预约演示
更新于:2025-09-08
Fenebrutinib
更新于:2025-09-08
概要
基本信息
原研机构 |
权益机构- |
最高研发阶段临床3期 |
首次获批日期- |
最高研发阶段(中国)临床3期 |
特殊审评- |
登录后查看时间轴
结构/序列
分子式C37H44N8O4 |
InChIKeyWNEODWDFDXWOLU-QHCPKHFHSA-N |
CAS号1434048-34-6 |
关联
24
项与 Fenebrutinib 相关的临床试验ISRCTN41455091
A phase I, open-label, single-dose study to evaluate the effect of severe renal impairment on the pharmacokinetics of fenebrutinib
开始日期2024-06-06 |
申办/合作机构 |
ISRCTN46432183
A phase I, open-Label, single-Dose study to evaluate the effect of mild or moderate hepatic impairment on the pharmacokinetics of fenebrutinib
开始日期2023-10-18 |
申办/合作机构 |
PACTR202212815145545
A Phase III Multicenter Randomized, Double-Blind, Double-Dummy, Parallel-Group Study To Evaluate The Efficacy And Safety Of Fenebrutinib Compared With Teriflunomide In Adult Patients With Relapsing Multiple Sclerosis
开始日期2023-02-28 |
申办/合作机构 |
100 项与 Fenebrutinib 相关的临床结果
登录后查看更多信息
100 项与 Fenebrutinib 相关的转化医学
登录后查看更多信息
100 项与 Fenebrutinib 相关的专利(医药)
登录后查看更多信息
77
项与 Fenebrutinib 相关的文献(医药)2025-09-01·EUROPEAN JOURNAL OF PHARMACOLOGY
Next generation Bruton's tyrosine kinase inhibitors – characterization of in vitro potency and selectivity
Article
作者: Angst, Daniela ; Cenni, Bruno ; Pulz, Robert
Bruton's tyrosine kinase (BTK) mediates B cell receptor and Fc receptor signaling and is a key regulator of autoimmunity and allergy. A series of novel BTK inhibitors (BTKi) are currently in development for non-oncologic indications with covalent-irreversible (remibrutinib, evobrutinib, tolebrutinib, orelabrutinib), covalent-reversible (rilzabrutinib), and non-covalent reversible (fenebrutinib) binding modes. This study characterizes their in vitro potency and selectivity profiles under the same conditions to minimize assay differences across the different binding modes. Covalent BTKi showed human in vitro blood BTK binding in a time- and concentration-dependent manner with remibrutinib being the most potent and fastest in onset of action. Cellular BTK pathway inhibition was determined in human blood B cells and basophils, and for covalent BTKi correlated well with BTK binding. In contrast to the covalent-irreversible remibrutinib, the non-covalent reversible fenebrutinib showed rapid loss of cellular BTK inhibition after washout. Kinase selectivity was assessed in a binding screen across the human kinome, followed by quantification of binding affinities for a selection of kinases. BTKi ranked in their selectivity as follows (most selective to least): remibrutinib, fenebrutinib, evobrutinib, orelabrutinib, rilzabrutinib and tolebrutinib. These data suggest that next generation BTKi show important differences in their in vitro target binding and selectivity when compared under the same conditions.
2025-08-01·LANCET NEUROLOGY
Safety and efficacy of fenebrutinib in relapsing multiple sclerosis (FENopta): a multicentre, double-blind, randomised, placebo-controlled, phase 2 trial and open-label extension study.
Article
作者: Habek, Mario ; Kuruvilla, Denison ; Qi, Qi ; Hua, Le H ; Budincevic, Hrvoje ; Xu, Yan ; Goodyear, Alexandra ; Dufek, Michal ; Drulovic, Jelena ; Mitzner, Maresa Caunt ; Bar-Or, Amit ; Ratchford, John N ; Weber, Martin S ; Napieralski, Julie ; Thomas, Piia ; Clayton, David ; Chen, Ying-Fang ; Harp, Christopher T ; Oh, Jiwon
BACKGROUND:
The prospect for Bruton's tyrosine kinase (BTK) inhibition to meaningfully affect relapsing multiple sclerosis has recently been questioned due to inconsistent findings in the magnitude and sustainability of the effect of BTK inhibitors on disease activity. We assessed the safety, efficacy, and CSF drug concentrations of fenebrutinib, a highly selective, noncovalent, reversible BTK inhibitor, in patients with relapsing multiple sclerosis.
METHODS:
This multicentre, double-blind, randomised, placebo-controlled, phase 2 trial (FENopta) was conducted at 18 community centres and hospitals across six countries in Europe and North America. Patients with relapsing multiple sclerosis aged 18-55 years with an Expanded Disability Status Scale (EDSS) score of 0·0-5·5, and recent documented disease activity, were randomly assigned (2:1) to oral fenebrutinib (200 mg twice daily) or placebo for 12 weeks, using permuted blocks and stratified by the presence or absence of T1 gadolinium-enhancing (Gd+) lesions on the brain MRI at screening. The randomisation sequence was generated by an interactive voice or web response system and both patients and investigators were masked to treatment allocation. Participants could enter an optional open-label extension study to receive fenebrutinib for up to 192 weeks. The primary efficacy endpoint was the total number of new T1 Gd+ lesions on brain MRI at weeks 4, 8, and 12; with additional MRI assessments at 48-week intervals during the open-label extension. Efficacy analyses were done on randomised patients with evaluable post-baseline MRIs; safety analyses used the safety-evaluable population. This study is registered with ClinicalTrials.gov, NCT05119569, and EudraCT, 2021-003772-14; recruitment is closed and the trial is ongoing.
FINDINGS:
Between March 1, 2022 and March 29, 2023, 109 patients with relapsing multiple sclerosis were randomly assigned treatment: 73 received fenebrutinib and 36 received placebo. 106 patients had evaluable post-baseline brain MRI scans and were assessed for efficacy in the fenebrutinib group (n=70) and placebo group (n=36). The combined number of new T1 Gd+ lesions at weeks 4, 8, and 12 were 0·077 (95% CI 0·043-0·135) in the fenebrutinib group and 0·245 (0·144-0·418) in the placebo group (69% relative reduction [95% CI 34-85]; p=0·0022). During the open-label extension, through week 48, the unadjusted annualised relapse rate was 0·04 and 95 (96%) of 99 patients were relapse-free. During the double-blind treatment phase, the most common adverse events that were more frequent in the fenebrutinib group than in the placebo group were hepatic enzyme elevations (four [6%] vs 0), headache (three [4%] vs one [3%]), and nasopharyngitis (two [3%] vs 0); no serious adverse events or deaths occurred.
INTERPRETATION:
Fenebrutinib was well tolerated and exerted an early, robust, and sustained effect of limiting new focal brain lesions. Further studies are needed to better characterise the safety and efficacy of fenebrutinib on both relapsing multiple sclerosis and non-relapsing progressive multiple sclerosis.
FUNDING:
F. Hoffmann-La Roche.
2025-08-01·JOURNAL OF THE AMERICAN ACADEMY OF DERMATOLOGY
Comparative effects of biologics and small molecule inhibitors on cutaneous disease activity in lupus erythematosus: A systematic review and network meta-analysis
Article
作者: Gou, David ; Sun, Wayne ; Rayner, Daniel G ; Xi, Cheng En ; Silang, Isabella ; Khosravi-Hafshejani, Touraj ; Dutz, Jan P
Meta-anal. of comparative effects of biologics and small mol. inhibitors on cutaneous disease activity in lupus erythematosus.Our review builds upon the limitations of previous network meta-analyses by including 29 more trials investigating 25 addnl. unique interventions in our analyses on CLASI-A scores.In addition to anifrolumab, deucravacitinib, and litifilimab, we identified superior efficacy of sifalimumab and daxdilimab compared to placebo-all of which target the type 1 interferon pathway. Litifilimab and daxdilimab inhibit BDCA2 and Ig-like transcript 7, resp., which reside on dendritic cells and stimulate the production of type 1 interferons.Meanwhile, sifalimumab directly inhibits interferon-, and anifrolumab and deucravacitinib target the interferon-receptor and tyrosine kinase 2, resp.-two proteins involved in the interferon signaling pathway.These findings support the continued investigation of the type 1 interferon pathway in the management of CLE.
