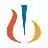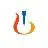预约演示
更新于:2025-05-07
Ecleralimab
更新于:2025-05-07
概要
基本信息
在研机构 |
权益机构- |
最高研发阶段临床2期 |
首次获批日期- |
最高研发阶段(中国)- |
特殊审评- |
登录后查看时间轴
结构/序列
Sequence Code 13223996L

来源: *****
Sequence Code 13223998H

来源: *****
关联
6
项与 Ecleralimab 相关的临床试验CTRI/2022/03/040746
A 12-week, randomized, participant-and investigator-blinded, placebo-controlled, parallel group study to explore the efficacy, pharmacodynamics, safety, and pharmacokinetics of two doses of inhaled CSJ117 in adults with Chronic Obstructive Pulmonary Disease (COPD)
开始日期2022-03-04 |
申办/合作机构 |
EUCTR2021-000692-36-CZ
A 12-week, randomized, participant-and investigator-blinded, placebo-controlled, parallel group study to explore the efficacy, pharmacodynamics, safety, and pharmacokinetics of two doses of inhaled CSJ117 in adults with Chronic Obstructive Pulmonary Disease (COPD)
开始日期2021-12-13 |
申办/合作机构 |
NCT04882124
A 12-week Randomized, participant-and Investigator-blinded, Placebo-controlled, Parallel Group Study to Explore the Efficacy, Pharmacodynamics, Safety, and Pharmacokinetics of Two Doses of Inhaled CSJ117 in Adults With Chronic Obstructive Pulmonary Disease (COPD)
This is a Phase 2 study in patients with chronic obstructive pulmonary disease (COPD) to assess the efficacy, pharmacodynamics (PD), pharmacokinetics (PK), and safety of two dose levels of CSJ117 in comparison to placebo. For this, the impact of CSJ117 on disease symptom burden and lung function will be explored.
开始日期2021-09-24 |
100 项与 Ecleralimab 相关的临床结果
登录后查看更多信息
100 项与 Ecleralimab 相关的转化医学
登录后查看更多信息
100 项与 Ecleralimab 相关的专利(医药)
登录后查看更多信息
4
项与 Ecleralimab 相关的文献(医药)2024-01-02·Expert Opinion on Investigational Drugs
Investigational thymic stromal lymphopoietin inhibitors for the treatment of asthma: a systematic review
Review
作者: Rogliani, Paola ; Bettin, Federica Roberta ; Manzetti, Gian Marco ; D’Auria, Maria ; Calzetta, Luigino
2023-03-01·European Respiratory Journal
Inhaled anti-TSLP antibody fragment, ecleralimab, blocks responses to allergen in mild asthma
Article
作者: O'Byrne, Paul M ; Korn, Stephanie ; Cao, Hui ; Jain, Monish ; Pertel, Peter E ; Cabanski, Maciej ; Boulet, Louis-Philippe ; Cockcroft, Donald W ; Watz, Henrik ; Kornmann, Oliver ; Davis, Beth E ; FitzGerald, J Mark ; Leigh, Richard ; Jones, Ieuan ; Mayers, Irvin ; Grant, Sarah S ; Hohlfeld, Jens M ; Gauvreau, Gail M ; Lecot, Jean R
2023-02-01·Pulmonary Pharmacology & Therapeutics
Development of an inhaled anti-TSLP therapy for asthma
Review
作者: Taube, Christian ; Fleming, Margaret ; Panettieri, Reynold A ; Altman, Pablo ; O'Byrne, Paul M ; Brindicci, Caterina
7
项与 Ecleralimab 相关的新闻(医药)2025-03-03
·微信
2024年6月26日,全球首个双重PDE3/4抑制剂Ensifentrine(恩塞芬汀)在FDA获批上市。这款号称“一药双效”的创新药物,成功打破COPD治疗僵局,开启了“抗炎+扩支”的整合治疗时代。
2024年9月27日,赛诺菲宣布,达必妥®(度普利尤单抗注射液)获得中国国家药品监督管理局(NMPA)批准,用于血嗜酸性粒细胞升高且控制不佳的慢性阻塞性肺疾病成人患者,借此开启了COPD生物治疗时代。
2024年12月20日,这款由健康元与拜耳合作开发的慢阻肺(COPD)治疗药物,是目前单靶点口服药市场仅有的新药产品,也可能成为中国首款创新机制的COPD口服药。
2025年2月21日,GSK宣布其IL-5单抗Nucala(美泊利珠单抗)的新药上市申请获国家药监局受理,用于作为嗜酸性粒细胞表型慢性阻塞性肺病(COPD)患者的附加维持治疗,再次将COPD领域的靶向生物药疗法推向了高潮。
不到一年,COPD领域的新药研究似乎就成为了香饽饽,不仅MNC接连布局,国内Biotech企业更是将其作为赶超全球的大好机会,这是为何?
更关键的是,COPD领域背后究竟有何魅力?如今的在研领域又是怎样一个局面?
