预约演示
更新于:2025-10-30
Kidney(Esperion Therapeutics)
更新于:2025-10-30
概要
基本信息
非在研机构- |
权益机构- |
最高研发阶段临床前 |
首次获批日期- |
最高研发阶段(中国)- |
特殊审评- |
关联
100 项与 Kidney(Esperion Therapeutics) 相关的临床结果
登录后查看更多信息
100 项与 Kidney(Esperion Therapeutics) 相关的转化医学
登录后查看更多信息
100 项与 Kidney(Esperion Therapeutics) 相关的专利(医药)
登录后查看更多信息
18
项与 Kidney(Esperion Therapeutics) 相关的文献(医药)2025-05-01·JOURNAL OF ETHNOPHARMACOLOGY
Iridoid glycosides in kidney-tonifying Chinese medicinal herbs: Mechanisms and implications for Alzheimer's disease therapy
Review
作者: Zheng, Lan ; Ding, Minrui ; Zhang, Mengxue ; Hu, Bing ; An, Hongmei ; Qu, Yanjie
ETHNOPHARMACOLOGICAL RELEVANCE:
Alzheimer's disease (AD) is an incurable and irreversible type of dementia. Existing drugs cannot meet clinical needs; thus, developing new treatments is necessary. Traditional Chinese medicine (TCM) has been used in the prevention and treatment of AD. TCM holds the theory that "the kidney support brain function" and believes that dementia can be addressed from a kidney-based perspective. Kidney-tonifying herbs are a class of medicines that have the effect of tonifying the kidney and benefiting the brain. Some of these herbs have been shown to have anti-AD effects. Iridoid glycosides (IGs), which are important components of kidney-tonifying herbs, may have the potential to prevent and treat AD. However, their effects on AD have not yet been reviewed.
AIM OF THE REVIEW:
This literature review provides a comprehensive summary of the potential of IGs in the prevention and treatment of AD. It also sets the foundation for future studies that will make the use of such drugs in clinical practice possible.
MATERIAL AND METHODS:
Kidney-tonifying Chinese herbs were selected with reference to the Chinese Pharmacopoeia (2020 edition) and the textbook of Chinese Materia Medica (5th edition). Literature survey was conducted using PubMed, Web of Science, Google Scholar, and CNKI, with "Alzheimer's disease," "kidney-tonifying Chinese medicinal herbs," and "Iridoid Glycosides" as the primary keywords.
RESULTS:
Kidney-tonifying herbal IGs include loganin, morroniside, verbenalin, cornuside, catalpol, rehmannioside A, geniposidic acid, and aucubin. These IGs have shown multiple pharmacological effects, including anti-AD effects. The effective mechanisms of IGs for AD treatment include anti-oxidative stress, inhibiting neuronal apoptosis, antagonizing amyloid neurotoxicity and tau protein hyperphosphorylation, regulating immune function, anti-inflammation, normalizing the function of the cholinergic nervous system, recuperating neurobiochemical, and regulating AD-related genes. Consequently, IGs can combat AD by modulating multiple targets and pathways.
CONCLUSION:
Kidney-tonifying herbal IGs have great potential to combat AD.
2023-11-30·Nephrology, dialysis, transplantation : official publication of the European Dialysis and Transplant Association - European Renal Association
Clinical implications of changes in metabolic syndrome status after kidney transplantation: a nationwide prospective cohort study
Article
作者: Ki, Ju Man ; Lee, Dong Won ; Berm, Park Jae ; Kwon, Oh Jung ; Song, Seung Hwan ; Han, Duck Jong ; Chae, Dong-Wan ; Park, Sung Kwang ; Lee, Sam Yeol ; Kim, Joong Kyung ; Park, Jung Hwan ; Chung, Ku Yong ; Kim, Chan-Duck ; Shin, Ho Sik ; Song, Sang Heon ; Min, Ji Won ; Lee, Jung Jun ; Yang, Jaeseok ; Yoon, Hye Eun ; Jeong, Kyung Hwan ; Lee, Yu Ho ; Lee, Sang-Ho ; Kim, Yeong Hoon ; Kim, Myoung Soo ; Cho, Hong Rae ; Ha, Kyu ; Han, Seungyeup ; Jeon, Jin Seok ; Jun, Heungman ; Hwang, Hyeon Seok ; Yang, Chul Woo ; Ahn, Curie ; Lee, Su Hyung ; Lee, Kang Wook ; Jung, Cheol-Woong ; Park, Jong-Won ; Choi, Soo Jin Na ; Park, Yeon Ho ; Kong, Jin Min ; Lee, Jeong-Hoon ; Ban, Tae Hyun ; Lee, Jung Pyo ; Lee, Dong Ryeol ; Kim, Deok Gie
ABSTRACT:
Background:
Metabolic syndrome (MetS) is prevalent in patients with end-stage kidney disease, and kidney transplantation is expected to modify the metabolic status. However, whether changes in metabolic status at the time of transplantation affect recipient outcomes remains unclear.