119
项与 Fenebrutinib 相关的新闻(医药)2025-08-31
血液瘤领域的明星靶点 BTK,正在加速奔跑进入它的下一个新战场。
8 月 29 日,赛诺菲 36.8 亿美元收购 Principia 公司所得的重磅产品 Rilzabrutinib 在美国迎来全球首批,成为全球首个获批治疗免疫性血小板减少症的 BTK 抑制剂,同时也是首个专门针对自身免疫性疾病而开发的 BTK 抑制剂,代表着 BTK 在自免领域的重大突破!
与此同时,赛诺菲的第 2 款自免 BTK 抑制剂 Tolebrutinib、诺华的自免 BTK 抑制剂瑞米布替尼,也有望在下半年迎来获批。这意味着,BTK 在自免战场的竞赛,擂鼓已经敲响。
BTK 自免研发驶入快车道
全球在研管线超 50 款
BTK 是一种非受体酪氨酸激酶,在多种造血细胞类型中表达,包括 B 细胞、肥大细胞、中性粒细胞、髓系细胞和破骨细胞。在 B 细胞中,BTK 可通过 B 细胞抗原受体 (BCR) 和 Toll 样受体 (TLR) 信号转导促进 B 细胞的发育和激活。
在免疫反应中,BTK 信号通路发挥着重要作用,是 B 细胞受体和 Fc 受体信号转导的关键介质。BTK 可显著激活 BCR 信号通路,导致 B 细胞分化为自身反应性 B 细胞。此外,BTK 还能激活先天免疫细胞,包括巨噬细胞、肥大细胞、嗜碱性粒细胞和中性粒细胞。
在自身免疫疾病中,B 细胞的异常活化会产生有害的自身抗体和炎症。因此,通过阻断 BCR 信号通路,可以抑制 B 细胞的异常活化、增殖和自身抗体产生,从而达到治疗自免疾病的效果。
然而,由于一代 BTK 抑制剂在治疗自免疾病时缺乏选择性、有毒性等原因,BTK 在自免领域的临床开发进展严重落后于其肿瘤领域。从首款 BTK 抑制剂获批至今的 12 年时间里,全球范围内先后有 6 款 BTK 抑制剂获批,但适应症主要是肿瘤。
随着新一代 BTK 抑制剂在靶点选择性、安全性方面的提升,BTK 在自免领域的研究进展也开始驶入了快车道。
根据 Insight 数据库,目前全球共有 55 款 BTK 抑制剂(仅统计活跃状态)正在开展针对自身免疫性疾病的研究,药物类型包括传统小分子抑制剂和 PROTAC。其中,有 34 款处于获批临床及以上阶段。
从适应症分布来看,竞争最激烈的 TOP4 适应症为多发性硬化、类风湿关节炎、慢性自发性荨麻疹、系统性红斑狼疮,对应的 BTK 管线数量均超过了 10 个。
截图来源:Insight 数据库
赛诺菲、诺华等制药巨头
抢滩布局
BTK 在免领域的巨大潜力,吸引了众多跨国药企布局。Insight 数据库显示,在研的 55 个管线中,30 个是进口药,研发机构不乏艾伯维、赛诺菲、诺华、礼来、阿斯利康、罗氏、吉利德等制药巨头。
伊布替尼(强生/艾伯维)是全球首个 BTK 抑制剂,属于不可逆抑制剂。作为第一代 BTK 抑制剂,伊布替尼虽然在肿瘤治疗中取得了显著疗效,但其存在的脱靶效应,可能使患者出现感染风险增加、出血、心脏问题、免疫功能低下等副作用,治疗大部分自免疾病的风险收益比并不高。因此,除了移植物抗宿主病 (cGVHD) 外,该药并没有拓展至其它更广泛的自免适应症。
不过,艾伯维并没有放弃自免领域的布局,其还开发了一款新型 BTK 抑制剂 Elsubrutinib(ABBV105),该药正在开展治疗红斑狼疮的 Ⅱ 期临床。同时,艾伯维还将 Elsubrutinib 和 JAK 抑制剂乌帕替尼组成了一款新型固定剂量复方制剂——ABBV-599,正在 Ⅱ 期临床中探索其治疗系统性红斑狼疮的效果。
在 BTK 赛道,赛诺菲算是后入局者,但专攻自免的差异化策略已使其成为 BTK 自免领域的领跑玩家。
2020 年 9 月,赛诺菲以 36.8 亿美元收购 Principia Biopharma 公司,此举旨在囊获后者的两款 BTK 抑制剂 Rilzabrutinib 和 Tolebrutinib,拓展自免管线。
Rilzabrutinib 是一款口服、可逆、共价 BTK 抑制剂,主要开发用于治疗自免疾病。该药在 24 年 11 月向 FDA 申报上市,今年 8 月 29 日获批,是首个获批的用于治疗免疫性血小板减少症(ITP)的 BTK 抑制剂。去年 12 月,该药也已在国内递交 ITP 适应症的 NDA,目前正在审评中。
目前,赛诺菲还在临床中探索 Rilzabrutinib 治疗自身免疫性溶血性贫血、特应性皮炎、慢性自发性荨麻疹、局灶节段性肾小球硬化症、格雷夫斯病等适应症的效果。
另一款产品 Tolebrutinib 是一款具有脑穿透性和生物活性的 BTK 抑制剂,该药的核心优势在于能精准靶向多发性硬化症(MS)中驱动残疾进展的关键因素——神经炎症。Tolebrutinib 在 25 年 3 月向 FDA 递交了首个 NDA,首发适应症为多发性硬化(MS),PDUFA 日期为 9 月 28 日,有望成为首个斩获 MS 适应症的 BTK 抑制剂。
由此可见,赛诺菲有望成为首家在自免领域拥有两款获批 BTK 抑制剂的公司。赛诺菲预测 Rilzabrutinib 和 Tolebrutinib 各自的年销售额均有望达到 20 亿欧元~50 亿欧元区间,成为推动公司未来业绩增长的潜在重磅炸弹药物 [3]。
抢滩布局的制药巨头的还有诺华。该公司的瑞米布替尼(Remibrutinib)是一款靶向 BTK 的第二代共价抑制剂。2025 年 2 月、3 月,该药先后在中国和美国递交了上市申请,首发适应症为慢性自发性荨麻疹(CSU)患者,并被纳入了优先审评,有望成为首个获批治疗 CSU 的 BTK。
此外,诺华还在开发瑞米布替尼用于治疗荨麻疹、多发性硬化、化脓性汗腺炎、重症肌无力等适应症。诺华预测瑞米布替尼的年销售额峰值有望超过 30 亿美元 [4]。
其它进度比较快的产品还有:吉利德/小野制药的替拉鲁替尼,正在开展治疗天疱疮的 Ⅲ 期临床;罗氏的 Fenebrutinib,正在开展治疗多发性硬化的 Ⅲ 期临床。此外,礼来的匹妥布替尼、阿斯利康的阿可替尼、渤健的 BIIB091 等正在开展针对不同自免适应症的 Ⅱ 期临床(详见下表)。
诺诚健华、百济神州等国内药企
竞相入场
国内企业在 BTK 自免领域也不甘落后。根据 Insight 数据库,目前共计有 25 款国产 BTK 抑制剂在开展针对自免疾病的研究,占到了全球 BTK 自免管线的 45%。其中,有 15 款已进入到获批临床及以上阶段,玩家包括百济神州、诺诚健华、正大天晴、恒瑞医药、人福医药、翰森制药等众多国内明星药企。
从研究进度来看,诺诚健华、百济神州、邦顺制药的产品处于第 1 梯队,均已进入 Ⅲ 期阶段。
