预约演示
更新于:2025-05-07

Aprinoia Therapeutics, Inc.
更新于:2025-05-07
概览
标签
神经系统疾病
其他疾病
内分泌与代谢疾病
诊断用放射药物
小分子化药
化学药
疾病领域得分
一眼洞穿机构专注的疾病领域
暂无数据
技术平台
公司药物应用最多的技术
暂无数据
靶点
公司最常开发的靶点
暂无数据
| 排名前五的药物类型 | 数量 |
|---|---|
| 诊断用放射药物 | 4 |
| 小分子化药 | 2 |
| 蛋白降解药物 | 1 |
| 单克隆抗体 | 1 |
| 化学药 | 1 |
| 排名前五的靶点 | 数量 |
|---|---|
| TAU(微管相关蛋白tau) | 5 |
关联
7
项与 新旭生技股份有限公司 相关的药物靶点 |
作用机制 TAU调节剂 |
在研机构 |
原研机构 |
最高研发阶段临床3期 |
首次获批国家/地区- |
首次获批日期- |
靶点 |
作用机制 TAU抑制剂 [+1] |
在研机构 |
非在研适应症- |
最高研发阶段临床2期 |
首次获批国家/地区- |
首次获批日期- |
靶点 |
作用机制 TAU抑制剂 |
在研机构 |
原研机构 |
在研适应症 |
非在研适应症- |
最高研发阶段临床1期 |
首次获批国家/地区- |
首次获批日期- |
7
项与 新旭生技股份有限公司 相关的临床试验NCT05344989
A Phase 1, Randomized, Double-Blind, Placebo-Controlled, Single Ascending Dose Study to Evaluate the Safety, Tolerability, Pharmacokinetics, and Immunogenicity of APNmAb005 in Healthy Subjects
This is a Phase 1, first-in-human (FIH), double-blinded, placebo-controlled study where healthy subjects are randomly allocated to receive APNmAb005 or placebo. Approximately 5 dosing groups (cohorts) are planned with 8 subjects (randomized to 6 active: 2 placebo) per cohort. the starting dose of APNmAb005 is 5 mg/kg and the anticipated doses for subsequent cohorts are 10, 25, 50 and 70 mg/kg. A Safety Review Team (SRT) will review data on an ongoing basis throughout the study and before progression to the next dose level cohort.
Subjects will receive a single dose of either APNmAb005 or placebo administered as a single IV infusion on Day 1 of the study and will remain in the study center until Day 3 (48 hours after dosing). They will return to the study center for 7 outpatient visits. The duration of the study, excluding screening, is approximately 71 days.
Subjects will receive a single dose of either APNmAb005 or placebo administered as a single IV infusion on Day 1 of the study and will remain in the study center until Day 3 (48 hours after dosing). They will return to the study center for 7 outpatient visits. The duration of the study, excluding screening, is approximately 71 days.
开始日期2022-05-06 |
申办/合作机构 |
NCT04141150
A Phase 2, Multicenter Study of [18F]APN-1607 Positron Emission Tomography in Subjects With Alzheimer's Disease Compared to Healthy Subjects
The overall objective of this study is to compare the overall pattern of [18F]APN-1607 uptake in subjects with MDAD, subjects with AD dementia, and healthy subjects.
开始日期2022-03-22 |
申办/合作机构 |
NCT05542953
A Phase 3, Multicenter Study of [18F]APN-1607 Positron Emission Tomography in Subjects With Alzheimer's Disease Compared to Healthy Subjects
The overall objective of this study is to compare the overall pattern of [18F]APN-1607 uptake in subjects with MCI, subjects with AD dementia, and healthy subjects.
开始日期2022-02-11 |
申办/合作机构 |
100 项与 新旭生技股份有限公司 相关的临床结果
登录后查看更多信息
0 项与 新旭生技股份有限公司 相关的专利(医药)
登录后查看更多信息
19
项与 新旭生技股份有限公司 相关的文献(医药)2025-03-11·Neurology
Self-Reported REM Sleep Behavior Disorder in Patients With Progressive Supranuclear Palsy
Article
作者: Zhao, Jue ; Zuo, Chuantao ; Yen, Tzu-Chen ; Wu, Jianjun ; Chan, KunWang ; Tang, Yilin ; Sun, Yi-Min ; Zhang, Qin ; Liang, Xiaoniu ; Tang, Gan ; Wang, Jian ; Li, Xin-Yi ; Wang, Jing ; Shen, Bo ; Lu, Jiaying ; Lin, Huamei ; Liu, Feng-Tao ; Zhao, Yixin
2025-02-01·Journal of Neurology
Patterns of Tau pathology in patients with anti-IgLON5 disease visualized by Florzolotau (18F) PET
Article
作者: Yen, Tzu-Chen ; Jia, Chenhao ; Guan, Hongzhi ; Cui, Ruixue ; Fan, Siyuan ; OuYang, Chujun ; Huang, Zhaoxia ; Li, Qijun ; Liang, Menglin ; Ren, Haitao ; Zhang, Tianhao
2025-01-01·European Journal of Nuclear Medicine and Molecular Imaging
Visual reading for [18F]Florzolotau Tau PET scans in progressive supranuclear palsy
Article
作者: Li, Xin-Yi ; Sun, Yi-Min ; Lu, Jia-Ying ; Rominger, Axel ; Lu, Jie ; Guan, Yi-Hui ; Lan, Xiao-Li ; Brendel, Matthias ; Cui, Rui-Xue ; Chen, Ming-Jia ; Tang, Gan ; Yao, Rui-Xin ; Zuo, Chuan-Tao ; Xu, Hao ; Wang, Jian ; Yen, Tzu-Chen ; Jiao, Fang-Yang ; Ge, Jing-Jie ; Liu, Feng-Tao ; Shi, Kuangyu ; Zhao, Jun
43
项与 新旭生技股份有限公司 相关的新闻(医药)2025-02-22
·药智网
近日,诺华公布2024年的最新业绩显示,旗下两款核药(Lutathera和Pluvicto)在过去一年共计为其贡献了21.16亿美元,且增长态势明显。其中,刚上市三年的Pluvicto 2024全年销售额达到13.92亿美元,同比增长42%,早已成为全球首个核药十亿美元分子(其前三季度累计销售额已超10亿美元)。
被外界寄予厚望的Pluvicto似乎已成为核药领域的风向标,搅动了2025开年的一池春水。
1
全方位布局
RDC是一种将精准靶向分子(单抗或多肽/小分子,Ligand)和强力杀伤因子(核素,Radioisotope)用连接臂(Linker)螯合剂(Chelator)偶联在一起而设计开发的药物形态;得益于其特殊的作用机制,RDC可实现高精度诊断及在治疗疾病的过程中具有不易耐药等优点,被认为是目前核药靶向治疗领域最具潜力的发展方向之一。
在全球核药市场中,诺华凭借一系列战略性收购和布局,已占据领先地位。2017年和2018年,诺华分别收购了法国公司AAA和美国公司Endocyte,从而获得了Lutathera和Pluvicto两款RDC标杆产品。这两款药物分别靶向SSTR和PSMA,用于治疗神经内分泌肿瘤和前列腺癌。
根据诺华管线披露情况,目前针对Pluvicto仍有四个适应症在研,其中针对转移性激素敏感前列腺癌(mHSPC)的研究处于Ⅲ期临床阶段,预计于2025年完成并计划提交申请。结合Pluvicto当下强劲的放量势头和诺华对其在适应症扩展、准入地区扩张和商业化上的进一步布局,该药未来可期。
除了已获批上市Pluvicto和Lutathera适应症扩展研究外,诺华的内部管线还包括多款创新靶点的Lu-177(如靶向FAP的AAA614和靶向GRPR的AAA603)。研究显示,FAP在肺癌、胰腺癌等多种实体瘤中高表达,而GRPR在乳腺癌、前列腺癌、胶质瘤等患者的肿瘤中呈过表达,这些特点可以为放射性配体开辟更广阔的临床应用空间。目前,这两款药物正在针对多种实体瘤开展I/Ⅱ期临床试验。
除了靶点创新外,诺华还将目光锁定在当前炙手可热的α核素-Ac-225身上。α核素与β核素相比,α核素放射性药物用于肿瘤治疗具有独特的优势,包括肿瘤杀灭效果好且不易复发;α核素射程短,对正常组织损伤极小且几乎无副作用,安全性更高。另外α核素杀伤癌细胞的同时可以引发肿瘤免疫反应,与免疫疗法有相互促进的作用,使肿瘤治疗达到“一加一大于二”的效果。
