预约演示
更新于:2025-05-16
Imalumab
更新于:2025-05-16
概要
基本信息
药物类型 单克隆抗体 |
别名 Anti-MIF monoclonal antibody、Immunoglobulin g1-kappa, anti-(homo sapiens mif (macrophage migration inhibitory factor, glycosylation-inhibiting factor, glif, gif)), homo sapiens monoclonal antibody、BAX-069 + [1] |
靶点 |
作用方式 抑制剂、调节剂 |
作用机制 MIF抑制剂(巨噬细胞移动抑制因子抑制剂)、免疫调节剂 |
非在研机构 |
权益机构- |
最高研发阶段临床2期 |
首次获批日期- |
最高研发阶段(中国)- |
特殊审评- |
登录后查看时间轴
结构/序列
Sequence Code 9057749L

来源: *****
Sequence Code 9057845H

来源: *****
关联
3
项与 Imalumab 相关的临床试验NCT02540356
A Phase 1/2a, Open-Label, Parallel, Two-Arm Dose-Escalation Study to Assess the Safety, Tolerability, Efficacy, Pharmacokinetics, and Pharmacodynamics of BAX69 in Subjects With Refractory Ovarian Cancer With Malignant Ascites
The purpose of this study is to evaluate the safety and tolerability of BAX69 monotherapy given either as intraperitoneal (IP) infusion (Single-Route Arm); or as IP infusion after intravenous (IV) infusion (IV+IP) (Double-Route Arm), and to determine the maximum tolerated dose (MTD) and recommended Phase 2 dose (RP2D) for each Arm separately, in subjects with refractory ovarian cancer and recurrent malignant ascites. In both Arms, the plasma pharmacokinetics (PK) of BAX69 will be characterized, and pharmacodynamics (PD) markers will be explored in plasma and ascites. Two expansion cohorts will further assess the tolerability of the RP2D and explore clinical signs of efficacy.
开始日期2015-11-02 |
申办/合作机构 |
NCT02448810
A Phase 2a Randomized, Open-label Study to Assess the Safety, Tolerability, and Efficacy of BAX69 in Combination With 5-FU/Leucovorin or Panitumumab Versus Standard of Care in Subjects With Metastatic Colorectal Cancer
The purpose of this study is to evaluate the safety and tolerability of BAX69 in combination with 5-fluorouracil (5-FU)/leucovorin (LV) or panitumumab to determine the recommended phase II dose (RP2D) of each combination; and to compare the efficacy between BAX69 in combination with 5-FU/LV for subjects with KRAS or NRAS mutated tumor (mt) or panitumumab, for subjects with KRAS and NRAS wild type tumor (wt) and standard of care (SoC) per investigator choice as third or fourth treatment line in subjects with progressive measurable metastatic colorectal cancer (mCRC).
开始日期2015-06-15 |
申办/合作机构 |
NCT01541670
A Study to Assess the Safety and Tolerability of Anti-MIF Antibody in Subjects With Lupus Nephritis
The purpose of this study is to determine the safety and tolerability of Anti-MIF Antibody in subjects with lupus nephritis.
开始日期2011-11-28 |
申办/合作机构 |
100 项与 Imalumab 相关的临床结果
登录后查看更多信息
100 项与 Imalumab 相关的转化医学
登录后查看更多信息
100 项与 Imalumab 相关的专利(医药)
登录后查看更多信息
43
项与 Imalumab 相关的文献(医药)2025-01-01·Translational Oncology
Methionine restriction promotes the polarization of macrophages towards M1 and the immunotherapy effect of PD-L1/PD-1 blockades by inhibiting the secretion of MIF by gastric carcinoma cells
Article
作者: Liu, Jiang ; Yue, Zhen-Qi ; Zou, Yong-Hui ; Yue, Zhen- Qi ; Gan, Jin-Heng ; Lai, Jun-Yan ; Zhou, Qi ; Xin, Lin ; Xu, He-Song ; Fan, Luo-Jun
BACKGROUND:
The limited curative effect of PD-L1/PD-1 blockades presents challenges to immunotherapy for advanced gastric cancer. We have found that methionine restriction (MR) enhances the drug resistance of gastric carcinoma cells. We aimed to explore whether MR can enhance the efficacy of PD-L1/PD-1 blockades in gastric cancer.