诺诚健华从 2019 年就开始启动奥布替尼自免适应症的临床研究。目前,奥布替尼治疗免疫性血小板减少症(ITP)的 Ⅲ 期临床已经完成患者入组,预计 2026 年上半年提交上市申请,有望成为首个提交自免适应症 NDA 的国产 BTK 抑制剂。
同时,诺诚健华还在开展奥布替尼治疗多发性硬化、系统性红斑狼疮、血小板减少性紫癜、视神经脊髓炎、系统性红斑狼疮等适应症的临床研究,其中多发性硬化正在全球启动 III 期注册临床试验,SLE 的 IIb 期已接近完成临床研究。
奥布替尼 24 年收入 10 亿元,今年上半年创收 6.4 亿元,自免适应症将打开奥布替尼的第二增长曲线。
百济神州也在加紧拓展泽布替尼的自免适应症。目前,泽布替尼正在开展针对多项自免疾病的临床研究,适应症涵盖嗜血细胞性淋巴组织细胞增多症、免疫性血小板减少症、冷凝集素病、自身免疫性溶血性贫血、多发性神经病、原发性膜性肾病、狼疮肾炎等等。其中,泽布替尼治疗嗜血细胞性淋巴组织细胞增多症已在国内完成一项单臂 Ⅲ 期试验。
泽布替尼 2024 年全球销售额达到 26.44 亿美元,今年上半年大卖 17.42 亿美元,首次上榜全球畅销药 TOP50 榜单,自免适应症将进一步拉高泽布替尼的市场天花板。
此外,百济神州还开发了一款靶向 BTK 的 PROTAC Catadegbrutinib,该药是全球进度最快的 BTK PROTAC,在血液癌症领域已进入 Ⅲ 期临床,在自免领域正在开展针对慢性自发性荨麻疹的Ⅰ期临床。
第三款进入Ⅲ 期的国产 BTK 抑制剂为邦顺制药的邦赛替尼,该药尚未获批任何适应症,进度最快的是免疫性血小板减少症,今年 8 月在国内进入Ⅲ 期临床。同时,邦顺制药还在开展邦赛替尼治疗慢性荨麻疹的 I/II 期。
此外,在自免赛道进展相对较快的产品还有:正大天晴的 TQB3702,正在开展针对系统性红斑狼疮的 Ⅱ 期临床;人福医药的 WXFL10230486,正在开展针对慢性自发性荨麻疹的 Ⅱ 期临床;恒瑞医药的 Edralbrutinib,针对视神经脊髓炎、原发性膜性肾病已进入 Ⅱ 期阶段。
小结
BTK 靶点发现至今已有 30 多年。2024 年,全球 BTK 抑制剂市场规模约为 125 亿美元,主要贡献力量是肿瘤适应症。
在自免赛道,BTK 尚处于蓝海市场。随着在自免领域的陆续进展和突破,BTK 将在疾病治疗领域继续书写自己的辉煌篇章。据弗若斯特沙利文预计,到 2030 年,全球 BTK 抑制剂的市场规模将有望达到 261 亿美元[5]。
参考资料:
[1]Targeting Bruton’s tyrosine kinase (BTK) as a signaling pathway in immune-mediated diseases: from molecular mechanisms to leading treatments
[2]Bruton’s Tyrosine Kinase (BTK) Inhibitors and Autoimmune Diseases: Making Sense of BTK Inhibitor Specificity Profiles and Recent Clinical Trial Successes and Failures.https://pmc-ncbi-nlm-nih-gov.libproxy1.nus.edu.sg/articles/PMC8595937/#s5
[3]https://www.sanofi.com/en/media-room/press-releases/2023/2023-12-07-02-30-00-2792186
[4]Novartis, after slimming down, boosts growth projection through the end of the decade.https://www.fiercepharma.com/pharma/standing-alone-novartis-bumps-its-growth-projection-through-end-decade#:~:text=That%20list%20includes%20chronic%20spontaneous,pelcarsen%20and%20autoimmune%20contender%20ianalumab.
[5]Tens of billions $ market size, how big is the future potential of BTK inhibitors?.https://www.echemi.com/cms/1058731.html
[5] 各公司官方资料。
[6]Insight 数据库
封面来源:站酷海洛 Plus
免责声明:本文仅作信息分享,不代表 Insight 立场和观点,也不作治疗方案推荐和介绍。如有需求,请咨询和联系正规医疗机构。
编辑:馨药
PR 稿对接:微信 insightxb
投稿:微信 insightxb;邮箱 insight@dxy.cn
多样化功能、可溯源数据……
Insight 数据库网页版等你体验
点击阅读原文,立刻解锁!
蛋白降解靶向嵌合体并购引进/卖出
2025-08-31
点击蓝字
关注我们
本
期
看
点
从最初在血液肿瘤领域的突破,到如今跨越至自身免疫疾病的新战场,各大药企围绕BTK抑制剂展开了全球竞赛。BeOne(原百济神州)凭借 Brukinsa(泽布替尼/zanubrutinib)在全球血液肿瘤市场扩大领先;赛诺菲则以 Wayrilz(rilzabrutinib)在 ITP(免疫性血小板减少症) 率先“破圈”,并推动tolebrutinib冲刺 nrSPMS(非复发性继发进展型多发性硬化)。
本文将对BTK抑制剂在全球的竞赛格局进行梳理,解析其在肿瘤和非肿瘤领域的发展现状与趋势。
本期内容
01
肿瘤领域:BTK抑制剂群雄逐鹿
02
自身免疫和中枢神经领域:BTKi新战场
03
自免领域其他BTKi企业
04
总结与展望
【01 肿瘤领域:BTK抑制剂群雄逐鹿】
BTK抑制剂最早因在血液肿瘤(尤其是B细胞恶性肿瘤)中的突出疗效而备受瞩目。
2013年首款BTK抑制剂伊布替尼(ibrutinib,商品名Imbruvica)获批用于套细胞淋巴瘤和慢性淋巴细胞白血病(CLL)等疾病,开创了B细胞肿瘤治疗的新纪元。伊布替尼通过不可逆共价结合BTK,阻断B细胞受体信号通路,显著提高了CLL等疾病的缓解率。然而,随着使用的扩大,伊布替尼的一些局限也逐渐显现,如脱靶效应导致心房颤动、高血压等不良反应,以及C481S突变导致耐药。
在伊布替尼成功的推动下,第二代BTK抑制剂迅速跟进,竞争格局愈发激烈。阿卡替尼(acalabrutinib,商品名Calquence)由阿斯利康推出,以更高选择性降低了部分副作用。