Methods:
We analyzed 4187 recipients registered in a nationwide prospective cohort from 2014 to 2020. MetS was defined as the presence of three or more components of the metabolic syndrome. Patients were classified based on the pre- and post-transplant MetS status: MetS-free, MetS-developed, MetS-recovered and MetS-persistent. Study outcomes were occurrence of death-censored graft loss and a composite of cardiovascular events and death.
Results:
Among recipients without pre-transplant MetS, 19.6% (419/2135) developed post-transplant MetS, and MetS disappeared in 38.7% (794/2052) of the recipients with pre-transplant MetS. Among the four groups, the MetS-developed group showed the worst graft survival rate, and the MetS-persistent group had a poorer composite event-free survival rate. Compared with the MetS-free group, the MetS-developed group was associated with an increased risk of graft loss [adjusted hazard ratio (aHR) 2.35; 95% confidence interval (CI) 1.17–4.98] and the risk of graft loss increased with increasing numbers of dysfunctional MetS components. MetS-persistent was associated with increased risks of cardiovascular events and death (aHR 2.46; 95% CI 1.12–5.63), but changes in the number of dysfunctional MetS components was not.
Conclusion:
Kidney transplantation significantly alters the metabolic status. Newly developed MetS after transplantation was associated with an increased risk of graft loss, whereas persistent MetS exposure before and after transplantation was associated with increased risks cardiovascular events and patient survival.
2020-03-01·Iranian journal of kidney diseases4区 · 医学
Comparing Sleep Quality in Patients Before and After Kidney Transplantation.
4区 · 医学
Article
作者: Boshra Hasanzamani ; Elham Pourranjbar ; Amir Rezaei Ardani
INTRODUCTION:
The purpose of the present study was to identify the prevalence of sleep disturbances in ESRD, and to compare the sleep quality before and after kidney transplantation.
METHODS:
A semi-experimental study was performed on 40 participants with ESRD from September 2017 to September 2018 in Mashhad, Iran. Participants were in the waiting list of kidney transplantation, aged 18-years-old or more, had no history of any major psychological problems. They were excluded from the study if new medical condition or psychiatric disorder was initiated throughout the study. Patients' medical information including the duration of dialysis and laboratory data was extracted from medical records. Their sleep quality was assessed with the Pittsburgh sleep quality index (PSQI) within1-month prior the kidney transplantation and at the 3rd and 6th months after it. Collected data was analyzed using SPSS-16. P < .05 considered as significant.
RESULTS:
The frequency of poor sleepers was 37.5%, 37.5%, and 20.0%; before the kidney transplantation, 3 months and 6 months after the surgery; respectively. The average sleep quality score decreased significantly 6-month post-operation compared to pre-transplant phase (P < 0.05). We found a significant relationship between the gender and quality of sleep before transplant surgery, whereas no correlation was found between sleep quality and the age, type or duration of dialysis, serum phosphorus or hemoglobin level, and the cause of kidney failure (P < .05, > .05, > .05, > .05, > .05, > .05, and > .05; respectively).
CONCLUSION:
Kidney transplantation has a positive effect on patients' sleep quality after 6 months.