作为α核素的Ac-225的半衰期为9.9天,长于Lu-177的6.647天,生产、治疗时间更为充足,并且基于其释放的α粒子的特性,结合Ac-225开发的药物,有效性和安全性方面在理论上会比Lu-177更有优势。
AAA817是一款Ac-225标记的靶向PSMA的RDC,即将进入临床Ⅱ/Ⅲ期,也是诺华在研核药中进展最快的资产,有望接力Lutathera、Pluvicto这两款诺华的RDC明星核药,成为下一款RDC“重磅炸弹”。
除了AAA817外,诺华还布局了下一代Ac-225核药Ac-PSMA-R2,在2023年末启动了无论是否接受过177Lu-PSMA靶向治疗的转移性激素敏感性前列腺癌(mHSPC)和转移性去势抵抗性前列腺癌(mCRPC)患者的临床I/Ⅱ期试验,预计2027年完成此项临床研究。
此外,尝到“甜头”后诺华还在持续加大投资与合作力度,2024年4月和5月先后达成两项总计46.5亿美元的合作,包括与PeptiDream共同开发多款大环肽靶向偶联核药,以及收购Mariana Oncology加码放射性配体疗法。
2
MNC纷纷加码
从全球市场来看,RDC凭借其作为唯一实现诊疗一体化的核药类型的优势,已成为市场增长的核心引擎。根据BBC Research的数据显示,RDC的全球市场规模预计将在2026年达到175亿美元。面对日益增长的全球核药市场这块“肥肉”,恐怕没有哪家MNC想错过。
拜耳作为较早布局核药赛道的MNC,早在2009年就与Algeta联合开发Xofigo(氯化镭223),并于2013年获批上市,用于治疗晚期骨转移型去势抵抗性前列腺癌。Xofigo虽然也是核药但与诺华的镥-177并不完全相同,Xofigo是全球首个α粒子辐射放射性治疗药物。除此之外,拜耳仍在专注于开发靶向α粒子的疗法。目前拜耳共有2个处于早期临床阶段RDC在研,且都靶向α核素225Ac,启动针对mCRPC的临床I期试验,设置了多个队列,其中包括177Lu-PSMA耐药的患者。
礼来早在2006年便开始关注核药,并成为近两年来核药领域最活跃的金主之一。就在2023年9月,礼来以1.75亿美元投资核药研发公司Mariana Oncology,而就在一个月后,以14亿美元收购核药生物技术公司Point Biopharma。进入2024年,礼来先在5月宣布与Aktis Oncology达成多靶点发现合作协议,使用Aktis的新型微蛋白技术平台生产抗肿瘤放射性药物。随后又宣布与Radionetics Oncology达成战略合作,推进Radionetics的专有GPCR靶向小分子放射性药物研发进展。而根据协议条款,Radionetics收到了1.4亿美元预付款,而作为战略合作的一部分,礼来还拥有未来以10亿美元收购Radionetics的独家选择权。2025开年之际,礼来又与AdvanCell达成的协议,双方将整合AdvanCell专有的Pb212(铅-212)生产技术与核素开发基础设施,以及礼来的药物候选项目和丰富的药物开发经验,共同推动更多靶向α放射性核素疗法的开发,并加速其临床进展。
除了诺华、拜耳和礼来,其他跨国药企如阿斯利康、默沙东、强生、罗氏和赛诺菲等也通过股权投资、技术引进等方式积极进入核药领域,近年来百亿美元的核药赛道持续升温,已经成为全球制药巨头们的必争之地。
3
国内企业加快布局
在过去相当长的一段时间里,中国核药市场呈现出双雄争霸的竞争格局,中国同辐和东诚药业作为行业巨头,长期占据主导地位。然而,近年来,这一格局正在悄然发生变化。随着核药市场的潜力逐渐被挖掘,越来越多的新鲜血液涌入这一领域。
如今,包括恒瑞医药、远大医药、先通医药、瑞迪奥、辐联医药、核欣医药等在内的近20家药企纷纷加速布局核药赛道。这些新兴力量凭借敏锐的市场洞察力和强大的研发能力,迅速崭露头角,成为推动中国核药市场发展的新生力量。与此同时,它们也凭借自身的优势和潜力,赢得了资本市场的高度关注与青睐。
东诚药业是国内核药全产业链布局的标杆企业,拥有核素供应、药物孵化、生产配送等五大平台,覆盖国内93.5%人口的核医学需求。核药方面,核素药物产品丰富,主要产品云克注射液(锝[99Tc]亚甲基二膦酸盐注射液)是中国自主研发的用于类风湿性关节炎(RA)临床治疗的核素药物,而碘[131I]化钠口服溶液和碳[14C]尿素胶囊是临床上最常用的核药品种之一。此外,东诚药业近年来着力打造1.1类放射性诊疗一体化药物创新平台—烟台蓝纳成,其具有放射性诊疗一体化药物创新研发和全球领先的纳米递送技术的特点,适应症涵盖前列腺癌、胃癌、结直肠癌、鼻咽癌等多种癌症的诊断与治疗产品,其中部分产品进行中美双报,靶向PSMA诊断药物氟[18F]思睿肽注射液正在进行Ⅲ期临床试验,靶向FAP的诊断用药物氟[18F]纤抑素注射液已完成I期临床试验,靶向FAP的177Lu-LNC1004注射液已经在2023年分别取得了美国、新加坡和中国的临床批件,并在去年11月获得了FDA授予的快速通道资格,用于治疗接受过一种及以上酪氨酸激酶抑制剂的转移性碘-131难治性分化型甲状腺癌患者。
远大医药作为国内RDC领域的领头企业,通过全球化并购与合作(如收购Sirtex、参股Telix、合作德国ITM),构建了覆盖肿瘤诊疗一体化的核药平台。其管线包括10款全球创新产品,涵盖68Ga、177Lu、131I等多种核素,适应症覆盖肝癌、前列腺癌等8大癌种。目前已有三款RDC药物进入Ⅲ期临床,包括诊断前列腺癌的产品TLX591-CDx、诊断透明细胞肾细胞癌产品TLX250-CDx,以及治疗GEP-NETs的产品ITM-11。截至目前,远大医药是进入中国Ⅲ期临床研究中诊断和治疗类RDC创新药储备最多的企业。
“医药一哥”恒瑞医药也算是比较早布局核药赛道的玩家,恒瑞医药在2020年成立了天津恒瑞,后者已布局5款核药管线,包括三款治疗用核药HRS-4357、镥[177Lu]氧奥曲肽注射液和HRS-6768,以及两款诊断用核药HRS-9815、镓[68Ga]伊索曲肽注射液。其中,HRS-9815用于前列腺癌诊断、HRS-4357用于转移性去势抵抗性前列腺,均靶向PSMA。而近期获批临床的HRS-6768则是一款靶向成纤维细胞激活蛋白α(FAP-α)的RDC。
去年5月,中药龙头云南白药子公司云核医药的1类新药INR101注射液获得NMPA临床试验默示许可,正式宣告杀入核药赛道。INR101注射液是云核医药研发的化学1类放射性诊断类创新药,适用于前列腺癌患者PSMA阳性病灶的PET成像。与此同时,国内核药新兴力量也正走入舞台中间。智核生物、辐联医药、核欣医药、晶核生物、禾泰健宇、诺宇医药、新旭医药等也各具特色,有望成为核药赛道的重要玩家。
参考来源:
[1]Next generation radiotheranostics promoting precision medicine.
[2]Radiotheranostics in oncology:current challenges and emerging opportunities.
[3]Radiopharmaceutical therapy in cancer:clinical advances and challenges.-
[4]《诺华管线梳理》Pharma知产视界
[5]《巨头重注核药赛道》医曜
声明:本内容仅用作医药行业信息传播,为作者独立观点,不代表药智网立场。如需转载,请务必注明文章作者和来源。对本文有异议或投诉,请联系maxuelian@yaozh.com。
责任编辑 | 史蒂文
合作、投稿、转载开白 | 马老师 18323856316(同微信)
阅读原文,是受欢迎的文章哦
免疫疗法临床3期并购临床2期
2024-11-06
核药“爆局”看中国,中国核药,看成都。
里程碑时刻!
诺华2024 Q3财报显示,核药(放射性药物)、RDC明星产品Pluvicto已经入列“十亿美元分子”阵营,前三季度收入达10.41亿美元(+47%)。这仅是Pluvicto商业化第三年。
“核”爆级创新药机遇,正在孕育。全球核药市场将由2023年的84亿美元加速提升至2030年的294亿美元,年复合增长率达20%。中国核药市场规模,也有望于2023年的78亿元,涨至2030年的260亿元。
不得不提,中国在这一技术赛道表现出了未曾预想到的生机与活力。核药产业在中国已成为国家重点支持的战略性新兴产业,多项利好政策陆续出台。
“场子”已经大热。双寡头中国同辐、东诚药业“翻红”,远大医药、恒瑞医药不再低调,乘势加快RDC研发进度,连云南白药也正式入局,在10月底拿到了辐射安全许可证。新生代核药公司渐次崛起,先通医药、智核生物、新旭医药、晶核生物、纽瑞特、通瑞生物、艾博兹医药等创新企业完成了亿元级融资。此外,今年诺华在中国的首个放射配体疗法生产基地奠基开建,也体现了中国市场作为核药布局具有战略意义的市场的重要性。
但众所周知,核药虽火,但在研发、生产制造供应、质量保证、物流运输、对应疾病领域销售经验,以及使用医用同位素进行治疗是否有特定就医环境等诸多方面,都还有很多难题未解决。想要入局、占位、站稳,最核心的,是依赖生态,以及有产业链资源可赋能。
在这一方面,地方性核药产业优势显得至关重要。而纵览近两年中国凭融资等“一炮而红”出圈的核药企业,如先通生物、辐联科技、艾博兹、通瑞生物、纽瑞特等,几乎都奔向、聚集在了同一个地方——成都。
成都的“野心”,藏不住了
就在两天前,11月4日,云克药业核药生产基地正式在成都落成。该基地是国内规模较大、功能齐全的核药产业基地,集成了医用同位素生产线、放射性药品研发平台和生产线、放射性药品CMO、CDMO、CSO平台,将为四川省核医疗产业的高质量发展增添重要的孵化和成果转化平台。
云克药业,国内专注于核素治疗的隐形王者,拥有从医用同位素和核素药物研发、生产、销售到核医疗专科医院的核医疗全产业链,已成功开发国内单品种销售额最高且具有自主知识产权的治疗类风湿性关节炎和骨疾病国际独家创新药品,其自主开发的精密逆流萃取器分离平台解决了90Y、223Ra等治疗用核素规模化生产“卡脖子”问题,在核素治疗药物的研发和供应上处于国内领先地位。
这样一家企业选择成都,其对这一城市核药产业配套和企业服务能力的认可,显而易见。
2023年上半年,正值资本寒冬,先通医药逆势完成超11亿元新一轮融资,这是当时最大的一笔市场化融资。今年7月,成立仅3年的辐联科技以5.715亿美元的交易总额,授权SK公司对于FL-091核药在全球范围内进行临床研究、开发、生产和商业化的独家权利,成为国内核药领域License-out首单。两家企业,也都落地在了成都。
另外,RDC产品数量和进度在国内数一数二,拥有核药全产业链布局的远大医药,早前历时600天时间,跑遍全国选址,经过长久而细致地对比、权衡,最终决定将斥资百亿收购的钇[90Y]树脂微球及核药板块,落户在了成都温江。
整体来看,在RDC领域,远大医药、先通生物、辐联科技、艾博兹、通瑞生物、纽瑞特等诸多明星核药企业,齐齐来自或落地成都。
而在远大医药落地前,成都拥有药明康德核药研究中心、省药检院、省辐射监测站等重要平台,以及华西医院等3家三甲医院核医学科,覆盖了从同位素供给,到研发,生产,再到运输,应用的全产业链发展体系。
除了药物研发企业,核医疗设备企业也纷纷选择落地成都。如一家名为永新医疗的公司,手握有望打破进口垄断格局的Insight四维定量SPECT/CT产品,今年,这家公司选择将总部落户在这一城市。
公开数据显示,目前国内上市的100多个核药,产品数量位居TOP15的企业,主要来自成都,如成都中核高通同位素股份有限公司,云克药业和华神生物。
为什么?