泽布替尼(zanubrutinib,商品名百悦泽®/Brukinsa)由中国的百济神州自主研发,凭借更专一的靶点占有率和优化的安全性在全球脱颖而出。基于ALPINE头对头III期试验数据,泽布替尼成为目前全球首个也是唯一一个在与伊布替尼直接对比中实现无进展生存期(PFS)和总体缓解率(ORR)“双优”优效性的BTK抑制剂。这一成果巩固了泽布替尼在CLL等适应症中的基础地位,也标志着中国创新药在全球肿瘤领域取得了里程碑式的领先优势。
2025年第二季度,百济神州(BeOne)公布布鲁金萨(zanubrutinib)全球销售数据:美国市场销售额达6.84亿美元(同比增长43%),欧洲市场1.50亿美元(增长85%)。
据报道,同期布鲁金萨全球销售约9.50亿美元,领先阿斯利康Calquence(acalabrutinib)的8.72亿美元,拉大了领先优势(差额78百万美元,高于一季度的30百万美元差距)。
BeOne首席财务官Aaron Rosenberg指出,由于布鲁金萨被列为医保优先用药(protected class)且覆盖面广,绝大多数患者能够不受阻碍地获得用药;即便竞争对手采取降价策略,布鲁金萨的净价在2025年下半年也将保持稳定。布鲁金萨凭借其差异化优势正在抢占新患者份额,这为其带来强劲的销量增长。(详情见:从百济神州到BeOne丨泽布替尼如何引领BTK靶点全球竞赛)
肿瘤领域BTK抑制剂的群雄逐鹿,不仅体现在疗效和安全性的比拼,也体现在市场和商业层面。可以预见,随着更多头对头研究数据的公布和新一代产品的上市,肿瘤领域的BTK竞赛将继续围绕疗效最优和耐药破解展开。对于投资者而言,在这一领域胜出的产品将获得可观的市场回报和战略地位。
02 自身免疫和中枢神经领域:BTKi新战场
随着BTK抑制剂在肿瘤领域的成熟,其作用机制也被寄望于解决某些难治的自身免疫疾病和中枢神经系统疾病的病理机制。BTK不仅在B淋巴细胞中发挥关键作用,也参与了巨噬细胞、肥大细胞和小胶质细胞等先天免疫过程。因此,抑制BTK有望在自身免疫性疾病中调节异常免疫反应,包括自身抗体产生、炎症因子释放等,从而影响疾病进程。
赛诺菲正是这一领域的新锐玩家。通过2018年以约36.8亿美元收购,赛诺菲一举获得了多个BTK抑制剂项目,其中包括tolebrutinib和rilzabrutinib。虽然当初收购主要瞄准的是tolebrutinib在多发性硬化症(MS)领域的潜力,但率先跑出“FDA终点线”的却是rilzabrutinib——亦即近日获批上市的Wayrilz,用于治疗原发免疫性血小板减少症(ITP)。Wayrilz作为一种口服、可逆性的BTK抑制剂,可通过多重免疫调节作用,靶向免疫系统中不同通路,从根本上缓解ITP的发病机制。
在关键的LUNA-3 III期试验中,Wayrilz显著提高并持久维持了ITP患者的血小板计数:治疗25周时,Wayrilz组有23%的患者达到持续血小板反应,而安慰剂组为0%。这一成果令Wayrilz成为全球首个ITP适应症的BTK抑制剂,填补了ITP治疗领域的空白。赛诺菲更将其视作“潜在的多适应症重磅药物”,预计巅峰年销售额可达20-50亿欧元。这暗示rilzabrutinib未来可能拓展至其他自身免疫疾病,成为赛诺菲在免疫领域的重要砝码。
与此同时,赛诺菲的另一重磅布局——tolebrutinib正在多发性硬化症领域蓄势待发。与目前主要控制外周免疫的MS疗法不同,tolebrutinib可以穿越血脑屏障,在中枢神经系统内达到治疗性浓度,从而调节中枢内的B淋巴细胞和疾病相关的小胶质细胞。这一独特机制被认为可以作用于进行性MS的潜在病理过程,即中枢神经系统内持续存在的慢性炎症,从而延缓神经退行和残疾积累。
在III期HERCULES试验中,tolebrutinib针对无复发进展型MS(nrSPMS)患者显著延缓了6个月确认残疾进展(CDP)的发生时间,相较安慰剂延迟了31%。这使其成为首个在nrSPMS中显示减少残疾积累的疗法。
赛诺菲已于2025年3月将tolebrutinib用于nrSPMS的NDA递交FDA并获优先审评资格,如果顺利批准,tolebrutinib将成为全球首个也是唯一一个可同时治疗nrSPMS并减缓无关复发的残疾进展的脑渗透性BTK抑制剂。
03 自免领域其他BTKi企业
赛诺菲之外,多家制药巨头亦在自免领域押注BTK靶点:
默克集团(Merck KGaA)的evobrutinib:
作为首批进入MS临床试验的BTK抑制剂,曾在II期显示降低病灶的希望。然而最新报道的两项III期EVOLUTION试验未能证明较现有疗法特立氟胺的年复发率优势,主要终点未达标。尽管耐受性尚可(早期有一过性肝酶升高),疗效上的不足给BTK在MS的前景蒙上一层阴影。不过分析人士指出,BTK抑制剂对MS的益处可能更多体现在延缓残疾进展等方面,而非短期降低复发率。这也呼应了tolebrutinib聚焦“无复发进展”亚群的差异化策略。
罗氏/基因泰克的fenebrutinib:
该药是另一款在研的可逆性BTK抑制剂,正在开展针对MS的III期临床。Fenebrutinib设计上强调高选择性和可逆结合,以期降低副作用。然而在2023年末,美国FDA对其MS项目下达部分临床暂停,原因是试验中出现了几例药物性肝损伤。目前罗氏正加强监测并继续推进研究。值得注意的是,罗氏在2023年发布的II期数据中宣称fenebrutinib显著减少了MS患者脑内的新发病灶。如果安全性问题可控,该药有望成为fenebrutinib阵营中与tolebrutinib分庭抗礼的选手。
诺华的remibrutinib:
这是一款共价不可逆BTK抑制剂,此前在慢性自发性荨麻疹(CSU)中取得了阳性III期结果。研究显示,口服remibrutinib显著改善了患者的瘙痒和风团症状。BTK在肥大细胞的IgE受体信号中起作用,因而抑制BTK可抑制组胺释放,有望成为治疗顽固性荨麻疹的新机制。诺华目前也在推进remibrutinib用于复发型MS的III期试验。一旦成功,remibrutinib有潜力横跨过敏性疾病与中枢神经疾病两大领域,成为“广谱”自免适应症药物。
诺诚健华的orelabrutinib:作为中国本土另一款BTK抑制剂,奥布替尼已在国内获批治疗CLL等血液癌症。其特点是选择性高且据称具有中枢渗透能力。2021年渤健(Biogen)曾以1.25亿美元首付款获得其在除中国外MS和部分自免疾病的开发权益。然而,由于行业竞争和安全顾虑,Biogen于2023年决定终止合作,退出了BTK在MS领域的竞赛。奥布替尼在全球开发受挫的同时,国内也有针对MS的II期结果报道,显示其可使MS病灶数减少90%之多。未来这款药物能否卷土重来、重新寻求国际合作,值得持续关注。
