预约演示
更新于:2025-08-14

Azienda Ospedaliero-Universitaria Meyer
更新于:2025-08-14
概览
关联
8
项与 Azienda Ospedaliero-Universitaria Meyer 相关的临床试验NCT06181175
Valutazione Dell'Efficacia Del Trattamento Dell'Ipertrofia Prostatica Benigna Con Serenoa Repens Estratta Con CO2 + PEA (Palmitoilethanolamide) in Monoterapia o in Combinazione Alla Tamsulosina: ProSeRePEA Trial
The objective of this study is to evaluate the efficacy of the supplement PEAPROSTIL 600 (FARMITALIA®) composed of Serenoa Repens combined with PEA in single or combined therapy with alpha-blocker in the reduction of voiding symptoms in benign prostatic hyperplasia (BPH) patients at low risk of progression to obstructing conditioning that need for surgical therapy. Any adverse events, intolerance, allergic reactions, complications related to the products used will be recorded throughout the study period.
开始日期2021-10-01 |
EUCTR2020-005131-74-IT
Phase II, single-arm, open-label interventional clinical trial to evaluate the role of anthracycline infusion after radiotherapy (RT) in pediatric and young adult patients with glioblastoma (pGBM) - Clinical Trial on glioblastoma with doxorubicin chemotherapy after radiotherapy
开始日期2021-02-25 |
NCT06341777
Telerehabilitation for Visual Field Defects: Clinical Efficacy of a Novel Multisensory Therapy for Adults and Children With Acquired Brain Lesions
Brain injuries may cause the loss of the ability to see portions of the visual field, the so-called visual field defects (VFDs). VFDs significantly impact the survivors' functional recovery and quality of life, with the majority of patients displaying no spontaneous recovery or being left with residual deficits. Among the available therapies for VFDs, the compensatory scanning training is considered the most promising. Yet, current evidence is insufficient to recommend it in clinical practice, and the scientific community has stressed the need of more high-quality research. The present randomized clinical trial in patients with chronic VFDs caused by brain lesions aims at verifying the feasibility and efficacy of a novel telerehabilitation using a multisensory scanning therapy, by measuring its effects on visual functions and daily activities, and by looking for neural indicators of the therapy-induced improvements.
开始日期2020-01-01 |
申办/合作机构 |
100 项与 Azienda Ospedaliero-Universitaria Meyer 相关的临床结果
登录后查看更多信息
0 项与 Azienda Ospedaliero-Universitaria Meyer 相关的专利(医药)
登录后查看更多信息
111
项与 Azienda Ospedaliero-Universitaria Meyer 相关的文献(医药)2025-03-15·Mutagenesis
A pleiotropy scan to discover new susceptibility loci for pancreatic ductal adenocarcinoma
Article
作者: Brenner, Hermann ; Adamonis, Kestutis ; Bunduc, Stefania ; Rizzato, Cosmeri ; Neoptolemos, John P ; Hlavac, Viktor ; Farinella, Riccardo ; Carrara, Silvia ; Theodoropoulos, George E ; Sperti, Cosimo ; Rende, Mariaconcetta ; Stocker, Hannah ; Hackert, Thilo ; Bambi, Franco ; Corradi, Chiara ; Goetz, Mara ; Giaccherini, Matteo ; Malecka-Wojciesko, Ewa ; Uzunoglu, Faik G ; Kauffmann, Emanuele F ; Greenhalf, William ; Arcidiacono, Paolo Giorgio ; Di Franco, Gregorio ; Aoki, Mateus N ; Cavestro, Giulia Martina ; Mohelnikova-Duchonova, Beatrice ; Morelli, Luca ; Izbicki, Jacob R ; Uno, Miyuki ; Campa, Daniele ; Hegyi, Peter ; Archibugi, Livia ; Chen, Xuechen ; Peduzzi, Giulia ; Tavano, Francesca ; Lucchesi, Maurizio ; Schöttker, Ben ; Bueno-de-Mesquita, Bas ; Maiello, Evaristo ; Pasquali, Claudio ; López de Maturana, Evangelina ; Lovecek, Martin ; Jamroziak, Krzysztof ; Vodicka, Pavel ; Petrone, Maria Chiara ; Pezzilli, Raffaele ; Gentiluomo, Manuel ; Bazzocchi, Francesca ; Gazouli, Maria ; Milanetto, Anna Caterina ; Bijlsma, Marteen F ; Kiudelis, Mindaugas ; Talar-Wojnarowska, Renata ; Katzke, Verena ; Mambrini, Andrea ; Vanella, Giuseppe ; Schneider, Marton ; Gioffreda, Domenica ; Capurso, Gabriele ; Perri, Francesco ; Malats, Nuria ; Testoni, Sabrina G G ; Kupcinskas, Juozas ; Canzian, Federico ; Soucek, Pavel ; Ermini, Stefano ; van Eijck, Casper H J ; Lawlor, Rita T ; Basso, Daniela ; Nappo, Gennaro ; Oliverius, Martin ; Mickevicius, Antanas ; Szentesi, Andrea
Abstract:
Pleiotropic variants (i.e. genetic polymorphisms influencing more than one phenotype) are often associated with cancer risk. A scan of pleiotropic variants was successfully conducted 10 years ago in relation to pancreatic ductal adenocarcinoma susceptibility. However, in the last decade, genetic association studies performed on several human traits have greatly increased the number of known pleiotropic variants. Based on the hypothesis that variants already associated with a least one trait have a higher probability of association with other traits, 61 052 variants reported to be associated by at least one genome-wide association study with at least one human trait were tested in the present study consisting of two phases (discovery and validation), comprising a total of 16 055 pancreatic ductal adenocarcinoma (PDAC) cases and 212 149 controls. The meta-analysis of the two phases showed two loci (10q21.1-rs4948550 (P = 6.52 × 10−5) and 7q36.3-rs288762 (P = 3.03 × 10−5) potentially associated with PDAC risk. 10q21.1-rs4948550 shows a high degree of pleiotropy and it is also associated with colorectal cancer risk while 7q36.3-rs288762 is situated 28,558 base pairs upstream of the Sonic Hedgehog (SHH) gene, which is involved in the cell-differentiation process and PDAC etiopathogenesis. In conclusion, none of the single nucleotide polymorphisms (SNPs) showed a formally statistically significant association after correction for multiple testing. However, given their pleiotropic nature and association with various human traits including colorectal cancer, the two SNPs showing the best associations with PDAC risk merit further investigation through fine mapping and ad hoc functional studies.