成都的产业链优势,也藏不住了
实际上,核药的快速发展,离不开整个核产业在成都的布局。
成都拥有一批国内顶尖的医用同位素及药物研发、药物安全性评价、药物临床试验及应用单位,还有多个医用同位素及药物领域的国家、省级科研平台及雄厚的创新资源优势。
目前,成都已形成“两中心四基地”核技术应用产业布局,并培育了核电装备、辐照加工、核医疗、核医药等细分领域产业,成为全国核技术应用产业发展新高地。2021年,由中国核动力研究设计院牵头组建同位素及药物国家工程研究中心,2022年该中心正式落户成都双流。中国核动力研究设计院已在四川布局形成核技术“两堆生产、两堆研发”之势,已攻克碳-14、锶-89、磷-32、碘-131、碘-125等同位素制备技术,成为全球医用同位素及药物的重要供应基地。
医用同位素是放射性药物的必要成分。但此前,目前,国内医用同位素需求量大,年增长率高,但严重缺乏医药同位素供应,且自主化产能低、缺口大、严重依赖进口,在买卖关系中处于较弱势地位,难以掌握定价权。
不过,这一情况正在得到改善。
公开资料显示,全国80%以上的医用同位素都是“四川造”,成都周围便拥有3座在役反应堆,能够提供镥-177、钇-90等14种医用同位素。
今年1月30日,国内首座医用同位素专用生产堆在四川开工建设,2027年建成投产后,将实现年产10万居里的钼-99、2万居里的碘-131。据业内人士根据市场需求估算,2万居里的碘-131刚好可以满足国内需求,10万居里的钼-99还有余量可以出口,反应堆的建成将让我国从进口国扭转为出口国。
无疑,这能为中国核药在国际舞台上建立起绝对的竞争优势。
战略上,基于产业资源,打造“ADC+RDC”双子塔,恰好是成都生物医药树立的清晰战略定位之一。而目前从成都“走”出来的ADC及RDC成果,有效诠释了这一定位。
政策上,多份文件连连释放支持信号。
今年1月,成都出台《关于前瞻培育未来产业构筑高质量发展新动能的实施意见》《关于前瞻培育未来产业的政策措施》,聚焦6大领域24条赛道,在“前沿生物”这一领域中,出现了“核医药”三个字。
今年7月发布的《关于促进核医疗产业高质量发展的意见》,提出以乐山、成都、绵阳、泸州为重点区域,一体推进科技创新和科技成果产业化,聚力打造贯通医用同位素生产、放射性药物研发、核医疗装备制造、临床应用推广的全产业链,形成“一链四极”的发展格局。
不过,建立产业链优势非一朝一夕之功,要想真正使中国核药崛起,实现国产化,攻克核药的难题,仍旧是一场长期的战役。
以眼下最火的RDC(放射配体疗法)为例,由于用于放射配体疗法的放射性同位素的半衰期很短,从制备到用药的时间控制必须非常精确,因此对放射性同位素和成品药物的生产与配送提出了极高的要求。现在国内虽然拥有了放射性同位素生产所必需的反应堆设计、试验及运行基础,但尚未形成较大产能。
另一面,虽然近年来核药中游明显表现出生机,但尚未形成研发能力。受上游卡脖子影响,研发与产业化进展缓慢。而初步跨入该领域的企业,一些在较长时间内体现出“三无”缺点:没有团队、亟需人才,没有资质,没有产品。
那么,如何核药的商业化问题(上游放射性同位素供应、运输,流程和配送等)?如何解决核药的安全性、有效性难题(非临床评价、CMC等)?如何解锁更多具备差异化的RDC创新产品?
由中国医药企业管理协会、中国医药生物技术协会、四川省医药行业协会主办、E药经理人承办的2024’第十六届中国医药企业家科学家投资家大会(2024启思会)召开在即。核药创新论坛作为大会的重要环节将于11月13日在成都举行。论坛将聚焦国内外核药发展趋势、研发难点、临床转化等热点问题,汇集数十家核药企业管理者,旨在为核药产业搭建有效的交流平台。
会议时间:2024年11月13日14:30-18:00
会议地点:成都生物城文化中心负一楼重楼厅(成都双流区·永安镇慧云路1号)
参会人员:核药企业董事长、CEO和研发负责人,医药分析师,投资人,园区相关负责人,核药产业链机构等
会议报名请联系:
Mia 15801222461 (同微信) map8581@163.com
扫描下方二维码,加入核药创新论坛嘉宾群
一审| 黄佳
二审| 李芳晨
三审| 李静芝
精彩推荐
CM10 | 集采 | 国谈 | 医保动态 | 药审 | 人才 | 薪资 | 榜单 | CAR-T | PD-1 | mRNA | 单抗 | 商业化 | 国际化 | 猎药人系列专题 | 出海
启思会 | 声音·责任 | 创百汇 | E药经理人理事会 | 微解药直播 | 大国新药 | 营销硬观点 | 投资人去哪儿 | 分析师看赛道 | 药事每周谈 | 医药界·E药经理人 | 中国医药手册
创新100强榜单 | 恒瑞 | 中国生物制药 | 百济 | 石药 | 信达 | 君实 | 复宏汉霖 |翰森 | 康方生物 | 上海医药 | 和黄医药 | 东阳光药 | 荣昌 | 亚盛医药 | 齐鲁制药 | 康宁杰瑞 | 贝达药业 | 微芯生物 | 复星医药 |再鼎医药|亚虹医药
跨国药企50强榜单 | 辉瑞 | 艾伯维 | 诺华 | 强生 | 罗氏 | BMS | 默克 | 赛诺菲 | AZ | GSK | 武田 | 吉利德科学 | 礼来 | 安进 | 诺和诺德 | 拜耳 | 莫德纳 | BI | 晖致 | 再生元
财报放射疗法
2024-07-30
点击上方的 行舟Drug ▲ 添加关注
报告由上海交通大学医学院附属仁济医院王刚教授牵头,组织中国疾病预防控制中心慢性非传染性疾病预防控制中心、复旦大学公共卫生学院、上海市精神卫生中心、上海交通大学医学院附属瑞金医院、福建医科大学等多家权威机构的专家学者共同编撰。
一
摘要
近年来,中国的AD发病率、患病率和死亡率均呈现上升趋势,对患者家庭、社会乃至整个医疗保健系统构成了沉重的经济负担。为了积极应对这一挑战,响应国家“健康中国行动”的号召,推动医疗模式从疾病治疗向健康维护转变,由上海交通大学医学院附属仁济医院牵头,组织中国疾病预防控制中心慢性非传染性疾病预防控制中心、复旦大学公共卫生学院、上海市精神卫生中心、上海交通大学医学院附属瑞金医院、福建医科大学等多家权威机构的专家学者,共同编撰了《中国阿尔茨海默病报告2024》。本报告将为AD的预防、诊断和治疗提供科学的技术指导和有力的数据支持,为政府和相关部门制定针对性的卫生政策和干预措施提供专业依据,同时也为促进国内外在该领域的学术交流与合作搭建平台。
背景
根据2022年第八次全国人口普查结果显示,我国目前60岁及以上人口为28004万人,占全国总人口的19.8%,其中65岁以上人口为20978万人,占14.9%,正式进入深度人口老龄化阶段,而与深度老龄化相关疾病的发病率、患病率及死亡率也均随之显著增高,给社会带来沉重压力。其中,阿尔茨海默病(Alzheimer’sdisease,AD)的发病人数持续增加,社会经济负担日益明显,已成为严重危害我国城乡居民的重大疾病和社会问题。2019年,中国AD及其他痴呆患病人数为13143950例(1314万),约占全球数量的25.5%,我国年龄标化和患病率为788.3/10万。而AD及其他痴呆导致的死亡人数,我国死亡人数为320715例(32万),占全球的19.8%。2019年,全球AD及其他痴呆的疾病负担为25276989(2527万)人年,其中23.6%的负担来源于中国。
一
数据来源及分析方法
1.1 疾病负担
(详见《中国阿尔茨海默病报告2024》)
1.2 相关研究数据
为更新自《中国阿尔茨海默病报告 2021》发布以来 AD 药物及非药物临床治疗新进展作者根据循证 (PICOSparticipant,intervention,comparison,outcome, study design)问题系统检索了自 2021 年 8月至 2024年 1月在中国开展的 AD 治疗相关研究。纳入标准为符合以下所有条件:①西药、中药及非药物干预,包括上市药物、临床试验药物(国内外多中心试验)、临床试验药物(国内);②国内外临床注册的单中心或多中心试验;③AD患者(包括中国人群);④发表时间为 2021 年 8 月 1 日至 2024 年 1月31日。排除标准为无干预对照组试验。检索过程及结果如图 1 所示。最终纳入新注册并在更新进展的 AD 治疗临床试验共 64 项,其中靶向 Aβ 蛋白治疗有 12 项,神经调控治疗 17 项,中医药治疗13项,及其他靶点药物22项(见图2)。
图1 AD的药物及药物治疗检索策略