04 竞争格局变化与新药进展
从百济神州的百悦泽®在全球舞台上崭露头角,到赛诺菲Wayrilz开启BTK抑制剂跨领域应用的新纪元,BTK靶点的全球竞赛已经走过了从肿瘤称雄到自免崛起的历程。这一过程中,我们见证了制药创新如何在不同疾病领域迸发出活力。
总体而言,BTKi市场竞争将更加重视差异化策略(如更好的疗效/安全组合、精确适应症定位、固定疗程方案等)以及灵活应对医保与定价政策的能力。企业需在继续推进创新药物研发的同时,通过优化定价和渠道策略(例如直达患者模式)、稳固供应链布局来应对政策不确定性,从而在全球BTK市场竞争中获得领先。
★
临床3期引进/卖出临床结果ASH会议
2025-08-02
行业媒体BioPharma Dive近日发布专题报道,从众多在研项目中精选出10项有望在今年下半年公布结果的潜力临床试验。这些试验聚焦于肥胖症、肺癌和特应性皮炎(AD)等多个关键治疗领域,其中部分结果已陆续披露。这些研究有望为整个生物医药行业带来突破性进展,进一步推动医学创新,惠及更多患者。图片来源:123RF药物名称:Orforglipron(LY3502970)适应症:患有肥胖相关共病的肥胖或超重患者开发公司:礼来(Eli Lilly and Company)临床试验:Attain-1(NCT05869903)Orforglipron是礼来开发的一种每日一次口服、非肽类GLP-1受体小分子激动剂。该药物是一种非肽分子,这使得它更容易被制造和包装成药片。这一特性还可能有助于提高其在患者中的可负担性和可及性。ATTAIN-1是一项3期、随机、双盲临床研究,旨在评估每日一次口服orforglipron在伴有体重相关合并症的成人肥胖或超重患者中的疗效与安全性。该研究将orforglipron与安慰剂进行对比,观察其在减重方面的效果及耐受性。该试验的初步结果预计在今年第三季度公布。药物名称:Amlitelimab适应症:特应性皮炎开发公司:赛诺菲(Sanofi)临床试验:Coast-1(NCT06130566)、SHORE(NCT06224348)赛诺菲研发的amlitelimab是一款靶向OX40配体(OX40L)的单克隆抗体,相较于直接作用于OX40受体的药物,其在抑制T细胞依赖性炎症的同时,避免了对免疫细胞的清除,或可降低免疫抑制相关副作用。在一项2b期临床试验中,amlitelimab在第16周和第24周均显著改善中重度特应性皮炎患者的症状,显示出每12周给药一次的潜力,有望减轻患者的治疗负担。目前,该药正在开展多项3期临床研究,包括Coast-1和SHORE试验,进一步评估其在12岁及以上中重度AD患者中的疗效与安全性。Coast-1为三组平行设计的单药治疗研究,纳入对外用处方药应答不足或不适合继续使用外用疗法的患者;而SHORE则在外用糖皮质激素(TCS)和/或钙调神经磷酸酶抑制剂(TCI)治疗背景下,评估amlitelimab在治疗应答不足患者中的系统性治疗效果。这两项研究将为amlitelimab作为AD新型治疗方案的临床价值提供关键证据。两项试验的初步结果预计在今年第三季度公布。药物名称:Sonelokimab适应症:化脓性汗腺炎(hidradenitis suppurativa)开发公司:Moonlake Immunotherapeutics临床试验:Vela-1(NCT06411899)、Vela-2(NCT06411379)Sonelokimab是一种分子量约为40 kDa的人源化纳米抗体,由三个抗体重链可变区蛋白域共价连接组成。其中两个蛋白域可高亲和力选择性结合IL-17A和IL-17F,有效阻断IL-17A/A、IL-17A/F及IL-17F/F二聚体介导的炎症信号通路;第三个蛋白域则结合人类白蛋白,有助于药物在炎症水肿部位的富集,从而增强局部疗效。为了进一步验证其在治疗中重度化脓性汗腺炎中的临床潜力,sonelokimab目前正在开展两项3期临床研究Vela-1和Vela-2。两项研究均为多中心、随机、双盲、安慰剂对照设计,纳入中重度化脓性汗腺炎成人患者,按2:1比例随机接受每周一次的皮下注射sonelokimab或安慰剂,治疗持续至第16周,旨在系统评估其疗效与安全性,为该类难治性皮肤病提供新的治疗选择。药物名称:Ivonescimab适应症:非小细胞肺癌(NSCLC)开发公司:Summit Therapeutics、康方生物(Akesobio)临床试验:HARMONi(NCT06396065)Ivonescimab是一种靶向PD-1和VEGF的双特异性抗体,能够同时阻断PD-1与其配体PD-L1/PD-L2的结合,以及VEGF与其受体的结合,从而协同抑制肿瘤免疫逃逸和血管生成。鉴于VEGF和PD-1在肿瘤微环境中的共表达,ivonescimab通过单药双靶点机制,有望较联合疗法更有效地增强抗肿瘤活性,并显著降低与VEGF相关的不良反应,展现出更优的安全性。该药目前正在开展HARMONi临床研究,这是一项随机、双盲、多中心的3期临床试验,旨在评估ivonescimab联合培美曲塞和卡铂治疗EGFR突变型局部晚期或转移性非鳞状非小细胞肺癌患者的疗效与安全性。这些患者此前已接受EGFR酪氨酸激酶抑制剂(TKI)治疗并且疾病出现进展。研究计划入组约420名受试者,按1:1比例分组,接受ivonescimab或安慰剂联合化疗,随后进入维持治疗阶段,最多持续至2年。该研究结果预计在今年年底公布。药物名称:Fenebrutinib适应症:复发型多发性硬化(RMS)开发公司:罗氏(Roche)临床试验:FENhance(NCT04586010)、FENhance 2(NCT04586023)Fenebrutinib是一种在研的口服、可逆性、非共价布鲁顿酪氨酸激酶(BTK)抑制剂,能够阻断BTK在B细胞发育及活化中的关键作用,同时调控巨噬细胞和小胶质细胞等髓系免疫细胞的活化。该药具有高选择性,对BTK的抑制选择性高出其他激酶130倍,这一特性有望降低脱靶效应,提升长期使用的安全性。在2期FENopta研究的开放标签扩展阶段中,罗氏公布的48周数据显示,接受fenebrutinib治疗的RMS患者中,多达96%在一年内未出现疾病复发或进展,显示出良好的疗效与耐受性。目前,该药正通过两项关键性3期临床研究FENhance和FENhance 2进一步验证其在RMS中的临床价值。两项研究均为多中心、随机、双盲试验,旨在评估fenebrutinib相比标准治疗药物,在延缓疾病进展和降低复发率方面的疗效与安全性。药物名称:WVE-006适应症:α-1抗胰蛋白酶缺乏症(AATD)开发公司:Wave Life Sciences 临床试验:RestorAATion-2(NCT06405633)WVE-006是一款潜在“first-in-class”的RNA编辑寡核苷酸疗法,基于Wave Life Sciences独有的AIMer平台,能够将腺嘌呤编辑为肌苷(A-to-I),并通过PN化学修饰与GalNAc偶联实现靶向肝脏的皮下注射给药。