2024-02-01·Journal of children's orthopaedics
As simple as it sounds? The treatment of simple bone cysts in the proximal femur in children and adolescents: Retrospective multicenter EPOS study of 74 patients
Article
作者: Soto-Montoya, Camilo ; Döring, Kevin ; Campanacci, Domenico A ; Kraus, Tanja ; Umer, Masood ; van der Heijden, Lizz ; van Geloven, Thomas PG ; Beltrami, Giovanni ; Funovics, Phillipp T ; Dammerer, Dietmar ; Badr, Ismail T ; Saeed, Javeria ; Scheider, Philipp ; Laitinen, Minna K ; Fiocco, Marta ; van de Sande, Michiel AJ ; de Witte, Pieter Bas ; Hobusch, Gerhard M ; Haara, Mikko
Purpose::
Simple bone cysts are among the most prevalent benign cystic tumor-like lesions in children. Proximal femoral simple bone cysts may require specific treatment because of increased fracture risk. With limited literature available on this specific localization, consensus regarding optimal treatment is lacking. We present a large international multicenter retrospective cohort study on proximal femoral simple bone cysts.
Methods::
All consecutive pediatric patients with proximal femoral simple bone cyst from 10 tertiary referral centers for musculoskeletal oncology were included (2000–2021). Demographics, primary treatment, complications, and re-operations were evaluated. Primary outcomes were time until full weight-bearing and failure-free survival.
Results::
Overall, 74 simple bone cyst patients were included (median age 9 years (range = 2–16), 56 (76%) male). Median follow-up was 2.9 years (range = 0.5–21). Index procedure was watchful waiting (n = 6), percutaneous procedure (n = 12), open procedure (n = 50), or osteosynthesis alone (n = 6). Median time until full weight-bearing was 8 weeks (95% confidence interval = 0.1–15.9) for watchful waiting, 9.5 (95% confidence interval = 3.7–15.3) for percutaneous procedure, 11 (95% confidence interval = −0.7 to 13.7) for open procedure, and 6.5 (95% confidence interval = 5.9–16.1) for osteosynthesis alone (p = 0.58). Failure rates were 33%, 58%, 29%, and 0%, respectively (p = 0.069). Overall failure-free survival at 1, 2, and 5 years was 77.8% (95% confidence interval = 68.2–87.4), 69.5% (95% confidence interval = 58.5–80.5), and 62.0% (95% confidence interval = 47.9–76.1), respectively.
Conclusion::
A preferred treatment for proximal femoral simple bone cysts remains unclear, with comparable failure rates and times until full weight-bearing. Watchful waiting may be successful in certain cases. If not feasible, osteosynthesis alone can be considered. Treatment goals should be cyst control, minimizing complications and swift return to normal activities. Therefore, an individualized balance should be made between undertreatment, with potentially higher complication risks versus overtreatment, resulting in possible larger interventions and accompanying complications.
Level of evidence::
Level IV, retrospective multicentre study
2023-12-02·Carcinogenesis
A scan of all coding region variants of the human genome, identifies 13q12.2-rs9579139 and 15q24.1-rs2277598 as novel risk loci for pancreatic ductal adenocarcinoma
Article
作者: Aoki, Mateus Nóbrega ; Sperti, Cosimo ; Mohelnikova-Duchonova, Beatrice ; Gioffreda, Domenica ; Carrara, Silvia ; Ermini, Stefano ; Kiudelis, Mindaugas ; Canzian, Federico ; Uzunoglu, Faik G ; Hegyi, Péter ; Małecka-Wojciesko, Ewa ; Izbicki, Jakob R ; Giaccherini, Matteo ; Neoptolemos, John P ; Landi, Stefano ; Gori, Leonardo ; Lawlor, Rita T ; Vezakis, Antonis ; Oliverius, Martin ; Milanetto, Anna Caterina ; Bunduc, Stefania ; Maleckas, Almantas ; Cavestro, Giulia Martina ; Dell’Anna, Giuseppe ; Zerbi, Alessandro ; Erőss, Bálint ; Tavano, Francesca ; Soucek, Pavel ; Skieceviciene, Jurgita ; van Eijck, Casper H J ; Dijk, Frederike ; Hussein, Tamás ; Szentesi, Andrea ; Boggi, Ugo ; Arcidiacono, Paolo Giorgio ; Lovecek, Martin ; Kupcinskas, Juozas ; Brenner, Hermann ; Capurso, Gabriele ; Furbetta, Niccolò ; Götz, Mara ; Gentiluomo, Manuel ; van Laarhoven, Hanneke W M ; Farinella, Riccardo ; Campa, Daniele ; Cervena, Klara ; Archibugi, Livia ; Pezzilli, Raffaele ; Morelli, Luca ; Pasquali, Claudio ; Ginocchi, Laura ; Gazouli, Maria ; Chammas, Roger ; Ponz de Leon Pisani, Ruggero ; Lucchesi, Maurizio ; Al-Saeedi, Mohammed ; Perri, Francesco ; Talar-Wojnarowska, Renata ; Basso, Daniela ; Holleczek, Bernd ; Schöttker, Ben
Abstract:
Coding sequence variants comprise a small fraction of the germline genetic variability of the human genome. However, they often cause deleterious change in protein function and are therefore associated with pathogenic phenotypes. To identify novel pancreatic ductal adenocarcinoma (PDAC) risk loci, we carried out a complete scan of all common missense and synonymous SNPs and analysed them in a case–control study comprising four different populations, for a total of 14 538 PDAC cases and 190 657 controls. We observed a statistically significant association between 13q12.2-rs9581957-T and PDAC risk (P = 2.46 × 10−9), that is in linkage disequilibrium (LD) with a deleterious missense variant (rs9579139) of the URAD gene. Recent findings suggest that this gene is active in peroxisomes. Considering that peroxisomes have a key role as molecular scavengers, especially in eliminating reactive oxygen species, a malfunctioning URAD protein might expose the cell to a higher load of potentially DNA damaging molecules and therefore increase PDAC risk. The association was observed in individuals of European and Asian ethnicity. We also observed the association of the missense variant 15q24.1-rs2277598-T, that belongs to BBS4 gene, with increased PDAC risk (P = 1.53 × 10−6). rs2277598 is associated with body mass index and is in LD with diabetes susceptibility loci. In conclusion, we identified two missense variants associated with the risk of developing PDAC independently from the ethnicity highlighting the importance of conducting reanalysis of genome-wide association studies (GWASs) in light of functional data.