庞大的患者群体
所谓慢阻肺,即一种常见的、可预防和治疗的慢性气道疾病,其特征是持续存在的气流受限和相应的呼吸系统症状,是一种较常见的慢性疾病,病死率较高,且严重影响患者的生命质量,并给其家庭与社会带来沉重的经济负担。
据悉,COPD已成为全球第三大死亡原因,全球约有3.9亿例COPD患者,中国约有1亿例COPD患者,占全球COPD病例的近25%,潜在用药市场庞大。
而随着慢阻肺规范化诊疗的推行,虽然慢阻肺死亡率逐年下降,但随着空气指数下降、吸烟等因素,其整体发病率却出现反向上涨的趋势。
更关键的是,由于目前慢阻肺的发病机制尚未完全明确,氧化应激、炎症反应、蛋白酶/抗蛋白酶失衡等多种因素均可导致组织重构,进而致病,相对复杂的致病原理也为COPD新药研究带来巨大困难。
局限严重的传统治疗
一直以来,临床上针对稳定期慢阻肺病治疗基本围绕两个目标进行,即减轻症状和降低风险,两个目标相互关联、相互促进,共同构成了慢阻肺病管理的重要内容。
尽管这些药物及干预措施虽能显著改善慢阻肺病患者的症状,但其局限性也相对比较大,比如治疗精准性不足、疾病异质性高、无法逆转病程、传统治疗副作用明显、耐药性严重等。
更关键的是现阶段临床药物治疗无法覆盖所有慢阻肺病疾病表型,并且鉴于慢阻肺病的发病机制相当复杂且尚未完全阐明,目前临床上仍缺乏针对病因的有效治疗药物。
这也使取得一定临床成就的创新疗法无法复制到 COPD 治疗领域,相关新药临床研究推进异常缓慢。
两极分化的在研方向
在历史上,COPD新药主要分为三个时代,即传统支气管扩张剂时代、抗炎治疗兴起时代、生物制剂革命时代。而围绕三个时代的发展,也演变出如今在研COPD新药的两大方向,即老药新发展与生物靶向药替代。
图片来源:博药(点击查看大图)
老药新发展
首先,有一点需要明确:老药并非“不行”。
事实上,在几十年临床使用上的经久不衰已是老药的最佳证明,而老药新发展,既是指临床目标不变(减轻症状+降低风险),针对不良反应、临床有效性等方向进行了诸多优化性设计。
新型吸入 β2 受体激动剂(LABA)
由于β2受体激动剂主要作用于气道平滑肌细胞、肥大细胞膜表面的β2受体,其在缓解COPD临床症状方面有着广泛认可的作用,也是目前COPD临床治疗主力药物之一。
从短效β2受体激动剂到长效β2受体激动剂,临床上用于COPD治疗的LABA在频繁用药、药物剂量、实用性、患者依从性、安全性方面做出系列产品更迭,也确定了新型LABA的主线方向。
药品名称
靶点
适应症最高临床阶段
原研单位
最新临床进展时间
(近三年有进展即“活跃管线”)
阿贝特罗 Abediterol
ADRB2
临床Ⅱ期
Almirall Ltd;阿斯利康
2019-12-12
琥珀酸巴芬特罗 Batefenterol Succinate
ADRB2;CHRM2;CHRM3
临床Ⅱ期
Innoviva Inc
2016-01-21
AZD-2115
ADRB2;mAChR
临床Ⅱ期
Pearl Therapeutics Inc;阿斯利康
2017-03-06
卡莫特罗 Carmoterol
ADRB2
临床Ⅱ期
田边三菱制药株式会社
2011-10-19
维兰特罗 Vilanterol
ADRB2
临床Ⅱ期
葛兰素史克
2007-08-21
数据来源:公开数据整理、药智数据
时至今日,研发端上仍有药企致力于新型β2受体激动剂方向,但受限于临床替代难度较大,其中大多数管线的临床推进已不再积极。其中,比较具有代表意义的有几种新型β2受体激动剂:
卡莫特罗(Carmoterol)活性及对β2受体的选择性高,起效快,作用时间达30h,治疗过程中耐受性和安全性与沙美特罗无显著差异。
维兰特罗(Vilanterol)较沙美特罗起效快、治疗指数高、内在活性好,作用时间超过24h。
但从目前该领域的研发活跃情况来看,可以预见的是未来新型LABA大概率将不再是COPD新药研发的主要方向,至少已很少有企业愿意在朝这方面努力了。
新型长效抗胆碱药(LAMA)
抗胆碱能药物主要通过阻断M1-M3胆碱受体,进而扩张气道平滑肌、改善气流受限和慢阻肺症状,20世纪70年代,短效抗胆碱药物(SAMA)开始被用于慢阻肺的治疗,但虽起效迅速,但作用时间仅6—8小时,对于COPD这样的慢病而言,局限性较大,因此21世纪初,长效抗胆碱能药物(LAMA)问世,作用时间大幅增长,部分产品甚至可超过24小时。
比如,2017年获批上市的格隆溴铵(Glycopyrrolate),对M3受体的选择性较噻托溴铵高,起效时间较噻托溴铵快4.8倍,安全性好;GSK的乌美溴铵改善FEV1的效果与噻托溴铵相似,效果与剂量无相关性,吸收迅速(Tmax=5~15min),在血液中代谢迅速,耐受性好。
药品名称
靶点
适应症最高临床阶段
原研单位
最新临床进展时间(近三年有进展即“活跃管线”)
乌美溴铵 Umeclidinium Bromide
CHRM1;CHRM2;CHRM3;CHRM4;CHRM5
已上市
葛兰素史克
2023-11-08
阿地溴铵 Aclidinium Bromide
CHRM3
已上市
Almirall SA;精鼎医药(许可)
2024-08-13
噻托溴铵 Tiotropium Bromide
CHRM3
已上市
勃林格殷格翰
2025-02-06
TRN-157
CHRM3
临床Ⅱ期
Theron Pharmaceuticals Inc;山东鲁抗医药(许可);长风药业(许可)
2024-08-09
数据来源:公开数据整理、药智数据
而目前,在新型长效抗胆碱能药(LAMA)研发层面,其整体情况与LABA的局面类似,绝大多数管线的临床进展并不积极,仅少数产品还在持续推进,其中山东鲁抗的TRN-157,目前其已在美国完成了I期和IIa期临床试验,在国内已完成了健康受试者单次给药的I期临床试验,安全性均良好,本品已获得国家药品监督管理局同意开展IIa期临床试验。
双靶点支气管扩张剂(MABA)
MABA是一类新型具有毒蕈碱拮抗剂和β2激动剂双重作用的双靶点药物,能够实现在一个分子上同时作用两大靶点的创新设计,具有M受体拮抗和β受体激动两种功能,可协同扩张气管和抗炎。
对比LABA与LAMA单靶点产品,从机制上其具备了核心的三大优势:
双靶点协同,疗效提升:双靶点机制不仅成功规避了LAMA、LABA单药治疗可能面临的疗效局限性和潜在副作用风险,更通过“双靶点”的协同作用,实现COPD疾病症状以及肺功能的双重改善,大幅提升治疗效果和患者的治疗依从性。
