预约演示
更新于:2025-05-07
Instituto Nacional de Cancerología
更新于:2025-05-07
概览
关联
60
项与 Instituto Nacional de Cancerología 相关的临床试验RBR-469x3sh
Awareness of oncology residents and clinical oncologists regarding the application of the Go Wish Cards Game for cancer patients: a multicenter pre and post-intervention study
开始日期2025-04-07 |
申办/合作机构 |
NCT06881940
Rationale and Design of a Cardiac Rehabilitation Program on the Prevention of Cardiotoxicity in Breast Cancer Patients Undergoing Treatment with Anthracyclines And/or Trastuzumab: a Randomized, Active Control Group, Open-Label Trial
This study aims to evaluate the effectiveness of a cardiac rehabilitation protocol, incorporating aerobic and resistance exercise, in reducing the incidence of cardiotoxicity in breast cancer patients receiving treatment with anthracyclines and/or trastuzumab through a randomized, active control group, open-label clinical trial.
开始日期2025-04-01 |
申办/合作机构 |
RBR-8h6tk9z
Evaluation of the effects of Auriculotherapy to control pain in lesions or tumor wounds in patients with advanced cancer undergoing palliative care
开始日期2024-10-03 |
申办/合作机构 |
100 项与 Instituto Nacional de Cancerología 相关的临床结果
