预约演示
更新于:2025-05-07

West Michigan Cancer Center, Inc.
更新于:2025-05-07
概览
关联
2
项与 West Michigan Cancer Center, Inc. 相关的临床试验NCT06364748
Expanding Access to Care Through Telemedical Support for Vital Sign Monitoring in High-risk Patients With Cancer
A randomized trial of remote blood pressure monitoring, compared to usual care, in patients receiving bevacizumab to determine whether remote blood pressure monitoring improves the collection of blood pressure data, identification and management of clinically significant hypertension, and patient satisfaction.
开始日期2024-03-11 |
NCT06063577
A Randomized Controlled Trial Evaluating the Use of Stratafix Symmetric™ to Prevent Incisional Hernia in Gastrointestinal and Abdominal Surgery
Comparing the use of Stratafix Symmetric™ sutures to standard laparotomy closure sutures.
开始日期2023-12-01 |
申办/合作机构 |
100 项与 West Michigan Cancer Center, Inc. 相关的临床结果
登录后查看更多信息
0 项与 West Michigan Cancer Center, Inc. 相关的专利(医药)
登录后查看更多信息
89
项与 West Michigan Cancer Center, Inc. 相关的文献(医药)2025-10-01·The American Journal of Surgery
Sheltered yet unscreened: Exploring cancer screening rates and barriers in the unhoused (homeless) population
Article
作者: Shebrain, Saad ; Olivier, Ryan C ; Kumar, Neya Suresh ; Kalina, Claire ; Dawood, Nataly ; Munene, Gitonga ; Laird, Madison C ; Al-Assil, Talal ; Dickson, Cheryl ; Riordan, Raven
2025-02-10·Journal of Clinical Oncology
Contemporary post-prostatectomy radiation therapy for prostate cancer within a statewide quality consortium.
作者: Paluch, Sarah ; Zaki, Mark A. ; Yin, Huiying ; Schipper, Matthew J. ; Jackson, William C. ; McLaughlin, Patrick ; Dykstra, Michael ; Dess, Robert Timothy ; Heimburger, David K. ; Mislmani, Mazen ; Smith, Andrea ; Kendrick, Danielle ; Regan, Samuel
2025-01-01·Gynecologic Oncology
Clinical trials are not the solution to inequities in cancer care
作者: Miller, Franklin G ; Shalowitz, David I
1
项与 West Michigan Cancer Center, Inc. 相关的新闻(医药)2025-01-29
BLINCYTO
Added to Multiphase Consolidation Chemotherapy Significantly Reduced the Risk of Death Versus Chemotherapy Alone
THOUSAND OAKS, Calif., Jan. 29, 2025 /PRNewswire/ -- Amgen (NASDAQ:AMGN) today announced that the European Commission (EC) has approved BLINCYTO® (blinatumomab) monotherapy as part of consolidation therapy for the treatment of adult patients with newly diagnosed Philadelphia chromosome-negative CD19-positive B-cell precursor acute lymphoblastic leukemia (B-ALL).
"This approval represents a significant advancement, offering patients the opportunity to receive BLINCYTO earlier in their treatment pathway, with the potential to improve outcomes," said Jean-Charles Soria, senior vice president of Global Oncology Development at Amgen. "The E1910 data that served as the basis of this approval adds to the growing body of evidence of the meaningful survival impact of BLINCYTO."
The Phase 3 E1910 clinical trial led by ECOG-ACRIN Cancer Research Group studied patients with newly diagnosed Philadelphia chromosome-negative B-ALL receiving postinduction consolidation treatment, which aims to deepen remission to achieve durable responses. Study results demonstrated that BLINCYTO added to multiphase consolidation chemotherapy showed superior overall survival (OS) versus chemotherapy alone. With a median follow-up of 4.5 years, the 5-year OS was 82.4% in the BLINCYTO plus chemotherapy arm (n=112) and 62.5% in the chemotherapy arm (n=112).
"While there has been some treatment progress, many patients with newly diagnosed Philadelphia chromosome-negative B-ALL remain at high risk of relapse," said Robin Foà, M.D., emeritus professor of hematology, Sapienza University of Rome. "The E1910 study results highlight that BLINCYTO has the potential to advance frontline consolidation treatment, including patients who are minimal residual disease (MRD)-negative, offering a crucial new option to achieve deeper remissions and improve long-term survival."
The E1910 study was designed and conducted independently from industry. ECOG-ACRIN led the trial with public funding and sponsorship provided by the National Cancer Institute (NCI), part of the National Institutes of Health (NIH). Other NCI-funded network groups took part in the study. In addition, Amgen provided BLINCYTO and support through an NCI Cooperative Research and Development Agreement.