兼顾速效与长效,治疗优势凸显:数据显示,该药物兼具速效与长效的双重治疗优势,能够迅速响应急性期的需求实现快速缓解,同时亦适合作为长期维持治疗的选择,有望对现有治疗方案形成强有力的补充甚至替代。
安全设计、无忧治疗:该药物独特的季铵盐结构设计能够有效避免药物进入中枢神经系统,从而大幅降低对中枢神经系统产生副作用的可能性,提升了治疗的安全性,为慢阻肺患者带来更加高效、便捷且安全的治疗新选择。
药品名称
靶点
关键适应症与阶段
适应症最高临床阶段
原研单位
最新临床进展时间(近三年有进展即“活跃管线”)
琥珀酸巴芬特罗 Batefenterol Succinate
ADRB2;CHRM2;CHRM3
临床Ⅱ期:慢性阻塞性肺病
临床Ⅱ期
Innoviva Inc
2016-01-21
CHF-6366
ADRB2;CHRM3
临床Ⅱ期:哮喘;慢性阻塞性肺病
临床Ⅱ期
意大利凯西制药公司
2017-12-14
DBM-1152A
ADRB2;CHRM3
临床Ⅰ期:慢性支气管炎;慢性阻塞性肺病;支气管痉挛;肺气肿引起支气管痉挛
临床申请:哮喘
临床Ⅰ期
硕佰医药
2024-08-08
TQC-3927
ADRB2;CHRM3
临床Ⅰ期:慢性阻塞性肺病
临床申请:哮喘
临床Ⅰ期
正大天晴
2024-12-02
数据来源:公开数据整理、药智数据
目前,MABA类双靶点制剂相对前两类药物的研发热情明显更高,是COPD新药研究的重要方向之一,其中Innoviva的Batefenterol、阿斯利康的Navafenterol与凯西制药的CHF-6366临床进度较靠前,但进展相对不那么积极。而对比之下,部分国内管线明显更加活跃,比如硕佰医药与健康元的DBM-1152A、正大天晴的TQC-3927,目前均已进入临床I期,且临床推进迅速。
PDE双靶点抑制剂
PDE主要分布于体内各种炎症细胞内,家族的成员多达11位,每位成员各司其职,参与不同的生理过程,其中PDE-4抑制剂可以阻止PDE-4对cAMP/cGMP的水解作用,使cAMP/cGMP在炎症细胞内聚集。
因此,PDE4抑制剂对于治疗慢性阻塞性肺疾病(COPD)非常有吸引力。
但由于PDE4在全身多处组织中广泛表达,导致其具备潜力的同时,不良反应也极大地限制了其发展。因此,寻求一款兼具高有效性与低不良反应的PDE4抑制剂成为该领域的主线任务。
多项研究表明,相比于单独抑制PDE3或PDE4,同时抑制PDE3和PDE4产生的抗炎和松弛平滑肌作用更强,同时较低的副作用也使得PDE3/4双重抑制剂顺势成为COPD新药研发的趋势之一。
数据来源:公开数据整理、药智数据(点击查看大图)
其中,2024年全球首个获FDA获批上市的PDE3/4抑制剂Ensifentrine(恩塞芬汀)就是显著代表,“一药双效”的创新药物,成功打破COPD治疗僵局,开启了“抗炎+扩支”的整合治疗时代。
国内领域,目前也有多家企业有所布局,进入临床阶段的产品包括正大天晴的TQC-3721与恒瑞医药的HRS-9821,不出意外的话,首款国产PDE3/4抑制剂将在两者中产生。
PI3Kδ 抑制剂
虽然PI3K药物大多集中肿瘤领域(包括实体瘤和血液肿瘤),目前已获批上市的PI3K抑制剂适应症也均为肿瘤,但近年来的研究表明PI3K在慢性阻塞性肺疾病(COPD)、哮喘、特发性肺纤维化(IPF)以及神经系统疾病病理过程中也扮演重要角色,这也导致部分企业对上述适应症的临床试验兴趣大涨。
其中,在一些COPD患者中对诸如皮质类固醇的常规疗法的抗性已被归因于PI3Kδ/γ途径的上调。另外,PI3Kδ/γ的双重抑制强烈地涉及气道及其他自身免疫性疾病的过敏及非过敏性炎症作为干预策略。
因此,针对PI3Kδ/γ信号传导的抑制提供了一种旨在对抗免疫炎性反应的新手段。
药品名称
靶点
关键适应症与阶段
产品最高临床阶段
适应症最高临床阶段
原研单位
最新临床进展时间(近三年有进展即“活跃管线”)
奈米利司 Nemiralisib
PI3Kdelta
临床Ⅱ期:PI3Kδ过度活化综合征;哮喘;慢性阻塞性肺病
临床Ⅱ期
临床Ⅱ期
葛兰素史克
2018-10-23
RV-6153
PI3K
临床Ⅰ期:慢性阻塞性肺病
临床Ⅰ期
临床Ⅰ期
RespiVert Ltd
2015-07-28
RV-1729
PI3K;PI3Kdelta;PIK3CG
临床Ⅰ期:慢性阻塞性肺病
临床Ⅰ期
临床Ⅰ期
RespiVert Ltd
2014-05-14
数据来源:公开数据整理、药智数据
目前,在该领域中涉及COPD的临床阶段管线数量不多,且绝大多数管线临床状态并不活跃,其中GSK的Nemiralisib是目前临床阶段最靠前的创新疗法,其次则是RespiVert的RV-6153与RV-1729。
CXCR拮抗剂
早些年,小分子趋化因子受体(CXCR)拮抗剂在呼吸系统疾病中的作用仍是一个活跃的研究领域,研究发现COPD患者体内CXCL8、CXCL1和CXCL5的水平升高,与CXCR2受体结合后,使中性粒细胞和单核细胞增多并激活。
口服CXCR拮抗剂具有抑制肺部慢性中性粒细胞性炎症的作用,临床研究还发现CXCR2拮抗剂同样具有抑制肺部慢性中性粒细胞性炎症的作用,提示对COPD具有潜在的治疗作用。
药品名称
靶点
关键适应症与阶段
产品最高临床阶段
适应症最高临床阶段
原研单位
最新临床进展时间(近三年有进展即“活跃管线”)
多西帕司他钠 Dociparstat Sodium
CXCL12;CXCR4
临床Ⅲ期:SARS-CoV-2感染;急性肺损伤;急性髓系白血病
临床Ⅱ期:慢性阻塞性肺病
临床Ⅲ期
临床Ⅱ期
Cantex Pharmaceuticals Inc;Chimerix Inc
2021-02-26
AZD-5069
CXCR2
临床Ⅱ期:呼吸系统疾病;哮喘;慢性支气管炎;慢性阻塞性肺病;支气管扩张;肝癌;肺气肿;肺病
临床Ⅱ期
临床Ⅱ期
阿斯利康
2022-03-07
达尼利星 Danirixin
CXCR2
临床Ⅱ期:慢性阻塞性肺病;流感病毒感染
临床Ⅰ期:呼吸道合胞病毒感染
临床Ⅱ期
临床Ⅱ期
葛兰素史克
2018-03-01
QBM-076
CXCR2
临床Ⅱ期:慢性阻塞性肺病
临床Ⅰ期:三阴性乳腺癌;结直肠癌;肾细胞癌;非小细胞肺癌
临床Ⅱ期
临床Ⅱ期
诺华制药
2016-05-09
数据来源:公开数据整理、药智数据
但随着研究深入,目前大多数针对趋化因子受体和介质的药物研究已经停止,仅有少数几个针对CXCR1与CXCR2拮抗剂的研究还在继续。
生物靶向药崛起