6
项与 Azienda Ospedaliero-Universitaria Meyer 相关的新闻(医药)2025-05-09
- 28-week data from the Phase 2b VANTAGE PBC study highlights statistically significant improvements in pruritus and numeric improvements in fatigue, the two most burdensome symptoms of PBC
- Seventy percent of patients treated with volixibat experienced a ≥50% reduction in serum bile acids
- Volixibat treated patients experienced reductions in IL-31
FOSTER CITY, Calif.--(BUSINESS WIRE)-- Mirum Pharmaceuticals, Inc. (NASDAQ: MIRM) today presented new data from its Phase 2b VANTAGE study at the European Association for the Study of the Liver (EASL) meeting in Amsterdam, the Netherlands. The VANTAGE study is evaluating volixibat in patients with cholestatic pruritus caused by primary biliary cholangitis (PBC).
“The extended VANTAGE analysis provides encouraging insights into the potential impact that volixibat may have in treating the most severe and bothersome symptoms for patients living with PBC, including pruritus and fatigue,” said Joanne Quan, MD, chief medical officer at Mirum. “We are also encouraged by the reductions seen in IL-31 in conjunction with sBA reductions, showing the potential for volixibat treatment to help alter the inflammatory condition present in PBC.”
Data from the interim analysis of VANTAGE were highlighted with new analyses through week 28. Patients were randomized to receive volixibat 20mg BID, 80mg BID, or placebo BID. The primary endpoint of the study was mean change in weekly averaged daily itch score, as measured by the adult ItchRO scale, from baseline to Week 17-Week 28. Volixibat treatment led to rapid (as early as week 1) and sustained reductions in ItchRO with the volixibat combined dose group achieving a statistically significant 3.78-point reduction from Baseline (p<0.0001) and a placebo-adjusted response of 2.51 (p=0.0004). Each volixibat dose achieved statistically significant and similar responses (20mg BID: -2.4 [P=0.0039]; 80mg BID: -2.6 [P=0.0010]). The analysis also provided data across secondary endpoints showing reductions in serum bile acids (sBA) and quality of life (QoL) measures. Overall, 70% of patients who received volixibat achieved ≥50% reduction in sBA. Further, the data showed improvement from baseline in health-related quality of life, including fatigue and sleep, for patients treated with volixibat. Reductions from baseline were observed in inflammatory biomarker IL-31 in patients treated with volixibat.
No new safety signals were observed, and adverse events were similar between the 20 mg and 80 mg treatment groups. The most common adverse event was diarrhea (77%) with all cases mild to moderate; one case resulted in discontinuation. Given the similar results with both efficacy and safety between the 20mg BID and 80mg doses BID, the 20mg BID dose was selected for the confirmatory portion of the VANTAGE study.
To view the presentation, please visit the Publications & Presentations on Mirum’s website.
About the VANTAGE Study
VANTAGE is a randomized, double-blind, placebo-controlled study evaluating the efficacy and safety of volixibat in patients with pruritus caused by primary biliary cholangitis (PBC). Patients were randomized to receive volixibat 20mg BID (n=10), 80mg BID (n=10), or placebo BID (n=11). The primary endpoint of the study was mean change in weekly averaged daily itch score, as measured by the adult ItchRO scale (an 11 point scale where 0 = no itch and 10 = worst itch imaginable), from baseline to Week 17-Week 28. VANTAGE is designed as a two-part study: the first part is intended to confirm dose (completed) and the second intended to be the confirmatory portion (currently enrolling patients). In the first part of the study, patients were randomized to receive either volixibat 20mg BID, 80mg BID, or placebo BID; the second part of the study randomized patients to receive either volixibat 20mg BID (the selected dose based on part one) or placebo BID.
About Primary Biliary Cholangitis
Primary Biliary Cholangitis (PBC) is a chronic, progressive, immune-mediated condition leading to the destruction of small intrahepatic bile ducts. The disease impacts an estimated 230,000 patients in the United States and the European Union, with women predominantly affected (a sex ratio of 9:1). Key clinical features and symptoms include cholestatic pruritus, fatigue, sicca syndrome, abdominal pain, cirrhosis, and hepatocellular carcinoma. Cholestatic pruritus (itch) and fatigue are two of the most debilitating symptoms and greatly affect overall health-related quality of life (HRQoL). Cholestatic pruritus can affect up to 80% of individuals and is thought to result in part from accumulation of toxic bile acids.
About Volixibat
Volixibat is an oral, minimally absorbed agent designed to selectively inhibit the ileal bile acid transporter (IBAT). Volixibat may offer a novel approach in the treatment of adult cholestatic diseases by blocking the recycling of bile acids, through inhibition of IBAT, thereby reducing bile acids systemically and in the liver. Volixibat is currently being evaluated in Phase 2b studies for primary sclerosing cholangitis (PSC) (VISTAS study), and primary biliary cholangitis (PBC) (VANTAGE study). In June, Mirum announced positive interim results from the Phase 2b VANTAGE study showing statistically significant improvement in pruritus as well as reductions in serum bile acids and improvements in fatigue for patients treated with volixibat. No new safety signals were observed, and the most common adverse event was diarrhea with all cases mild to moderate. Volixibat has been granted breakthrough therapy designation for the treatment of PBC.
About LIVMARLI® (maralixibat) oral solution and LIVMARLI® (maralixibat) tablets
LIVMARLI® (maralixibat) is an orally administered, ileal bile acid transporter (IBAT) inhibitor approved by the U.S. Food and Drug Administration for two pediatric cholestatic liver diseases, in both liquid and tablet formulations. It is approved for the treatment of cholestatic pruritus in patients with Alagille syndrome (ALGS) in the U.S. three months of age and older and in Europe for patients two months of age and older. It is also approved in the U.S. for the treatment of cholestatic pruritus in patients with progressive familial intrahepatic cholestasis (PFIC) 12 months of age and older and in Europe for the treatment of PFIC in patients three months of age and older. For more information for U.S. residents, please visit LIVMARLI.com.
LIVMARLI is currently being evaluated in the Phase 3 EXPAND study in additional settings of cholestatic pruritus. To learn more about ongoing clinical trials with LIVMARLI, please visit Mirum’s clinical trials section on the company’s website.
U.S. IMPORTANT SAFETY INFORMATION
Limitation of Use: LIVMARLI is not for use in PFIC type 2 patients who have a severe defect in the bile salt export pump (BSEP) protein.
LIVMARLI can cause side effects, including:
Liver injury. Changes in certain liver tests are common in patients with Alagille syndrome and PFIC but can worsen during treatment. These changes may be a sign of liver injury. In PFIC, this can be serious or may lead to liver transplant or death. Your healthcare provider should do blood tests and physical exams before starting and during treatment to check your liver function. Tell your healthcare provider right away if you get any signs or symptoms of liver problems, including nausea or vomiting, skin or the white part of the eye turns yellow, dark or brown urine, pain on the right side of the stomach (abdomen), bloating in your stomach area, loss of appetite or bleeding or bruising more easily than normal.