登录后查看更多信息
0 项与 Instituto Nacional de Cancerología 相关的专利(医药)
登录后查看更多信息
3,707
项与 Instituto Nacional de Cancerología 相关的文献(医药)2025-07-01·Archives of Medical Research
Narrowing the Gap: Understanding Lung Cancer Care Intervals and Their Barriers in Latin American Low and Middle-Income Countries
Article
作者: Williams, Haydee ; Muñoz-Montaño, Wendy R ; Reynoso-Noverón, Nancy ; Arrieta, Oscar ; Rios-Garcia, Eduardo ; Corona-Cruz, Jose ; Cores, Vanessa ; Flores-Estrada, Diana ; Gómez-García, Ana Pamela ; Palomares-Palomares, Cittim B ; Cardona, Andrés F ; Turcott, Jenny G ; Hernandez-Martinez, Juan-Manuel
2025-07-01·Archives of Medical Research
Founder Variants in the Mexican Population: A Systematic Review
Article
作者: Metta-Harari, Teresa ; Taja-Chayeb, Lucia ; González-Barrios, Rodrigo ; Wegman-Ostrosky, Talia ; Harari-Arakindji, Sylvia ; Zatarain-Barrón, Zyanya Lucia ; Espino-Gutiérrez, Isabel ; García-Ortiz, José Elias
2025-06-01·Epilepsy & Behavior
Association between metabolic patterns in 18-FDG PET-CT scan and postsurgical seizure outcomes in patients with temporal lobe epilepsy
Article