对COPD生物药的开发探索,一直都是当前创新药研发的重点方向,但由于创新疗法的局限性,对新开发项目来说,不确定因素往往更多,这也导致十数年里全球制药企业在COPD生物药研发过程中折戟无数。
不过,随着医药基础研究水平的进步,靶向生物药市场验证机会也越来越多,近年来COPD生物靶向药逐渐有了新的希望,相关疗法也陆续取得不错的成绩,目前来看“IL/TSLP单抗”与“靶向双抗”是现阶段最被寄予厚望的技术方向。
单抗
多项研究表明,COPD患者的整个气道、肺实质和肺血管中都存在慢性炎症。这就表示包括1型细胞因子肿瘤坏死因子α(TNF-α),2型细胞因子IL-4、IL-5、IL-13及其警报素IL-33、TSLP等都会参与COPD病理生理,而随着研究深入,TNF-α抑制剂单抗在COPD实际治疗中的临床疗效相对有限,逐渐被研究者放弃。
因此,COPD单抗的相关研究开始集中转向2型炎症,IL-4、IL-5、IL-33与TSLP逐渐成为COPD单抗研究的“四强”。
IL-5单抗方面,由于率先在嗜酸性粒细胞表型重症哮喘方面取得突破,如阿斯利康、GSK等MNC都希望能一鼓作气,将其药物用途拓展至COPD领域,彼时IL-4也被认为是最可能应用于COPD领域的IL单抗方向。但现实却是多个IL-5单抗在COPD适应症上接连失利。
数据来源:公开数据整理、药智数据(点击查看大图)
直至2024年9月,GSK的Mepolizumab治疗COPD的Ⅲ期MATINEE研究取得了积极结果,并于2025年2月11日在中国申报上市。
IL-4单抗方面,由于IL-5单抗在COPD领域的接连失利,其幸运地迎来了反超机会,2024年7月赛诺菲/再生元合作开发的IL-4Ra单抗Dupixent(Dupilumab/度普利尤单抗)在全球率先获得欧洲药品管理局(EMA)批准用于治疗血液嗜酸性粒细胞(BEC)升高且未得到控制的COPD成人患者,从而摘得首款COPD生物药桂冠。
数据来源:公开数据整理、药智数据(点击查看大图)
在其主要临床终点中,度普利尤单抗AECOPD平均年恶化率分别降低30%和34%,且肺功能(支气管扩张剂前FEV1)在12周时较基线改善160mL和139mL,而基线时分别为77mL和57mL。Dupixent的成功进一步通过试验验证了IL-4和IL-13信号传导在COPD中的作用。
IL-33单抗方面,作为驱动病毒感染和诱发AECOPD的关键细胞因子,在COPD患者的血浆和支气管上皮中可明显观察到IL-33的过度表达。目前已有多款靶向IL-33的单抗正处于COPD的Ⅲ期临床试验阶段
数据来源:公开数据整理、药智数据(点击查看大图)
赛诺菲的IL-33单抗Itepekimab,目前已处于临床Ⅲ期阶段,其临床数据显示其虽对急性加重率降低无统计学意义,但对曾吸烟者COPD急性加重率降低>40%,赛诺菲对其年销售峰值预期达50亿欧元。
而国内领域的布局管线虽临床进度较上述两者有所不及,但也极具潜力,其分别是正大天晴的TQC-2938、荃信生物的QX-007-N与三生国健的SSGJ-621。
TSLP单抗方面,相比于IL-4R等靶点,TSLP位于更上游,位于多个炎症级联反应顶端,是2型炎症重要驱动因素,在各种类型的炎症和免疫类疾病中充当促炎细胞因子。
图片来源:《TSLP: from allergy to cancer》
靶向TSLP抗体通常是通过阻断TSLP与其受体之间的相互作用来抑制TSLP介导的信号通路,从而抑制DC细胞、肥大细胞、自然杀伤细胞、TH2细胞介导炎症反应。目前TSLP靶点肿瘤适应症开发布局较为集中,其中哮喘适应症的临床进展最快,而由于COPD与哮喘的关联性,导致TSLP单抗用于COPD治疗的研究也同样火热。
数据来源:公开数据整理、药智数据(点击查看大图)
截止目前,全球领域尚无任何一款TSLP单抗获批用于治疗COPD,临床推进最快的是安进与阿斯利康的Tezepelumab、博奥信生物的BSI-045B、诺华制药的Ecleralimab、荃信生物的QX-008-N,均已进入临床Ⅱ期。但同时,值得注意的是,在TSLP单抗用于COPD治疗的在研药物领域中,国内Biotech企业得管线数目却占比较高,后续有望成为全球该领域的主要力量。
双抗
原则上来讲,双抗较单抗,确实具备诸多技术优势,比如双重靶向下的协同作用使得它在处理肿瘤的异质性和复杂生物学特性时,比单抗有更全面的覆盖、在增强治疗效果、克服耐药性等方面优势明显。
也正是因此,全球制药企业不出意外的均将其作为潜在创新疗法布局,而在COPD领域,目前已有少数企业开始积极推进,靶点主要主要集中于TSLP+IL、IL+IL两大方向。
分类
药品名称
靶点
关键适应症与阶段
产品最高阶段
适应症最高临床阶段
原研单位
最新临床进展时间(近三年有进展即“活跃管线”)
双抗
HB-0056
IL11;TSLP
临床Ⅰ期:哮喘;慢性阻塞性肺病;特发性肺纤维化;特应性皮炎
临床Ⅰ期
临床Ⅰ期
华奥泰生物
2025-01-24
RC-1416
IL4RA;IL5
临床Ⅰ期:哮喘
临床申请:慢性阻塞性肺病;特应性皮炎;肿瘤
临床Ⅰ期
临床申请
融捷康生物
2024-10-17
PM1017
IL4RA;IL5
临床前:哮喘;嗜酸粒细胞增多症;慢性阻塞性肺病
临床前
临床前
普米斯生物
2022-08-12
数据来源:公开数据整理、药智数据
据不完全统计,COPD双抗领域目前以华奥泰生物的HB-0056推进最快,前已处于临床I期,其次是融捷康生物的RC-1416与普米斯生物的PM1017,分别处于临床申请与临床前阶段。
华奥泰生物的HB-0056,是以抗TSLP人源化单克隆抗体为亲本抗体,在N端连接抗IL-11(白细胞介素-11)单链纳米抗体的双特异性抗体,能高特异性地靶向TSLP和IL-11这两个靶点。而TSLP和IL-11均以不同的机制参与诱导Th2(辅助型T细胞2)反应、气道炎症和COPD的发病机制,两者可以互补作用来影响该疾病。
融捷康生物的RC-1416,可以选择性结合IL-4R和IL-5,同时下调由IL-4、IL-5和IL-13诱导的信号,显著抑制炎症性Th2(2型炎症因子)细胞,以及下游的参与炎症反应的嗜酸性粒细胞、肥大细胞、嗜碱性粒细胞的活性,对多种Th2通路诱导的疾病都具备治疗效果。而IL-5目前被认为是Th2通路的关键驱动因子之一,IL-5与其受体结合后进一步激活下游JAK-STAT信号通路。