Stomach and intestinal (gastrointestinal) problems. LIVMARLI can cause stomach and intestinal problems, including diarrhea and stomach pain. Your healthcare provider may advise you to monitor for new or worsening stomach problems including stomach pain, diarrhea, blood in your stool or vomiting. Tell your healthcare provider right away if you have any of these symptoms more often or more severely than normal for you.
A condition called Fat Soluble Vitamin (FSV) Deficiency caused by low levels of certain vitamins (vitamin A, D, E, and K) stored in body fat is common in patients with Alagille syndrome and PFIC but may worsen during treatment. Your healthcare provider should do blood tests before starting and during treatment and may monitor for bone fractures and bleeding which have been reported as common side effects.
LIVMARLI is available in oral solution or tablet formulations and is taken by mouth 30 minutes before a meal. For Alagille syndrome, LIVMARLI is taken one time each day in the morning. For PFIC, LIVMARLI is taken two times each day. If you take the oral solution, use the oral dosing dispenser to measure your dose.
US Prescribing Information EU SmPC Canadian Product Monograph
About Mirum Pharmaceuticals, Inc.
Mirum Pharmaceuticals, Inc. is a biopharmaceutical company dedicated to transforming the treatment of rare diseases affecting children and adults. Mirum has three approved medications: LIVMARLI® (maralixibat) oral solution/LIVMARLI® (maralixibat) tablets, CHOLBAM® (cholic acid) capsules, and CTEXLI™ (chenodiol) tablets.
LIVMARLI, an IBAT inhibitor, is approved for the treatment of two rare liver diseases affecting children and adults. It is approved for the treatment of cholestatic pruritus in patients with Alagille syndrome in the U.S. (three months and older), in Europe (two months and older), and in other regions globally. It is also approved in the U.S. in cholestatic pruritus in PFIC patients 12 months of age and older; in Europe, it is approved for patients with PFIC three months of age and older. Mirum has initiated the Phase 3 EXPAND study, a label expansion opportunity for LIVMARLI in additional settings of cholestatic pruritus. CHOLBAM is FDA-approved for the treatment of bile acid synthesis disorders due to single enzyme deficiencies and adjunctive treatment of peroxisomal disorders in patients who show signs or symptoms of liver disease.
CTEXLI is FDA-approved for the treatment of cerebrotendinous xanthomatosis (CTX) in adults. Mirum's late-stage pipeline includes two investigational treatments for several rare diseases.
Volixibat, an IBAT inhibitor, is being evaluated in two potentially registrational studies including the Phase 2 VISTAS study for primary sclerosing cholangitis (PSC) and Phase 2b VANTAGE study for primary biliary cholangitis. Volixibat has been granted Breakthrough Therapy Designation for the treatment of cholestatic pruritus in patients with PBC. Mirum is also planning for a Phase 2 study evaluating MRM-3379, a PDE4D inhibitor for the treatment of Fragile X syndrome, a rare genetic neurocognitive disorder.
To learn more about Mirum, visit mirumpharma.com and follow Mirum on Facebook, LinkedIn, Instagram and Twitter (X).
Forward-Looking Statements
Statements contained in this press release regarding matters that are not historical facts are “forward-looking statements” within the meaning of the Private Securities Litigation Reform Act of 1995. Such forward-looking statements include statements regarding, among other things, data from Mirum’s volixibat studies, including the VANTAGE study of volixibat in patients with pruritus due to PBC and such implications for patients in real world settings. Because such statements are subject to risks and uncertainties, actual results may differ materially from those expressed or implied by such forward-looking statements. Words such as “will,” “could,” “can,” “would,” “potential,” “hope,” “opportunity,” and similar expressions are intended to identify forward-looking statements. These forward-looking statements are based upon Mirum’s current expectations and involve assumptions that may never materialize or may prove to be incorrect. Actual results could differ materially from those anticipated in such forward-looking statements as a result of various risks and uncertainties, which include, without limitation, risks and uncertainties associated with Mirum’s business in general, the impact of macroeconomic and geopolitical developments, and the other risks described in Mirum’s Annual Report on Form 10-K for the year ended December 31, 2024, filed with the U.S. Securities and Exchange Commission on February 26, 2025, and subsequent filings with the U.S. Securities and Exchange Commission, which are available at www.sec.gov. All forward-looking statements contained in this press release speak only as of the date on which they were made and are based on management’s assumptions and estimates as of such date. Mirum undertakes no obligation to update such statements to reflect events that occur or circumstances that exist after the date on which they were made, except as required by law.
Media Contact: Erin Murphy media@mirumpharma.com
Investor Contact: Andrew McKibben ir@mirumpharma.com
临床2期临床结果上市批准突破性疗法临床3期
2025-05-07
·生物谷