作者: Díaz-Meneses, Iván ; Robles-Lomelín, Pilar ; Martínez-Juárez, Iris E ; Moreno-Jiménez, Sergio ; Kerik-Rotenberg, Nora ; Sebastián-Díaz, Mario A ; Camiro-Zúñiga, Antonio ; Vázquez-Cruz, Betsy C ; Fuentes-Calvo, Irving ; Gonzalez-Salido, Jimena ; Solís-Vivanco, Rodolfo ; Martínez-Medina, Salvador ; Rosales-García, Juan Salvador ; Vasquez-Lopez, Fernando ; Colado-Martinez, Jimena ; Gutiérrez-Aceves, Guillermo Axayacalt ; Arellano-Reynoso, Alfonso
100 项与 Instituto Nacional de Cancerología 相关的药物交易
登录后查看更多信息
100 项与 Instituto Nacional de Cancerología 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2025年11月03日管线快照
无数据报导
登录后保持更新
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
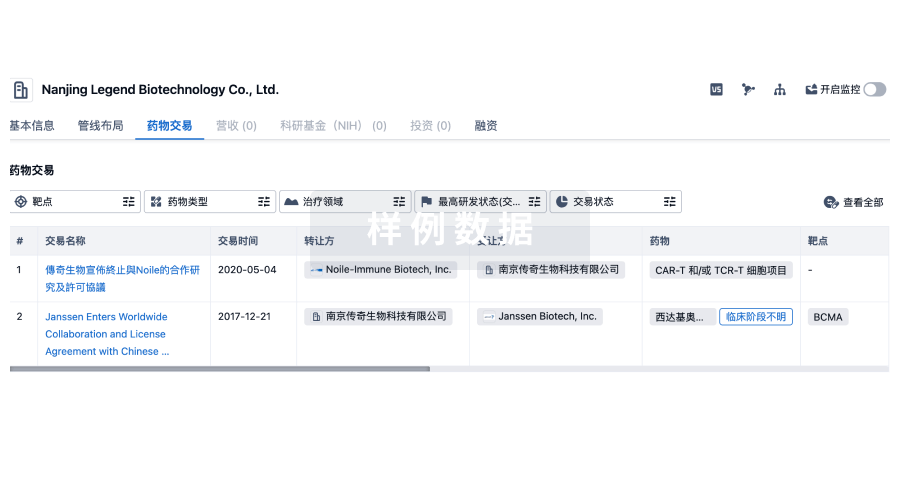
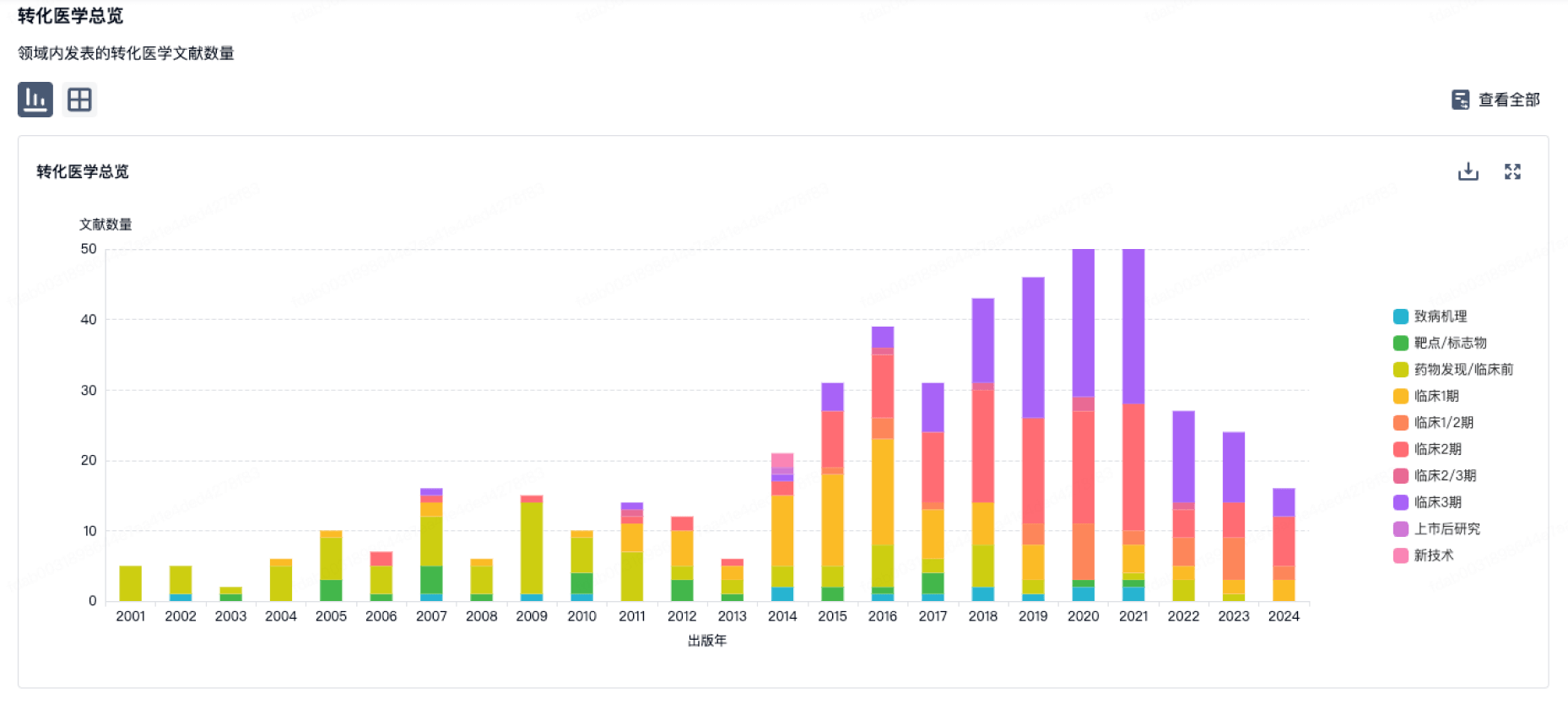
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
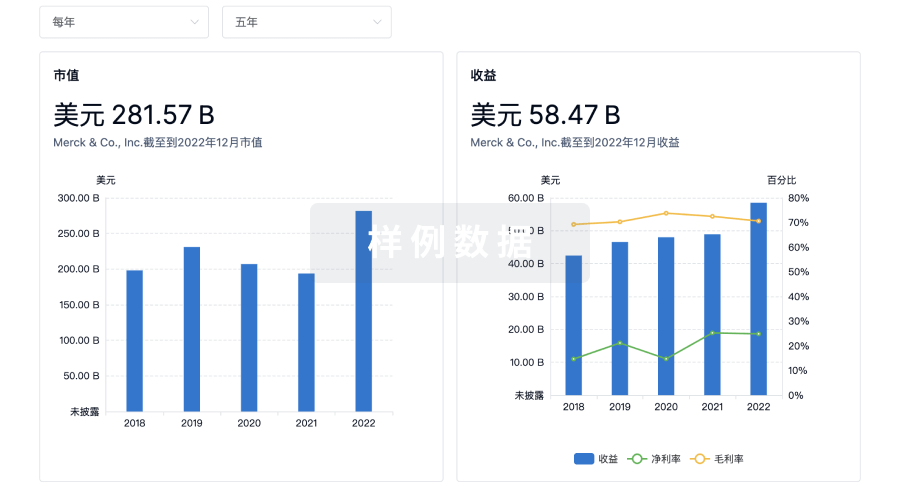
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
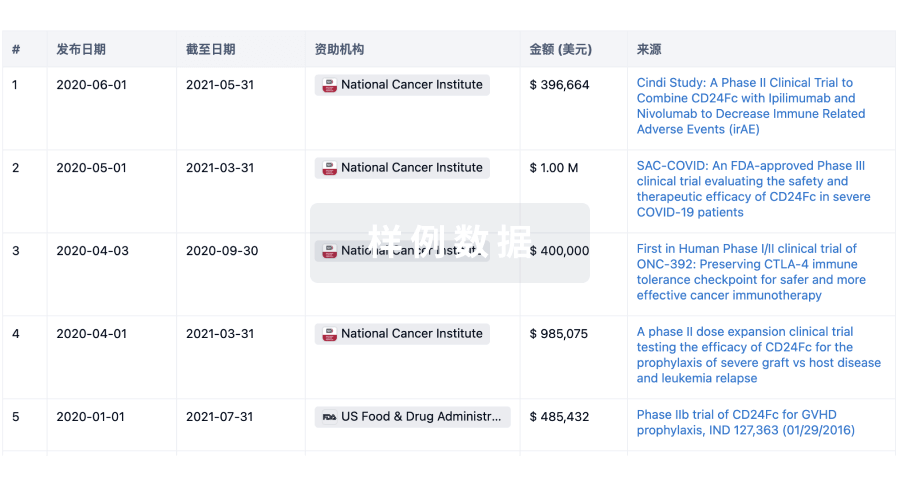
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
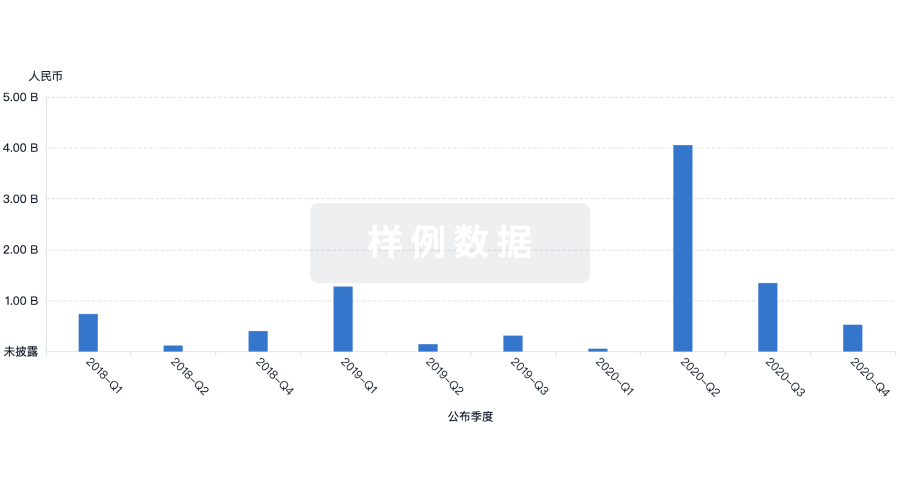
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
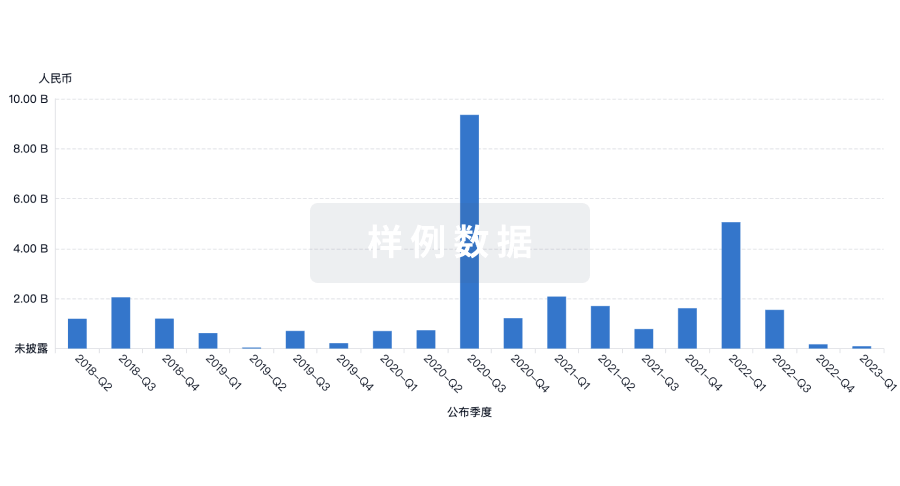
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