1
项与 Kidney(Esperion Therapeutics) 相关的新闻(医药)2025-02-27
·动脉网
2023年10月,美国生物科技公司United Therapeutics宣布完成对Iviva Medical的收购,收购资金为5000万美元现金首期支付,并包括潜在的收益条款,即Iviva肾脏产品净销售额的2%作为特许权使用费。
Iviva Medical是一家从哈佛大学器官实验室分拆出来的生物技术公司,专注于开发用于移植的生物人工肾脏,以解决器官短缺问题。该公司开发的Iviva Kidney是一种利用患者自身细胞制造的植入式生物人工肾脏,能够模拟天然肾脏的过滤和重吸收功能,解决终末期肾脏病人的肾源问题。
这起收购完成后不久,United Therapeutics就宣布以总金额约9100万美元收购异种器官支架上市公司Miromatrix,收获其正在开发中的生物工程肾脏产品Mirokidney™。
而这两起收购的背后,都有一家产业投资基金——德摩资本——的身影。公开资料显示,在两家肾脏产业公司被收购之前,德摩资本曾两次领投Iviva,其海外医疗证券基金Harmony Fund也曾投资Miromatrix。据德摩资本创始合伙人郑立新透露,United Therapeutics收购Iviva Medical的成功完成,实现了德摩资本在再生医学产业投资的第一例超10倍回报的成功退出,而第二起收购实现了其在肾科再生医学的两连胜,彰显出德摩资本在肾脏产业投资深厚功力。
从2017年开始投资肾脏科学至今,德摩资本已经陆续投资12家肾脏医疗公司,覆盖了从多伦多到旧金山,从阿联酋到日本全球主要的再生医学研究中心。在肾脏再生医学产业,建立了超过500个项目公司库,并已完成3个投资项目成功退出。2025年,基于丰富的肾脏科学行业投资经验、专家和项目资源,德摩资本预计将筹备发行国内外首家肾脏产业专业投资的系列基金。
今年2月,肾脏科学再次迎来重大突破。United Therapeutics宣布,公司已获得FDA批准,全面启动猪肾移植的大规模临床试验,开启肾脏再生医学的下一段征程。值此学科产业突飞猛进之际,动脉网有幸与国内首家肾脏学科产业投资基金德摩资本创始合伙人、董事长郑立新进行对话,探寻其在肾脏科学赛道获得超高投资回报的密钥。
左:德摩资本创始合伙人、董事长 郑立新;右:德摩肾脏学科和产业基金合伙人 李政海
德摩资本供图
01
牙科产业投资的15:0和早期AI医疗投资的3:2
古希腊传说中,手持一捆谷物的女神德摩忒尔常常被认为象征着智慧、洞察力和对未来的预见。
数千年后,在充满机遇和梦想的2000年,德摩资本应运成立,开始在医疗行业细分市场精耕细作,致力于通过产业链投资,为人类健康事业播撒希望的种子,收获未来的硕果。
