预约演示
更新于:2025-10-16

Connolly Hospital Blanchardstown
更新于:2025-10-16
概览
关联
14
项与 Connolly Hospital Blanchardstown 相关的临床试验NCT07084077
Investigating the Effects of a Short Narratology Education Module on Empathy and Patient-centred Communication in Early-stage Medical Students: an Empirical Mixed-methods Pilot Study.
Effective communication is a fundamental skill in clinical medicine; however, traditional approaches often fail to equip learners with an ability to authentically and empathically engage with the complexities of real patients' experiences. Narratology education has been proposed as a pedagogical framework for augmenting empathy and patient-centred communication in medical students.
In April 2025, we undertook a mixed-methods pilot study to evaluate the impact of a one-week narratology education module on second-year undergraduate medical students at the Royal College of Surgeons in Ireland (RCSI), Dublin. The module involved close reading, group viewings, facilitated small-group workshops, and whole-group discussions in response to narrative works by Irish writers and storytellers, followed by written personal reflections. At the outset and conclusion of the module, each student undertook a clinical history with a simulated patient (SP) portraying early-stage dementia. SPs assessed each student's empathy and communication using the CARE Measure.
In April 2025, we undertook a mixed-methods pilot study to evaluate the impact of a one-week narratology education module on second-year undergraduate medical students at the Royal College of Surgeons in Ireland (RCSI), Dublin. The module involved close reading, group viewings, facilitated small-group workshops, and whole-group discussions in response to narrative works by Irish writers and storytellers, followed by written personal reflections. At the outset and conclusion of the module, each student undertook a clinical history with a simulated patient (SP) portraying early-stage dementia. SPs assessed each student's empathy and communication using the CARE Measure.
开始日期2025-04-02 |
NCT07088471
Cardiac Left Atrial Evaluation and Response in HFrEF With Sacubitril/Valsartan: The CLEAR Study.
Heart failure is an increasingly common condition that can have a significant impact on quality of life and reduce life expectancy. In recent decades, a number of drugs have been developed specifically for this condition. One such drug, called Sacubitril/valsartan (SV) has been shown to reduce hospitalizations and prolong life expectancy of patients with heart failure. It works by reversing some of the structural and functional changes to the heart that occur in heart failure. However, not all patients respond to the drug. Further research is needed to better understand the reasons for this and predict who will benefit most from the drug.
Left atrial strain is a relatively new measurement that can be obtained using ultrasound imaging of the heart, and it provides objective information about how one of the heart's four chambers is functioning. The investigators aim to assess the effect of SV therapy on left atrial strain in patients with heart failure. The investigator's objective is to understand whether abnormal left atrial strain or changes in left atrial strain help predict response to SV therapy.
Left atrial strain is a relatively new measurement that can be obtained using ultrasound imaging of the heart, and it provides objective information about how one of the heart's four chambers is functioning. The investigators aim to assess the effect of SV therapy on left atrial strain in patients with heart failure. The investigator's objective is to understand whether abnormal left atrial strain or changes in left atrial strain help predict response to SV therapy.
开始日期2024-11-01 |
NCT07102693
Left Atrial Strain Assessment in Ischemic Stroke Patients: a Retrospective Case-control Study - the ASSISTANT Study
This study is investigating a potential link between a novel measurement made on cardiac ultrasound and the risk of ischemic stroke in patients with a normal heart rhythm. The novel measurement is called left atrial strain. It uses speckle tracking echocardiography to measure the muscle function of the left atrium, one of the cardiac chambers. Investigators investigated whether patients with lower function of this chamber are at a higher risk of developing stroke from blood clots traveling to the brain. It is already known that patients with an irregular heart rhythm known as atrial fibrillation are at higher risk of these types of strokes. Investigators wanted to determine if there is a similar association in patients with normal heart rhythm but low left atrial strain.
开始日期2024-07-15 |
100 项与 Connolly Hospital Blanchardstown 相关的临床结果
登录后查看更多信息
0 项与 Connolly Hospital Blanchardstown 相关的专利(医药)
登录后查看更多信息
165
项与 Connolly Hospital Blanchardstown 相关的文献(医药)2025-09-01·CLINICAL JOURNAL OF SPORT MEDICINE
Return to Sport After Conservative Management of Midshaft Clavicle Fractures in Professional Jockeys
Article
作者: Kenny, Patrick ; Pugh, Jennifer ; Fahy, Stephen ; Ó Doinn, Tiarnán
Objective::
This study explores the functional recovery and rates return to play (RTP) of professional jockeys following midshaft clavicle fractures, which have been managed conservatively. The high incidence of these fractures in horse racing underscores the importance of evaluating nonsurgical recovery paths for effective RTP.