普米斯生物的PM1017,可以同时阻断慢性阻塞性肺病患者体内IL-4/IL-13/IL-4Rα/IL-13Rα1,以及IL-5/IL-5Rα两条非冗余的信号通路,从而更大限度地抑制疾病进展,同时避免临床上使用度普立尤单抗治疗,患者发生的嗜酸性粒细胞增多症等副作用。皮下注射剂型加上工程化改造的Fc片段缩短给药频率,PM1017可以为患者提供更加便捷,安全,有效的治疗方案。
难以看清的未来趋势
对于绝大多数自免、慢病而言,其患者群体庞大是其最大的优势,更何况其临床上还存在大量未满足的临床需求,因此近年来逐渐成为全球创新技术领域除肿瘤外的最大竞争地。
而对于COPD新药研发而言,虽然现阶段IL、TSLP等靶向制剂均以单抗技术为主,但就疗法未来而言,其患者顺应性的弊端或许也将成为限制其发展的关键之处(调查显示至少超过20%的患者不愿意使用注射剂型)。
放眼隔壁的IL-17领域,目前全球范围内已有多家创新药企在尝试推进IL-17口服制剂,且不乏辉瑞、礼来、赛诺菲等MNC药企的身影。比如礼来DC-806折戟后寄希望的小分子IL-17靶向药DC-853,赛诺菲以700万美金首付从C4X引进的IL-17A临床前小分子抑制剂;强生/Protagonist首个口服IL-23受体的靶向口服肽JNJ-2113。
当然,考虑到COPD用药特殊性,此处的IL单抗口服趋势不一定完全适用(毕竟长久以来吸入制剂制在呼吸系统的临床地位明显高于口服小分子),未来大概率会做出因地制宜的改变,比如IL单抗的吸入制剂、TSLP吸入单抗等。
但可以肯定的是,随着未来COPD靶向生物药的发展,COPD单抗制剂的竞争加剧,关于患者顺应性的考虑或许会在恰当的时候,进入研究者的视野中。
小结
综上所述,从数十年前LABA、LAMA被临床应用于COPD治疗,再到如今临床上LABA+LAMA+ICS的临床联用方案,很明显COPD的新药研发较肿瘤、自免疾病而言,明显慢了很多。
固然,这一方面是由于COPD相关基础临床研究不足,另一方面也是由于COPD短期研发收益低于肿瘤、肥胖、自免等风口疾病领域。但这并不表示COPD领域的市场不大,不存在临床需求。相反,长时间的无药可用的压抑之下,或许还会造就COPD领域更加迫切的临床需求。
而从目前COPD新药在研的情况来看,一部分企业选择继续沿用传统研发路线,对老药进行新的优化与升级,过程中诞生了一系列新型LABA、新型LAMA以及双靶点支气管扩张剂(MABA)等等,比如成功打破COPD治疗僵局的恩塞芬汀;而另一部分企业则倾向于将在肿瘤、自免新药开发上获得的经验复制于COPD领域,积极推进IL单抗、TSLP单抗与靶向双抗,比如赛诺菲与再生元的度普利尤单抗、GSK的美泊利珠单抗。
目前来看,就老药新发展与靶向生物药两方面发展而言,预计未来很长一段时间,靶向生物药或将成为COPD新药的主线剧情,直到双抗同质化那天,而过程中也必将有越来越多中国Biotech企业从中崛起。
当然,无论是老药新用,还是靶向生物药的大趋势,对于目前COPD的临床需求而言,仍不够完美,或未来,在逆转COPD病程、针对病因治疗、解决患者顺应性需求方面,小分子与生物药能协同一起,为更核心的需求服务。
来源 | 博药(药智网获取授权转载)
撰稿 | 博药内容中心
责任编辑 | 八角
声明:本文系药智网转载内容,图片、文字版权归原作者所有,转载目的在于传递更多信息,并不代表本平台观点。如涉及作品内容、版权和其它问题,请在本平台留言,我们将在第一时间删除。
合作、投稿 | 马老师 18323856316(同微信)
阅读原文,是受欢迎的文章哦
上市批准
2024-05-13
摘要:全球超过3亿人饱受哮喘困扰,且发病率逐年增加,作为最常见的慢性疾病之一,哮喘激发机制复杂,异质性强,是一类免疫介导的炎症疾病。随着基于生理、病理等机制深入研究,陆续推出的治疗性小分子和激素药物已实现对大多数患者的控制和治疗,但仍有5%~10%的患者为难控制、难治疗性哮喘,即重度哮喘。近十年来,得益于生物医药的迅猛发展,蛋白、抗体类药物凭借高有效性、高特异性、高安全性成为关键的重度哮喘治疗药物,然而由于生物制剂通常经注射给药,不可无创、快速地递送药物直接入肺迅速吸收起效,故而临床中亟需起效快、便捷、经济、安全的吸入式生物制剂。本综述通过对哮喘发病机制的阐释,概括现行的小分子、激素类和生物类治疗药物,并总结吸入式哮喘生物制剂的研发历程,对其未来前景进行分析,旨在加深对大分子吸入药物研究方向的认知,更新该领域前沿动态,以期为更多吸入式生物制剂的开发提供参考。关键词:哮喘;给药途径;吸入给药;生物制剂_正文_支气管哮喘简称哮喘,以呼吸急促、咳嗽和胸闷等多种症状为特征,与慢性气道炎症,广泛、可逆性呼气性气流阻塞和气道高反应性等症状有关[1]。全球超过3亿人饱受哮喘困扰,且发病率逐年增加。根据全球哮喘指南全球哮喘防治创议(global initiative for asthma,GINA)建议,需对患者采用阶梯式治疗方案,尤其推荐个性化治疗方案。随着生物制剂的发展,抗体类生物制剂已成功应用至哮喘治疗,为中重度哮喘患者带来了更有效、更安全的药物选择,但其注射的给药方式,缓慢的起效速度,频繁的入院用药、高昂的用药成本在很大程度上限制了药物的推广,故而吸入式抗体药物的临床呼声日益高涨。本综述对哮喘机制、现有治疗药物及吸入抗体药物的开发历程进行了调查研究,以期加深对哮喘发病机制及治疗药物的全面认识,同时对吸入式抗体药物的开发必要性、开发难度、研发现状进行汇总更新。1哮喘发病机制哮喘传统上被分为两类,外源性哮喘和内源性哮喘,外源性哮喘又被称为过敏性哮喘,由过敏原引起,主要归因于异常的辅助性T细胞(helper T lymphocyte,Th)2型炎症。内源性哮喘是由多种因素引发的,如阿司匹林、肺部感染、运动、寒冷、压力、肥胖等[2]。根据Th2炎症的状态,哮喘疾病又被分为高Th2和低Th2哮喘[3]。高Th2哮喘的特征是嗜酸性气道炎症,这与血液中嗜酸性粒细胞数目的增加或呼出一氧化氮(fractional exhaled nitric oxide,FeNO)分数升高有关,而低Th2哮喘包括中性粒细胞哮喘和寡粒细胞性哮喘。哮喘的病理机制是复杂的,新研究表明,哮喘的发病机制也可不依赖于非免疫应答/炎症发生,但相关研究有限[4]。2哮喘标志物由于丰富的异质性外源、内源表型特征,哮喘非常适合精准治疗方案,因而非侵入性生物标志物的鉴别将有助于其诊断和治疗。Th2和2型固有淋巴细胞(innate lymphoid cells,ILC2)通路的激活是2型炎症哮喘发生的核心,Th2型细胞因子主要有一系列白介素(interleukin,IL),如IL-4、IL-5、IL-9、IL-13、IL-31,而ILC2s产生的2型细胞因子主要有IL-5、IL-9和IL-13,上述因子均为哮喘有效标志物。