预约演示
更新于:2025-07-06

Tokyo Dental College
更新于:2025-07-06
概览
标签
神经系统疾病
其他疾病
内分泌与代谢疾病
小分子化药
疾病领域得分
一眼洞穿机构专注的疾病领域
暂无数据
技术平台
公司药物应用最多的技术
暂无数据
靶点
公司最常开发的靶点
暂无数据
| 排名前五的药物类型 | 数量 |
|---|---|
| 小分子化药 | 1 |
| 排名前五的靶点 | 数量 |
|---|---|
| TRPA1(瞬时受体电位离子通道亚基1) | 1 |
关联
1
项与 Tokyo Dental College 相关的药物US20240041733
专利挖掘靶点 |
作用机制- |
非在研适应症- |
最高研发阶段药物发现 |
首次获批国家/地区- |
首次获批日期- |
18
项与 Tokyo Dental College 相关的临床试验JPRN-UMIN000051907
Visual function of eyes implanted with non-diffractive extended depth of focus intraocular lens - Visual function of non-diffractive EDOF IOL
开始日期2023-07-25 |
申办/合作机构 |
JPRN-UMIN000051512
Comparison of the preventive effect of ondansetron and dexamethasone on nausea and vomiting after orthognathic surgery between remimazolam and propofol anesthesia. - Comparison of the preventive effect of ondansetron and dexamethasone on nausea and vomiting after orthognathic surgery between remimazolam and propofol anesthesia.
开始日期2023-07-04 |
申办/合作机构 |
JPRN-UMIN000051727
Elucidation of gene polymorphisms that contribute to nausea and vomiting after administration of ondansetron - Elucidation of gene polymorphisms that contribute to nausea and vomiting after administration of ondansetron
开始日期2023-05-03 |
申办/合作机构 |
100 项与 Tokyo Dental College 相关的临床结果
登录后查看更多信息
0 项与 Tokyo Dental College 相关的专利(医药)
登录后查看更多信息
4,371
项与 Tokyo Dental College 相关的文献(医药)2025-12-31·Journal of Oral Microbiology
Patients with periodontitis exhibit persistent dysbiosis of the gut microbiota and distinct serum metabolome
Article
作者: Miura, Nobuaki ; Imamura, Kentaro ; Okuda, Shujiro ; Takahashi, Naoki ; Ono, Shigeru ; Yamazaki, Kazuhisa ; Sasaki, Nobuo ; Miyauchi, Eiji ; Mizuno, Kentaro ; Kikuchi, Jun ; Tsuboi, Yuuri ; Yamazaki, Kyoko ; Morita, Hidetoshi ; Ohno, Hiroshi ; Nakajima, Takako
Objectives:
Animal studies suggest that periodontopathic bacteria induce gut dysbiosis and related pathology, possibly connecting periodontitis to non-oral diseases. However, the effects on the gut ecosystem in periodontitis patients are not fully understood.
Methods:
We conducted a comprehensive analysis of the salivary and gut microbiota using 16S rRNA sequencing in periodontitis patients before and after treatment, comparing them to healthy participants. Serum metabolites were also analyzed.
Results:
Periodontitis patients showed high alpha diversity in both salivary and gut microbiota with a strong correlation. Significant differences were also observed in the gut microbiota composition between patients before treatment and healthy participants, irrespective of the ectopic colonization of periodontitis-associated bacteria in the gut. Co-abundance group analysis demonstrated that the gut microbiota of healthy participants was enriched with short-chain fatty acid producers. Changes in the gut microbiota coincided with alterations in the serum metabolite profile. While periodontal therapy improved salivary microbiota, it did not significantly affect gut microbiota.
Conclusions:
Gut dysbiosis of periodontitis patients may impact systemic metabolite profiles. Given that periodontal therapy alone did not substantially improve the gut microbiota, adjunctive strategies targeting the gut microbiome may be effective in reducing the risk of periodontitis-associated diseases.
2025-08-01·INTERNATIONAL JOURNAL OF SURGICAL PATHOLOGY
Ectopic Salivary Duct Cyst in the Median Mandible: A Case Report with Radiological, Immunohistochemical and Genetic Studies
Article
作者: Watanabe, Joji ; Ide, Fumio ; Ito, Yumi ; Kikuchi, Kentaro ; Yamamoto, Hidetaka ; Muramatsu, Takashi
Median mandibular cyst is defined as an odontogenic cyst in a rare midline location. In spite of this definition, there have been two reports of a peculiar lesion, so-called “ciliated” median mandibular cyst associated with vital teeth, the origin of which cannot be explained in terms of odontogenic epithelium multipotentiality. We describe a thorough profile of an additional example. On the basis of the cone-beam computed tomography images of a wide open cavity in the midline of the lingual bone, the surgical findings of no association with the vital incisor roots, the immunophenotypes of the excretory duct epithelium and the absence of oncogenic mutations, the present “ciliated” median mandibular cyst associated with vital teeth may be an artifact caused by impingement of the lingual bone due to pedicled extension from an extra-glandular salivary duct cyst in the anterior mouth floor. Awareness of this ectopic presentation is of clinical importance for the differential diagnosis of radiolucencies in the median mandible.