Design::
We used a retrospective cohort study to assess treatment outcomes.
Setting::
The research is set in the professional horse racing scene of Ireland.
Participants::
Sixteen professional Irish jockeys with conservatively managed midshaft clavicular fractures were examined. Jockeys who underwent surgery or were inactive at injury time were excluded.
Interventions::
The study involved no direct interventions.
Main Outcome Measures::
Recovery was assessed using the Quick Disabilities of the Arm, Shoulder, and Hand (QuickDASH) score and Patient-Reported Outcome Measures, alongside racing records to track RTP.
Results::
The all-male cohort had an average age of 27 years. Results showed an average 67.1-day absence from racing, with 94% returning to preinjury competition levels. Complications were minimal, and patient outcomes were positive, as indicated by a mean QuickDASH score of 2.58, suggesting minimal residual disability.
Conclusions::
Findings highlight the success of conservative management for midshaft clavicle fractures in professional jockeys, enabling them to return to prior competitive levels with few complications and excellent functional recovery.
2025-08-01·OSTEOPOROSIS INTERNATIONAL
Benefits of an advanced nurse practitioner led hip fracture clinic in an Irish Orthopaedic Trauma Service
Article
作者: Timon, Charlie ; Kenny, Paddy ; Gantley, Karen ; Cassar-Gheiti, Adrian Jesmond ; Coveney, Eamonn ; Kotze, Nicolaas
PURPOSE:
Ireland has one of the highest rates of hip fracture in the world. With a rapidly aging and increasing population, more stress will be put on services for hip fracture patients. Furthermore, accurate data collection with regard to Irish Hip Fracture Data standards needs to be collected to ensure optimal care for this vulnerable patient cohort. To address this, our unit has begun an advanced nurse practitioner (ANP) led hip fracture clinic. The purpose of this study is to assess the benefit of an ANP led hip fracture clinic in a single orthopaedic trauma unit.
METHODS:
Prospectively, over an 8-month period, all patients from a single Irish trauma hospital aged 60 years or older who suffered a hip fracture were seen post discharge at 30 days and again, but virtually, at 120 days in an ANP led clinic. X-rays, wound reviews, and hip exam are assessed initially while residential status, recent hospital re-admission, unplanned return to theatre, bone health, mobility assessment, and health questionnaire are assessed during both sessions. We wanted to assess the impact of our new clinic in terms of service provision and measuring outcomes.
RESULTS:
Then, 87 patients were seen in clinic at 30 days. Then, 64 had 120-day follow-up. Significant improvements were made with regard to patients pain scores, mobility, and wellbeing. All patients followed up had been prescribed bone protection by 120-day follow-up. Data were also collected with regard to surgical complications, patient residential status, and functional outcomes.
CONCLUSIONS:
ANP led hip fracture clinic provide safe, holistic hip fracture care. It addresses an urgent care gap in bone health management post hip fracture.
2025-08-01·IRISH JOURNAL OF MEDICAL SCIENCE
Referral patterns and patient characteristics observed during the first year of Ireland’s inaugural community hub diabetes service: a retrospective analysis
Article
作者: McDermott, John H ; Sreenan, Seamus ; Davenport, Colin ; Kyaw-Tun, Tommy ; De Jong, Katie
Abstract:
Background:
Enhanced Community Care (ECC) for type 2 diabetes mellitus (T2DM) in Ireland introduces episodic, community-based, consultant-led multidisciplinary care of diabetes that in turn supports the general practitioner (GP)-delivered chronic disease management programme (CDMP). The Dublin North West (DNW) hub, Ireland’s first fully operational ECC hub, began providing its diabetes service in March 2023.
Aims:
This study reviewed the first year of the DNW hub’s diabetes operations, focusing on referral patterns, patient demographics, clinical characteristics, and CDMP eligibility (only those people living with T2DM with a medical card or a GP visit card are eligible for CDMP for T2DM; otherwise, people living with T2DM must self-pay for GP-provided T2DM care).
Methods:
A retrospective analysis was conducted on patient charts and hospital databases for all referrals to the DNW hub from March 2023 to March 2024.
Results:
Out of 204 referrals, 67% were redirected from hospital waiting lists, 22% were direct GP referrals, and 11% were internal from other hub services. The average wait time from referral to first appointment was 8.6 weeks. Attendees were 44% female and 56% male, with an average age of 56.2 years. Notably, only 46% were eligible for CDMP. During the study period, the number of people living with T2DM waiting for diabetes appointments at Connolly Hospital decreased by 61%, with the average waiting time reduced from 11 to 5 months.
Conclusions:
The first year of activity in the DNW hub illustrates the potential of the ECC model to positively impact hospital waiting lists. Our data also suggests that eligibility to access the CDMP may merit expansion as part of the ongoing implementation of ECC in Ireland.