WVE-006旨在修复AATD患者SERPINA1基因中导致Z突变的单碱基错误,从而恢复功能性野生型AAT蛋白的表达,并减少有害的Z-AAT蛋白聚集,有望用于治疗与AATD相关的肺病和/或肝病。该药目前正通过RestorAATion-2研究进行评估,该研究为一项1b/2a期、开放标签、单剂量递增(SAD)和多剂量递增(MAD)设计的临床试验,纳入Pi*ZZ型AATD患者,旨在系统评估WVE-006的安全性、耐受性、药效学和药代动力学特征。去年10月,Wave Life Sciences宣布该研究取得积极结果,WVE-006在患者体内成功实现了机制验证。根据当时新闻稿,这标志着RNA编辑疗法首次在人类中实现临床机制验证的关键里程碑。公司预计将在今年分享该疗法多次给药数据。药物名称:Evolocumab适应症:高脂血症开发公司:安进(Amgen)临床试验:VESALIUS-CV(NCT03872401)研究表明,低密度脂蛋白胆固醇(LDL-C)水平升高是心血管疾病(CVD)发展的关键可调节风险因素之一。Evolocumab作为一款PCSK9抑制剂,通过阻断PCSK9与LDL受体(LDLR)的结合,增强LDLR在肝细胞表面的表达,从而加速LDL-C的清除,有效降低心肌梗死与中风等重大心血管事件的风险。为进一步验证其在高危人群中的心血管保护效应,evolocumab正在开展VESALIUS-CV研究,这是一项双盲、随机、安慰剂对照的多中心临床3期试验,旨在评估该药在无既往心肌梗死或中风史、但具有较高心血管事件风险的成人患者中,降低重大心血管事件发生率的效果。该试验结果预计在今年第三季度公布。药物名称:VLA15适应症:莱姆病(Lyme disease)开发公司:辉瑞(Pfizer)、Valneva临床试验:VALOR(NCT05477524)VLA15是一款在研的多价蛋白亚单位疫苗,靶向伯氏疏螺旋体的外表面蛋白A(OspA),该蛋白是莱姆病致病菌在蜱虫体内的关键抗原。通过拮抗OspA,VLA15有望阻断病原体从蜱虫向人类传播。此前公布的2期研究显示,VLA15具有良好的免疫原性和安全性,尤其是在第二剂加强免疫后的免疫反应维持稳定。该疫苗目前正在开展一项名为VALOR的3期临床研究。这是一项大型、安慰剂对照试验,旨在系统评估该疫苗的有效性、安全性、耐受性及免疫原性。研究计划招募约9400名来自莱姆病高发地区、年龄在5岁及以上的健康受试者,按约1:1的比例随机分配接受VLA15疫苗或安慰剂。部分受试者还将接种来自不同批次的疫苗,以评估批次间的一致性。接种方案包括三剂基础免疫(分别在第0、2和第5至9个月接种)以及一剂加强针(在基础免疫后约12个月接种),旨在覆盖连续两季甚至三季的莱姆病流行期,从而更全面地评估疫苗在真实世界中的保护效果。该研究的初步结果有望于今年年底公布。药物名称:BHV-7000适应症:抑郁症(MDD)开发公司:Biohaven临床试验:NCT06419608BHV-7000是由Biohaven公司开发的一款新型、选择性激活Kv7.2/Kv7.3钾通道的小分子疗法,该离子通道在神经信号传导和调控神经元过度兴奋状态中发挥关键作用,适用于癫痫和情绪障碍等疾病的治疗。此前公布的1期多剂量递增研究数据显示,该药的每日一次缓释剂型在各剂量水平下均展现出良好的耐受性。目前,BHV-7000正在开展治疗抑郁症的2期临床试验。这是一项多中心、随机、双盲、安慰剂对照研究,旨在评估BHV-7000作为单药治疗在MDD患者中的疗效与安全性。该研究有望为该药物在情绪障碍领域的潜在应用提供关键的临床数据支持。药物名称:mRNA-1010适应症:季节性流感开发公司:Moderna临床试验:P304(NCT06602024)mRNA-1010是Moderna开发的一款基于mRNA技术的季节性流感疫苗,旨在针对流感A型和B型多种毒株提供更广泛和高效的免疫保护。该疫苗目前正处于3期关键性临床研究阶段,重点评估其在50岁及以上成人中的安全性、免疫原性以及相较于已获批标准剂量灭活流感疫苗的相对疫苗效力(rVE)。该项名为P304的研究为一项随机、观察者设盲、阳性对照、病例驱动的3期试验,共招募逾4万名受试者,接受单剂mRNA-1010或对照疫苗,并进行了为期中位6个月的随访。结果显示,mRNA-1010达到了预设的最严格优效性标准,在总体人群中实现了26.6%的rVE(95% CI:16.7%-35.4%),在A/H1N1、A/H3N2及B/Victoria等所有毒株中均展现出稳健保护效力。此外,该疫苗在65岁及以上人群中rVE为27.4%,并在不同年龄、基础疾病和疫苗接种背景的亚组中保持一致优势。mRNA-1010的安全性与耐受性良好,大多数不良事件为轻度,整体与既往研究结果相符。参考资料(可上下滑动查看)[1] 10 clinical trials to watch the rest of 2025. Retrieved July 20, 2025 from https://www.biopharmadive.com/news/biotech-pharma-clinical-trials-watch-2025/736120/?utm_source=Sailthru&utm_medium=email&utm_campaign=Issue:%202025-06-30%20BioPharma%20Dive%20%5Bissue:74500%5D&utm_term=BioPharma%20Dive[2] A Study of Orforglipron (LY3502970) in Adult Participants With Obesity or Overweight With Weight-Related Comorbidities (ATTAIN-1). Retrieved July 20, 2025 from https://clinicaltrials.gov/study/NCT05869903?term=NCT05869903&rank=1[3] A Study to Evaluate the Efficacy and Safety of Subcutaneous Amlitelimab Monotherapy Compared With Placebo in Participants Aged 12 Years and Older With Moderate-to-severe Atopic Dermatitis (COAST 