CodeBreaK 300试验为KRAS G12C突变结直肠癌患者带来了新的希望,索托拉西布联合帕尼单抗的组合疗法在延长无进展生存期和提高客观缓解率方面表现出显著优势,为患者提供了一种新型治疗选择。
在癌症治疗领域,结直肠癌一直是全球范围内发病率和死亡率较高的恶性肿瘤之一,其中,KRAS G12C突变的结直肠癌更是因其对传统化疗的耐药性而成为治疗难题。
然而,近日,一篇发表在国际杂志Journal of Clinical Oncology上题为“Overall Survival Analysis of the Phase III CodeBreaK 300 Study of Sotorasib Plus Panitumumab Versus Investigator's Choice in Chemorefractory KRAS G12C Colorectal Cancer”的研究报告中,来自City of Hope等机构的科学家们通过进行一项名为CodeBreaK 300的III期临床试验后发现,索托拉西布(sotorasib)联合帕尼单抗(panitumumab)的新型组合性疗法有望为化疗耐药的KRAS G12C突变结直肠癌患者带来更好的治疗效果。
结直肠癌是全球第三大常见癌症,每年新增病例超过190万例。尽管手术、化疗和靶向治疗等手段不断进步,但仍有约50%的患者最终会发展为转移性结直肠癌(mCRC);其中KRAS基因突变是结直肠癌中最常见的驱动因素之一,约45%的结直肠癌患者存在KRAS突变,而KRAS G12C突变在这些患者中占比约10%,KRAS蛋白的异常激活会导致肿瘤细胞的无限制生长和增殖,使得治疗变得极为复杂。
近年来,随着对KRAS G12C突变机制的深入研究,科学家们逐渐找到了破解这一难题的钥匙。作为一种特异性KRAS G12C抑制剂,索托拉西布能精准靶向作用KRAS G12C蛋白从而阻止其激活,进而抑制癌细胞的生长;而帕尼单抗则是一种针对表皮生长因子受体(EGFR)的单克隆抗体,其能阻断EGFR介导的细胞生长信号通路,将这两种药物联合使用有望实现协同作用,并为患者带来更好的治疗效果。
CodeBreaK 300试验是一项国际多中心、随机、对照的三期临床试验,旨在评估索托拉西布联合帕尼单抗在KRAS G12C突变的化疗耐药转移性结直肠癌患者中的疗效和安全性。试验中,研究人员共纳入了160名患者,将其随机分为三组,一组接受960 mg索托拉西布联合帕尼单抗治疗;一组接受240 mg索托拉西布联合帕尼单抗治疗;另一组则接受研究者选择的标准治疗(trifluridine/tipiracil或regorafenib)。
患者分配的CONSORT流程图
研究结果表明,接受960 mg索托拉西布联合帕尼单抗治疗的患者,其无进展生存期(PFS)显著延长,中位PFS达到5.7个月,而标准治疗组仅为2.0个月。此外,客观缓解率(ORR)也显著提高,960 mg联合治疗组的ORR为30.2%,240 mg联合治疗组为7.5%,而标准治疗组仅为1.9%。尽管总生存期(OS)的统计学差异未达到显著性,但960 mg联合治疗组的OS显示出30%的相对降低风险趋势,中位OS尚未达到,而标准治疗组为10.3个月。
这项研究的亮点在于,索托拉西布联合帕尼单抗的组合疗法在多个关键指标上均优于标准治疗,特别是960 mg剂量组的患者,其不仅在PFS和ORR上表现出显著优势,而且在OS上也显示出潜在的改善趋势,这一结果表明,这种联合疗法能更有效地控制肿瘤进展从而延长患者的生存时间,这就为KRAS G12C突变结直肠癌患者提供了一种新的治疗选择。此外,这种联合疗法的安全性也得到了验证,在治疗过程中,虽然患者出现了一些常见的不良反应,比如腹泻、肌肉骨骼疼痛、恶心、疲劳、肝毒性等,但这些不良反应大多能通过调整剂量或对症治疗得到控制。而且研究中研究人员未观察到新的安全信号,这就为该联合疗法的临床应用提供了有力支持。
CodeBreaK 300试验的成功为KRAS G12C突变结直肠癌的治疗带来了新的希望。然而这项研究也存在一些局限性,比如由于样本量较小,OS的统计学差异未能达到显著性,这或许会影响结果的说服力,此外,尽管联合疗法在PFS和ORR上表现出显著优势,但在OS上的改善趋势仍需在更大规模的试验中进一步验证。未来,研究人员计划在更大样本量的患者中开展进一步的研究从而验证这种联合疗法在一线治疗中的效果。此外,他们还将探索如何优化联合疗法的剂量和给药方案从而进一步提高疗效和安全性。随着对KRAS G12C突变机制的深入研究,以及更多新型靶向药物的不断涌现,我们有理由相信,联合疗法将在结直肠癌的治疗中发挥越来越重要的作用。
综上,CodeBreaK 300试验为KRAS G12C突变结直肠癌患者带来了新的希望,索托拉西布联合帕尼单抗的组合疗法在延长无进展生存期和提高客观缓解率方面表现出显著优势,这就为患者提供了一种新型治疗选择。随着未来研究的不断深入,这种联合疗法有望成为结直肠癌治疗的新标准。(生物谷Bioon.com)
参考文献:
Filippo Pietrantonio,Lisa Salvatore, Taito Esaki, et al. Overall Survival Analysis of the Phase III CodeBreaK 300 Study of Sotorasib Plus Panitumumab Versus Investigator's Choice in Chemorefractory KRAS G12C Colorectal Cancer, Journal of Clinical Oncology (2025). DOI:10.1200/JCO-24-02026
临床3期临床2期临床结果
2025-04-30
Results of part 1 of the ESSENCE phase 3 trial, published in The New England Journal of Medicine, demonstrated that a greater proportion of patients with MASH achieved resolution of steatohepatitis with no worsening of liver fibrosis compared to placebo. Patients with MASH also saw statistically significant and superior improvement in liver fibrosis with no worsening of steatohepatitis compared to placebo1
Approximately one in 20 people in the US are living with MASH.2 Left untreated, MASH can progress to serious and even fatal outcomes, such as cirrhosis, liver cancer, and the need for liver transplant3
Additionally, Novo Nordisk's application for Wegovy® (semaglutide) injection 2.4 mg for the treatment of metabolic dysfunction-associated steatohepatitis (MASH) was recently accepted by FDA and granted Priority Review
PLAINSBORO, N.J., April 30, 2025 /PRNewswire/ -- Today, The New England Journal of Medicine (NEJM) published results from part 1 of the ongoing phase 3 ESSENCE trial which investigated the effects of once-weekly subcutaneous semaglutide 2.4 mg on liver histology compared to placebo at 72 weeks in adults with MASH and moderate to advanced liver fibrosis (stage 2 or 3). At Week 72, the first primary endpoint showed 62.9% of people treated with semaglutide 2.4 mg achieved resolution of steatohepatitis with no worsening of liver fibrosis compared to 34.3% on placebo with estimated difference in responder proportions (EDP) of 28.7% (95% CI, 21.1 to 36.2; P<0.001). For the second primary endpoint at Week 72, 36.8% of people treated with semaglutide 2.4 mg achieved improvement in liver fibrosis with no worsening of steatohepatitis compared to 22.4% on placebo (EDP, 14.4%; 95% CI, 7.5 to 21.3; P<0.001).1
"ESSENCE part 1 demonstrates the effects of semaglutide 2.4 mg on the key histological elements, which may reduce disease progression to cirrhosis and end-stage liver disease," said Arun Sanyal, MD, lead author, principal investigator, and Director, Stravitz-Sanyal Institute for Liver Disease and Metabolic Health, Virginia Commonwealth University. "This is crucial, given the strong link between MASH and other cardiometabolic conditions."
A confirmatory secondary endpoint at Week 72 showed 32.7% of patients treated with semaglutide 2.4 mg achieved both resolution of steatohepatitis and improvement in liver fibrosis compared to 16.1% of patients on placebo (EDP, 16.5%; 95% CI, 10.2 to 22.8; P<0.001).1
Furthermore, Novo Nordisk also announced that the US Food and Drug Administration has accepted the supplemental New Drug Application (sNDA) and granted Priority Review for Wegovy® (semaglutide) injection 2.4 mg to treat noncirrhotic MASH in adults with moderate to advanced liver scarring (fibrosis). Priority review designation means that FDA will review the application in six months, rather than the standard nine-month review period.