嗜酸性粒(eosinophil,EOS)细胞、免疫球蛋白(immunoglobulin,Ig)E、表达ILC2s的循环趋化因子受体(cyclic chemokine receptor,CCR)10、血浆CCL(CC chemokine ligand)27水平和Fe-NO是哮喘诊断和预后的常见生物标志物。此外,如图1所示,IgE、IgG亚族,血清IgE抑制活性,嗜碱性粒细胞活化,趋化因子和细胞因子,调节性T(regulatory T,Treg)细胞,调节性B(regulatory B,Breg)细胞和树突状细胞等标记物已被推荐作为跟踪过敏原耐受诱导治疗的生物标记物[5]。3哮喘现有小分子、激素治疗药物GINA指南推荐使用药物种类包括糖皮质激素、β2-受体激动剂、胆碱能受体阻断药物、茶碱类药物、白三烯受体拮抗剂和生物靶向制剂[6]。除上述药物外,基于创新机制的新型小分子药物研发处于临床研究不同阶段,如正大天晴的前列腺素D2受体拮抗剂(又称为CRTH2拮抗剂)TQC3564正在中国临床I期研究阶段;针对磷酸二酯酶4(PDE4)抑制剂的NCT04108377正处于临床I期患者招募阶段。此外,基于蛋白激酶抑制剂(NCT00676572)、选择性糖皮质激素受体调节剂(AZD7594)、他汀类药物(NCT02433535)均以控制哮喘为目标并处于临床开发中[7]。新型小分子哮喘治疗药物的有效开发离不开对哮喘机制以及哮喘的不同表型和内型的理解,但从临床效果上看,针对中重度哮喘,生物制剂展现出更加明确的应用前景,因此在另一方向上,生物靶向药物的发展也在高歌猛进,力求在新维度上实现哮喘疾病的控制及治疗。4哮喘现有靶向治疗药物随着病情严重,在以糖皮质激素为基础治疗后仍会出现控制不佳、反复重症发作等情况,此时患者即可被认定是重度患者,高达10%的成人和2.5%的儿童哮喘群体患有重度哮喘,因固定气流受限、病情恶化、常年就医、住院和死亡风险的增加等因素致使生活质量严重下降。因此,在整个哮喘患者谱系中,重症哮喘患者是临床中最迫切的未满足医疗需求群体,目前推荐的有效控制方案是生物制剂添加疗法。目前共6款针对Th2通路的哮喘治疗性单克隆抗体获批,包括靶向IgE的奥马珠单抗(omali-zumab)、靶向IL-5的瑞替珠单抗(reslizumab)、IL-5受体药物贝那利珠单抗(benralizumab)、针对IL-4Rα的度普利尤单抗(dupilumab)以及靶向TSLP的特泽鲁单抗(tezepelumab)。目前针对低Th2型、中性粒细胞为主的重度哮喘发病机制相关分子靶点的试验性药物非常稀缺,因此,针对不同表型基础生物学机制的深入研究将对临床有关重度哮喘治疗方案的开发起到关键性驱动作用[8]。抗体类生物制剂的获批为重度哮喘病人带来了更新、更安全、更有效的治疗方式,表1对Th2通路相关靶点哮喘治疗药物关键信息进行统计,以期对哮喘生物制品有更为系统的理解。上述靶向药物已在临床试验及疾病用药过程中验证了有效性和安全性,多种潜在疾病治疗靶点药物研发正在进展中,包括细胞因子、膜分子和细胞内信号通路,如IL-37、IL-11,基质相互作用分子1(STIM1),CD200R、OX40L和CD30L、HMGB等[9]。5吸入式大分子哮喘治疗药物发展现状5.1 药物通过吸入途径递送的优势吸入给药(肺给药)可快速、无创地输送至呼吸道并传导至肺部,肺内巨大的表面积和广泛的血管分布能使药物快速吸收并发挥治疗效果,其剂量对身体其他部位的暴露量较低,可最大限度地减少全身性不良反应。吸入给药是一种无创的局部和全身给药方式,在治疗多种疾病方面具有巨大的潜力,已应用于包括哮喘、慢性阻塞性肺疾病、呼吸道病毒感染和糖尿病、囊性纤维化等多种疾病领域[10]。吸入给药作为治疗呼吸系统疾病优选的给药方案,可满足如下几项对给药方式的特殊需求[11]:(1)药物通过系统性给药在肺内很难达到有效富集的药物浓度,生物利用度低,而吸入给药具有肺内高浓度的优势。(2)当以达到肺部有效治疗浓度为目标给药时,药物剂量通常较大并呈现全身性毒性,吸入给药用药量低,规避胃肠降解作用和肝脏首过效应,安全性更好。(3)需要快速起效的肺部疾病治疗药物,吸入给药可快速实现肺部药物沉降,并由于肺部表面积大、血管化丰富、组织通透性好,药物可以快速吸收并起效。(4)在确保肺部疾病治疗药物药效的同时,若对用药成本关注,亦通过吸入给药的方式改进。5.2 吸入制剂的临床应用吸入型产品可分为雾化溶液吸入、干粉吸入和软雾吸入三大种类,吸入制剂被广泛应用于多种呼吸系统疾病领域[11]:如(1)糖皮质激素、β2受体激动剂、毒蕈碱乙酰胆碱受体拮抗剂等激素和小分子类吸入制剂(组合)用于哮喘和慢性阻塞性肺疾病治疗。(2)妥布霉素、氨曲南赖氨酸盐、左氧氟沙星、阿米卡星、多粘菌素、神经氨酸酶抑制剂、利巴韦林、喷他脒等吸入制剂在抗感染领域的应用。(3)吸入重组人脱氧核糖核酸酶在囊性纤维化适应症的治疗应用。(4)吸入甘露醇在气道黏液清除、囊性纤维化及支气管扩张中的应用。(5)吸入前列腺环素发挥血管扩张机制用于肺动脉高压的治疗。(6)吸入肺表面活性剂用于呼吸窘迫综合征的治疗。(7)吸入核酸药物如重组新型冠状疫苗在抗病毒感染领域的开发应用。吸入制剂主要应用在呼吸系统疾病领域,但从口鼻吸入通过呼吸道将药物递送至肺部并交换进入体循环,也为系统性疾病的治疗提供了创新性的方案[11]。在中枢神经系统领域,尼古丁吸入剂(器)已在尼古丁替代疗法中得到成功应用以减轻或摆脱尼古丁依赖。全球首款左旋多巴吸入粉雾剂INBRIJA®已在美国和欧盟获批上市用于帕金森的吸入治疗。糖尿病领域,辉瑞与Mannkind曾先后获批两种吸入胰岛素药物Exu-bera®与Afrezza®,为糖尿病治疗提供了新的治疗选择。5.3 吸入大分子药物在哮喘治疗领域的开发现状抗体具有高特异性、高亲和力和高安全性等优势,已被广泛用于治疗肺部疾病,如肺癌和严重哮喘。目前共有6款针对重度哮喘的单克隆抗体上市,并取得了优异的临床治疗效果。然而,已上市产品均以皮下注射或静脉输注方式递送,其局限性包括侵入性、系统毒性(如细胞因子风暴),需专业医师操作等因素使得大量患者难以院外治疗。因此,吸入给药凭借直接呼吸道给药,无创、局部效应增强、全身暴露最小和易于自我给药等优点,已在多个吸入性单克隆抗体及其衍生物在临床试验中得到治疗潜力的评估[12],表2汇总了吸入式生物制剂在哮喘领域的简要总结。