图2 AD的流行病及疾病负担
二
AD的流行病学及疾病负担
研究提出,2021年我国现存的AD及其他痴呆患病人数达16990827(将近1700万)例,全国各省及直辖市(各省市)的AD及其他痴呆发病率为(90.8~326.4)/10万,各省市的年龄标化发病率为(137.0~158.8)/10万。2021年,我国AD及其他痴呆的患病率为1194.2/10万,年龄标化患病率为900.8/10万;死亡率为34.6/10万,年龄标化死亡率为30.9/10万。我国AD及其他痴呆的患病率、死亡率等随着年龄增加不断上升,且女性的相关数据高于男性,其中女性的患病率(1558.9/10万)、死亡率(47.4/10万),高于男性的患病率(846.3/10万)、死亡率(22.5/10万)。
2.1 我国和全球AD及其他痴呆的疾病负担比较
(详见《中国阿尔茨海默病报告2024》)
2.2 2021年我国AD及其他痴呆的死亡情况
2.2.1 分性别的AD及其他痴呆的死亡情况
如表 1 所示,2021 年我国因 AD 及其他痴呆导致的死亡者中,女性死亡人数远大于男性,男性死亡率为 22.5/10 万[(5.3~64.0)10 万],女性死亡率为47.4/10 万[(11.9~126.2)10 万],女性死亡率是男性的2倍以上。年龄标化后,女性的标化死亡率仍高于男性(33.9/10万比25.9/10万)。
表1 2021年中国AD及其他痴呆的死亡情况
2.2.2 分年龄组的AD及其他痴呆的死亡情况
(详见《中国阿尔茨海默病报告2024》
2.2.3 分省市的AD及其他痴呆的死亡情况
(详见《中国阿尔茨海默病报告2024》)
2.2.4 1990年至2021年我国AD及其他痴呆的死亡率变化
1990至2021年,我国AD及其他痴呆的总的粗死 亡 率 由 10.2/10 万 增 长 至 34.6/10 万 ,增 长239.2%。年龄标化后,我国 AD 及其他痴呆的标化死亡率总体呈现平稳趋势,总标化死亡率在 29.5/10 万~31.5/10 万小范围内波动。分性别看,女性AD及其他痴呆的粗死亡率和标化死亡率始终高于男性(见图4)。
图4 1990年至2021年我国AD及其他痴呆的死亡率变化
2.3 2021年我国AD及其他痴呆的发病情况
2.3.1 分性别的AD及其他痴呆的发病情况
如表 3 所示,2021 年我国 AD 及其他痴呆的发病人数达2914 112 例(908448 例~1248194 例),其中男性发病率为148.0/10万[(124.8~171.4)10万],女性发病率为264.4/10万[(229.4~302.5)10万],女性发病率明显高于男性,约为男性的 1.8 倍。年龄标化后,女性的标化发病率仍高于男性(171.8/10万比126.5/10万)。
表3 2021年中国AD及其他痴呆的发病情况
2.3.2 分年龄组的AD及其他痴呆的发病情况
(详见《中国阿尔茨海默病报告2024》)
2.3.3 分省市的AD及其他痴呆的发病情况
(详见《中国阿尔茨海默病报告2024》)
2.3.4 1990年至2021年我国AD及其他痴呆的发病率变化
1990至2021年,我国AD及其他痴呆的粗发病率由 59.8/10 万增长到 204.8/10 万,增长 242.5%。年龄标化后,标化发病率总体呈现波动式缓慢上升的趋势,其中女性的标化发病率由135.4/10万增长到 171.8/10 万,增长 26.9%;男性的标化发病率由100.2/10 万增长到 126.5/10 万,增长 26.2%。女性AD及其他痴呆的发病率和标化发病率始终高于男性(见图6)。
图6 1990年至2021年我国AD及其他痴呆的发病率变化
2.4 2021年我国AD及其他痴呆的患病情况
2.4.1 分性别的AD及其他痴呆的患病情况
如表 4 所示,2021 年我国现存的 AD 及其他痴呆的患病人数达 16 990 827 例(14 488 494 例~19 672 741 例),其 中 男 性 患 病 率 为 846.3/10 万[(706.3~980.9)10 万],女性患病率为 1 558.9/10 万[(1 341.1~1 801.8)10 万],女性患病率明显高于男性,约为男性的1.8倍。年龄标化后,女性的标化患病率仍显著高于男性(1 025.1/10万比731.2/10万)。
表4 2021年中国AD及其他痴呆的患病情况
2.4.2 分年龄组的AD及其他痴呆的患病情况
(详见《中国阿尔茨海默病报告2024》)
2.4.3 分省市的AD及其他痴呆的患病情况
(详见《中国阿尔茨海默病报告2024》)
2.4.3 分省市的AD及其他痴呆的患病情况
(详见《中国阿尔茨海默病报告2024》)
2.4.4 1990年至 2021年我国 AD 及其他痴呆的患病率变化
1990至2021年,我国AD及其他痴呆的总患病率由342.1/10万增长到1194.2/10万,增长249.1%。年龄标化后,标化患病率总体呈现波动式缓慢上升的趋势,其中女性的标化患病率由785.2/10万增长到1025.1/10万,增长 30.6%;男性的标化患病率由574.5/10 万增长到 731.2/10 万,增长 27.3%。女性AD及其他痴呆的患病率和标化患病率始终高于男性(见图8)。
图8 1990年至2021年我国AD及其他痴呆的患病率变化
本报告中对比我国和全球的AD及其他痴呆的疾病负担,包括死亡情况、患病情况、DALY(伤残调整寿命年),我国皆高于全球平均水平。
分别从性别、年龄、省市三个层面对比了2021年我国AD及其他痴呆的死亡情况、发病情况、患病情况、YLL(早亡所致生命年损失),研究报告显示,AD及其他痴呆导致的女性发病率、患病率明显高于男性,约为男性的1.8倍,死亡人数远大于男性;年龄层面,在≥40 岁人群中均呈现随着年龄增加不断上升的趋势,发病率在70~74 岁年龄组快速上升,患病率、死亡率在≥80岁年龄组中达到最高,具体数据详见原文。
三
AD的临床诊断
3.1 神经影像学检查
3.1.1 临床常用的影像检查方法
临床上主要采用磁共振扫描(magnetic resonance imaging,MRI)和电子计算机断层扫描(computed tomography,CT)检查。其中,MRI因其对于脑组织更为清晰的成像效果而作为首选,常用序列包括T1加权成像(T1-weighted imaging,T1WI)、T2WI、液体衰减反转恢复序列成像(水平位+海马冠状位)、扩散加权成像等。海马 MTA 被认为是 AD 的早期特异性标志。从认知正常人群中鉴别出AD的MTA临界值分别为,50~64 岁 ≥1.0(灵 敏 度 和 特 异 度 分 别 为 92.3% 和68.4%),65~74 岁≥1.5(灵敏度和特异度分别为90.4% 和 85.2%),75~84 岁≥2.0(灵敏度和特异度分别为 70.8% 和 82.3%),疑似AD患者,推荐加做斜冠状位T1W1序列,进行海马内侧颞叶萎缩(medial temporal lobe atrophy,MTA)评分。
需要注意的是,MTA评分在区分遗忘型轻度认知障碍(mild cognitive impairment,MCI)与认知正常人群中,显示出相对较低的诊断价值。另外,MTA鉴别早发型AD与额颞叶痴呆的准确率较低[AUC 0.53-0.35],1.5T MRI 与 3.0T MRI 在海马萎缩诊断中的效能无差异,但 3T MRI 拥有更好的信噪比和效应量。对于因体内金属异物、幽闭恐惧症等原因无法行颅脑 MRI检查者,则推荐用多层CT薄层扫描代替。
静息态及任务态功能MRI检查能够显示脑网络拓扑结构在不同痴呆类型中的差异性,故成为了潜在的AD早期筛查、诊断方法。但由于①不同MRI机器、扫描参数所得的图像异质性大;②尚无统一的数据预处理、标准化、分析流程;③机器学习模型在外部数据中泛化能力不佳,限制了功能MRI的临床应用。目前静息态及任务态功能MRI仅用于AD脑网络机制的临床研究,还无法真正用于临床诊断。
3.1.2 分子影响检查方法
2018年美国国立老化研究所(National Institute of Aging ,NIA)与阿尔茨海默病协会(Alzheimer's Association,AA)发布了AD研究框架,即A/T/N框架,在2023年国际阿尔茨海默病协会国际会议上发布的一项最新的AD诊断指南草案,即ATNVIS框架。