About Acute Lymphoblastic Leukemia (ALL)
ALL, also known as acute lymphoblastic leukemia, is a fast-growing type of blood cancer that develops in the bone marrow and can sometimes spread to other parts of the body, including the lymph nodes, liver, spleen and central nervous system. In Europe, ALL has an estimated prevalence of 1.28 persons per 100,000 people.1 Among both children and adults, the most common subtype of ALL is B-ALL.1 B-ALL begins in immature cells that would normally develop into B-cell lymphocytes, which are white blood cells that grow in bone marrow.2,3 B-ALL is the most common type of ALL, constituting approximately 75% of cases in adults.4
About BLINCYTO® (blinatumomab)
BLINCYTO is the first globally approved Bispecific T-cell Engager (BiTE®) immuno-oncology therapy that targets CD19 surface antigens on B cells. BiTE® molecules fight cancer by helping the body's immune system detect and target malignant cells by engaging T cells (a type of white blood cell capable of killing other cells perceived as threats) to cancer cells. By bringing T cells near cancer cells, the T cells can inject toxins and trigger cancer cell death (apoptosis). BiTE® immuno-oncology therapies are currently being investigated for their potential to treat a wide variety of cancers.
In the European Union (EU), BLINCYTO is indicated as monotherapy for the treatment of:
Adults with Philadelphia chromosome-negative CD19-positive relapsed or refractory B-ALL. Patients with Philadelphia chromosome-positive B-ALL should have failed treatment with at least two tyrosine kinase inhibitors (TKIs) and have no alternative treatment options.
Adults with Philadelphia chromosome-negative CD19-positive B-ALL in first or second complete remission with MRD greater than or equal to 0.1%.
Pediatric patients aged 1 month or older with Philadelphia chromosome-negative CD19-positive B-ALL which is refractory or in relapse after receiving at least two prior therapies or in relapse after receiving prior allogeneic hematopoietic stem cell transplantation.
Pediatric patients aged 1 month or older with high-risk first relapsed Philadelphia chromosome-negative CD19-positive B-ALL as part of the consolidation therapy.
Adult patients with newly diagnosed Philadelphia chromosome-negative CD19-positive B-ALL as part of consolidation therapy.
BLINCYTO was granted breakthrough therapy and Priority Review designations by the U.S. FDA and is approved in the U.S. for the treatment of:
Adult and pediatric patients one month or older with CD19-positive Philadelphia chromosome-negative B-ALL during the consolidation phase of multiphase therapy.
CD19-positive B-ALL in first or second complete remission with MRD greater than or equal to 0.1% in adults and pediatric patients one month or older.
Relapsed or refractory CD19-positive B-ALL in adults and pediatric patients one month or older.
EU SAFETY INFORMATION FOR BLINCYTO®
The safety profile of BLINCYTO in the Phase 3 E1910 study was consistent with the known safety profile for BLINCYTO.
See BLINCYTO® full Summary of Product Characteristics (SmPC) at
About BiTE® Technology
Bispecific T-cell Engager (BiTE®) technology is a targeted immuno-oncology platform that is designed to engage patient's own T cells to any tumor-specific antigen, activating the cytotoxic potential of T cells to eliminate detectable cancer. The BiTE® immuno-oncology platform has the potential to treat different tumor types through tumor-specific antigens. The BiTE® platform has a goal of leading to off-the-shelf solutions, which have the potential to make innovative T cell treatment available to all providers when their patients need it. Amgen is advancing multiple BiTE® molecules across a broad range of hematologic malignancies and solid tumors, further investigating BiTE® technology with the goal of enhancing patient experience and therapeutic potential. To learn more about BiTE® technology, visit .
About Amgen
Amgen discovers, develops, manufactures and delivers innovative medicines to help millions of patients in their fight against some of the world's toughest diseases. More than 40 years ago, Amgen helped to establish the biotechnology industry and remains on the cutting-edge of innovation, using technology and human genetic data to push beyond what's known today. Amgen is advancing a broad and deep pipeline that builds on its existing portfolio of medicines to treat cancer, heart disease, osteoporosis, inflammatory diseases and rare diseases.
In 2024, Amgen was named one of the "World's Most Innovative Companies" by Fast Company and one of "America's Best Large Employers" by Forbes, among other external recognitions. Amgen is one of the 30 companies that comprise the Dow Jones Industrial Average®, and it is also part of the Nasdaq-100 Index®, which includes the largest and most innovative non-financial companies listed on the Nasdaq Stock Market based on market capitalization.
For more information, visit Amgen.com and follow Amgen on X, LinkedIn, Instagram, YouTube and Threads.