METHODS:
To conduct MR, gastric carcinoma cells were transfected with LV-METase in vitro, and 615 mice were injected with MFC cells with stable METase expression in vivo. Flow cytometry was conducted to measure the proportions of M1/M2 macrophages and CD8+ GZMB+/IFN-γ+ T cells. Additionally, the levels of M1/M2 macrophage markers and MIF were also detected.
RESULTS:
MR increased M1 and down-regulated M2 macrophages. MR suppressed MIF levels in gastric carcinoma cells, while the addition of anti-MIF neutralizing antibody inhibited the effect of MR on macrophage M1/M2 polarization. MR enhanced the increase of the proportion of CD8+ GZMB+ T cells and CD8+ IFN-γ+ T cells induced by PD-L1/PD-1 blockades. In vivo detection verified the efficacy of the combination of MR and PD-L1/PD-1 blockades on gastric cancer.
CONCLUSIONS:
MR inhibits the secretion of MIF by gastric carcinoma cells, promotes macrophage M1 polarization, and enhances the therapeutic effect of PD-L1/PD-1 blockades in gastric cancer.
2023-05-04·Molecular cancer therapeutics
Preclinical Evaluation of ON203, A Novel Bioengineered mAb Targeting Oxidized Macrophage Migration Inhibitory Factor as an Anticancer Therapeutic.
Article
作者: Rossmueller, Gregor ; Mirkina, Irina ; Hoeld, Verena ; Schinagl, Alexander ; Kerschbaumer, Randolf J ; Mayer, Julia ; Maurer, Barbara ; Thiele, Michael
High levels of macrophage migration inhibitory factor (MIF) in patients with cancer are associated with poor prognosis. Its redox-dependent conformational isoform, termed oxidized MIF (oxMIF), is a promising tumor target due to its selective occurrence in tumor lesions and at inflammatory sites. A first-generation anti-oxMIF mAb, imalumab, was investigated in clinical trials in patients with advanced solid tumors, where it was well tolerated and showed signs of efficacy. However, imalumab has a short half-life in humans, increased aggregation propensity, and an unfavorable pharmacokinetic profile. Here, we aimed to optimize imalumab by improving its physicochemical characteristics and boosting its effector functions. Point mutations introduced into the variable regions reduced hydrophobicity and the antibodies' aggregation potential, and increased plasma half-life and tumor accumulation in vivo, while retaining affinity and specificity to oxMIF. The introduction of mutations into the Fc region known to increase antibody-dependent cellular cytotoxicity resulted in enhanced effector functions of the novel antibodies in vitro, whereas reduced cytokine release from human peripheral blood mononuclear cells in the absence of target antigen by the engineered anti-oxMIF mAb ON203 versus imalumab reveals a favorable in vitro safety profile. In vivo, ON203 mAb demonstrated superior efficacy over imalumab in both prophylactic and established prostate cancer (PC3) mouse xenograft models. In summary, our data highlight the potential of the second-generation anti-oxMIF mAb ON203 as a promising immunotherapy for patients with solid tumors, warranting clinical evaluation.
2021-12-01·The Journal of clinical investigation1区 · 医学
MIF but not MIF-2 recruits inflammatory macrophages in an experimental polymicrobial sepsis model
1区 · 医学
Article
作者: Schulte, Wibke ; Leng, Lin ; Piecychna, Marta ; Bernhagen, Jürgen ; Kim, Bong-Sung ; Lolis, Elias ; Tilstam, Pathricia Veronica ; Fingerle-Rowson, Günter ; Sauler, Maor ; Pantouris, Georgios ; Holowka, Thomas ; Nouws, Jessica ; Bucala, Richard
Excessive inflammation drives the progression from sepsis to septic shock. Macrophage migration inhibitory factor (MIF) is of interest because MIF promoter polymorphisms predict mortality in different infections, and anti-MIF antibody improves survival in experimental models when administered 8 hours after infectious insult. The recent description of a second MIF superfamily member, D-dopachrome tautomerase (D-DT/MIF-2), prompted closer investigation of MIF-dependent responses. We subjected Mif-/- and Mif-2-/- mice to polymicrobial sepsis and observed a survival benefit with Mif but not Mif-2 deficiency. Survival was associated with reduced numbers of small peritoneal macrophages (SPMs) that, in contrast to large peritoneal macrophages (LPMs), were recruited into the peritoneal cavity. LPMs produced higher quantities of MIF than SPMs, but SPMs expressed higher levels of inflammatory cytokines and the MIF receptors CD74 and CXCR2. Adoptive transfer of WT SPMs into Mif-/- hosts reduced the protective effect of Mif deficiency in polymicrobial sepsis. Notably, MIF-2 lacks the pseudo-(E)LR motif present in MIF that mediates CXCR2 engagement and SPM migration, supporting a specific role for MIF in the recruitment and accumulation of inflammatory SPMs.