"Novo Nordisk continues to explore semaglutide across metabolic and cardiovascular health including MASH, a condition with limited treatment options for patients and healthcare professionals," said Anna Windle, PhD, senior vice president of Clinical Development, Medical & Regulatory Affairs at Novo Nordisk. "We are encouraged by these published findings in the NEJM and what this could mean for patients. Based on these data, we look forward to working with regulatory authorities to bring this potential new treatment option to patients."
Non-invasive tests (NITs) are valuable in supporting the screening of people at risk of developing MASH and may address early MASH detection. Implementing NITs may allow for fibrosis risk stratification earlier in the disease progression journey.4,5 The expanded analysis of ESSENCE showed apparent improvements of pre-specified NITs, including vibration-controlled transient elastography (VCTE), the Enhanced Liver Fibrosis (ELF)™ test, and PRO-C3, in adults treated with semaglutide 2.4 mg compared to placebo. These were supportive secondary endpoints, not controlled for multiplicity.1
Safety endpoints in the ESSENCE trial included adverse events and laboratory assessments. By Week 72, 88% of participants received and maintained the full target dose of semaglutide 2.4 mg. No new safety signals emerged, and the safety profile was consistent with the vast body of evidence for semaglutide. The most common adverse events were gastrointestinal-related, including nausea (36.3% semaglutide; 13.2% placebo), diarrhea (26.9% semaglutide; 12.2% placebo), constipation (22.3% semaglutide; 8.4% placebo), and vomiting (18.6% semaglutide; 5.6% placebo). Adverse events leading to trial discontinuation were 2.6% for the semaglutide group and 3.3% for the placebo group.1
Semaglutide 2.4 mg is not approved in the US for the treatment of MASH.
About ESSENCE
ESSENCE is a phase 3 trial evaluating the effect of once-weekly subcutaneous semaglutide 2.4 mg in adults with metabolic dysfunction-associated steatohepatitis with moderate to advanced liver fibrosis (stage 2 or 3). It is a two-part trial where an estimated 1,200 planned participants are randomized 2:1 to receive semaglutide 2.4 mg or placebo, on top of standard of care for 240 weeks. Lifestyle counseling and management of coexisting diseases were recommended in alignment with guidelines. In part 1, the objective was to demonstrate that treatment with semaglutide 2.4 mg improves liver histology compared with placebo at 72 weeks based on biopsy sampling from the first 800 randomized patients. In part 2, which is ongoing, the objective is to demonstrate that treatment with semaglutide 2.4 mg lowers the risk of liver-related clinical events compared to placebo in adults with MASH and moderate to advanced liver fibrosis at 240 weeks.1,6
About semaglutide 2.4 mg
Semaglutide injection 2.4 mg is previously approved along with a reduced calorie diet and increased physical activity, for adults and children aged 12 years and older with obesity, or some adults with overweight who also have weight-related medical problems, to help them lose excess body weight and keep the weight off and to reduce the risk of major CV events such as death, heart attack, or stroke in adults with known heart disease and either obesity or overweight.7
It is important to note that semaglutide injection 2.4 mg contains a Boxed Warning for possible thyroid tumors, including cancer and should not be used in those with a personal or family history of medullary thyroid carcinoma (MTC) or Multiple Endocrine Neoplasia syndrome type 2 (MEN 2).7
Semaglutide is not approved for the treatment of adults with MASH. Safety and efficacy are not established, and there is no guarantee that semaglutide will become commercially available for this use under clinical investigation.
About Metabolic Dysfunction-Associated Steatohepatitis (MASH)
MASH is a chronic, progressive metabolic disease affecting the liver, which can be potentially life-threatening if not properly managed.8,9 Among people who are living with overweight or obesity, approximately one in three also have MASH.10 Excess fat can build up in the liver, which, over time, can lead to inflammation and severe scarring of the liver.11 People living with MASH often experience few or no specific symptoms in the early stages of the disease, which often results in a delayed diagnosis.12 Approximately, one in 20 people in the United States are living with MASH.2 The disease progresses to cirrhosis in an estimated 20% of cases.13 MASH is a leading cause of cirrhosis in adults in the US, and MASH-related cirrhosis is the second indication for liver transplants in the country.14
About Novo Nordisk
Novo Nordisk is a leading global healthcare company that's been making innovative medicines to help people with diabetes lead longer, healthier lives for more than 100 years. This heritage has given us experience and capabilities that also enable us to drive change to help people defeat other serious chronic diseases such as obesity, rare blood, and endocrine disorders. We remain steadfast in our conviction that the formula for lasting success is to stay focused, think long-term, and do business in a financially, socially, and environmentally responsible way. With a US presence spanning 40 years, Novo Nordisk US is headquartered in New Jersey and employs over 10,000 people throughout the country across 12 manufacturing, R&D and corporate locations in eight states plus Washington DC. For more information, visit novonordisk-us.com, Facebook, Instagram, and X.
Novo Nordisk is committed to the responsible use of our semaglutide-containing medicines which represent distinct products with different indications, dosages, prescribing information, titration schedules, and delivery forms. These products are not interchangeable and should not be used outside of their approved indications. Learn more at semaglutide.com.
Contacts for further information
References
Sanyal AJ, Newsome PN, Kliers I, et al. Phase 3 trial of semaglutide in metabolic dysfunction-associated steatohepatitis. New Eng J Med. 2025;392(17). doi:10.1056/NEJMoa2413258
Younossi ZM, Mangla KK, Chandramouli AS, et al. Estimating the economic impact of comorbidities in patients with MASH and defining high-cost burden in patients with noncirrhotic MASH. Hepatol Commun. 2024;8:e0488. doi:10.1097/HC9.0000000 000000488
Fichez J, Mouillot T, Vonghia L, et al. Non-invasive tests for fibrotic MASH for reducing screen failure in therapeutic trials. JHEP Reports. 2025;7(4);101351. doi:10.1016/j.jhepr.2025.10135
Wattacheril JJ, Abdelmalek MF, Lim JK, et al. AGA clinical practice update on the role of noninvasive biomarkers in the evaluation and management of nonalcoholic fatty liver disease: expert review. Gastroenterology. 2023;165:1080-1088. doi:10.1053/j.ga stro.2023.06.013
Rinella ME, Neuschwander-Tetri BA, Siddiqui MS, et al. AASLD practice guidance on the clinical assessment and management of nonalcoholic fatty liver disease. Hepatology. 2023;77:1797-1835. doi:10.1097/HEP.0000000000000323
Newsome PN, Sanyal AJ, Engebretsen KA, et al. Semaglutide 2.4 mg in participants with metabolic dysfunction-associated steatohepatitis: baseline characteristics and design of the phase 3 ESSENCE trial. Aliment Pharmacol Ther. 2024;10:18331. doi:10.1111/apt.18331
Wegovy® (semaglutide) injection [package insert]. Plainsboro, NJ: Novo Nordisk Inc.