2
项与 Connolly Hospital Blanchardstown 相关的新闻(医药)2025-04-03
·美通社
司美格鲁肽
2.4mg
(商品名:诺和盈
®
)可使超重或肥胖且已确诊心血管疾病(
CVD
)但无糖尿病的患者总体心血管事件发生风险降低
22%
。
1
肥胖症可直接导致心血管疾病发病率、死亡率和卒中风险上升,其中约三分之二的与肥胖相关的死亡与心血管疾病相关。
2,3
此次分析基于
SELECT
研究的结果,
SELECT
是首个验证肥胖症治疗药物可改善心血管结局的试验。
4
北京
2025年4月3日
/美通社/ -- SELECT试验的最新二次分析结果显示,与安慰剂相比,司美格鲁肽2.4mg(诺和盈
®
)在超重或肥胖且已确诊心血管疾病但无糖尿病的患者中,可显著降低总体心血管事件负担。
1
这些数据结果在第74届美国心脏病学会科学年会暨博览会(ACC 2025,3月29日至31日在伊利诺伊州芝加哥市举行)上公布。这些结果为SELECT心血管结局试验的现有证据提供了补充,并进一步提供了在首次发生心血管事件后使用司美格鲁肽2.4mg获益的相关数据。
1
这些研究结果具有重要意义。大多数心血管结局试验的主要分析通常仅评估首次心血管事件,而肥胖症患者是心血管疾病高风险群体,可能会在一定时间内经历多次心血管事件。因此,仅分析首次心血管事件无法完全反映肥胖症对健康的长期负担及患者面临的损伤或过早死亡风险。
1,5
在SELECT试验的此项预设二次分析中,与安慰剂相比,司美格鲁肽2.4mg可使主要不良心血管事件(MACE)的首次发生风险降低20%(HR: 0.80; 95% CI 0.73–0.87; P<0.001),并使总体(首次及后续)心血管事件发生风险降低22%(MR: 0.78; 95% CI 0.70–0.86; P<0.001)。[*]
1
此外,与安慰剂相比,司美格鲁肽2.4mg可使总体心脏病发作风险降低31%(MR 0.69; 95% CI 0.58–0.82; P<0.001),总体冠状动脉血管重建风险降低26%(MR: 0.74; 95% CI 0.65–0.84; P<0.001),共同推动了总体心血管事件风险下降。
1
此项分析共纳入17,604名受试者,平均随访时间39.8个月,共计发生3,031例心血管事件,其中,1,947例(64%)为首次事件,1,084例(36%)为后续事件。
1
在首次心血管事件中,冠状动脉血管重建的比例为27.2%,心脏病发作的比例26.2%;而在后续心血管事件中,冠状动脉血管重建的比例为72.9%,心脏病发作为10.3%。
1
总体而言,SELECT研究的最新次要分析结果表明,在超重或肥胖且已确诊心血管疾病但无糖尿病的患者中,司美格鲁肽2.4mg显著降低了首次、后续及总体心血管事件风险。
1
这进一步印证了司美格鲁肽2.4mg在已证实的健康获益外,还具有降低心血管风险的潜力。
4,6-16
关于肥胖症与心血管疾病
肥胖症是一种慢性疾病,可直接导致心血管发病率、死亡率及住院风险增加,
17,18
肥胖相关的死亡有三分之二与心血管疾病相关。
2,3
肥胖还与高血压、慢性肾病和炎症等多种风险因素有关。
19
对于已患有心血管疾病的超重或肥胖患者而言,及时的干预至关重要,以降低包括心脏病发作和卒中在内的MACE的残余风险。
5
尽管治疗手段不断进步,但针对肥胖相关疾病的有效治疗方案仍存在巨大的未被满足的需求。
20
关于
SELECT
研究
SELECT是一项国际性随机、双盲、平行分组、安慰剂对照试验,旨在评估司美格鲁肽2.4mg和安慰剂结合标准治疗在超重或肥胖且已确诊心血管疾病但无糖尿病病史的人群中预防MACE的有效性。
9
被纳入试验的人群年龄≥45岁、BMI≥27 kg/m
2
,最长随访时间达到5年。
9
SELECT试验的主要目标是证实与安慰剂相比,司美格鲁肽2.4mg在降低3点MACE(包括心血管死亡、非致死性心脏病发作(心肌梗死)或非致死性卒中)发生率方面的优效性。
4
关键的次要目标是比较司美格鲁肽2.4mg相较于安慰剂在死亡率、心力衰竭、心血管风险因素(包括糖代谢、体重和肾功能)方面的疗效
4
。
SELECT研究于2018年启动,共招募了17,604名成人受试者,在41个国家和地区的800多个研究中心开展了研究。
SELECT研究的主要研究结果已于2023年11月在美国心脏协会科学年会上公布,并发表于《新英格兰医学杂志》(NEJM)。
4
迄今为止,SELECT研究已衍生出多个数据集和次要分析,相关研究结果已在多个心血管、肾脏及代谢疾病相关的科学大会上发布,相关成果也已发表于众多权威医学期刊
4,10-16
。
参考文献
1. Lincoff, MA, Colhoun HM, Emerson S. (2025) Effect of the GLP-1 receptor agonist semaglutide on total cardiovascular events in patients with cardiovascular disease and overweight or obesity but no diabetes in the SELECT trial. Presented at ACC 2025, Chicago, United States.