2006年,牙科行业在全球范围内迎来了前所未有的发展机遇。在中国,随着居民收入水平的提高和对口腔健康重视程度的提升,牙科医疗服务的需求迅速增长,特别是种植牙和正畸等高端服务成为市场的主要增长点。消费升级的浪潮推动了对高端牙科产品和服务的需求,而数字化技术的普及则进一步提升了牙科服务的质量和效率。在欧美市场,老龄化人口对牙科服务的需求不断增加,技术创新如先进的种植体材料和数字化手术规划工具的应用,推动了牙科服务的质量提升。全球牙科行业的投资机会也逐渐显现,口腔医疗服务的连锁化经营成为重要趋势,高端牙科产品和服务的市场需求不断增加,新兴技术的应用为行业带来了新的增长点。
Opportunity knocks but once.这一年,德摩资本敏锐地将目光投向牙科,并在2007年年初出手投资后来在港股上市的隐形正畸龙头企业时代天使。“2006年,时代天使的首个产品——时代天使标准版获得国家药监局批准上市,成为中国首个获得专利的隐形矫治产品。然而,尽管这一技术在国际上已经展现出一定的成熟度和应用前景,但在中国市场,隐形正畸尚处于起步阶段。许多惯用钢丝矫正的正畸医生普遍认为‘太早、技术不成熟’,对隐形正畸持观望态度。”郑立新说。
自此以后,德摩资本便开始以精准而具有深度的风格集中在牙科领域进行投资。为此,德摩资本从创始人到基金经理,“几乎每一个人都在核心的被投企业锻炼、任职过很多年,参加国内外所有大型的口腔展会和论坛。”而郑立新本人走遍全球去拜访几乎所有的牙科领军企业,并到德国的专业牙科学校学习牙科相关知识。经过多年的深耕,德摩资本建立了一个涵盖牙科医疗服务、牙齿种植等牙科8大细分赛道、500个项目的产业库。
2014年,为了进一步推动中国牙科产业的发展,覆盖牙科产业链上下游,德摩资本和安信证券直投部合作设立由国际牙科巨头支持的安信德摩牙科产业基金,成为国内首支专注于牙科产业细分领域的股权投资基金,开创了“产业专项基金”模式。
从第一次投资牙科到2015年,德摩资本几乎创造了“战无不胜的神话”——累计在牙科产业投资15次,“15次投资无一失败。”这些投资组合除了隐形矫正领域的龙头企业时代天使外,还包括舌侧矫治垄断型企业瑞通生物、牙科修复及正畸解决方案提供商现代牙科等。
相较于精准而具有深度的牙科产业投资,德摩资本在2015年发起的早期AI医疗投资,成功率锐减至60%——“投资的5个项目中出现两次失误,损失较重。”在郑立新看来,失败的主要原因是进入AI医疗赛道时,对行业的技术发展、市场需求和商业模式的认知还不够深入。因此在选择投资项目时,未能充分评估技术的可行性和市场的接受度。
过去10年间,无论是德摩资本,还是其他风投机构的投资尝试,都在证明一个投资的“秘诀”——“深入介入一个赛道、一个学科,让自己的投资团队变成行业内专家,穷尽这个领域的知识、信息、人脉、项目,才有可能打造出投资领域的优秀基金。”
02
投资前的三个必备动作
“在投资领域,有一句广为流传的观点:人无法赚到超出自身认知范围的财富。学习巴菲特的投资理念,寻找长坡厚雪,构建起自身坚固护城河的伟大企业,坚守在自己的核心能力圈范围内进行投资,从而降低失误概率,获取长期稳定的投资回报,已经成为中国资本界一级、二级市场的普遍共识。然而,如何有效拓宽认知边界,获得精准而深刻的认知,在投资圈内却是一个见仁见智的复杂问题。”郑立新说。
