
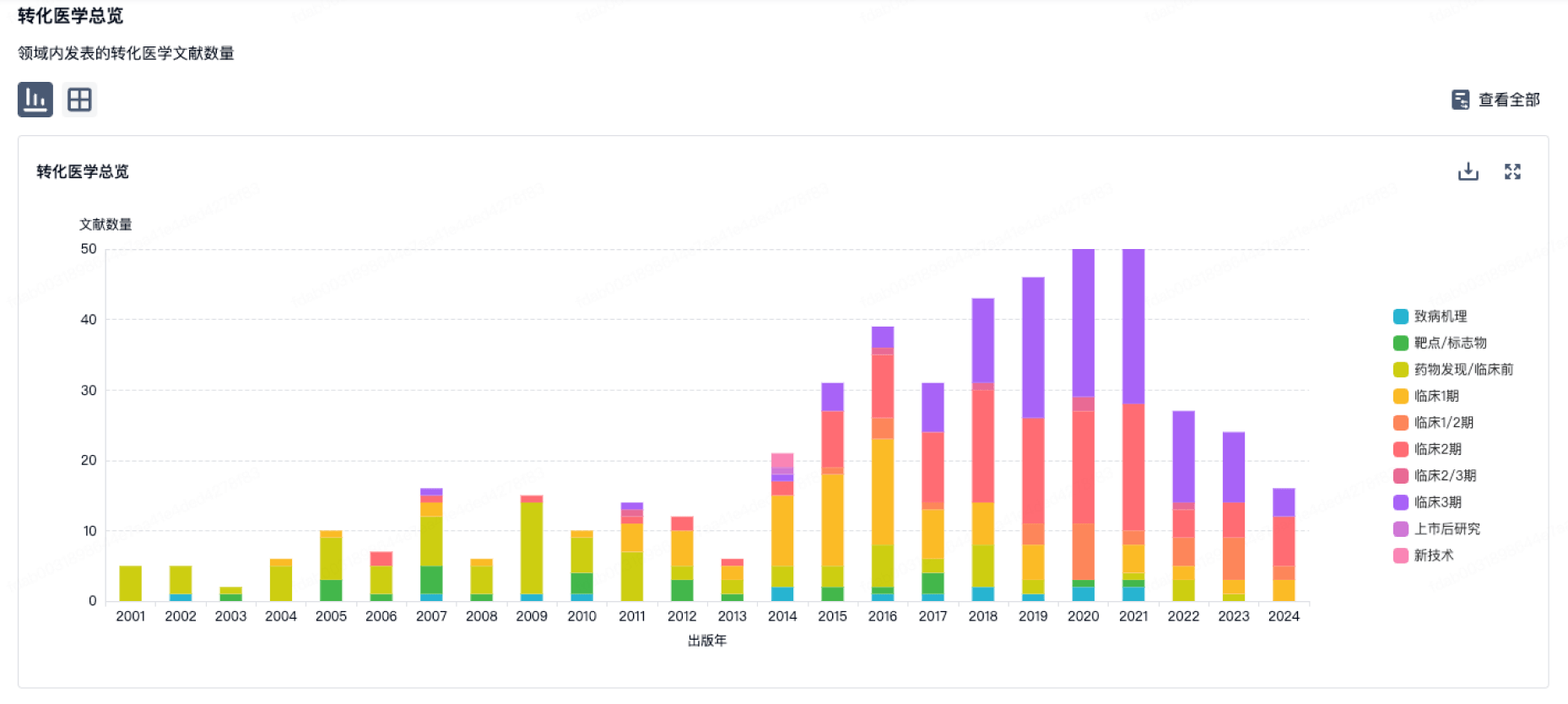
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
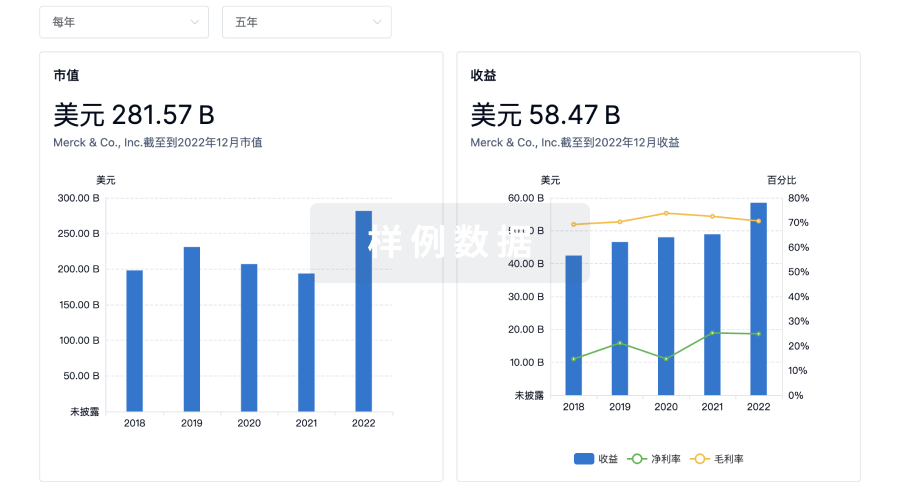
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
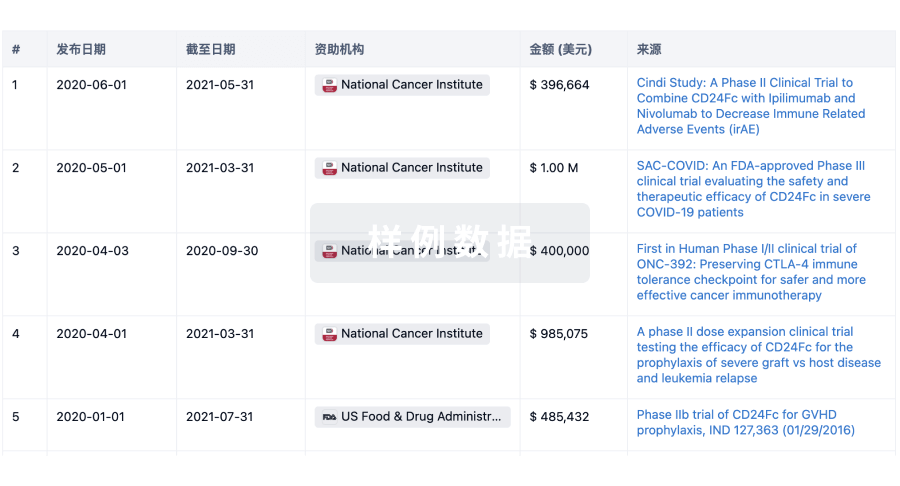
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