Amgen Forward-Looking Statements
This news release contains forward-looking statements that are based on the current expectations and beliefs of Amgen. All statements, other than statements of historical fact, are statements that could be deemed forward-looking statements, including any statements on the outcome, benefits and synergies of collaborations, or potential collaborations, with any other company (including BeiGene, Ltd. or Kyowa Kirin Co., Ltd.), the performance of Otezla® (apremilast) (including anticipated Otezla sales growth and the timing of non-GAAP EPS accretion), our acquisitions of Teneobio, Inc., ChemoCentryx, Inc., or Horizon Therapeutics plc (including the prospective performance and outlook of Horizon's business, performance and opportunities, any potential strategic benefits, synergies or opportunities expected as a result of such acquisition, and any projected impacts from the Horizon acquisition on our acquisition-related expenses going forward), as well as estimates of revenues, operating margins, capital expenditures, cash, other financial metrics, expected legal, arbitration, political, regulatory or clinical results or practices, customer and prescriber patterns or practices, reimbursement activities and outcomes, effects of pandemics or other widespread health problems on our business, outcomes, progress, and other such estimates and results. Forward-looking statements involve significant risks and uncertainties, including those discussed below and more fully described in the Securities and Exchange Commission reports filed by Amgen, including our most recent annual report on Form 10-K and any subsequent periodic reports on Form 10-Q and current reports on Form 8-K. Unless otherwise noted, Amgen is providing this information as of the date of this news release and does not undertake any obligation to update any forward-looking statements contained in this document as a result of new information, future events or otherwise.
No forward-looking statement can be guaranteed and actual results may differ materially from those we project. Discovery or identification of new product candidates or development of new indications for existing products cannot be guaranteed and movement from concept to product is uncertain; consequently, there can be no guarantee that any particular product candidate or development of a new indication for an existing product will be successful and become a commercial product. Further, preclinical results do not guarantee safe and effective performance of product candidates in humans. The complexity of the human body cannot be perfectly, or sometimes, even adequately modeled by computer or cell culture systems or animal models. The length of time that it takes for us to complete clinical trials and obtain regulatory approval for product marketing has in the past varied and we expect similar variability in the future. Even when clinical trials are successful, regulatory authorities may question the sufficiency for approval of the trial endpoints we have selected. We develop product candidates internally and through licensing collaborations, partnerships and joint ventures. Product candidates that are derived from relationships may be subject to disputes between the parties or may prove to be not as effective or as safe as we may have believed at the time of entering into such relationship. Also, we or others could identify safety, side effects or manufacturing problems with our products, including our devices, after they are on the market.
Our results may be affected by our ability to successfully market both new and existing products domestically and internationally, clinical and regulatory developments involving current and future products, sales growth of recently launched products, competition from other products including biosimilars, difficulties or delays in manufacturing our products and global economic conditions. In addition, sales of our products are affected by pricing pressure, political and public scrutiny and reimbursement policies imposed by third-party payers, including governments, private insurance plans and managed care providers and may be affected by regulatory, clinical and guideline developments and domestic and international trends toward managed care and healthcare cost containment. Furthermore, our research, testing, pricing, marketing and other operations are subject to extensive regulation by domestic and foreign government regulatory authorities. Our business may be impacted by government investigations, litigation and product liability claims. In addition, our business may be impacted by the adoption of new tax legislation or exposure to additional tax liabilities. If we fail to meet the compliance obligations in the corporate integrity agreement between us and the U.S. government, we could become subject to significant sanctions. Further, while we routinely obtain patents for our products and technology, the protection offered by our patents and patent applications may be challenged, invalidated or circumvented by our competitors, or we may fail to prevail in present and future intellectual property litigation. We perform a substantial amount of our commercial manufacturing activities at a few key facilities, including in Puerto Rico, and also depend on third parties for a portion of our manufacturing activities, and limits on supply may constrain sales of certain of our current products and product candidate development. An outbreak of disease or similar public health threat, such as COVID-19, and the public and governmental effort to mitigate against the spread of such disease, could have a significant adverse effect on the supply of materials for our manufacturing activities, the distribution of our products, the commercialization of our product candidates, and our clinical trial operations, and any such events may have a material adverse effect on our product development, product sales, business and results of operations. We rely on collaborations with third parties for the development of some of our product candidates and for the commercialization and sales of some of our commercial products. In addition, we compete with other companies with respect to many of our marketed products as well as for the discovery and development of new products. Further, some raw materials, medical devices and component parts for our products are supplied by sole third-party suppliers. Certain of our distributors, customers and payers have substantial purchasing leverage in their dealings with us. The discovery of significant problems with a product similar to one of our products that implicate an entire class of products could have a material adverse effect on sales of the affected products and on our business and results of operations. Our efforts to collaborate with or acquire other companies, products or technology, and to integrate the operations of companies or to support the products or technology we have acquired, may not be successful. There can be no guarantee that we will be able to realize any of the strategic benefits, synergies or opportunities arising from the Horizon acquisition, and such benefits, synergies or opportunities may take longer to realize than expected. We may not be able to successfully integrate Horizon, and such integration may take longer, be more difficult or cost more than expected. A breakdown, cyberattack or information security breach of our information technology systems could compromise the confidentiality, integrity and availability of our systems and our data. Our stock price is volatile and may be affected by a number of events. Our business and operations may be negatively affected by the failure, or perceived failure, of achieving our environmental, social and governance objectives. The effects of global climate change and related natural disasters could negatively affect our business and operations. Global economic conditions may magnify certain risks that affect our business. Our business performance could affect or limit the ability of our Board of Directors to declare a dividend or our ability to pay a dividend or repurchase our common stock. We may not be able to access the capital and credit markets on terms that are favorable to us, or at all.