从牙科到AI医疗,德摩资本已经摸索出一套关于投资的方法论。首先是梳理产业细分赛道,搭建产业链项目库、公司库和专家库——没有庞大的数据库,就难以深入了解赛道、全面覆盖细分产业链并指导投资决策。目前,在肾脏科学领域,德摩资本已经积累CGT(细胞和基因疗法)、器官再生医学赛道的知识、项目和人脉,并覆盖了从多伦多到旧金山,再从阿联酋到日本全球主要的再生医学研究中心,建立起超过500个项目公司库。
其次,研究产业中成功或失败的案例,从中寻找产业的底层逻辑。“只有通过剖析最成功或最失败的投资案例,才能真正找到投资的底层逻辑。这种逻辑不仅能够帮助投资者在复杂多变的市场中把握机会,还能够在竞争激烈的产业赛道中脱颖而出。”郑立新说。
以丹麓资本为例,其创始合伙人创立丹麓资本之前,在红杉资本成功投资健帆生物并赢得了其历史上最高的回报率,也让该专业学习肾科的合伙人声名鹊起。随后,该合伙人离开红杉资本,创办丹麓资本,继续在肾脏科学领域深耕。
“健帆生物的成功,堪称肾脏科学领域最成功的案例之一,让我们看到了肾脏疾病治疗领域的巨大潜力。这是一个很难攻克的疾病领域,但一旦进入并站稳脚跟,就能获得可观的回报。”郑立新指出,透析产业已经是一个存在了几十年的庞大市场,像费森尤斯这样的巨头长期垄断,几乎没有新进入者能够颠覆其地位。这背后的原因在于该产业的底层逻辑非常稳固,一旦形成竞争优势,就很难被撼动。
他进一步解释说,这种稳固的产业逻辑吸引了像巴菲特这样的投资大师。巴菲特长期持有美国前三大肾脏透析服务商之一达维塔(Da Vita)的股票,证明了该产业内在的底层逻辑和投资逻辑的稳固性。德摩资本在探索新的投资机会时,也着重分析产业的底层逻辑,确保投资决策能够经受住市场的考验。
“我们发现,在肾脏疾病治疗领域,失败的案例并不多,成功的案例比比皆是。”郑立新总结道,“这说明,只要能够精准把握产业的底层逻辑,投资者就能在这个领域取得成功。”
第三点,构建全球产业智慧网络并运用系统化的产业分析模型,以帮助投资机构精准把握产业趋势,并在投资决策中占据制高点。
郑立新指出,德摩资本在全球范围内积极拜访肾脏研究领域的顶尖实验室和专家,通过资本纽带与哈佛、京都、旧金山等地的肾脏病学专家建立合作关系。这种战略布局不仅让德摩资本获得了全球产业的前沿智慧和人脉资源,还为其投资决策提供了坚实的学术支持。“如果能够与全球肾脏病学领域的顶级专家建立联系,甚至成为合伙人,那么这个产业的智慧和人脉基本在你的掌控之中。”郑立新补充道,“这就好比在AI领域与Hinton教授或李飞飞教授交朋友,有了这样的资源,投资失败的可能性微乎其微。”
而在系统化的产业分析模型方面,德摩资本借鉴了麦肯锡的SCP(产业结构、市场绩效、企业行为)模型,并结合波特五力模型,构建了一个全面的产业分析框架。“我们几乎将SCP模型应用到所有投资分析中,从产业结构、上下游谈判,到技术冲击和消费趋势,再到产业未来的演变,都进行了深入分析。”郑立新解释道。在肾脏疾病治疗领域,德摩资本在过去七八年中对SCP模型中的每一个参数进行了大量模拟,包括上游供应系统、下游患者和临床医生,以及国家监管政策等。