点击链接,了解详情:
【神经类】丨阿尔茨海默病诊断和分期标准修订:阿尔茨海默病协会工作组(2024正式发表版本)
A/T/N框架和修订版ATNVIS诊断标准,都明确了PET技术在AD临床前阶段到痴呆阶段全过程诊断中的重要作用。使用不同的分子探针进行PET显像,如Aβ-PET、Tau-PET就可以对Aβ和病理性tau的生物标志物进行特异性显像,FDG-PET低代谢可反映局部脑区的神经元损伤,因此PET显像可以全面反映患者ATN的改变,有助于AD的早期诊断和病程判断。
目前,一方面考虑到PET费用昂贵且尚未纳入医保,相应的分子探针仍然稀缺,另一方面鉴于我国正电子显像设备数量有限。。根据“2020 年全国核医学现状普查结果简报”,全国共有427台,其中PET/MRI 23台、PET/CT 404台,而其中配置于三级医疗机构的占 87.2%。在国内有限的PET配置条件下,具有Aβ/Tau-PET检查能力的医院更是为数不多,因此该项检查的临床应用在国内较为局限,能否广泛应用于临床亟需卫生经济学综合评估其成本及效益。
3.1.2.1 Aβ-PET
Aβ-PET可以实现AD关键的致病性病理蛋白Aβ活体分子显像,提供可定量及可视化的生物信息,而显得尤为重要。最早成功应用的Aβ分子探针是11C-匹兹堡化合物B,第2代Aβ分子探针主要包括18F-florbetapir(又称18F-AV-45,应用最为广泛)、18F-florbetaben(AV-1)、18F-flutemetamol(GE -067),这 3 种分子探针先后通过美国食品与药品监督管理局(Food and Drug Administration,FDA)和欧洲药品管理局的审批,特别是,2023年9月中国国家药品监督管理局批准了Sinotau 公司开发的18F-florbetaben(AV-1)作为新型 Aβ-PET 成像示踪剂。AV-1 是国内第一个获批用于诊断 AD 的 Aβ-PET 成像示踪剂。Aβ-PET阳性预测非痴呆受试者进展为AD的灵敏度可达95%(特异度<60%)因此它对于识别临床前AD患者的意义远非其他检查所能比拟。Aβ-PET阴性结果则将排除痴呆患者的AD病因。相关研究显示Aβ-PET分子探针可与血管壁中的Aβ沉积物结合,故不推荐Aβ-PET显像用于路易体痴呆和脑淀粉样血管病与AD的鉴别诊断。
3.1.2.2 Tau-PET
Tau-PET针对的是病理性错误折叠的Tau蛋白,其常用的示踪剂18F -Flortaucipir(AV⁃1451)于2020年获FDA批准上市。中国首个Tau蛋白示踪剂产品18F-APN-1607( 苏州新旭医药)于 2020 年 11 月获得国家药品监督管理局的批准进行Ⅲ期临床试验,结果有待公布。
Tau-PET显像对认知功能的变化有较好的预测作用,优于MRI皮质厚度变化和Aβ-PET。在AD的前驱期和临床前阶段,Tau-PET显像可能是预测个体认知功能变化的理想影像学标志物。AD患者Tau-PET显像显示Tau蛋白主要沉积在内侧颞叶、颞叶皮质或者广泛的大脑皮质。Tau-PET显像可反映AD患者的临床严重程度和分子病理学特征,对AD早期诊断、临床严重程度、认知功能变化评估及以异常Tau蛋白为靶点的AD治疗策略等具有重要意义。
3.1.2.3 FDG-PET
作为一种拥有 PET 仪器的医疗单位几乎都可以临床采用的检测手段,FDG-PET通过18F-FDG反映脑内葡萄糖代谢水平。脑葡萄糖代谢异常减少或低代谢是神经退行性痴呆的一个标志。脑FDG-PET的低代谢代表了神经元和星形胶质细胞的代谢降低,提示脑突触功能障碍。因此,基于FDG-PET低代谢的痴呆诊断已广泛用于诊断神经退行疾病。AD患者的FDG-PET特征改变多为后扣带回和颞顶叶代谢减退,并随病程进展逐渐累及额叶。
相关PET研究显示,在认知功能正常的健康人群中,脑内Aβ高水平者发展成为AD的概率要显著高于Aβ低水平者,若配合内嗅皮层FDG代谢水平降低的特征,则可以更好地发现处于AD临床前阶段的人群,为疾病的早期干预提供可能,但缺少特异性。国内一项针对认知障碍患者代谢特征的多中心临床研究提示,认知障碍患者的FDG-PET显像中特定的低代谢模式与其神经精神症状相关,FDG-PET显像可用于认知障碍患者神经精神症状的早期识别和管理,目前倾向于推荐AD的鉴别诊断(与额颞叶痴呆)及非典型AD(后皮层萎缩综合征、额叶变异性AD)的诊断以及BPSD症状的早期识别。
3.1.2.4 分子影像技术与其他技术的融合
国内基于A/T/N框架的多探针PET/MRI显像研究提示,与迟发性AD相比,早发性AD的tau负荷和神经元损伤更为严重,多探针PET/MRI可能有助于评估早发性AD的病理特征。随着人工智能的发展,其与分子影像学技术的结合也大大提高了分子影像学技术诊断的准确率、灵敏度和特异度。
分子影像学技术在AD中的应用除了经典的Aβ-PET、 Tau-PET、FDG-PET,神经炎症和突触密度分子探针的研发,以及各种神经受体、其他病理蛋白分子探针的研发应用都将为AD的机制研究、临床诊断及鉴别诊断、病情评估、疗效评价以及治疗药物的研发提供有价值的可视化生物信息。
3.2 神经心理测评
3.2.1 认知评估
国内记忆门诊采用的主流认知评估量表可分为以下几类。①总体认知评估量表:包括简易精神状态检查量表(mini-mental state examination,MMSE)、蒙特利尔认知评估(Montreal cognitive as-sessment,MoCA)、阿尔茨海默病认知功能评价量表(Alzheimer’s disease assessment scale-cognitive,ADAS-Cog)、Addenbrooke认知功能检查评分;②不同认知域的评估量表:评价记忆功能常用听觉词语学习测验、韦氏成人记忆量表第四版等;③程度分级量表:以临床痴呆评估量表最为常用。
MMSE具有所评价的认知域全面、操作简单的优势,在我国的各级医院均有应用。MMSE评估耗时5~10min,信效度高,筛查痴呆的灵敏度和特异度均在85%左右,是目前国内临床使用率最高的认知量表。然而,MMSE对于处于痴呆早期的患者的识别灵敏度较差,故对于怀疑处于痴呆早期的患者,测试者有必要使用MoCA量表或Addenbrooke认识功能检查量表进一步评估。Addenbrooke认识功能检查量表测评注意力、记忆力、语言流畅性、语言和时空间5个特定认知功能,其鉴别早期痴呆及痴呆阶段患者的准确率较高,还可鉴别额颞叶痴呆。
MoCA量表强化了对执行功能以及注意力的评估。一项关于北京地区MoCA量表的应用研究 显示,MoCA量表对于MCI的检测灵敏度达92.4%,显著优于MMSE(灵敏度 24.2%,考虑到MoCA量表对低教育人群适用性不佳,国内郭起浩等汉化了改良的 MoCA 基础版量表量表,目前也在临床被广泛使用此外,部分记忆门诊在候诊过程中采用更为简易的AD-8认知障碍自评问卷对患者进行快速筛查,一项纳入3728名研究对象的荟萃分析发现,8条目痴呆筛查问卷(ascertain dementia 8,AD-8)判别 MCI的灵敏度在72%以上,特异度在67%以上。
3.2.2 非认知评估
认知障碍患者因记忆遗忘,逐渐丧失日常生活所需技能。日常生活活动能力(activities of daily living,ADL)分为基础性ADL和工具性ADL两类。基础性ADL主要包括如厕、进食、穿衣、梳洗、行走、洗澡这6项生活必需功能,以提示患者是否需要额外照料人,目前国内常用的评定方法包括Bar-thel指数、改良Barthel指数(最常用)、Katz指(Katz index of independence in ADL)等。工具性ADL包括购物、娱乐、使用交通工具等高级生活活动技能,最常用的评价工具是社会活动功能量表。
认知障碍患者常伴随抑郁焦虑、幻觉、妄想等精神症状和行为障碍,早期识别有助于临床医生对其进行心理疏导,必要时须给予药物干预,提高患者的生活质量,减轻照护负担。常用的量表有老年抑郁量表、汉密尔顿焦虑量表、神经精神量表(neu-ropsychiatric inventory,NPI)等。此外,一些非认知评估的神经心理测试被用来辅助痴呆的鉴别诊断。
3.2.3 新型电子化诊断工具
计算机化认知测试可分为移植型、研究型和调试型。