2. Collaborators GBDO, Afshin A, Forouzanfar MH, et al. Health Effects of Overweight and Obesity in 195 Countries over 25 Years. N Engl J Med. 2017; 377:13-27.
3. Martin-Timon I, Sevillano-Collantes C, Segura-Galindo A, et al. Type 2 diabetes and cardiovascular disease: Have all risk factors the same strength? World J Diabetes. 2014; 5:444-470.
4. Lincoff MA, Brown-Frandson K, Colhoun HM, et al. Semaglutide and Cardiovascular Outcomes in Obesity without Diabetes. N Engl J Med. 2023;389:2221-2232.
5. Koskinas KC, Van Craenenbroeck EM, Antoniades C et al. Obesity and cardiovascular disease: an ESC clinical consensus statement. European Heart Journal. 2024;45(38):4063–4098.
6. Kosiborod MN, Abildstrom SZ, Borlaug BA, et al. Semaglutide in Patients with Heart Failure with Preserved Ejection Fraction and Obesity. N Engl J Med. 2023; 389:1069-1084.
7. Kosiborod MN, Petrie MC, Borlaug BA, et al. Semaglutide in Patients with Obesity-Related Heart Failure and Type 2 Diabetes. N Engl J Med. 2024; 390:1394-1407.
8. Bliddal H, Bays H, Czernichow S, et al. Once-weekly semaglutide in people with obesity and knee osteoarthritis. N J Engl J Med. 2024:391(17):1573-1583.
9. Lingvay I, Brown-Frandsen K, Colhoun HM, et al. Semaglutide for cardiovascular event reduction in people with overweight or obesity: SELECT study baseline characteristics. Obesity (Silver Spring). 2023; 31:111-122.
10. Deanfield JE, Verma S, Scirica BM, et al. Semaglutide and cardiovascular outcomes in patients with obesity and prevalent heart failure: a prespecified analysis of the SELECT trial. Lancet. 2024;404(10458).
11. Ryan DH, Lingvay I, Deanfield JE, et al. Long-term weight loss effects of semaglutide in obesity without diabetes in the SELECT trial. Nat Med. 2024;30:2049–2057.
12. Scirica BM, Lincoff AM, Lingvay I, et al. The effect of semaglutide on mortality and COVID-19–related deaths: an analysis from the SELECT trial. J Am Coll Cardiol. 2024;84(10):1350–1359.
13. Kahn SE, Deanfield JE, Jeppesen OK, et al. Effect of semaglutide on regression and progression of glycemia in people with overweight or obesity but without diabetes in the SELECT trial. Diabetes Care. 2024;47(8):1350–1359.
14. Kosiborod MN, Deanfield JE, Pratley RE, et al. Semaglutide versus placebo in patients with heart failure and mildly reduced or preserved ejection fraction: a pooled analysis of the SELECT, FLOW, STEP-HFpEF, and STEP-HFpEF DM randomised trials. Lancet. 2024;404(10456):949-961.
15. Colhoun HM, Lingvay I, Brown PM, et al. Long-term kidney outcomes of semaglutide in obesity and cardiovascular disease in the SELECT trial. Nat Med. 2024;30:2058–2066.
16. Nicholls SJ, Ryan DH, Deanfield JE, et al. Semaglutide reduces hospital admissions in patients with obesity or overweight and established CVD. Presented at ObesityWeek® 2024, San Antonio, USA, November 3, 2024.
17. Haidar A, Horwich T. Obesity, Cardiorespiratory Fitness, and Cardiovascular Disease. Curr Cardiol Rep. 2023;25:1565–1571.
18. Zizza C et al. Length of Hospital Stays Among Obese Individuals. Am J Public Health. 2004;94:1587–1591; 3.
19. Powell-Wiley TM, Poirier P, Burke LE, et al. Obesity and Cardiovascular Disease: A Scientific Statement From the American Heart Association. Circulation. 2021;143:e984-e1010.