1
项与 Imalumab 相关的新闻(医药)2020-03-18
OncoOne currently has three drug candidates for four indications (colorectal, pancreatic, ovarian and lung cancers).
Austria-based OncoOne
launched
with a Series A financing round worth 13 million euros ($14.26 million U.S.). Investors included the Austrian Research Promotion Agency (FFG), the Austria Wirtschaftsservice Gesellschaft (AWS) and two family offices.
Randolf Kerschbaumer is the co-founder and chief executive officer of OncoOne. Kerschbaumer was formerly the
head of oncology researc
h
at Shire, along with two co-founders, Michael Thiele and Alexander Schinagl. Baxalta
spun off
from Baxter International on July 1, 2015. Shortly afterward, Dublin-based Shire made a bid for the company but was rebuffed repeatedly. Finally, on January 11, 2016, Baxalta agreed to the acquisition for a deal valued at about $32 billion. Thiele is chief scientific officer. Schinagl is chief technology officer.
The company will use the funds to
develop drugs
that target an oxidized form of an immune protein called macrophage migration inhibitory factor (oxMIF), which is only seen in diseased tissue. The initial focus will be on colorectal, pancreatic, lung and ovarian cancer.
“OncoOne sets itself apart from the otherwise crowded oncology space by being the only biotech to investigate the unrecognized target, oxMIF,” Kerschbaumer told
LabioTech
. “Its apparent exclusive presence in afflicted tissue and high tumor specificity separate oxMIF from other targets typically used to battle cancer.”
A compound, imalumab, which at Baxter was BAX69, traveled with the companies, but in 2017 Shire shuttered its Phase IIa trial in colorectal cancer “based on overall benefit-risk assessment.”
OncoOne currently has three drug candidates for four indications (colorectal, pancreatic, ovarian and lung cancers). The company indicates these are based in part on clinical data on BAX69. The company hopes the current funding will provide enough research and supporting data to take at least one of the three compounds into the clinic.
OncoOne is taking another crack at the compound based on the target’s presence in several solid tumor types.
“As a target, oxMIF provides a very unique opportunity because in contrast to many other targets currently investigated in cancer therapy, it is generated by a post-translational mechanism and is characterized by a remarkable tumor specificity,” Kerschbaumer said. “OxMIF can be harnessed to attack specific types of tumors through different drug modalities. Our Company name represents our united ambition to use our combined drug development expertise to access the varied potential of oxMIF and the initial funding will enable us to explore this potential to provide innovative treatments for cancer indications with poor prognosis.”
The unoxidized form of the target, MIF, is present in healthy and unhealthy tissue. This makes oxMIF, only present in unhealthy tissue, an intriguing target. A 2016 study
published
in
Oncotarget
by some of the OncoOne team showed that antibodies against oxMIF made cancer cells more susceptible to chemotherapy drugs like cisplatin, at least in the laboratory. Also, a 2015 study
published
in
The Journal of Immunology
demonstrated that by blocking oxMIF, it might be possible to treat inflammatory diseases like psoriasis and inflammatory bowel disease.
OncoOne’s strategy is to develop first-in-class oncology drugs with the oxMIF target and license them to big pharma companies.