①移植型是指将纸质测试内容移植到计算机中,不涉及内容和方法上的改变。②研究型则无纸质版参考,而是根据神经心理学研究中发现的对认知障碍有预测作用的认知内容重新设计而成。③调试型的特点是使用计算机工具来修改原有测试的数量、内容和逻辑等,从而提高测试的信效度和准确度。
与传统的纸质测试相比,计算机化的认知筛查具有多个优点。一是改变了测试的形式,减少了多种偏倚,二是计算机化的认知筛查工具的受众更为广泛,三是计算机可通过VR等技术,沉浸式地模拟日常生活情景,一方面比纸质测试更具趣味性,老人接受度高,另一方面由于更为真实,筛查结果也更准确,四是计算机化的认知筛查测试可以移植,便于携带管理和大范围推广,适用于不同的环境,五是计算机技术可引入时间变量,使筛查结果更具有准确性。
2023年《中国数字化记忆门诊临床应用指南》 指出,随着数字化技术的推广普及,在各级医院建设符合自身条件的数字化记忆门诊或将成为大势所趋 。国外市场上已有Cogstate 、Mindstreams等诸多商业化的电子化认知筛查工具。目前,国内也已经出现了 CatCog 、CoCoSc、老年认知障碍多维度评估系统和脑动激光等数字化评估工具,但还未真正广泛用于临床尚待进一步验证和实践。与之相对的是,计算机化也因为其技术特征,对于没有接触过计算机的老年人来说接受度较低,且筛查结果可能受到计算机因素,如软件、安装等的影响。更重要的是,计算机筛查的结果同样会出现漏诊或误诊的情况,误诊会增加老人的心理压力,并导致不必要的检查, 而漏诊则会使患病的老人错失治疗的机会,因此不能单纯依靠计算机筛查的结果作出诊断,最终诊断还是应基于临床结果。
3.3 体液标志物
理想AD体液标志物应具有较高的灵敏度和特异度(一般大于80%),能够反映AD病程发展中病理生理特点,同时又需兼顾良好的临床可实践性。它们大致有三个来源:CSF、血液和尿液。
3.3.1 CSF生物标志物检测
目前国内有条件的临床记忆门诊已经对拟诊AD的患者常规进行CSF的β淀粉样蛋白(Aβ)、总蛋白(T-tau)和磷酸化蛋白(P-tau)检测。但与国外记忆门诊不同的是,国内患者需要入院行脊髓穿刺获取CSF进行检测,而无法直接在门诊完成。目前CSF生物标志物还缺乏国内多中心大样本的常模及临界值,是否异常的判断还多借鉴于之前国内的相关报道。
3.3.1.1 Aβ相关标志物
CSF Aβ生物标志物主要包括Aβ42和Aβ40。使用免疫分析仪电化学发光检测区分。目前国内临床酶联免疫分析法检测多采用之前国外研究中CSFAβ42<550 pg/mL 的标准判断淀粉样病变,551~650 pg/mL则提示可疑病变。另在散发性AD中,CSF Aβ42 水平明显下降。特别是在早期在MCI患者中,CSF Aβ42对诊断AD的合并灵敏度为86%,合并特异度为81%,可以一定程度上预测早期AD的发生。Aβ40水平在AD患者CSF中往往不变或者轻度升高,其单独作为诊断标志物价值不大,但大量研究证实Aβ42/Aβ40比值降低对于鉴别AD与其他神经疾病有很好的灵敏度和特异度,弥补了Aβ42、Aβ40单独用于预测和诊断AD 的不足。
3.3.1.2 Tau相关标志物
CSF Tau生物标志物主要包括T-tau和P-tau(P-tau181、P-tau231和P-tau217)。CSF和血浆P-tau在疾病早期就已升高,因此在检测AD的早期病理变化方面,似乎优于tau-PET。在AD患者中,CSF T-tau的含量显著增加约300%。其合并灵敏度为0.77,特异度为0.86;然而T-tau是从整体反映大脑皮质轴索的损害,在路易体痴呆、卒中、脑创伤和CJD中也可见升高,故其在鉴别AD与其他神经系统疾病间的特异度不高。相较于T-tau,CSF P-tau升高更能反映AD病理变化-脑内神经纤维缠结形成,表现出更好的灵敏度和特异度。目前已经发现有30多个Tau蛋白磷酸化表位,其中P-tau217能较好反映AD病程的变化过程,其水平升高反映病情由MCI向AD进展,并伴有认知能力迅速下降。P-tau217 在 Aβ 斑块形成时开始增加,P⁃tau205在神经元开始出现功能障碍时增加。此在AD临床前阶段,P-tau217和P-tau231可以区分Aβ阳性和Aβ阴性个体。P-tau217在区分AD与其他神经退行性疾病方面的表现略好于CSF P-tau181,且其与基线及纵向Tau-PET间的相关性更强。这些发现表明,P-tau217可能最适用于AD的诊断。
在诊断AD时,联合应用并综合考虑CSF标志物水平能够获得更高的准确率和特异度。Aβ42/Aβ40比值和P-tau/Aβ42比值在预测AD神经病理学改变时,具有非常高的准确率(AUC为0.95~0.96)。Aβ42/Aβ40比值和P-tau/Aβ42比值分别优于单独的Aβ42检测,P-tau/Aβ42比值优于单独的P-tau检测。
3.3.1.3 CSF生物标志物的预测价值
贾建平教授等近期报道了迄今为止世界上规模最大、随访时间最长的反映AD诊断前生物标志物变化的纵向队列研究结果,首次揭示了AD患者无症状期到有症状期的CSF和影像学生物标志物的动态变化规律,详尽地阐明了AD发病出现生理病理变化过程中最早的关键节点。该研究结果显示,AD组与认知正常组间生物标志物出现差异的先后顺序和时间点分别为:Aβ(诊断前18年)、Aβ42/40(诊断前14年)、p-tau181(诊断前11年)、t-tau(诊断前10年)、NfL(诊断前9年)、海马萎缩(诊断前8年)、认知减退(诊断前6年)。该研究还发现,随着认知功能衰退,AD患者CSF中Aβ42和Aβ42/40比值的变化率最初明显加快,大约在MMSE分数为25和逻辑记忆分数为11时达到峰值。随后,尽管认知得分进一步下降,变化的速度逐渐放缓,揭示了认知水平和外周标志物之间的变化规律。
3.3.2 血液学生物标志物检测
尽管PET检查、CSF生物标志物检测对疾病预测性较高,但其成本高、样本少、侵入性的特点限制了临床运用,而血浆生物标志物检测避开了这一缺点。目前国内临床尚无血液学标志物诊断AD的统一临界值。淀粉样前体蛋白(amyloid precursor protein, APP)、Tau、Nfl、GFAP 等 AD血液标志物在临床研究中展现出不错的应用前景,但同时要注意对这些指标异常值的定义。2023年,阿尔茨海默病协会国际会议上发布的一项最新的AD诊断指南草案纳入了血液生物标志物,血液生物标志 物近年来在 AD 诊断中显示出高准确率,该草案列出了体液和影像学生物标志物的预期用途。
表8 体液和影像生物标志物的预期用途
3.3.2.1 一般指标
认知障碍可能是由代谢、感染、中毒等因素导致,对于首次就诊的认知障碍患者需常规进行血液学检测,包括血常规、生化指标、甲状腺功能、叶酸、维生素B12、梅毒抗体等指标,以明确病因、危险因素和有无伴随疾病。
3.3.2.2 Aβ相关标志物
血浆总Aβ或Aβ42水平在家族性AD患者中增高,在散发性AD患者中早期增高,随着明显认知障碍出现,Aβ42水平及Aβ42/Aβ40比值均下降。相较于Aβ42或Aβ40的单独检测,血浆Aβ42/Aβ40比值与CSF Aβ42/Aβ40比值及Aβ-PET相关,在预测正常人向MCI或者向AD转化时更有价值。血浆 Aβ42/Aβ40比值在 AD 症状前阶段已经出现改变,因此可以准确识别认知未受损(CU)的 Aβ 病理学。然而,血浆 Aβ42/Aβ40 比值在 Aβ 阳性和 β阴性个体之间的倍数变化小(与CSF中的40%~ 60% 相比,减少为 8%~15%),因此可能没有 CSF Aβ42/Aβ40比值稳健。
3.3.2.3 Tau相关标志物
血液和CSF中T-tau水平间的相关性也较差,表明血液中大部分T-tau为外周来源,而中枢来源部分占比较小(约20%),导致无法检测正在发生的神经退行性变。然而,高基线水平的T-tau预示着更快的认知能力下降。血液中P-tau水平会随着Aβ的积累和AD病情严重程度的增加而增加,而在非AD引起的认知障碍个体中无该情况。血液中P-tau水平与Aβ、tau、神经退行性变程度、CSF生物标志物水平以及PET测量值相关,并能预测其变化;血浆P-tau231和P-tau217是提示早期Aβ变化的生物标志物。在早期已有Aβ沉积的个体中,P-tau231和P-tau217与Aβ-PET摄取密切相关;在基线尚无Aβ病理沉积的个体中,P-tau231及 P-tau217与Aβ-PET 摄取的纵向增加相关。血浆P-tau231及P-tau217的改变,发生在病理性Aβ斑块出现之前,能更早地反映早期大脑的Aβ变化,尤其是P-tau231,可能是最早异常的AD血液标志物。随着临床痴呆评估量表评分从0到3,P-tau181水平持续上升,但分别在CSF和PET发现Aβ异常后6.5年和5.7年才达到异常水平。此外,在MCI患者中,血浆P-tau181和P-tau217已被证明可以准确预测患者未来2~6年的认知能力下降和转化为AD痴呆的风险。然而,虽然血浆 P-tau是AD早期诊断的潜在生物标志物,但其在多种合并症(如慢性肾脏病、高血压等)患者中都会升高,易导致假阳性。