20. Rigopoulos AG, Bakogiannis C, de Vecchis R, et al. Acute heart failure: An unmet medical need. Herz. 2019; 44:53-55.
[*]研究所定义的"扩大的MACE综合结局"包括心血管死亡、心脏病发作、卒中、冠状动脉血管重建或因不稳定型心绞痛住院。
关于诺和诺德
诺和诺德公司成立于1923年,是一家全球领先的生物制药公司
,总部位于丹麦。立足于在糖尿病领域的百年传承,我们的使命是驱动改变,携手战胜严重慢性疾病。为达成这一目标,我们引领科研突破,扩大公司药物可及性,并致力于预防及最终治愈疾病。诺和诺德在全球80个国家和地区拥有约7.63万名员工,向全球约170个国家和地区提供产品和服务。诺和诺德中国官方网站:
http:\/\/www.novonordisk.com.cn
免责声明
本新闻稿仅用于传递相关前沿科学信息和市场资讯。本新闻稿不构成对任何药物或治疗方案的推荐、推广或广告。读者不应参考、依据或依赖本新闻稿的任何内容,作出购买、使用任何药物或治疗方案的任何决定。如读者有药物或治疗方面的问题,请咨询医疗卫生专业人士。
本新闻稿含有关于诺和诺德产品的前瞻性信息,包括但不限于其潜在益处、研发进展、商业化进程、市场竞争情况等。这些信息涉及到重大的不确定性。仅依赖此信息进行解读、判断和推测可能导致实际结果与此信息所表达或暗示的结果有实质性的差异。请读者充分知悉上述不确定性以及由此可能导致的风险。
本新闻稿中所含信息的原始信息来自于诺和诺德,该等信息的有效性仅截至其发布日期。诺和诺德无义务就由于新信息、未来事件、事件进展或其他原因产生的任何变化对相关信息进行更新。对于因使用、依赖本新闻稿中包含的任何信息或任何信息遗漏而直接或间接产生的任何损失,诺和诺德不承担任何责任。
在转发、使用或以其它方式处理本新闻稿中的信息前,相关行为人应负责确保其行为符合所有相关国家或司法管辖区的任何适用法律、法规和监管要求。任何由于引用、转载、编辑或通过其它方式使用本新闻稿中所含信息而产生的一切直接或间接的后果,均由相关行为人自行承担全部责任,诺和诺德不对此承担任何责任。建议相关行为人在转发、使用或以其它方式处理本新闻稿中的信息前审慎评估风险,必要时请咨询专业法律人士的意见。
特此声明。
临床结果临床研究
2024-11-03
Results from Novo Nordisk, presented at ObesityWeek®, showed treatment with semaglutide injection 2.4 mg resulted in significant reductions in hospital admissions as well as overall time spent in the hospital1
Cardiovascular disease represents the leading cause of death globally,2 and adults with obesity are at a higher risk of developing cardiovascular disease3
The analysis is based on SELECT, a large cardiovascular outcomes trial that evaluated the effect of semaglutide 2.4 mg on the risk of MACE (heart attack, stroke, or death) in adults with overweight or obesity and known heart disease4
PLAINSBORO, N.J., Nov. 3, 2024 /PRNewswire/ -- Today, Novo Nordisk presented an exploratory post hoc analysis from the SELECT phase 3 cardiovascular outcomes trial that showed semaglutide 2.4 mg significantly reduced hospital admissions and overall length of hospital stay for adults with obesity or overweight with established cardiovascular disease (CVD) and without diabetes.1 The results were presented during an oral session at the annual ObesityWeek® conference and provide further insights based on data from SELECT– a large cardiovascular outcomes trial that evaluated the effect of semaglutide 2.4 mg on the risk of MACE (heart attack, stroke, or death) in this population.
CVD covers a wide range of conditions that, when combined, represent the leading cause of death globally and are associated with substantial healthcare costs.2,5 Obesity directly increases the risk of CVD, including heart attack and stroke, while also contributing to the progression of other cardiovascular (CV) risk factors including elevated blood pressure and cholesterol.3,5 Two in three patients with overweight or obesity die from CVD.6
"People with obesity or overweight with established cardiovascular disease (CVD) and without diabetes are more likely to be admitted to the hospital for events like heart attack or stroke, contributing to reduced patient well-being, higher use of healthcare resources, and disease burden," said Dr. Steven E. Kahn, M.D., Ch.B., Division of Metabolism, Endocrinology and Nutrition, Department of Medicine, VA Puget Sound Health Care System and University of Washington, Seattle. "In the SELECT trial, this cohort of patients had a high rate of hospital admissions, but for those given once-weekly semaglutide 2.4 mg, we observed significant reductions in hospital admissions and overall time they spent in the hospital. We are pleased to have this analysis that further examines the effects of semaglutide."