5.3.1 吸入单克隆抗体/片段诺和诺德及诺华曾在轻度过敏性哮喘患者中开展了奥马珠单抗自我雾化给药疗效研究,虽然33名受试者在分别连续雾化用药2周和8周后血清中均检测到奥马珠单抗,但血清IgE水平无明显变化,变应原诱导的气道反应不受抑制,推测无效的原因是肺组织中覆盖IgE效应细胞的奥马珠单抗浓度不足,无法中和肺部产生的IgE。此外,一名受试者产生了抗奥马珠单抗抗体,这也令人担心吸入单抗可能比注射给药免疫原性更强[13]。2014年,来自比利时的研究团队发表了关于雾化吸入抗原结合片段(fragment of antigen binding,Fab)在哮喘小鼠模型(NMRI)中的研究结果[14],该研究通过聚乙二醇化延长了IL-17A Fab2和IL-13Fab双抗在呼吸道局部停留时间,肺内聚乙二醇化抗体含量在给药后4h达到平台期,而未成功偶联聚乙二醇的抗体则入肺后就开始清除,研究阐释了聚乙二醇化修饰对治疗性蛋白局部递送到肺部后的长效具有显著效果。此后,该团队又相继针对不同分子量聚乙二醇分别对IL-17A Fab和IL-13Fab长效后肺部沉积进行了探索,上述研究主要聚焦肺部药物长效化机制研究,并未对抗体靶点组合的药效及成效性进行深入探索,但初步论证了吸入抗体给药途径的可行性。比利时布鲁塞尔的优时比制药(UCB Pharma)在食蟹猴过敏性哮喘模型中布局了针对雾化吸入IL-13靶点Fab抗体CDP7766的研究,该研究发现通过振动网筛雾化器产生的气溶胶仍保持优异的分子活性及纯度,没有明显的降解和聚体产生,并且在动物模型中表现出良好的耐受性,未观察到局部刺激相关的不良反应,并显著抑制了肺泡灌洗液中过敏原诱导的细胞因子和趋化因子的上调,临床上可快速持久地抑制FeNO,健康和哮喘受试者均表现出良好的耐受性(NCT02473939),证明了吸入性抗IL-13抗体片段药物治疗过敏性哮喘的潜力[15]。Faghihi等通过喷雾干燥将肿瘤坏死因子α(tumor necrosis factorα,TNFα)单克隆抗体Infliximab开发成干燥粉剂,用于局部炎症性哮喘治疗,探讨通过吸入给药途径抑制肺部分泌TNFα的可行性,但其粉剂分子与TNFα结合降低了21%,在卵清蛋白刺激小鼠哮喘模型中表现出的TNFα分子抑制活性相对于单抗降低了2个数量级,虽然抗体干粉开发成功与否主要取决于喷雾干燥条件、配方成分及抗体雾化稳定性,但该研究初步提示了单克隆抗体并不合适用于吸入制剂开发[16]。CSJ117是诺华布局的一款针对TSLP靶点的Fab拮抗剂(Ecleralimab),CSJ117采用粉雾剂药物开发方式用以治疗成人轻度特应性哮喘,在其I期临床研究(NCT03138811)中,CSJ117耐受性良好,并减轻过敏原激发后的支气管收缩[17]。2020年诺华启动了一项II期试验,目的是研究CSJ117治疗未得到控制的重度哮喘的药效和安全性研究(NCT04410523),II期临床研究已完成,但暂未数据揭盲,并且由于诺华产业战略调整,该项目暂停了后续开发,正在积极寻求合作转让。安进及阿斯利康在携手成功推出TSLP单克隆抗体Tez-epelumab商业化上市后,快速对上市药物分子进行工程化改造将单克隆抗体皮下注射液开发成为Fab干粉吸入剂型,项目代码为AMG104/AZD8630,该项目已于2022年启动临床I期研究,以评估安全性、耐受性和药代动力学(NCT05110976)。5.3.2 吸入纳米抗体除了单克隆抗体及抗体片段外,诸如Nanobodies®、Anticalin®、Affibody®等新型蛋白骨架类型在基于蛋白质的吸入治疗领域引起了轰动。与全长单克隆抗体相比,新型蛋白骨架体积较小、结构简单,更容易结合隐蔽结合位点、组织渗透面积更大、药物聚集更方便、热稳定性更强[18]。纳米抗体是由驼科动物体内重链抗体(95kDa)可变区扩增而来的单域抗体,又称为VHH抗体(variable domain of heavy chain of heavy-chain antibody,VHH),从属于基因工程抗体范畴。纳米抗体晶体尺寸直径2.5nm,长4nm,是目前可与抗原结合的最小片段。2018年,首创的Nano-body®caplacizumab(Cablivi®)获得欧洲药品管理局的首个上市许可,用于治疗获得性血栓性血小板减少性紫癜,虽然caplacizumab是肠外用药,但吸入型Nanobody®平台及产品一直在临床开发中。吸入型抗合胞病毒纳米抗体药物ALX-0171的安全性和耐受性已在一项首次婴儿I/IIa期临床试验中得到证实,并观察到抗病毒活性[19]。尽管IIb期剂量范围研究已经完成(NCT02979431),但在下呼吸道感染和炎症发生的基础上,继续雾化ALX-0171并不能改善临床治疗结果,所以该项目未达预期而被搁置研究,但该研究表明ALX-0171在早期的使用干预可产生重要的临床抗病毒作用。随着新冠疫情爆发,许多纳米抗体也被开发成吸入制剂以对抗SARS-CoV-2感染,如洛启生物的Nb11-59表现出强效的体外真病毒中和活性[20]。在哮喘类领域,目前有两款来自洛启生物的纳米抗体吸入产品处于中国临床I期开发阶段,洛启生物靶向IL-4Rα的LQ036产品适应症为嗜酸性粒细胞哮喘,LQ043H靶向TSLP,其适应症为非嗜酸性粒细胞哮喘。LQ036与LQ043H是目前全球推进速度最快的同靶点吸入纳米抗体产品。LQ036及LQ043H均具有优异的体外阻断活性,并按照吸入制剂开发标准进行了完整的空气动力学研究,具有雾化后粒径均匀、生物活性完整保留、药物纯度稳定等优势,同时两款产品均采用毕赤酵母生产系统表达,产量高,工艺简单,药物成本优势明显。LQ036已完成针对安全性、耐受性、免疫原性和药代动力学的澳洲临床I期研究(NCT04993443),安全性、耐受性优异,无药物相关免疫原性发生;目前该项目正处于中国临床I期开发阶段,评价雾化经口吸入LQ036在中国健康受试者体内的耐受性、安全性、免疫原性和药代动力学(CTR20223011)。洛启LQ043H项目同期处于中国临床I期研究阶段,评价LQ043H单域抗体雾化液在中国健康受试者中单次给药后的耐受性、安全性、药代动力学和免疫原性(CTR20230092)。此外,LQ036的慢性阻塞性肺疾病适应症IND申请获得国家药监局药品审评中心(CDE)受理(受理号:CXSL2300435)。