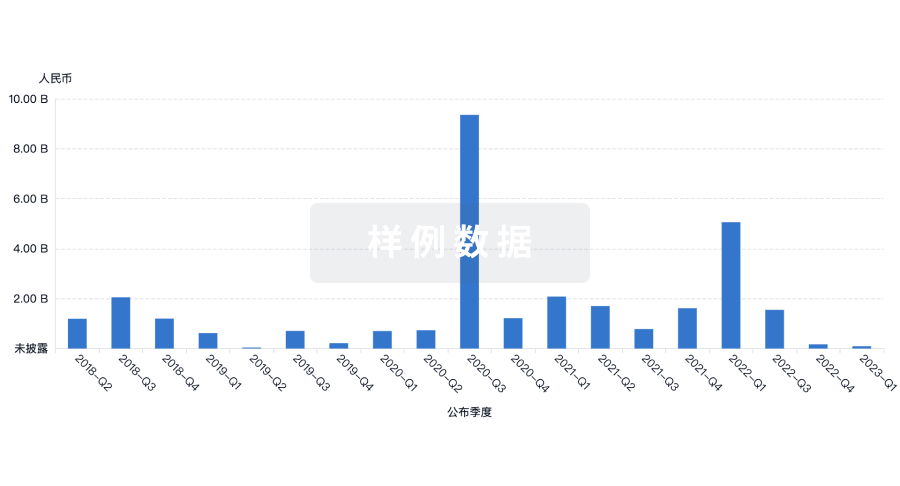
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
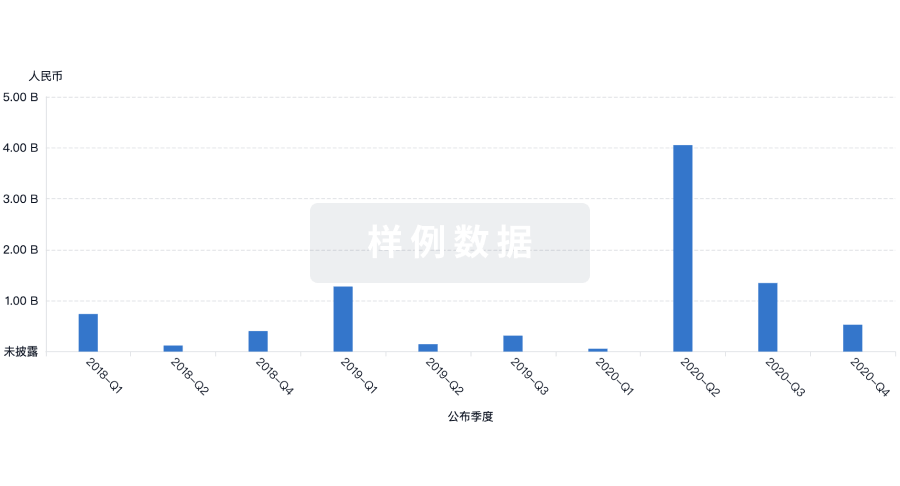
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
Eureka LS:
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用