According to this SELECT analysis, a lower percentage of patients taking semaglutide 2.4 mg experienced a first hospital admission for any indication versus placebo (33.4 vs 36.7%, hazard ratio [HR] 0.89 [0.84, 0.93], p<0.0001) and for serious adverse events (30.3 vs 33.4%, HR 0.88 [0.84, 0.93], p<0.0001).1 In addition, the number of total hospitalizations was lower in the semaglutide 2.4 mg group versus placebo for all indications (18.3 vs 20.4 admissions per 100 patient years, HR 0.90 [0.85, 0.95], p=0.0002) and for serious adverse events (15.2 vs 17.1 admissions per 100 patient years, HR 0.89 [0.84, 0.94], p<0.0001).1 The number of days hospitalized per 100 patient years was lower in the semaglutide 2.4 mg group for all hospitalizations (157.2 vs 176.2 days, risk ratio [RR] 0.89 [0.82, 0.98], p=0.01) and for hospitalizations related to serious adverse events (137.6 vs 153.9 days, RR 0.89 [0.81, 0.98], p=0.02).1 The widths of the confidence intervals have not been adjusted for multiplicity and therefore the confidence intervals and p-values should not be used to infer definitive treatment effects for this exploratory post hoc analysis. Semaglutide is not approved in the U.S. for hospitalization-related outcomes.
Safety data collection in the SELECT trial was limited to serious adverse events (including death), adverse events leading to discontinuation, and adverse events of special interest.4,7 In the SELECT trial, the proportion of patients for whom serious adverse events were reported was 33.4% in patients randomized to semaglutide 2.4 mg and 36.4% of patients receiving placebo.4 Sixteen percent (16%) of semaglutide 2.4 mg-treated patients and 8% of placebo-treated patients, respectively, discontinued study drug due to an adverse event.7 The most common adverse event leading to discontinuation was gastrointestinal disorders, occurring in 10% of patients in the semaglutide 2.4 mg group and 2% in the placebo group.4
"We are pleased to continue building on the strong foundation of SELECT trial data that demonstrated the effectiveness of semaglutide 2.4 mg in lowering CV risk in patients with obesity and established cardiovascular disease, and to continue our ongoing commitment to improve the lives of people facing serious chronic diseases," said Michelle Skinner, PharmD, Vice President, Medical Affairs at Novo Nordisk. "This new SELECT analysis represents another step forward, exploring how semaglutide 2.4 mg impacted repeat hospitalizations and prolonged hospital stays, which are two pressing issues in terms of healthcare cost and quality."
About the SELECT trial
SELECT (Semaglutide Effects on Cardiovascular Outcomes in People with Overweight or Obesity) was a multicenter, randomized, double-blind, placebo-controlled, event-driven superiority trial designed to evaluate the efficacy of semaglutide 2.4 mg versus placebo as an adjunct to cardiovascular standard of care for reducing the risk of major adverse cardiovascular events in people with established CVD with overweight or obesity with no prior history of diabetes.4
The trial, initiated in 2018, enrolled 17,604 adults and was conducted in 41 countries at more than 800 investigator sites.4
About Novo Nordisk
Novo Nordisk is a leading global healthcare company that's been making innovative medicines to help people with diabetes lead longer, healthier lives for more than 100 years. This heritage has given us experience and capabilities that also enable us to drive change to help people defeat other serious chronic diseases such as obesity, rare blood, and endocrine disorders. We remain steadfast in our conviction that the formula for lasting success is to stay focused, think long-term, and do business in a financially, socially, and environmentally responsible way. With U.S. headquarters in New Jersey and commercial, production, and research facilities in seven states plus Washington DC, Novo Nordisk employs approximately 8,000 people throughout the country. For more information, visit novonordisk-us.com, Facebook, Instagram, X, LinkedIn, and YouTube.
References:
Nicholls SJ, Ryan D, Deanfield J, et al. Semaglutide Reduces Hospital Admissions in Patients with Obesity or Overweight and Established CVD. Presented at ObesityWeek® 2024, Nov 3, 2024.
World Health Organization. Cardiovascular diseases (cvds). Accessed October 31, 2024. (cvds).
Powell-Wiley TM, Poirier P, Burke LE, et al. Obesity and cardiovascular disease: a scientific statement from the American Heart Association. Circulation. 2021;143(21):e984-e1010. doi:10.1161/CIR.0000000000000973.
Lincoff MA, Brown-Frandson K, Colhoun HM, et al. Semaglutide and cardiovascular outcomes in obesity without diabetes. N Engl J Med. 2023;389:2221-2232.