Ilan Y. Analogy between non-alcoholic steatohepatitis (NASH) and hypertension: a stepwise patient-tailored approach for NASH treatment. Ann Gastroenterol. 2018;
31:296-304. doi:10.20524/aog.2018.0248
Tesfay M, Goldkamp JW, Neuschwander-Tetri BA. NASH: the emerging most common form of chronic liver disease. Mo Med. 2018;115:225-229.
Quek J, Chan KE, Wong ZY, et al. Global prevalence of non-alcoholic fatty liver disease and non-alcoholic steatohepatitis in the overweight and obese population: a systematic review and meta-analysis. Lancet Gastroenterol Hepatol. 2023;8:20-30. doi: 10.1016/S2468-1253(22)00317-X
National Institute of Diabetes and Digestive and Kidney Diseases. Definition & facts of NAFLD & NASH. Accessed November 7, 2024. Available at:
Allen AM, Charlton M, Cusi K, et al. Guideline-based management of metabolic dysfunction-associated steatotic liver disease in the primary care setting. Postgrad Med. 2024;136:229-245. doi:10.1080/00325481.2024.2325332
Sheka AC, Adeyi O, Thompson J, et al. Nonalcoholic steatohepatitis: a review. JAMA. 2020;323:1619. doi:10.1001/jama.2020.5249