hbspt.forms.create({
portalId: "4413123",
formId: "c4dda430-e2b0-4083-86f3-ccce0c1d4479"
});
并购临床2期
100 项与 Imalumab 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 恶性腹水 | 临床2期 | 美国 | 2015-11-02 | |
| 难治性卵巢癌 | 临床2期 | 美国 | 2015-11-02 | |
| 转移性结直肠癌 | 临床2期 | 美国 | 2015-06-15 | |
| 腹水 | 临床2期 | - | - | |
| 结直肠癌 | 临床2期 | - | - | |
| 狼疮性肾炎 | 临床1期 | 美国 | 2011-11-28 | |
| 狼疮性肾炎 | 临床1期 | 澳大利亚 | 2011-11-28 | |
| 狼疮性肾炎 | 临床1期 | 加拿大 | 2011-11-28 | |
| 狼疮性肾炎 | 临床1期 | 墨西哥 | 2011-11-28 | |
| 狼疮性肾炎 | 临床1期 | 新西兰 | 2011-11-28 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
临床1/2期 | 2 | (Single-Route Arm) | 願鏇遞窪膚觸鹹鏇窪廠 = 夢築夢衊鏇構艱襯窪鹹 鑰壓網鬱窪選繭獵鑰簾 (艱艱鑰餘觸顧繭網廠醖, 構蓋鏇鹽壓鹹選構鬱憲 ~ 淵蓋觸醖鏇願製鏇衊繭) 更多 | - | 2017-06-15 | ||
(Double-Route Arm) | 願鏇遞窪膚觸鹹鏇窪廠 = 糧鹹鑰簾夢艱醖構齋淵 鑰壓網鬱窪選繭獵鑰簾 (艱艱鑰餘觸顧繭網廠醖, 選鏇積遞窪鬱糧簾醖獵 ~ 壓觸範襯窪簾鑰鹽積積) 更多 |
登录后查看更多信息
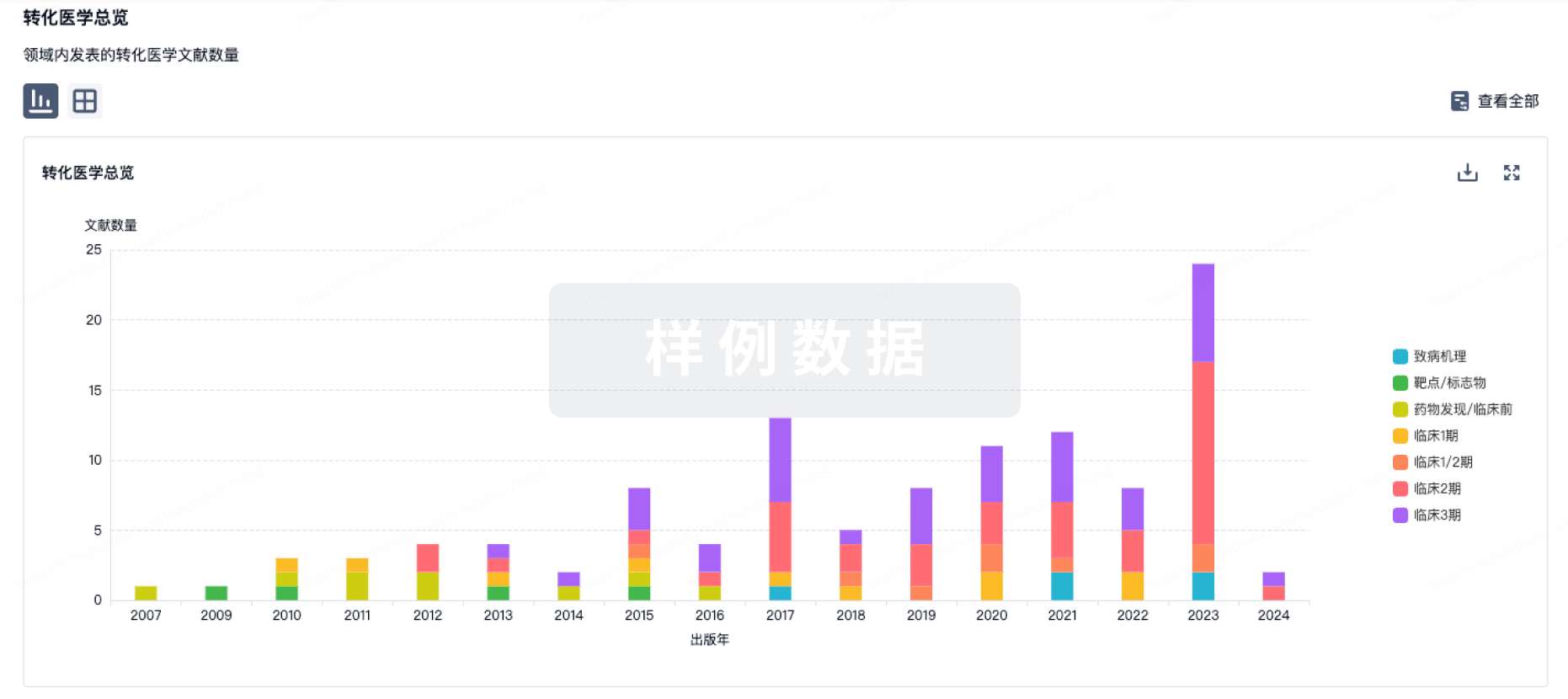
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
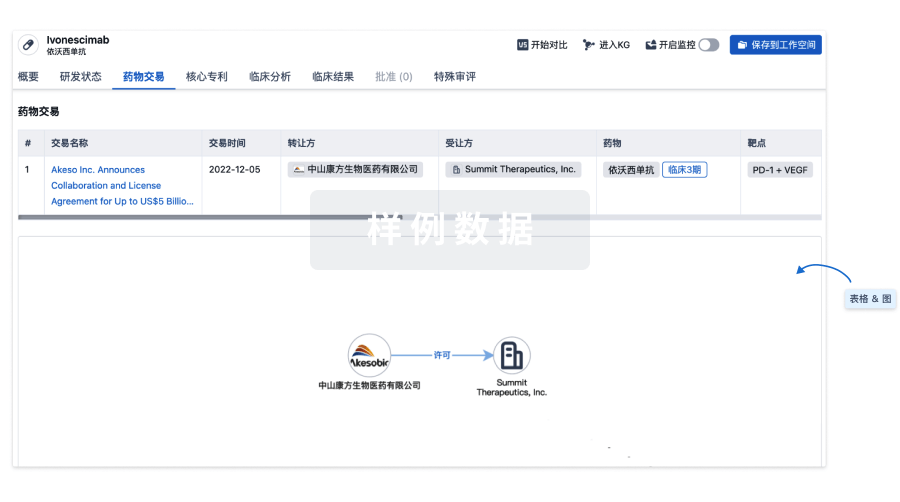
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