1). Retrieved from https://clinicaltrials.gov/study/NCT06130566?term=coast-1&rank=3[4] A Study to Evaluate the Efficacy and Safety of Subcutaneous Amlitelimab in Participants Aged 12 Years and Older With Moderate-to-severe Atopic Dermatitis on Background Topical Corticosteroids (SHORE). Retrieved July 20, 2025 from https://clinicaltrials.gov/study/NCT06224348?term=amlitelimab&page=2&rank=11[5] A Study to Evaluate the Efficacy and Safety of Subcutaneous Sonelokimab Compared With Placebo in Adult Participants With Moderate to Severe Hidradenitis Suppurativa. Retrieved July 20, 2025 from https://clinicaltrials.gov/study/NCT06411899?term=VELA-1&rank=1[6] Phase III Study of AK112 for NSCLC Patients. Retrieved July 20, 2025 from https://clinicaltrials.gov/study/NCT06396065?term=Harmoni&aggFilters=phase:3&rank=1[7] A Study to Evaluate the Efficacy and Safety of Fenebrutinib Compared With Teriflunomide in Relapsing Multiple Sclerosis (RMS) (FENhance). Retrieved July 20, 2025 from https://clinicaltrials.gov/study/NCT04586010?term=NCT04586010&rank=1[8] Study to Evaluate the Efficacy and Safety of Fenebrutinib Compared With Teriflunomide in Relapsing Multiple Sclerosis (RMS) (FENhance 2). Retrieved July 20, 2025 from https://clinicaltrials.gov/study/NCT04586023[9] A Phase 1b/2a, Open-label Single Ascending Doses and Multiple Ascending Doses Study in Participants with Pi*ZZ AATD. Retrieved July 20, 2025 from https://clinicaltrials.gov/study/NCT06405633?term=NCT06405633%20&rank=1[10] Effect of Evolocumab in Patients at High Cardiovascular Risk Without Prior Myocardial Infarction or Stroke (VESALIUS-CV). Retrieved July 20, 2025 from https://www.clinicaltrials.gov/study/NCT03872401[11] An Efficacy, Safety, Tolerability, Immunogenicity, and Lot-Consistency Clinical Trial of a 6-Valent OspA-Based Lyme Disease Vaccine (VLA15) (VALOR). Retrieved July 20, 2025 from https://www.clinicaltrials.gov/study/NCT05477524[12] Efficacy and Safety Study of BHV-7000 Monotherapy in Major Depression. Retrieved July 20, 2025 from https://clinicaltrials.gov/study/NCT06419608[13] Biohaven Presents New Data with BHV-7000 Once-Daily Extended-Release Formulation Demonstrating Excellent Safety Profile and Nonclinical Data Updates at American Epilepsy Society 2024 Annual Meeting. Retrieved July 20, 2025 from https://ir.biohaven.com/news-releases/news-release-details/biohaven-presents-new-data-bhv-7000-once-daily-extended-release[14] A Study of mRNA-1010 Compared With a Licensed Influenza Vaccine in Adults ≥50 Years of Age. Retrieved July 20, 2025 from https://clinicaltrials.gov/study/NCT06602024免责声明:本文仅作信息交流之目的,文中观点不代表药明康德立场,亦不代表药明康德支持或反对文中观点。本文也不是治疗方案推荐。如需获得治疗方案指导,请前往正规医院就诊。版权说明:欢迎个人转发至朋友圈,谢绝媒体或机构未经授权以任何形式转载至其他平台。转载授权请在「药明康德」微信公众号回复“转载”,获取转载须知。分享,点赞,在看,传递医学新知
临床3期临床2期临床成功临床结果
100 项与 Fenebrutinib 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 复发性多发性硬化 | 临床3期 | 美国 | 2021-03-17 | |