2025-07-01·Oral Surgery Oral Medicine Oral Pathology Oral Radiology
Misleading ameloblastomatoid and squamobasaloid rests growing within the nerve: a 100-year-old concept revisited
Article
作者: Ide, Fumio ; Sakamoto, Shinnichi ; Kikuchi, Kentaro ; Nishimura, Michiko ; Miyazaki, Yuji ; Muramatsu, Takashi
OBJECTIVE:
The jawbone contains a large number of unnamed epithelial rests that are remnants of the tooth-forming process. One of these uniquely extends naturally along neurovascular bundles, and was originally described at least 100 years ago as "epithelial nests in the bone nerve canal." As this concept has been forgotten in the years since then, any association of epithelial rests with the nerve has remained diagnostically enigmatic.
STUDY DESIGN AND RESULTS:
In jawbone sections, we have found common resting squamobasaloid and rare proliferating ameloblastic nests within neurovascular bundles. The latter type of large organoid follicle, when viewed in isolation, closely resembles ameloblastoma, but notable immunohistochemical differences are evident, suggesting classification as ameloblastomatoid hyperplasia.
CONCLUSIONS:
Recognition of challenging intraneural epithelial rests in marrow spaces within cancellous bone as a normal microanatomic finding may help prevent diagnostic confusion and misdiagnosis. (Oral Surg Oral Med Oral Pathol Oral Radiol YEAR;VOL:page range).
100 项与 Tokyo Dental College 相关的药物交易
登录后查看更多信息
100 项与 Tokyo Dental College 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2025年08月20日管线快照
管线布局中药物为当前组织机构及其子机构作为药物机构进行统计,早期临床1期并入临床1期,临床1/2期并入临床2期,临床2/3期并入临床3期
药物发现
1
1
其他
登录后查看更多信息
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
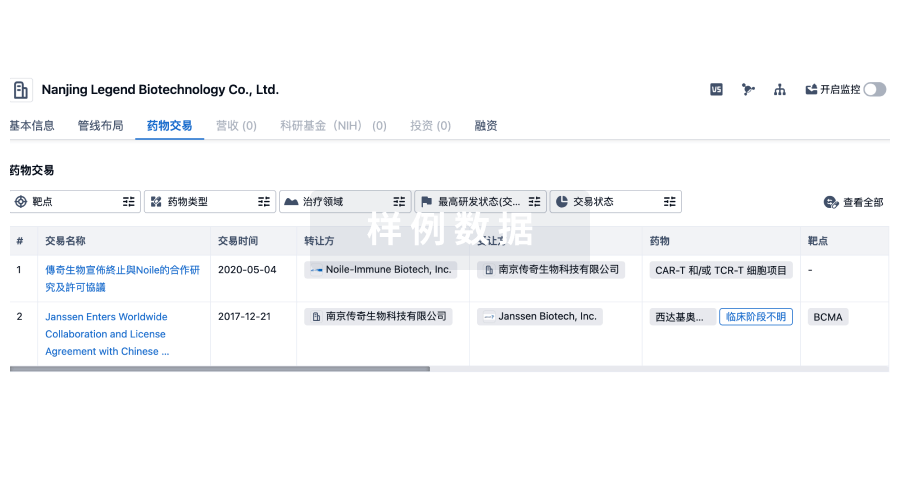
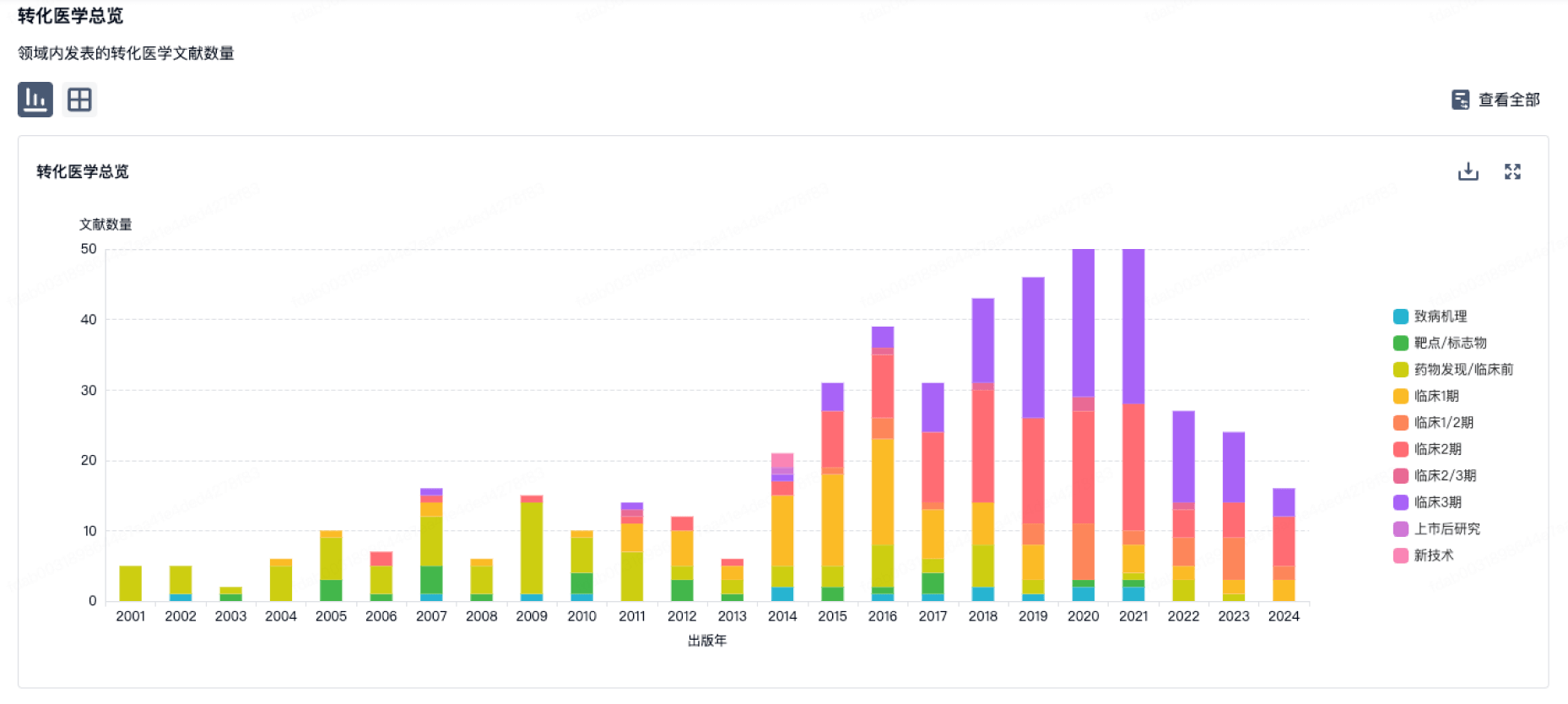
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
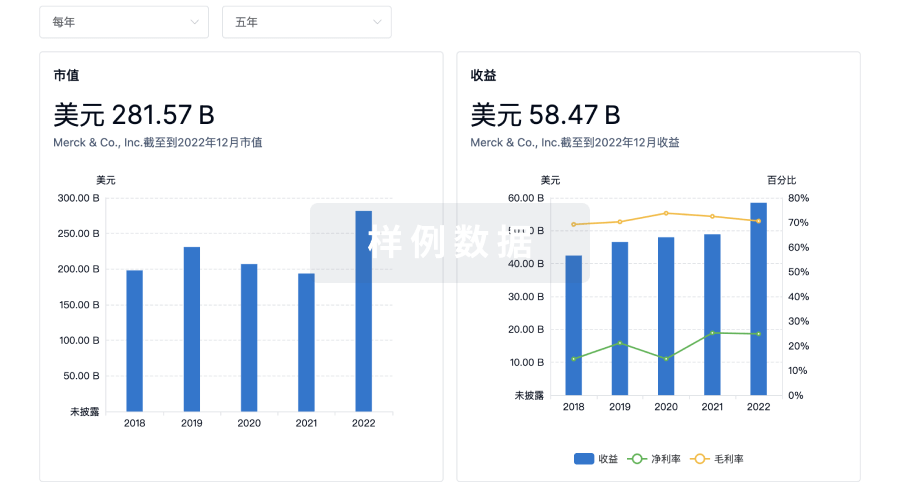
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
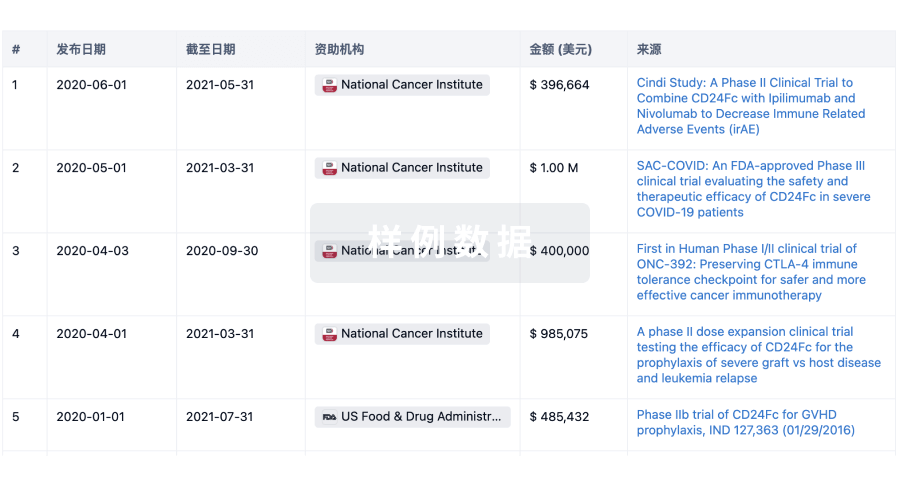
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
Eureka LS:
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用