03
大器官大赛道
行情总在绝望中诞生,在半信半疑中成长,在憧憬中成熟。随着时间的推移,郑立新逐渐意识到化学药物作为临床治疗手段的局限性,其新药发现越来越稀少,投资回报与研发投入已不成正比。郑立新比喻说,当一扇门被关闭时,总会有一扇窗被打开,而当化学药物和器械的发展接近极限时,新的技术突破也应运而生。
“2015年,我们认为人工智能会成为医疗技术革命的那扇窗,这也是我们成立人工智能基金的原因。”郑立新表示。然而,经过两年的探索,他意识到人工智能可能并非唯一的突破点。最终,德摩资本将目光转向了细胞与基因治疗(CGT)领域,这一技术让郑立新看到了从微观的基因编辑到宏观的器官替换全面覆盖的可能性——这种技术不仅能够在胚胎期进行干预,还能在疾病晚期进行器官替换,覆盖了从出生到生命终结的全过程。郑立新认为,CGT技术、AI、合成生物学等构成了前所未有的生命科技革命,不亚于前几十年的化学工业、大分子生物药,将在未来几十年内推动人类寿命的显著延长,甚至可能成为未来医疗技术的主导力量。
“我们与波士顿和哈佛的同事们进行了长期探讨,最终确定肾脏作为投资和创业的重点。”郑立新解释说,“要解决肾脏疾病,仍需依赖基因技术,因为基因改造能够赋予细胞更强的功能,而细胞正是构建人工肾脏的活性成分。”2017年,德摩资本开始调整投资方向,专注于大器官领域。郑立新指出,鉴于基因技术的底层研究需要大量投入和专业人才,团队更倾向于靠近临床应用的领域。因此,德摩资本选择了人体器官作为投资重点,尤其是肾脏、肝脏和心脏等重要脏器。“当我们对人体的各大器官进行技术性排序时,肾脏科学赛道的几个显著特点吸引了我们的注意。”郑立新说。
首先,肾脏疾病的发病率高达10%,与糖尿病和一些严重的肝病患者数量相当。然而,肾脏疾病具有不可逆性,病情会持续加重,且目前缺乏特效药物。肾脏的复杂性在于其细胞种类繁多,多达二三十种,这使得基础研究和临床治疗面临巨大挑战。在全球范围内,直到2015年以前,肾脏疾病相关的科研论文和临床研究数量几乎停滞不前,表明该领域存在许多未解决“黑箱”。
肾脏疾病不仅对患者个人造成巨大痛苦,还会延伸至终末期肾衰竭— 尿毒症。患者要么面临死亡,要么每周三次、每次四个小时的透析治疗,这不仅是身体上的折磨,也是巨大的经济负担。肾源的稀缺性进一步加剧了这一问题。从临床医生和医疗投资者的角度来看,肾脏疾病是一个巨大的痛点,但解决方案却极为稀少。
“从投资者的角度来看,这是一个非常值得投入的领域。肾脏疾病存在巨大的痛点,而现有的技术无法解决这一问题。但随着CGT技术的发展,有望彻底颠覆这一领域。”郑立新指出,“这几乎是每一个投资者的梦想赛道——巨大的社会痛点与潜在的技术突破机会相结合。”
谈到在肾脏科学赛道的投资策略,郑立新表示:“我们首先会衡量一个项目是否能够颠覆现有的常规技术,提供一种全新的解决方案。如果一个技术与现有的常规技术截然不同,并且能够针对肾脏疾病的不同阶段(从CKD一期到五期)提供有效的解决方案,那么这个项目就值得我们深入研究。”