CONTACT: Amgen, Thousand Oaks
Elissa Snook, 609-251-1407 (media)
Justin Claeys, 805-313-9775 (investors)
Hoelzer, D, Bassan R, Dombret H, et al. et al. Ann Oncol. 2016;27(suppl 5):v69-v82.
Terwilliger T, Abdul-Hay M.. Blood Cancer J. doi:10.1038/bcj.2017.53.
American Cancer Society. What is Acute Lymphocytic Leukemia (ALL)? Available at: . Accessed on January 2, 2025.
Leukemia & Lymphoma Society. Acute Lymphoblastic Leukemia (ALL). Available at: . Accessed on January 2, 2025.
Logo -
WANT YOUR COMPANY'S NEWS FEATURED ON PRNEWSWIRE.COM?
440k+
Newsrooms &
Influencers
9k+
Digital Media
Outlets
270k+
Journalists
Opted In
GET STARTED
临床结果临床3期免疫疗法上市批准细胞疗法
100 项与 West Michigan Cancer Center, Inc. 相关的药物交易
登录后查看更多信息
100 项与 West Michigan Cancer Center, Inc. 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2025年06月30日管线快照
无数据报导
登录后保持更新
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
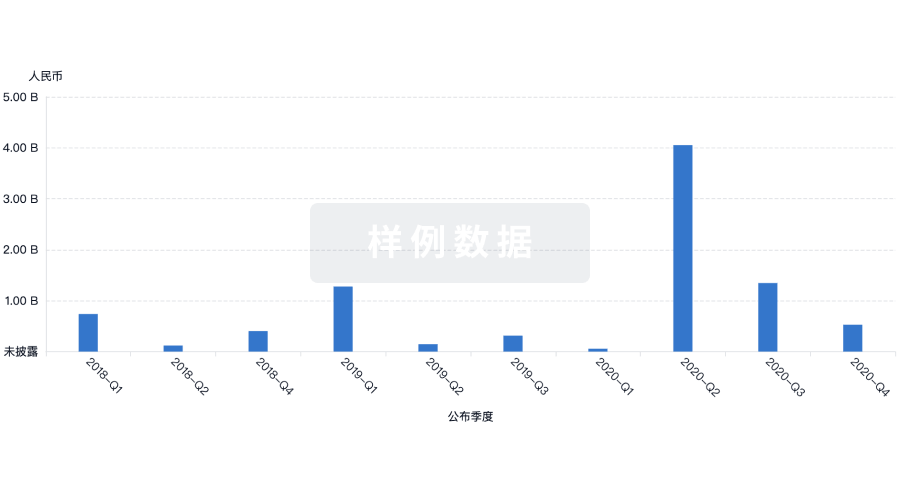
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
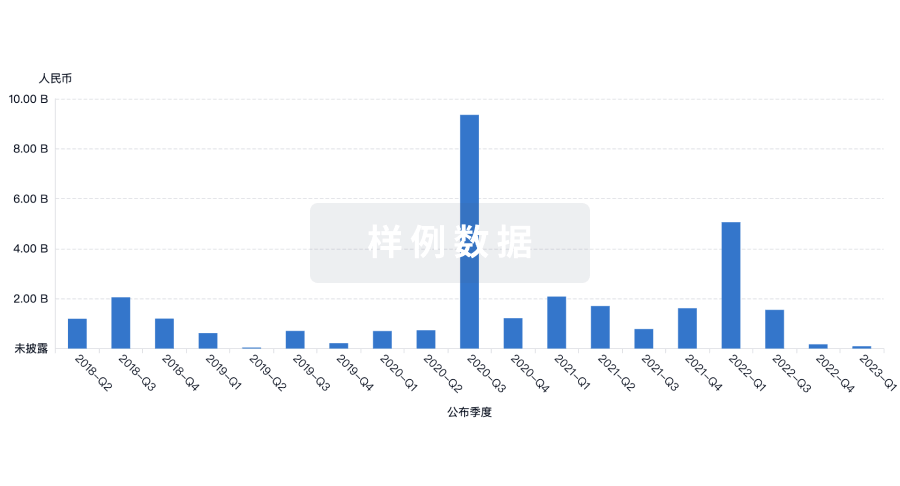
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
Eureka LS:
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用