3.3.2.4 NFL
Nfl是神经轴突损伤的标志,可以在CSF、血浆(血清)中同时检测,是目前最有前景的神经退行性病变(N)标志物。在认知正常群体中,血浆NfL水平随着年龄的增长而显著增加,并且在65岁以后更加明显。尽管血浆NfL作为AD诊断生物标志物相对于P-tau181或P-tau231表现较弱,但高于临界值的NfL水平预示着更快的认知衰退,因此,NfL可能作为认知衰退的预测因子。值得注意的是,在60岁以上的人群中,年龄对血清NfL水平的影响会越来越大,对肾功能和血容量等其他因素也有一定程度的影响。
3.3.2.5 GFAP
GFAP是反应性星形胶质细胞增生症的标志。与AD的其他血液生物标志物不同,血清GFAP在确定脑Aβ病理加重方面远远优于CSF的GFAP。可能在于周期性冻融对 CSF 中的 GFAP 水平有显著影响,但对血清 GFAP 水平无明显影响。血浆GFAP在AD临床前阶段就开始升高,与临床AD发病率相关;而P-tau181及NfL水平与中度AD风险相关(9年以内),表明GFAP可能是一种早期AD生物标志物,早于P-tau181和NfL,这一观点也被近期研究证实。最后,血清GFAP还能鉴别AD与额颞叶痴呆,并预测CU的认知下降,以及MCI向痴呆状态的转换。
3.3.3 尿液无创性生物标志物检测
尿液也可以反映AD的病理特征,其中的代谢物、蛋白质和核酸等可能作为AD的生物标志物。尿液中AD7C神经丝蛋白作为AD标志物,其灵敏度和特异度都很高。其他潜在的尿液生物标志物还包括尿外泌体中Aβ42和P-S396-tau,尿液单核细胞趋化蛋白1,尿精氨酸代谢失调等,但其诊断价值仍需进一步临床实验证据支持。
3.3.4 其他体液生物标志物检测
AD体液标志物检测呈现高灵敏度、高特异度、早期预测的趋势特点,目前仍有许多有潜力的体液标志物在临床研究中。研究验证了外周血神经源性外泌体中的 Aβ42、T⁃tau 和 P⁃tau181可以区分AD患者与健康个体,并且外泌体突触蛋白可以作为在认知障碍出现前 5~7年预测 AD和 MCI 的生物标志物。
通过蛋白组学分析发现了神经源性外泌体的6种蛋白组合能够高精度地区分AD 患者和健康对照人群(AUC=0.978)。还有研究通过新开发的AD聚体活性检测器实现了对AD患者血浆中 Aβ 聚体活性和 Tau 聚体活性的无抗体检测,并证实Aβ聚体活性能够识别AD患者将其与CU 或非AD 痴呆区分开来(AUC=0.85~ 0.86。)
沈璐团队发现AD的发生、发展伴随着特异性的自身抗原抗体反应,并首次鉴定出具有诊断价值的7种 AD 特异性血清自身抗体,分别为MAPT、DNAJC8、KDM4D、SERF1A、CDKN1A、AGER 和 ASXL1。
3.4 基因检测
目前国内临床并不推荐非所有 AD 患者都进行基因检测。AD作为最常见的痴呆类型,家族性AD数量较少,仅占5%左右,而其中常染色体显性遗传的早发AD又仅占所有病例的1%,目前研究较多并确认的AD致病基因有早老素1(presenilin 1,PSEN1)基因、早老素2(presenilin 2,PSEN2)基因、APP基因,其中PSEN1基因突变最为常见,占75%~80%,而PSEN2基因突变则相对罕见,PSEN1突变的AD患者平均发病年龄比 APP 突变患者发病年龄更早,行为异常、语言功能受损、计算障碍等更易发生。PSEN2突变的AD患者发病年龄更大,易出现幻觉,2022年新报道了42个与AD及相关痴呆有关的基因位点,目前已有超过70 个基因位点被认为与AD及相关认知障碍相关。
编码载脂蛋白E(apolipoprotein E,AopE)的等位基因之一ApoE ε4是目前证据最强,同时也是研究最为广泛的AD易感基因,也是MCI向AD转化的危险因素。ApoE ε4杂合子携带者AD的患病风险增加2~4倍,ApoE ε4纯合子携带者患病风险更高,可以增加8~16倍。而对于有AD家族史的老年人来说,若携带ApoEε4则患病风险会更高。
目前国内临床开展应用较多的有ApoE基因分型,ε4纯合子及杂合子占20%~30%,但该阳性结果并不代表AD,仅能提示发病风险较高。而据临床表型对候选基因进行筛查有助于提高检出率。PSEN2突变可能更多导致迟发型AD,因此无论患者的发病年龄早晚,对于有痴呆家族史的AD患者都推荐行基因检测,尤其是家族史结合发病年龄和临床表型是预测有害变异的重要预测因子。鉴于临床表型和基因型的多样性,常染色体显性遗传AD家系推荐使用基因Panel或WES/WGS检测。
3.5 进行中的临床诊断试验
(详见《中国阿尔茨海默病报告2024》)
四
AD的防治及相关临床试验
4.1 AD的社区预防
由于目前AD的发病机制尚不明确,缺乏治愈AD的治疗手段,因此疾病一旦进展为AD将不可逆转。在疾病转归过程中,MCI阶段被认为具有高度异质性。研究表明,MCI患者可以逆转为认知正常状态,因此在MCI阶段开展早期识别与干预是防治AD的有效策略。在疾病进展至需要临床介入之前,社区可充分发挥其作用,基于简单社区筛查-早期影响因素识别-非药物干预-照护者赋能的全流程模式,实现AD的早期预防。居民可以自行实施或由社区组织个体简单的认知功能筛查,早期识别可能的影响因素。若发现问题,将对患者提供简单的非药物干预或科普居家干预方式,同时通过照护者赋能提高AD老年患者的居家生活质量。
4.1.1 基于社区的简单认知筛查
普及可供老年人及其家庭自行筛查或由社区提供初步简单筛查方式,有助于提高AD早期症状的发现率,更早地发现认知障碍症状。目前使用较多的可应用于社区的简单自我筛查问卷包括AD-8及简易认知量表(Mini-Cog)等。WHO也提出,先通过简单的记忆和定位测试筛查是否有认知减退,若发现认知衰退再进一步使用MMSE等量表评估认知能力。
4.1.2 基于社区的早期影响因素识别
MCI状态有3种临床转归结局:①部分进展为AD与其他类型痴呆;②不进展,不好转,病情保持稳定;③逆转为认知正常状态。若在MCI状态对相关因素及早实施措施,可实现认知功能的逆转。老年人发生MCI的影响因素众多,复杂且分布维度多样,总体可分为社会人口学、生活方式、疾病和心理维度,根据影响因素是否可改变可分为如吸烟、饮酒、饮食、运动、高血压、糖尿病、高脂血症、社交、文化程度、社会经济水平、独居、抑郁、睡眠、社区环境因素、认知活动等的可控因素,以及年龄、性别和基因测定等不可控的因素。识别可能的影响因素,有助于社区定位重点风险人群,有针对性地开展筛查与非药物干预等预防手段,在疾病早期或未发病时预防认知功能的下降。
4.1.3 基于社区的非药物干预方式
在识别了可改变的危险因素后,针对性地开展非药物干预是预防认知功能恶化的有效措施。在社区可开展的非药物干预方式包括单一干预或联合干预。单一干预中主要的干预方式为认知干预,分为认知训练、认知刺激和认知康复。运动干预主要包含有氧运动、抗阻运动和心身运动等,涵盖有氧运动、抗阻训练、平衡训练的综合运动干预方式。有条件的社区可在综合为老服务中心等老年 人活动场地设置计算机或 VR 训练设备,通过互联网技术手段开展非药物干预。除单一干预外,社区内可综合多种干预方式,形成联合干预,为MCI老人提供多样干预形式和丰富干预环境,对其整体认知功能及多个认知领域有良好的改善效果。
此外,继美国和欧盟等之后,中国脑计划于2021年正式启动,该计划拟通过建设“脑健康大数据平台(Brain Health Platform)”这一涵盖基因组学、影像学、症状学等多模态数据的平台,为我国的多种脑疾病的预防干预 提供支撑。基于该计划平台的开展,社区内的干预模式也将进一步更新。
4.1.4 基于社区的照护者赋能