Younossi ZM, Koenig AB, Abdelatif D, et al. Global epidemiology of nonalcoholic fatty liver disease-Meta-analytic assessment of prevalence, incidence, and outcomes. Hepatology. 2016;64(1):73-84. doi:10.1002/hep.28431
SOURCE NOVO NORDISK INC.
WANT YOUR COMPANY'S NEWS FEATURED ON PRNEWSWIRE.COM?
440k+
Newsrooms &
Influencers
9k+
Digital Media
Outlets
270k+
Journalists
Opted In
GET STARTED
临床结果临床3期优先审批临床2期
100 项与 Azienda Ospedaliero-Universitaria Meyer 相关的药物交易
登录后查看更多信息
100 项与 Azienda Ospedaliero-Universitaria Meyer 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2025年09月16日管线快照
无数据报导
登录后保持更新
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
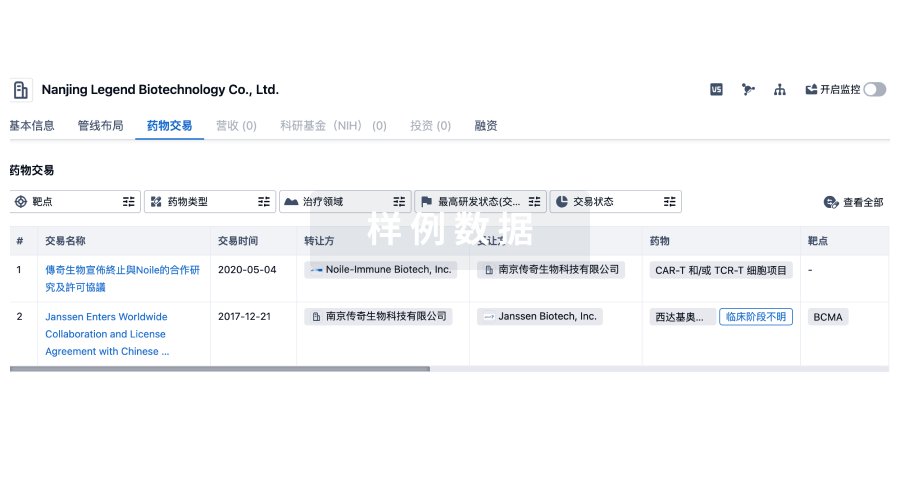
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
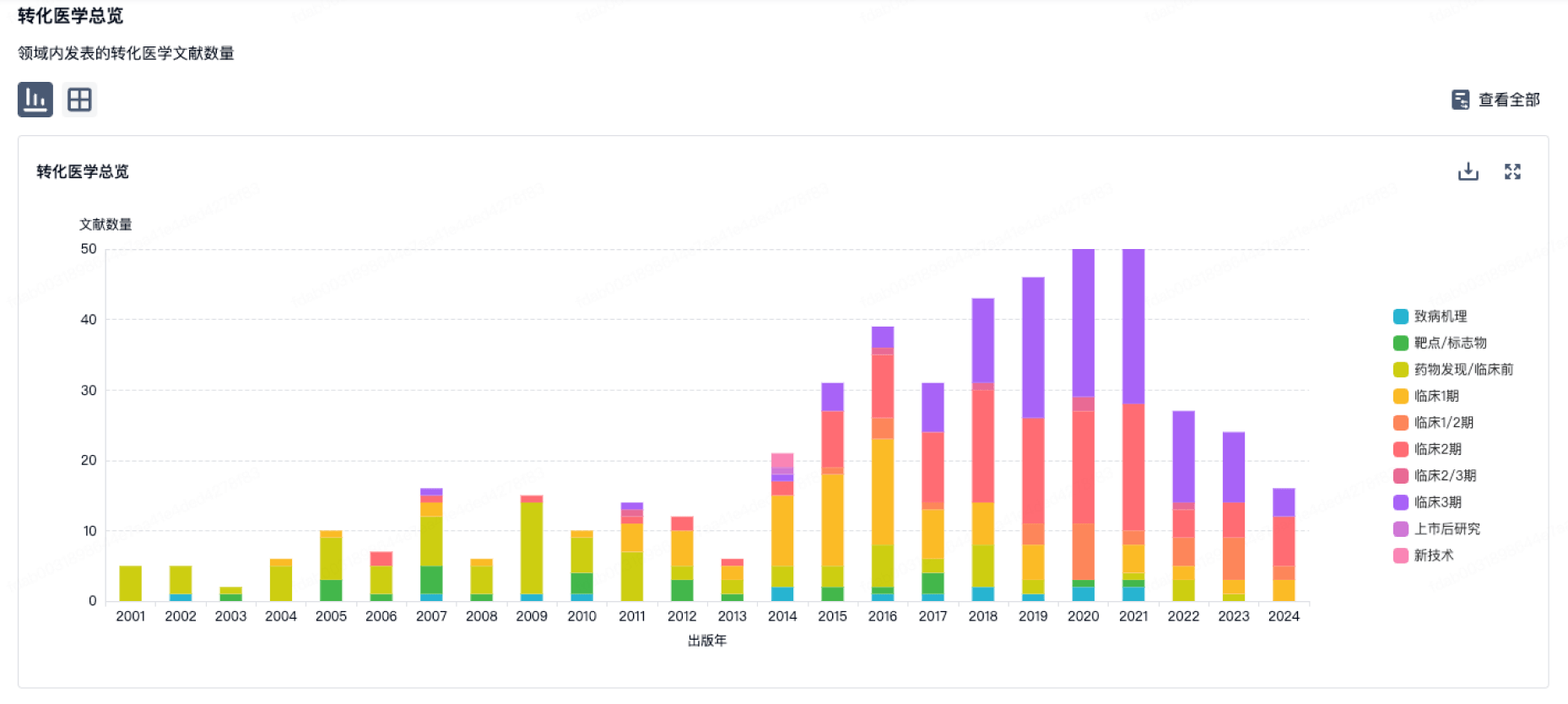
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
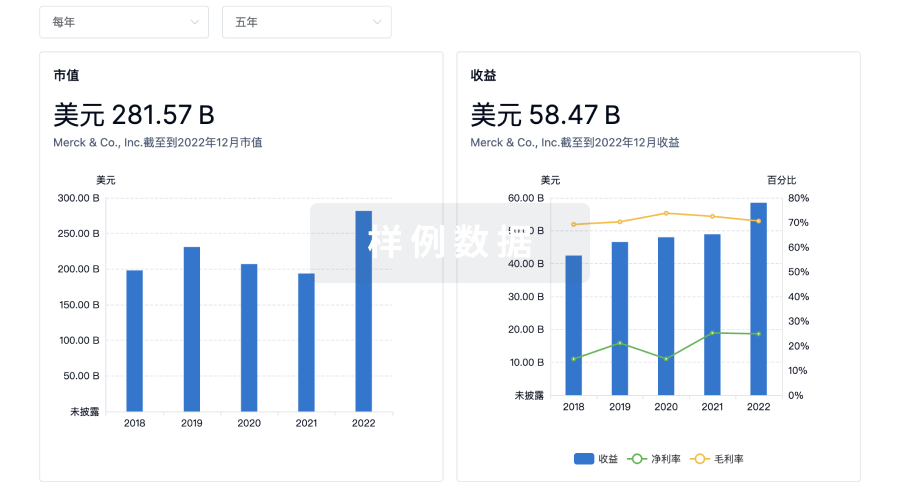
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
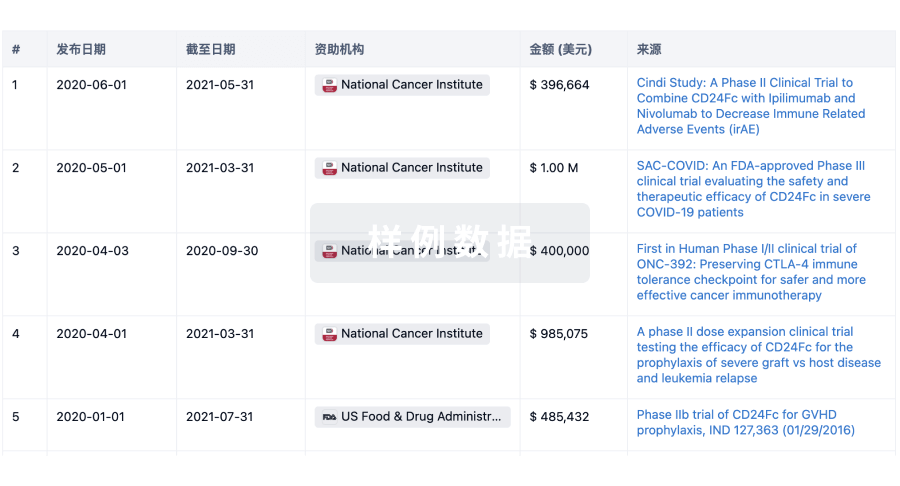
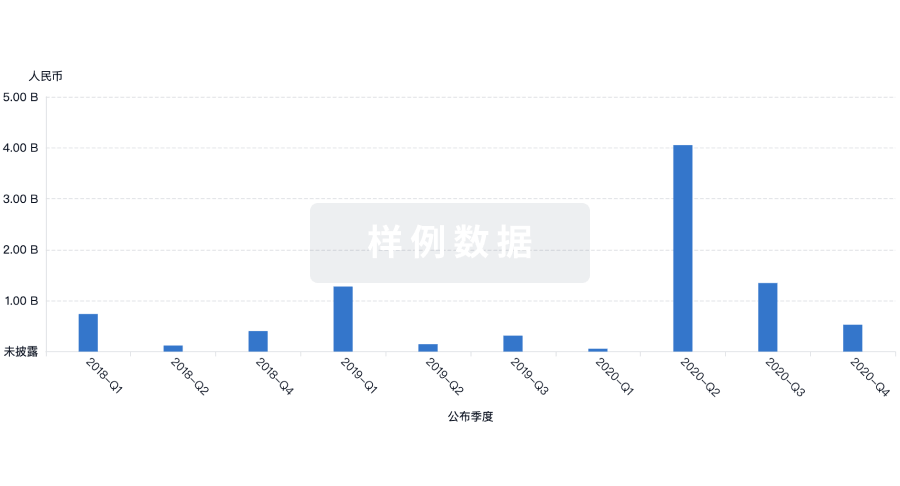
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
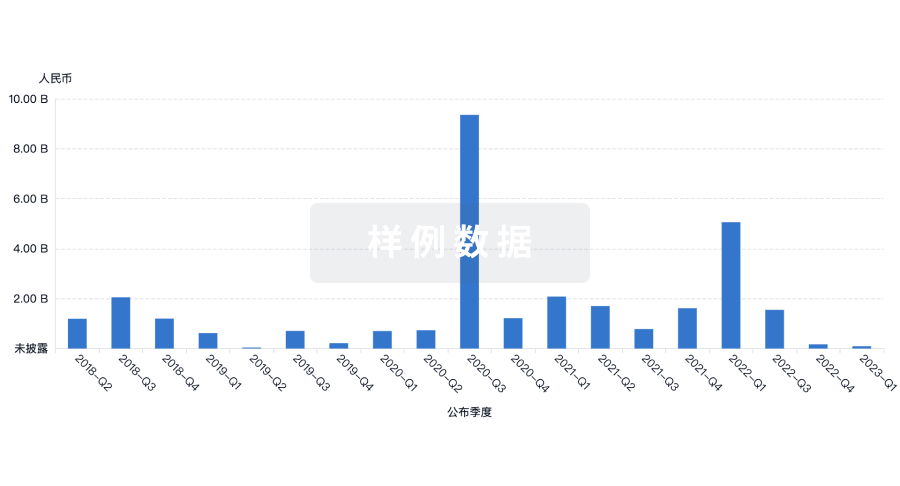
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
Eureka LS:
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