Reiter-Brennan C, Dzaye O, Davis D, et al. Comprehensive care models for cardiometabolic disease. Curr Cardiol Rep. 2021;23(3):22. Published 2021 Feb 24. doi:10.1007/s11886-021-01450-1.
The GBD 2015 Obesity Collaborators. Health effects of overweight and obesity in 195 countries over 25 years. N Engl J Med. 2017;377(1):13-27. doi:10.1056/nejmoa1614362.
Wegovy® (semaglutide) injection 2.4 mg Prescribing Information. Plainsboro, NJ: Novo Nordisk Inc.
© 2024 Novo Nordisk All rights reserved. US24SEMO01281 November 2024
SOURCE NOVO NORDISK INC.
WANT YOUR COMPANY'S NEWS FEATURED ON PRNEWSWIRE.COM?
440k+
Newsrooms &
Influencers
9k+
Digital Media
Outlets
270k+
Journalists
Opted In
GET STARTED

临床结果临床3期AHA会议
100 项与 Connolly Hospital Blanchardstown 相关的药物交易
登录后查看更多信息
100 项与 Connolly Hospital Blanchardstown 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2025年11月05日管线快照
无数据报导
登录后保持更新
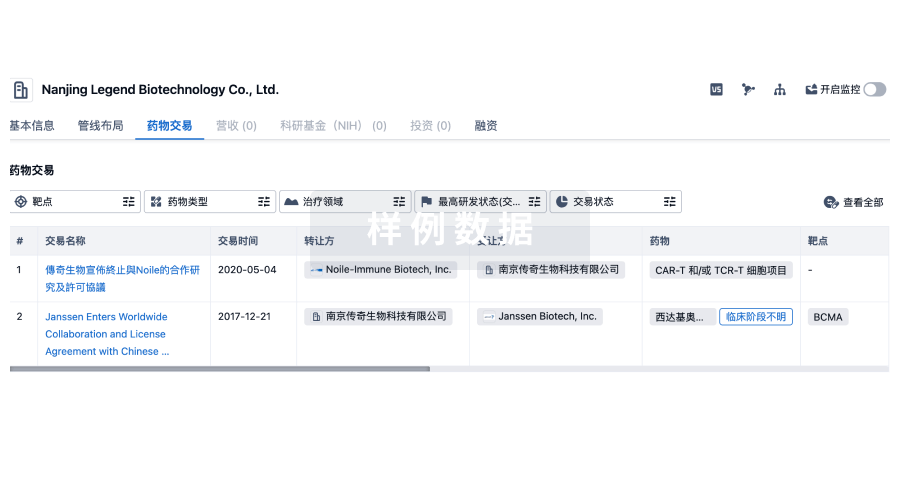
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
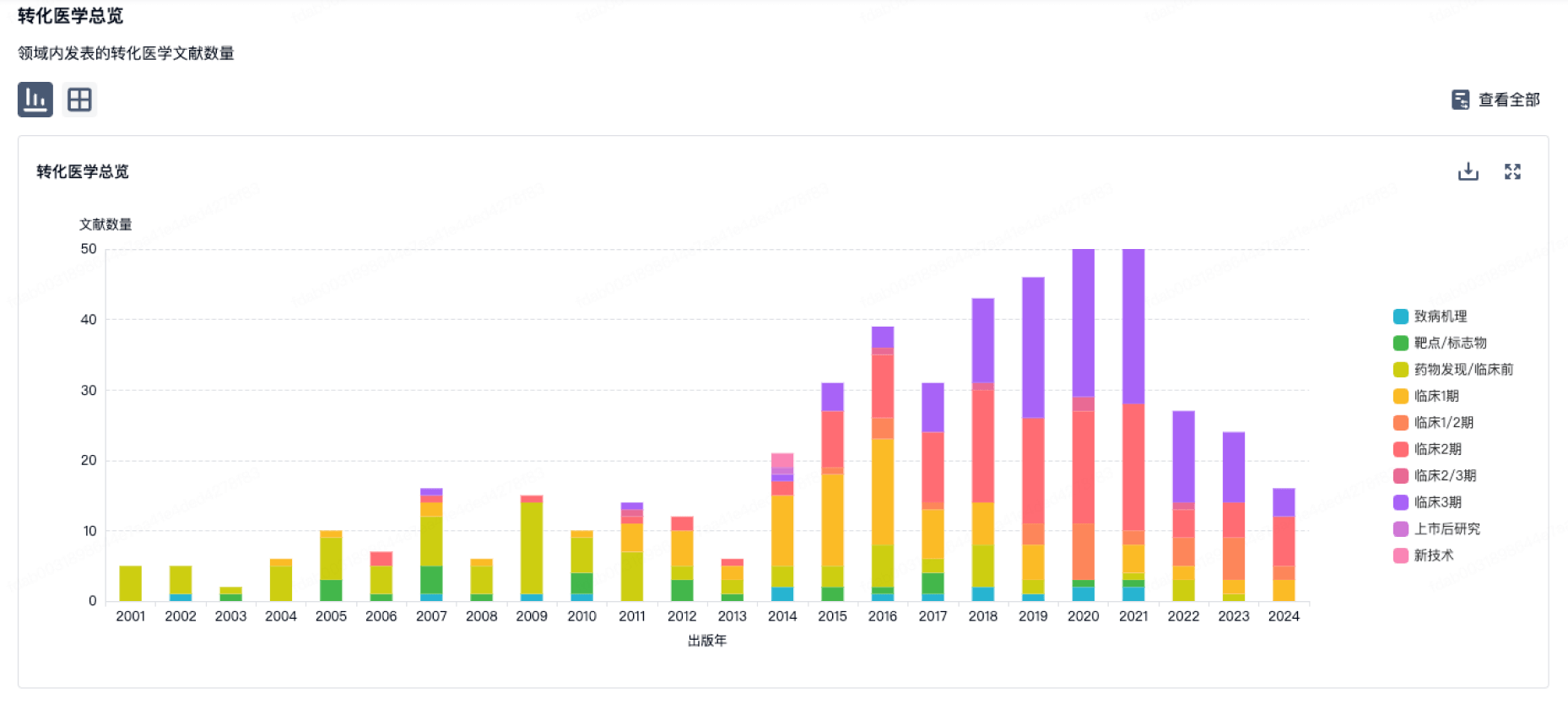
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
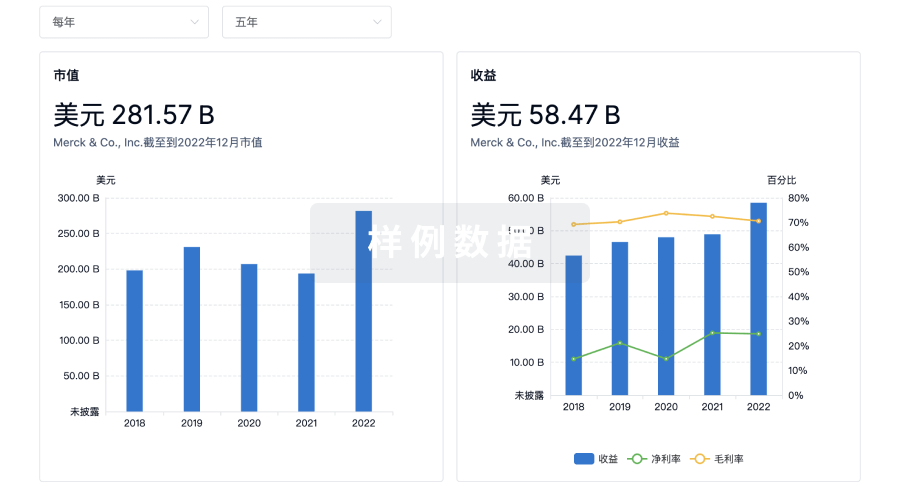
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
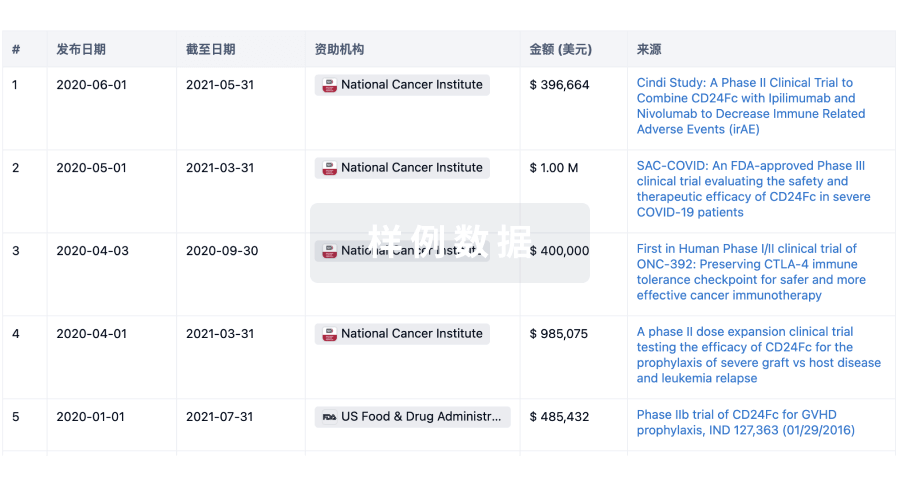
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用