目前我国AD患者的照护形式主要为居家照护 ,相较于社区及机构照护,居家照护多由配偶或子女实施,缺少照护的专业性,且持续不间断的照护多造成照护者压力、抑郁、焦虑等不良情绪。社区可充分发挥其紧密联系居民的特点,通过开展照护者赋能,在减轻照护者负担的同时提高其照护能力,有助于提高 AD 患者及其家庭的生活质量。可以从培训照护者及适老化改善居家照护环境入手,提高居家照护的效果,同时对家庭照护者提供心理和生理支持,减少其躯体及心理压力。
4.2 AD的治疗
目前已上市的AD治疗药物主要有多奈哌齐、加兰他敏、卡巴拉汀、美金刚以及甘露酸钠胶囊(GV-971)等,均以改善AD临床症状为主。近年来,以AD疾病修饰疗法(disease modifying treatment,MDT)为靶向的新药,尤其是针对Aβ和Tau蛋白的单克隆抗体等,成为了抗AD治疗的研究热点。此外,神经调控治疗、中医药治疗等也进展迅速。
4.2.1 Aβ单抗治疗
Aβ单抗药物是AD疾病修饰疗法的代表之一,其通过干预Aβ的产生、聚集和清除,延缓早期AD的发生、发展。近期,Aβ单抗治疗AD的临床试验取得了重要进展。
4.2.1.1 Aducanumab
由渤健研发的 Aducanumab(商品名 Aduhelm)是首个以 AD 疾病修饰疗法为靶向的治疗药物,主要适用于轻度痴呆阶段的 AD 患者。Ⅲ期临床试验 EMERGE研究显示,Aducanumab治疗78周后,主要临床终点临床痴呆评估量表⁃SB 评分下降延缓 22%,次要临床终点MMSE、ADAS-Cog13以及ADCS -ADL⁃MCI评分分别下降延缓18%、27%和40%,与对照组相比有显著差异,而在Ⅲ期ENGAGE研究中未达到主要及次要临床终点。
4.2.1.2 Lecanemab
2023 年 7 月 6 日,Lecanemab(商品名 Leqembi) 正式获 FDA 批准用于治疗 AD,成为全球第二款获 FDA批准上市的Aβ单抗药物,2024年1月中国国家药品监督管理局正式批准 Lecanemab(商品名乐 意保)在中国上市,治疗 18 个月后,治疗组主要结局指标临床痴呆评分总和下降幅度减少 27%,受试者脑内Aβ蛋白沉积及认知评分下降均改善,但Lecanemab 导致 26.4% 的受试者出现输液相关反应,12.6% 出现水肿或渗出等淀粉样蛋白相关的影像学异常。
4.2.1.3 Donanemab
2024 年 6 月 FDA 专家委员会通过了对 Don-anemab的上市前申请。目 前 ,Donanemab 已在国内完成Ⅰ期临床试验招募,Ⅲ期在国内的多中心临床试验正在招募中。
4.2.1.4 SHR-1707
SHR-1707是首款由国内恒瑞医药主导开发的用于治疗早期 AD 的人源化抗 Aβ 单克隆抗体,目前已在国内及澳大利亚健康人群中完成Ⅰ期临床试验。
4.2.2 神经调控治疗
基于AD病理生理学机制和神经调控技术的脑网络调节模式,开发安全有效的神经调控技术为治疗AD提供了新的思路。随着近年来无创神经调控技术的发展,神经调控技术不仅应用于改善AD患者认知功能,其对AD患者精神症状、睡眠障碍的作用也受到广泛关注。
神经调控治疗主要包括重复经颅磁刺激(repetitive transcranial magnetic stimulation,rTMS)、经颅交流电刺激(transcranial alternating current stimulation,tACS)、近红外光治疗、深部脑刺激、神经调控的联合治疗等方式。
目前对于临床阶段应用神经调控技术治疗AD仍有诸多问题需要解决。临床疗效与 刺激频率、刺激部位和刺激时间等参数密切相关。在临床研究中还需注意与刺激相关的不良反应以及相应的评估和记录,如头晕、头痛和皮肤感觉不适等。
(详见《中国阿尔茨海默病报告2024》)
4.2.3 干细胞及外泌体治疗
王刚等人报告国际首个采用人脂肪来源间充质干细胞外泌体(allogenic human adipose mesen- chymal stromal cells - derived exosomes,ahaMSCs -Exos)经鼻给药治疗 AD 的临床试验。与基线水平相比,中剂量组(4× 108 微粒)在第12 周时 ADAS -cog 评分下降 2.33 (1.19)分,MoCA 基础版评分增加 2.38(0.58)分,3组受试者Aβ或tau沉积改变差异尚无统计学意义。中剂量组显示海马萎缩程度可能存在偏少趋势,有待进一步临床试验探索验证。该试验无不良事件报告。
4.2.4 中医药疗法
肖天祎等人用美金刚作为基础用药,观察花青素治疗AD的有效性,结果显示,花青素联合美金刚治疗组与安慰剂联合美金刚相比,治疗前后 MMSE、MoCA 及 ADAS-cog 评分差异有统计学意义。针灸联合多奈哌齐(5 mg/d)干预12周后,与对 照组相比,治疗组 AD 患者 ADAS-cog 得分降低,干预后右侧楔前叶的 fALFF变化值最大。基于右侧楔前叶的功能连接分析表明治疗组改变的功能连接主要位于双侧颞中回。此外,国内目前正在进行的中医药治疗 AD 的临床试验还有益智清心方、黄芪、养血清脑片、虎杖益智颗粒等中药,以及针灸、穴位电刺激联合音乐治疗、针刺联合认知训练等疗法。
4.2.5 其他
包括补充维生素D3、音乐运动疗法、 园艺疗法、降糖药司美格鲁肽、抗癫痫药拉考沙胺和左乙拉西坦改善AD患者认知的临床试验也在进行中。
五
AD防止管理的公共卫生资源
(详见《中国阿尔茨海默病报告2024》)
文章信息源于公众号Proteinnews,登载该文章目的为更广泛的传递行业信息,不代表赞同其观点或对其真实性负责。文章版权归原作者及原出处所有,文章内容仅供参考。本网拥有对此声明的最终解释权,若无意侵犯版权,请联系小编删除。
学如逆水行舟,不进则退;
心似平原走马,易放难收。
行舟Drug
每日更新 欢迎订阅+
医药大数据|行业动态|政策解读
100 项与 新旭生技股份有限公司 相关的药物交易
登录后查看更多信息
100 项与 新旭生技股份有限公司 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2025年07月21日管线快照
管线布局中药物为当前组织机构及其子机构作为药物机构进行统计,早期临床1期并入临床1期,临床1/2期并入临床2期,临床2/3期并入临床3期
临床前
4
1
临床1期
临床2期
1
1
临床3期
登录后查看更多信息
当前项目
| 药物(靶点) | 适应症 | 全球最高研发状态 |
|---|---|---|
[18F]Florzolotau ( TAU ) | Tau蛋白病 更多 | 临床3期 |
APN-1701 ( TAU ) | 神经变性 更多 | 临床2期 |
APNmAb-005 ( TAU ) | 阿尔茨海默症 更多 | 临床1期 |
APN-1808 ( TAU ) | 额颞痴呆 更多 | 临床前 |
Tau Degrader (Aprinoia Therapeutics) ( TAU ) | 额颞痴呆 更多 | 临床前 |
登录后查看更多信息
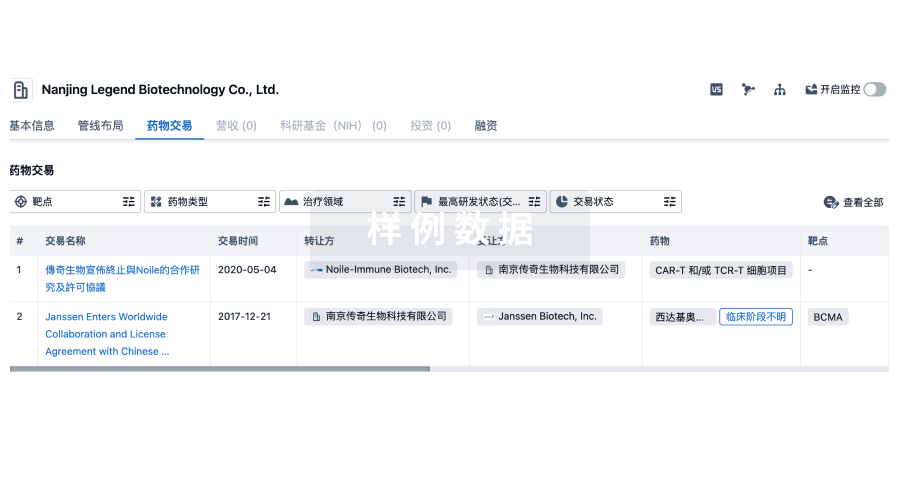
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
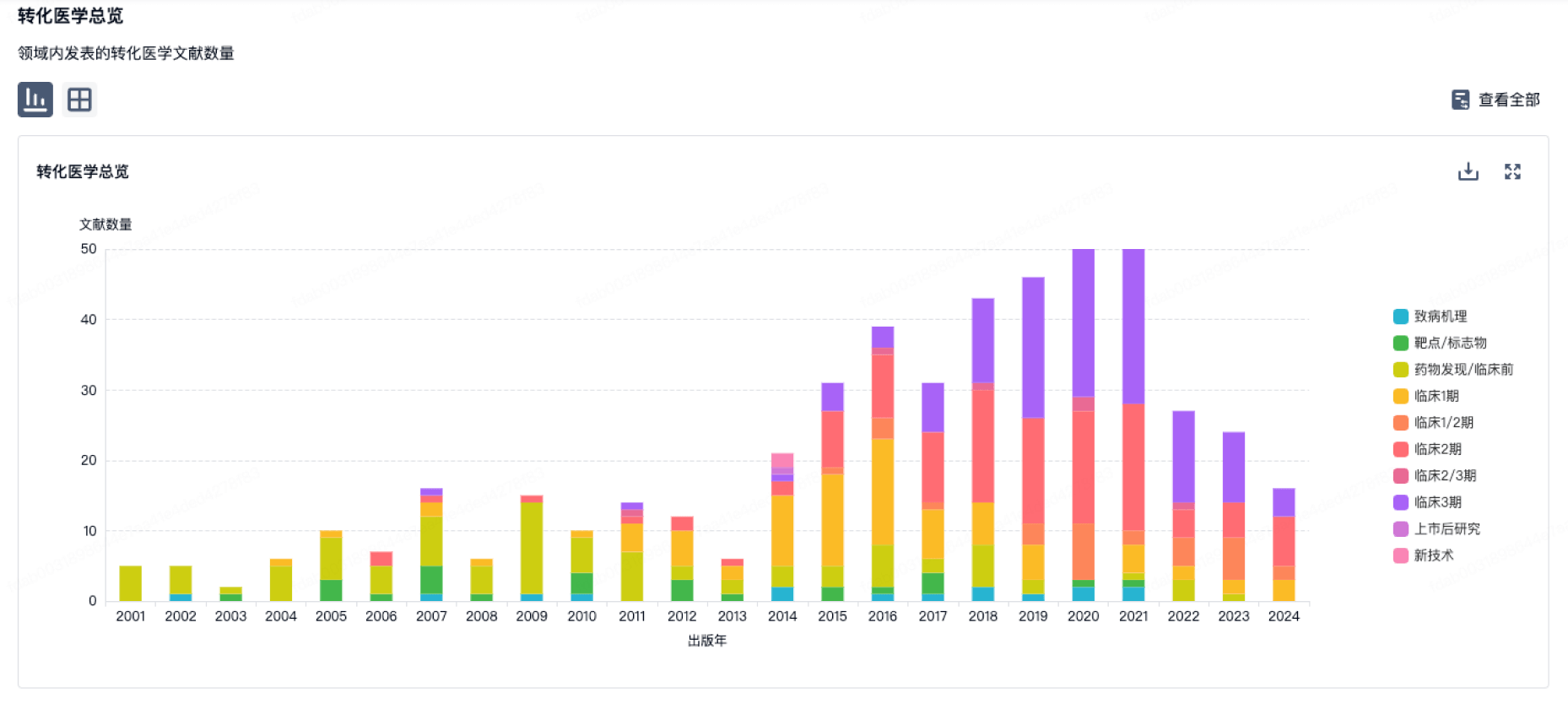
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
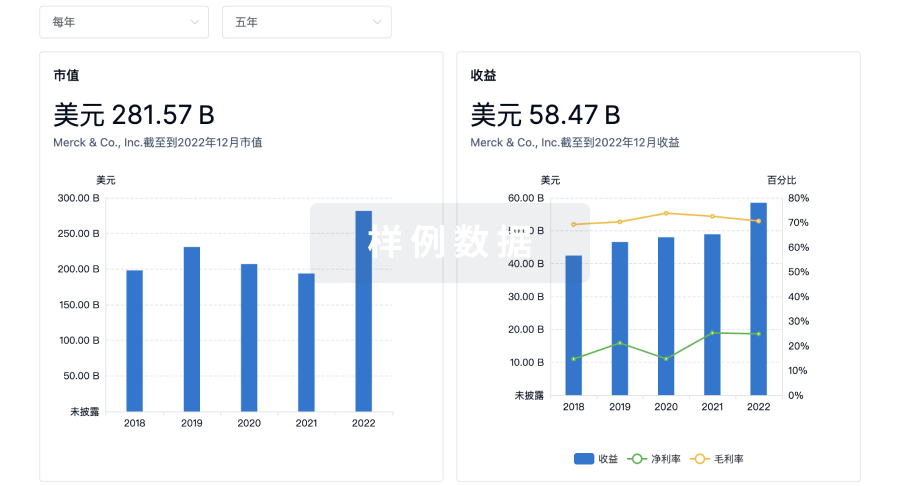
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
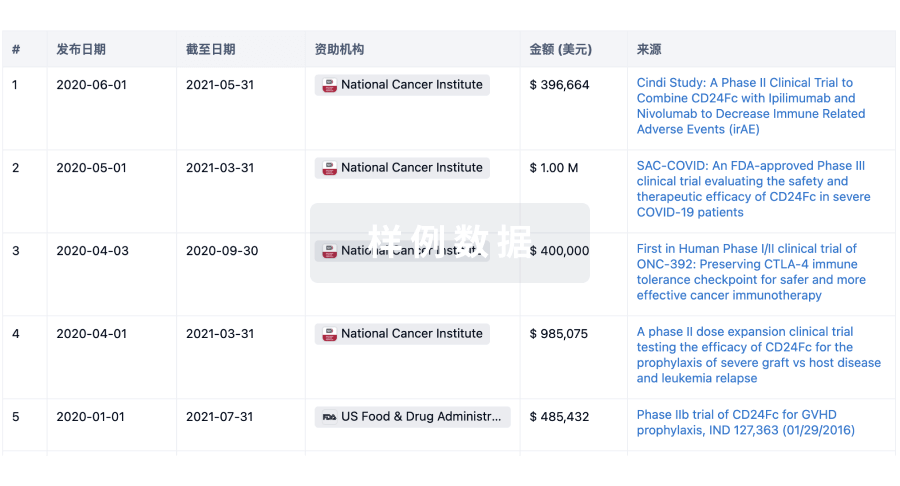
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
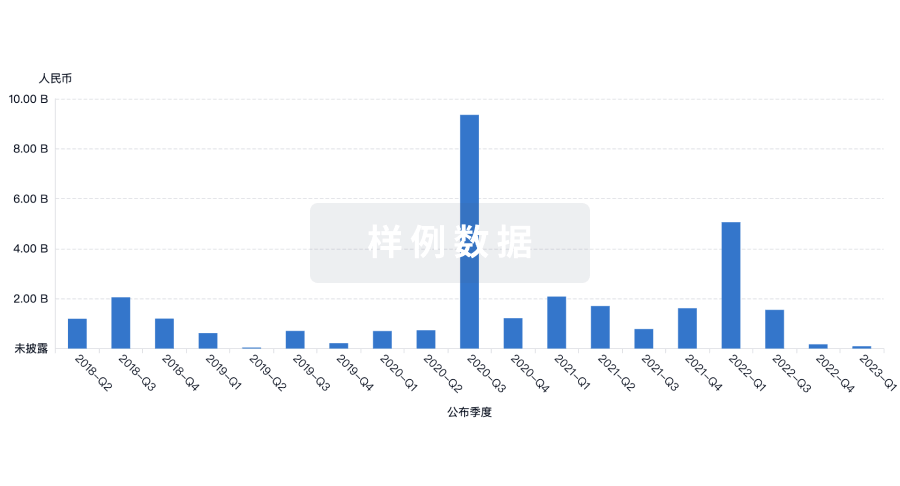
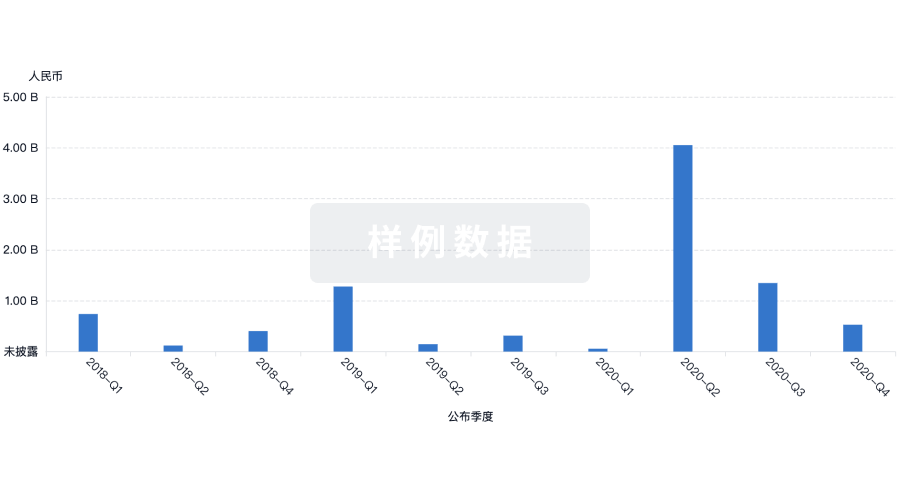
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
Eureka LS:
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