除了技术的突破性,德摩资本还会评估公司的估值是否合理。如果由于市场对赛道的认知不足,导致某些项目的估值被严重低估,这将是一个重要的投资机会。“如果市场对某个项目存在认知障碍,而我们能够看懂它的价值,那么重新估值后就会发现其中的投资回报潜力。”郑立新解释道。
最后一个角度则是从产业链的角度评估项目的价值。指出:“我们会考察一个项目在整个产业链中的角色,它是否是一个底层技术,是否处于产业链的制高点,或者是否是关键的收费环节。如果一个项目在这些方面具有优势,哪怕其技术含量稍低,我们也会考虑对其进行投资。”
正是基于这样的投资逻辑,2017年,德摩资本在全球范围内研究肾脏学科和产业,并将第一单落在背靠麻省总医院(MGH)和哈佛大学医学院的Ott器官实验室。该实验室由脱细胞支架重建器官技术的全球开创者Ott教授领导,并得到了哈佛大学干细胞研究所执行所长Brock Reeve的全力支持。随后,基于对这一前沿技术的高度认可,德摩资本领投了人工肾脏公司Iviva Medical公司,并吸引了包括美国著名的硅谷长寿基金、Singularity大学创始人Peter Diamandis旗下的Bold Capital等知名机构地跟投。
目前,德摩资本在肾脏科学领域已经投资了12个项目,实现了从微观到宏观的全产业链覆盖。通过投资组合之一的深圳华源再生医学——亚洲领先的肾脏细胞疗法、药物研发、生物人工肾研制公司,德摩资本与中山大学成立了全国唯一“中山大学-华源肾脏再生和重建医学实验室”。同时,通过另一投资组合华津肾科研究公司,德摩资本和超过50多个中国肾脏学科的教授团队建立了肾病研发、药物筛选的合作关系。“目前,我们应该是全球覆盖PI最多的肾科专业研究基础服务平台。”郑立新说。
04
写在最后:CGT、器官合成与临床CRO
郑立新指出,当前医疗技术的迭代速度极为迅猛,尤其是基因编辑技术领域,新的技术不断涌现。这种快速的技术演进意味着,如果投资者稍有不慎,就可能被新兴技术所颠覆。无论是合成生物学的突破,还是AI与蛋白组学的融合,任何一项新技术都有可能彻底改变行业格局。
“在这种情况下,投资公司必须具备多代技术的储备,以应对快速变化的技术环境。”郑立新强调,“不能仅仅依赖某一项单一技术。如果那项技术停滞不前,公司可能会随之消亡。”
因此,在肾脏领域,除了CGT技术外,器官合成技术也是德摩资本看好的领域之一。郑立新认为,这一领域在未来五到十年内可能实现重大突破,带来千亿美金的市场机会。器官合成技术结合了细胞编辑技术和材料科学,为器官衰竭患者提供了新的希望。“器官合成技术代表了未来临床治疗的顶级模式。”郑立新指出,“未来,器官衰竭患者可能直接通过器官替换来恢复健康,而无需依赖药物治疗。”
此外,德摩资本还特别关注肾脏疾病研究领域的增长。过去几年,肾脏疾病的研究活动和学术文章数量每年增长40%,显示出该领域正处于爆发前期。郑立新认为,为肾脏疾病研究提供底层解决方案的企业,如药物开发和临床试验服务提供商,将成为这一领域的“卖水人”,在未来获得巨大收益。