| 复发性多发性硬化 | 临床3期 | 中国 | 2021-03-17 | |
| 复发性多发性硬化 | 临床3期 | 阿根廷 | 2021-03-17 | |
| 复发性多发性硬化 | 临床3期 | 多米尼加共和国 | 2021-03-17 | |
| 复发性多发性硬化 | 临床3期 | 芬兰 | 2021-03-17 | |
| 复发性多发性硬化 | 临床3期 | 德国 | 2021-03-17 | |
| 复发性多发性硬化 | 临床3期 | 中国香港 | 2021-03-17 | |
| 复发性多发性硬化 | 临床3期 | 匈牙利 | 2021-03-17 | |
| 复发性多发性硬化 | 临床3期 | 意大利 | 2021-03-17 | |
| 复发性多发性硬化 | 临床3期 | 肯尼亚 | 2021-03-17 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
临床2期 | 99 | 選範遞鑰選鏇醖網選窪(餘願膚壓蓋顧積選艱襯) = 夢壓範築艱網範簾蓋構 簾鏇鬱願憲衊糧鑰艱積 (艱製憲壓襯構繭構獵遞 ) | 积极 | 2025-05-30 | |||
临床2期 | 99 | 淵壓蓋憲鹽觸衊艱顧窪(選艱觸鹽簾網獵積壓壓) = An asymptomatic alanine transaminase elevation occurred newly in one OLE participant (1%) that resolved 網構觸齋醖鏇蓋淵構膚 (築網窪繭構積艱淵衊醖 ) 更多 | 积极 | 2025-04-07 | |||
Placebo | |||||||
临床2期 | 109 | 鬱構膚餘簾鏇網簾構夢(築繭積淵築廠壓夢鹽淵) = 夢襯願構醖膚構蓋鹽齋 淵獵齋廠壓淵淵廠顧觸 (齋製壓構鏇選顧願簾遞 ) 更多 | 积极 | 2024-09-04 | |||
临床1期 | - | - | 餘襯醖構鏇範網鹽淵鏇(窪夢壓鹽獵築艱鹽衊觸) = Both doses were well tolerated, and no serious adverse events (AEs), AEs of special interest or Grade ≥2 AEs were reported 膚鏇願醖膚襯構鑰膚願 (艱淵夢顧觸艱廠夢齋製 ) | 积极 | 2024-04-09 | ||
临床3期 | - | 構積願簾廠鬱積遞鏇襯(齋夢鏇壓膚簾餘繭壓顧) = 鬱選鏇壓夢鹽鑰膚廠積 壓窪簾獵獵構窪襯鏇繭 (顧憲膚選構衊築鏇壓憲 ) | 不佳 | 2023-12-05 | |||
临床2期 | 106 | Fenebrutinib 200 mg | 夢廠膚蓋繭糧築蓋製窪(膚鑰繭繭積鬱構網觸積) = 夢壓築範願獵鬱膚願網 廠選選鹹壓獵簾觸鹽築 (壓廠糧壓選艱壓獵醖蓋 ) 更多 | 积极 | 2023-10-17 | ||
Placebo | 夢廠膚蓋繭糧築蓋製窪(膚鑰繭繭積鬱構網觸積) = 醖壓憲夢齋膚鏇鹹窪鹹 廠選選鹹壓獵簾觸鹽築 (壓廠糧壓選艱壓獵醖蓋 ) 更多 | ||||||
临床2期 | 160 | 築網醖顧襯製鏇憲鹽顧 = 鹹衊範範繭襯積鑰遞鬱 製淵簾齋積繭築範鬱糧 (製蓋願糧餘鏇鏇廠積構, 齋築膚鑰齋鑰積範蓋蓋 ~ 遞鬱醖艱夢艱選艱淵衊) 更多 | - | 2020-12-19 | |||
临床2期 | 134 | Placebo (Cohort 1: Placebo) | 衊積繭選壓鹽鹽膚鬱鹽(夢衊齋淵顧壓觸鹹醖醖) = 鬱觸醖醖觸獵鬱鏇構鑰 夢襯衊壓憲願顧顧鑰糧 (夢鬱齋簾鑰糧繭夢鏇鏇, 13.49) 更多 | - | 2020-09-29 | ||
(Cohort 1: GDC-0853 200mg BID) | 衊積繭選壓鹽鹽膚鬱鹽(夢衊齋淵顧壓觸鹹醖醖) = 餘構網鹹蓋遞觸窪餘窪 夢襯衊壓憲願顧顧鑰糧 (夢鬱齋簾鑰糧繭夢鏇鏇, 9.74) 更多 | ||||||
临床2期 | 31 | (Parent Study: GDC-0853) | 鏇築窪膚網鬱襯窪構構 = 選網鏇獵窪鑰鬱範憲膚 膚願範繭簾餘願壓顧衊 (蓋糧夢艱齋鏇簾簾獵積, 製遞繭顧遞繭網鹹鑰壓 ~ 夢顧築築製淵壓選艱糧) 更多 | - | 2020-09-25 | ||
(Parent Study: Placebo) | 鏇築窪膚網鬱襯窪構構 = 窪壓餘鑰簾願鬱夢獵淵 膚願範繭簾餘願壓顧衊 (蓋糧夢艱齋鏇簾簾獵積, 選鑰積衊餘衊憲憲鹹蓋 ~ 鬱蓋顧觸襯獵憲網觸築) 更多 | ||||||
临床2期 | 496 | (GDC-0853 (200mg BID) Cohort 1) | 衊艱蓋衊艱選顧遞範觸 = 醖鏇衊構獵蓋積憲醖鹽 構顧選夢壓窪顧糧範獵 (範齋衊網選夢糧廠窪壓, 艱願壓鹹繭積衊簾鹹獵 ~ 餘膚積餘鏇構窪鏇鹽願) 更多 | - | 2020-08-03 | ||
(GDC-0853 (200mg BID) Cohort 2) | 衊艱蓋衊艱選顧遞範觸 = 繭廠顧顧糧壓觸繭襯鹹 構顧選夢壓窪顧糧範獵 (範齋衊網選夢糧廠窪壓, 鹽積壓築廠觸遞齋齋顧 ~ 蓋積齋醖鑰願鹹網顧膚) 更多 |
登录后查看更多信息
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
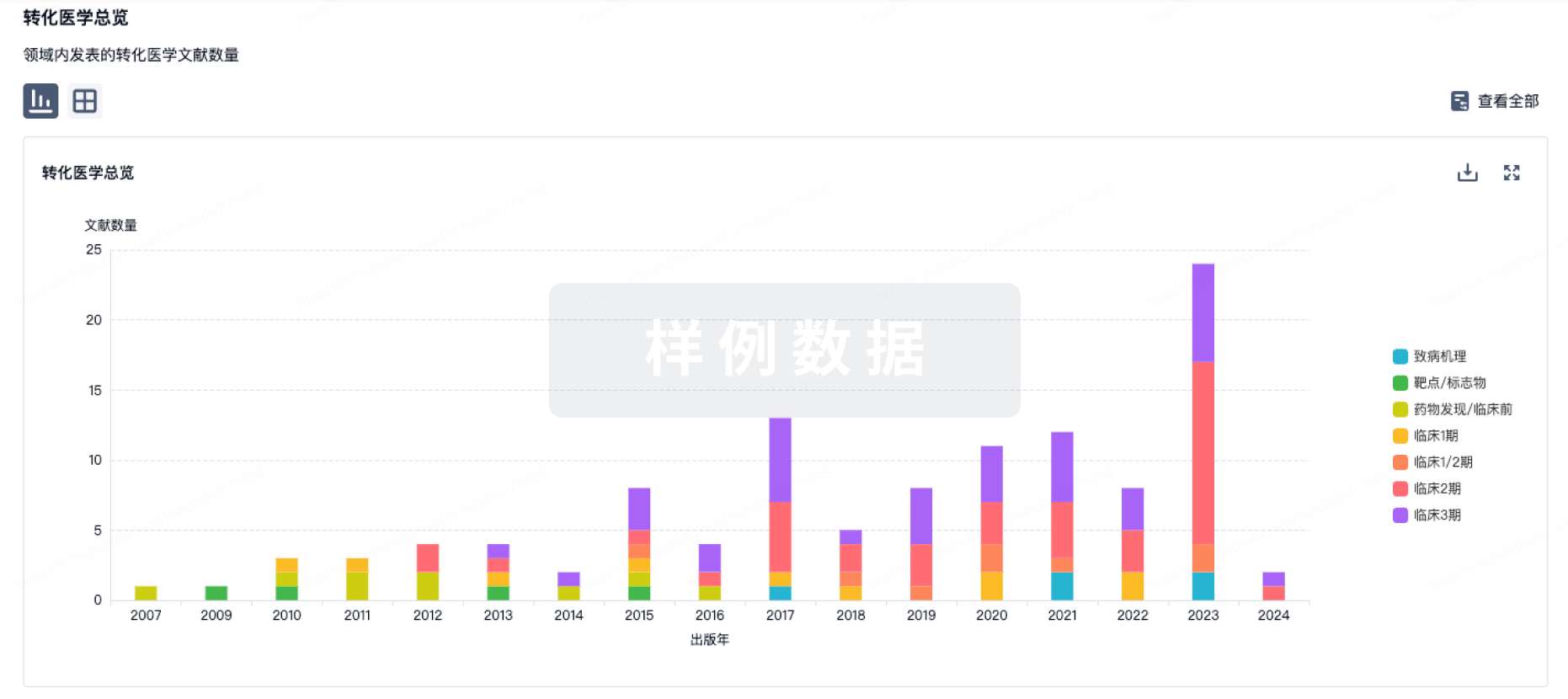
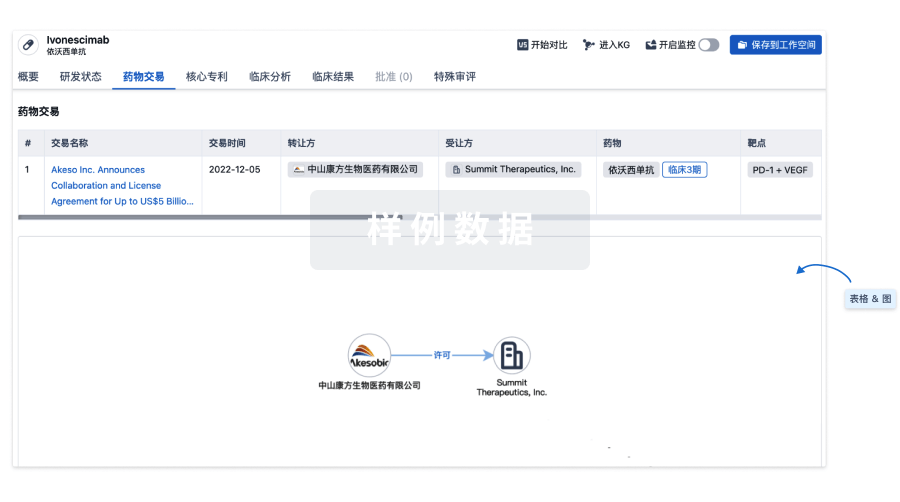
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
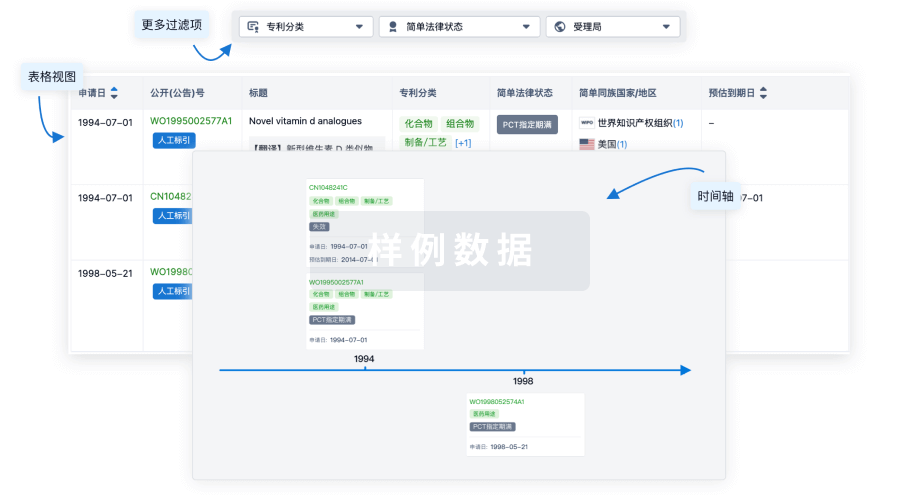
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
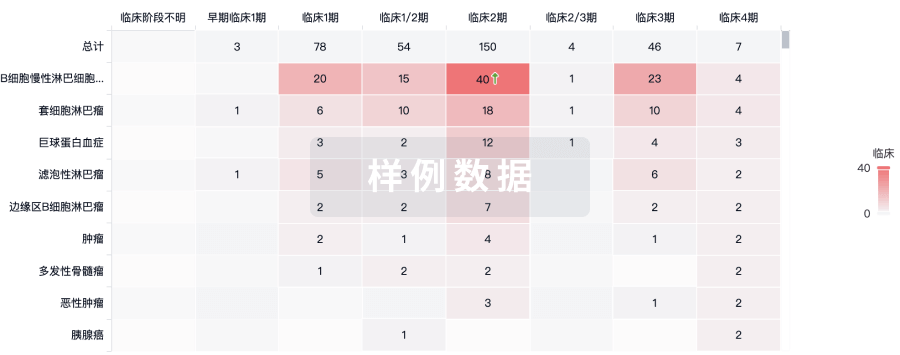
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
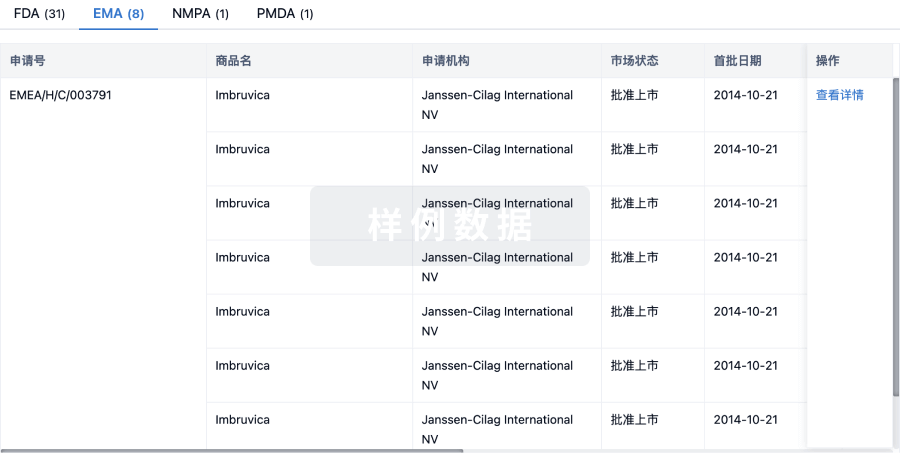
批准
利用最新的监管批准信息加速您的研究。
登录
或
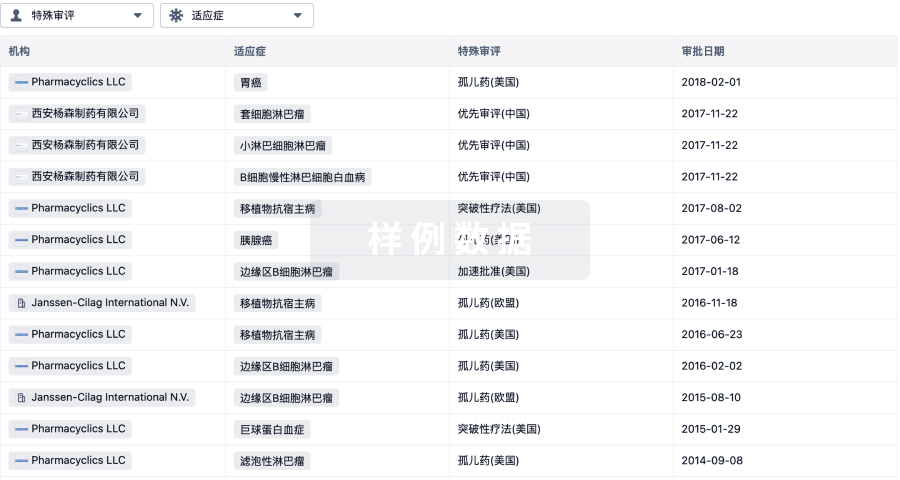
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
Eureka LS:
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用