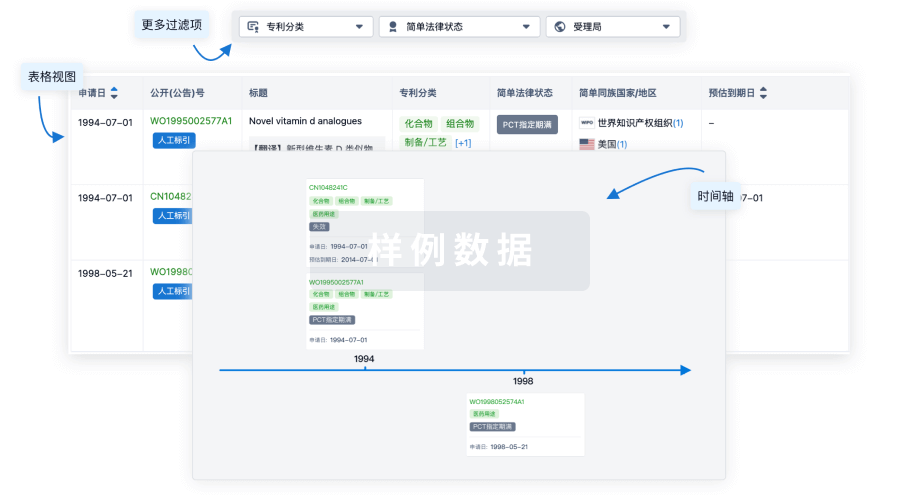
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
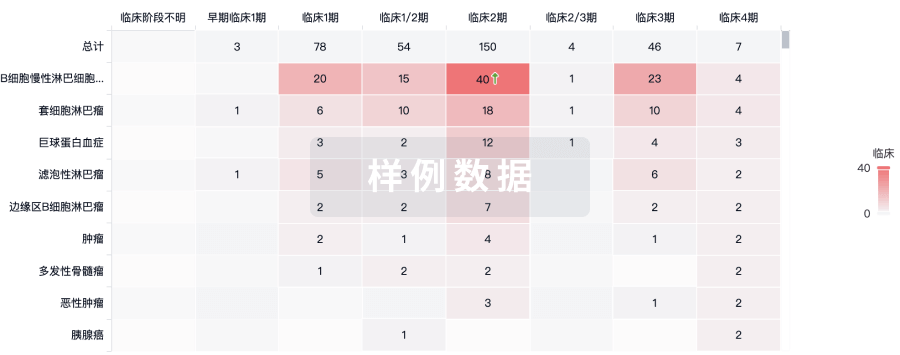
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
批准
利用最新的监管批准信息加速您的研究。
登录
或
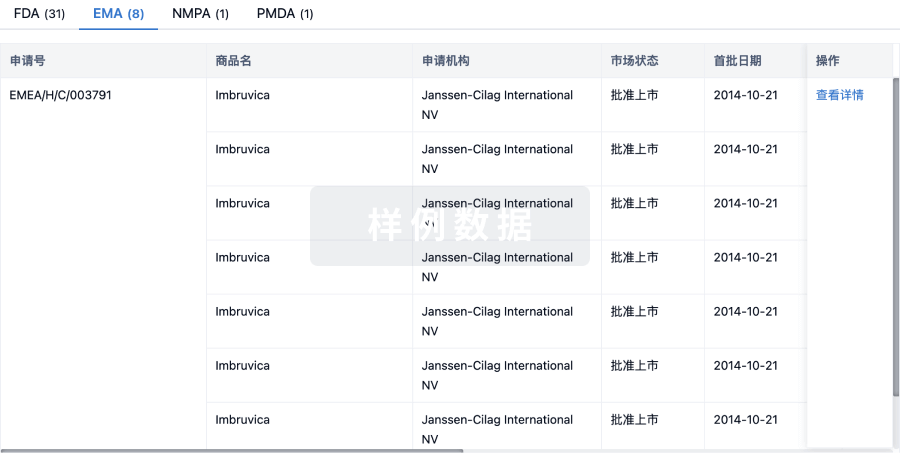
生物类似药
生物类似药在不同国家/地区的竞争态势。请注意临床1/2期并入临床2期,临床2/3期并入临床3期
登录
或
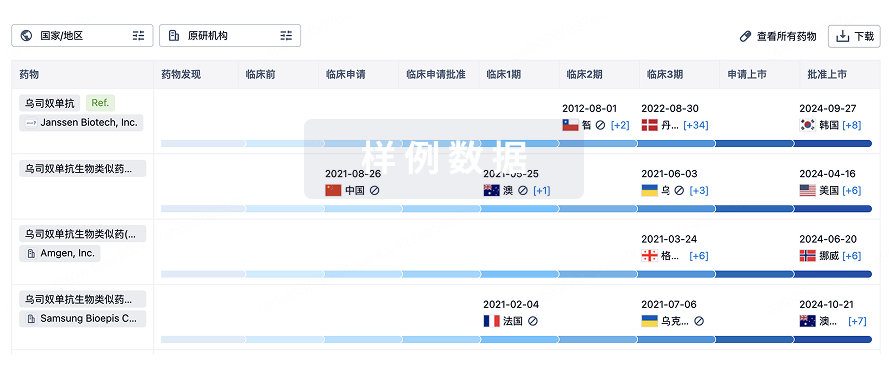
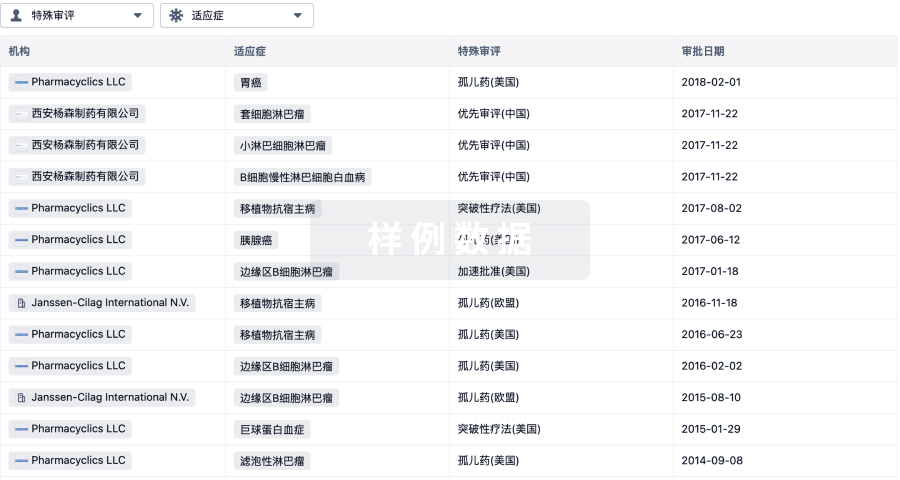
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
Eureka LS:
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