当前,全球肾脏赛道竞争在中美脱钩的背景下,异常激烈。2019年,美国成立肾脏重建联盟(Rebuilding the Kidney, RBK),将东亚科学家拒之门外,地缘政治因素对科研合作构成了巨大冲击。此后,德摩资本开始深耕亚洲肾脏科学生态圈,积极与日本的四所顶尖大学以及欧洲、新加坡和阿布扎比等地区的科研机构建立了合作关系,形成了亚洲肾科再生医学联盟。郑立新表示:“未来5到10年,肾科学术、产业和资本界避免不了受到地缘政治因素的影响,通过亚洲肾科再生医学联盟这种跨区域的合作,我们希冀能够更好地应对全球竞争,推动肾脏再生医学技术的发展和应用。”
*封面图片来源:123rf
如果您想对接文章中提到的项目,或您的项目想被动脉网报道,或者发布融资新闻,请与我们联系;也可加入动脉网行业社群,结交更多志同道合的好友。
近
期
推
荐
声明:动脉网所刊载内容之知识产权为动脉网及相关权利人专属所有或持有。未经许可,禁止进行转载、摘编、复制及建立镜像等任何使用。
动脉网,未来医疗服务平台
并购
100 项与 Kidney(Esperion Therapeutics) 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 慢性肾病 | 临床前 | 美国 | 2024-05-08 | |
| 常染色体显性多囊肾病 | 临床前 | 美国 | 2024-05-08 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
No Data | |||||||
登录后查看更多信息
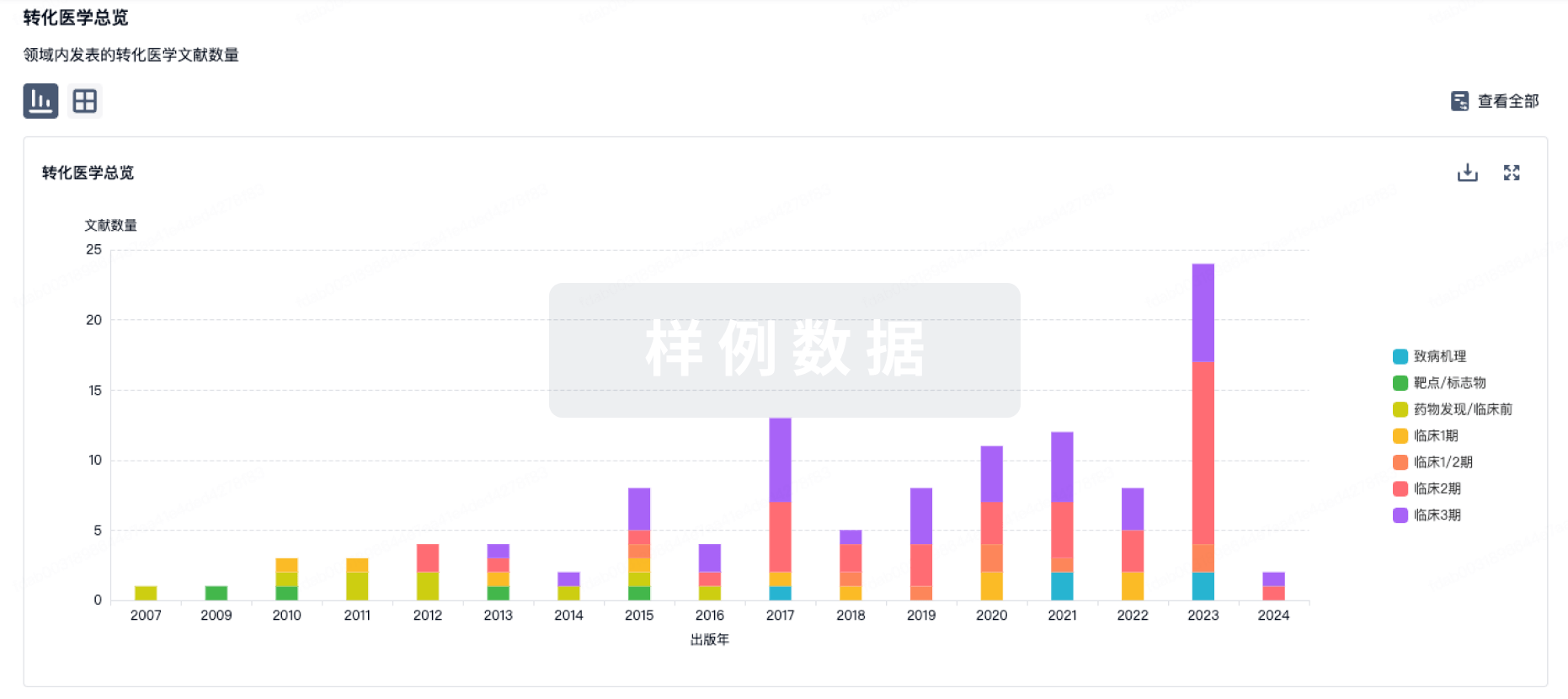
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
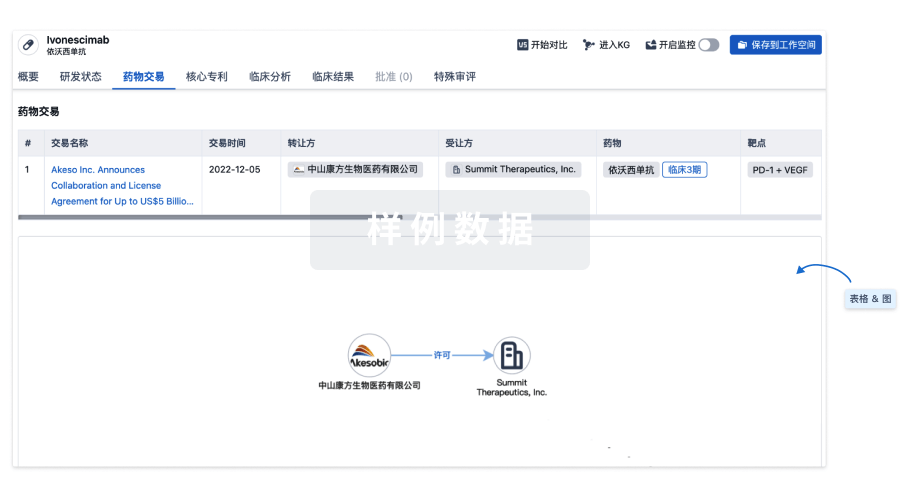
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
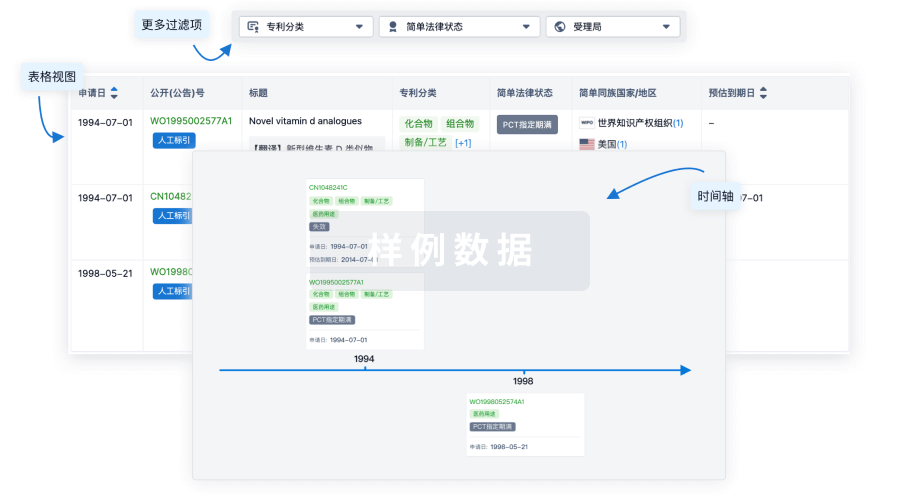
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
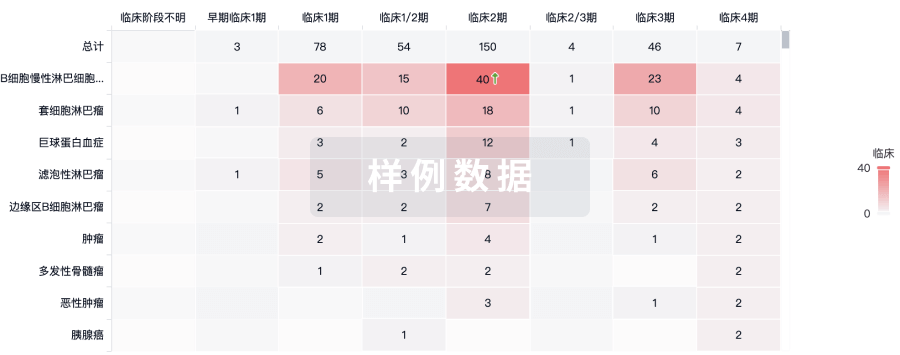
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
批准
利用最新的监管批准信息加速您的研究。
登录
或
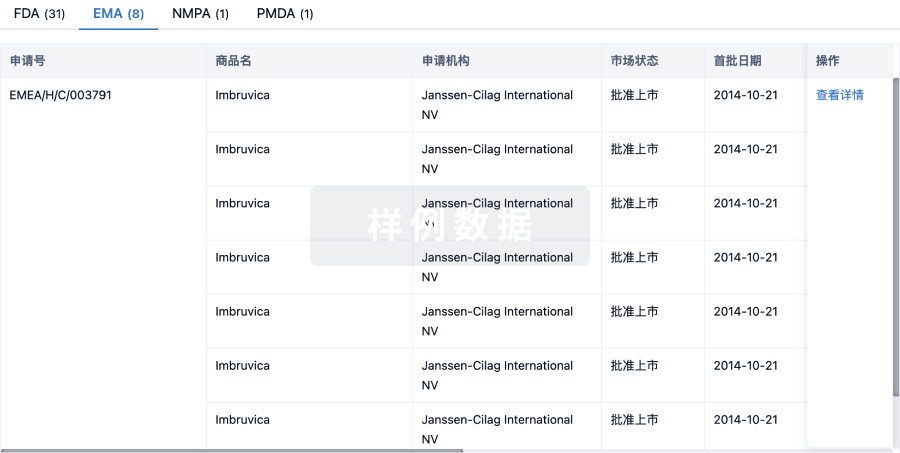
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
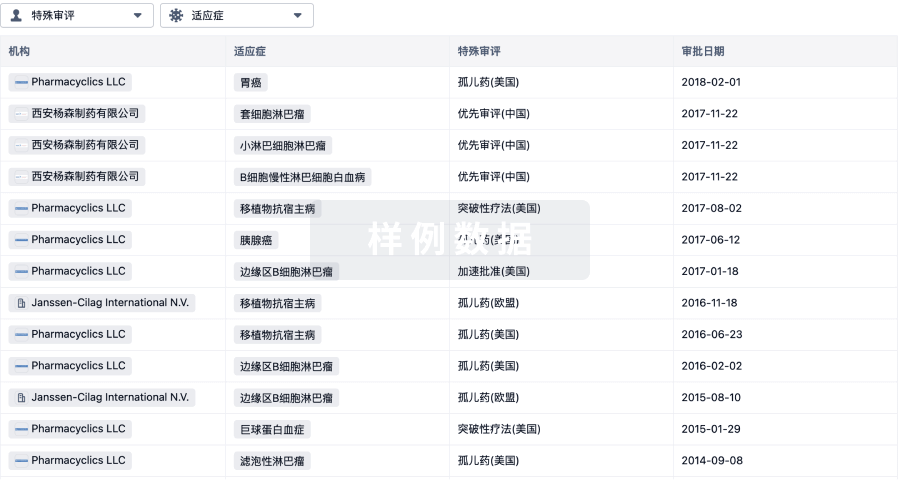
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