LQ036和LQ043H的顺利推进将为纳米抗体在吸入给药方向上的临床应用提供有力支持,并创新性地为哮喘和慢性阻塞性肺疾病患者提供更有效、更安全、更便捷、更经济的治疗方案。5.3.3 吸入类抗体骨架蛋白Anticalin®是Astra Zeneca与Pieris公司蛋白研发平台推出的一类基于丰富血浆及体液来源脂质运载蛋白骨架修饰开发而成的工程化蛋白,通过对脂质运载蛋白1进行定向蛋白质突变,经过系统性修饰推出了Elarekibep项目(PRS-060),Elarekibep是一款靶向IL-4Rα的高亲和力、缓慢解离、长效拮抗剂,用于治疗中度至重度哮喘。Elarekibep的小尺寸和稳定性使其可以被直接吸入肺部,其临床I期以雾化液方式开展,试验显示轻度哮喘患者的FeNO水平显著降低(NCT03384290,NCT03574805)。在其干粉吸入制剂临床II期向3mg及1mg更低剂量组进行药效探索时,其非人类灵长类动物长期毒性研究出现了非药物剂量依赖的炎症介导的肺组织损伤,随即其合作方阿斯利康终止了该项目后续临床开发(NCT04643158)。该项目的失败原因更多指向于Anticalin®平台分子自身结构毒性问题,这一结论为类抗体支架蛋白Anticalin®的未来研发应用蒙上了阴影[21]。Affibody®是Affibody公司推出的一类新型抗体模拟物,该类药物是由58个氨基酸残基组成的新型亲和配体,相对分子质量约为6500,由3个螺旋结构组成,功能与抗体相似,但具备相对分子质量小、折叠速度快、选择性和亲和力高、结构稳定等优势。Affibody最近宣布接受Chiesi投资,使用Affibody专有技术布局开发呼吸系统疾病吸入性创新疗法,根据公司最新官网更新,ABY-062作为一种靶向TSLP的候选药物,很有可能是按照吸入式治疗药物方向开发,这也意味着吸入大分子药物开发行列迎来了新抗体骨架Affibody®的加入,我们期待其在吸入性创新疗法上的表现。5.3.4 吸入重组蛋白除吸入抗体类药物之外,重组蛋白也曾尝试开发成吸入制剂。拜耳医药曾尝试过IL-4蛋白突变体雾化吸入开发方向,Pitrakinra(AER-001,BAY-16-9996)是IL-4蛋白的变体,具有2个氨基酸变化,使其能够结合IL-4Rα链并抑制IL-4Rα与γC或IL-13Rα1的相互作用。在Pitrakinra的一项II期临床研究中,吸入Pitrakinra可减弱过敏原激发后哮喘受试者的晚期哮喘反应和气道炎症,但对哮喘患者应对过敏原挑战的肺功能没有显著影响[22]。虽然在一项药物遗传学研究中,在携带IL-4Rα基因特异性单核苷酸多态性的患者中,Pitrakinra显著降低哮喘急性发作的频率,但最终其临床III期不明原因并未继续推进。Altrakincept是一款通过雾化给药开发的竞争性重组人可溶性IL-4Rα蛋白,已在临床试验中进行了测试,并证明可预防中重度哮喘患者因停用皮质类固醇而导致的肺功能恶化,但进一步的长期研究结果令人失望,该项目也未再进一步推进[23]。6小结在过去的15年里,生物制剂的开发和临床应用显著扩大,但这些药物的给药途径仍主要以局部或系统性注射为主,吸入抗体是一种明显的无创替代方案,为多种疾病的局部治疗提供了机会,尤其对于呼吸系统疾病治疗,同时也尝试应用于系统性疾病的治疗。但由于抗体三维结构复杂,三级结构是其作用的核心,在吸入给药过程中遭受各种应力下容易产生降解和聚体,这种结构的破坏严重影响产品有效性和安全性等性能的评估,所以维持其结构完整性和生物活性对于成功开发吸入性生物制剂至关重要,这无疑对分子特性、配方设计、辅料选择、加工工艺和吸入装置等方面提出了系统性挑战。后续基础研究对上皮细胞转运机制的理解,辅助抗体稳定性、吸收和雾化性能的相容性赋形剂的开发,适配性更高、便携性更好、操作更便捷吸入装置的开发等都会对吸入抗体药物的开发提供更坚实的开发基础。并且随着纳米抗体、抗体片段、抗体骨架等新形式生物制剂的诞生为更多创新药物的开发提供了保障,未来我们期待更多吸入相关创新技术的诞生。总而言之,吸入型生物制剂的开发是一个系统过程,需要全面、充分考虑发病机理、患者群体、药物分子类型选择及其与肺内生物屏障的相互作用等因素,并合理地选择制剂、赋形剂和装置,同时也涉及上述学科和领域的共同发展。我们希望未来会有治疗效果更佳、安全数据更好、自行用药更便捷、药物价格更低廉的吸入生物制剂产品的诞生以满足日渐复杂、日益壮大的临床未满足需求。参考文献详见《中国临床药理学与治疗学》 2024 Apr; 29(4)识别微信二维码,添加生物制品圈小编,符合条件者即可加入生物制品微信群!请注明:姓名+研究方向!版权声明本公众号所有转载文章系出于传递更多信息之目的,且明确注明来源和作者,不希望被转载的媒体或个人可与我们联系(cbplib@163.com),我们将立即进行删除处理。所有文章仅代表作者观点,不代表本站立场。
2024-01-09
GSK moved quickly to add the long-acting anti-TSLP antibody to its portfolio,
Well, that was fast. Seventy seven days after Aiolos Bio launched to the public, GSK has disclosed a deal to buy the biotech and its phase 2 asthma treatment for $1 billion upfront and up to $400 million in regulatory milestones.
Aiolos broke cover in late October, launching with a $245 million series A round co-led by Atlas Venture, Bain Capital Life Sciences, Forbion and Sofinnova Investments. The biotech raised the money to fund the development of a long-acting anti-TSLP monoclonal antibody, AIO-001, that it picked up from Jiangsu Hengrui Pharmaceuticals two months earlier.
Other companies got to the TSLP opportunity before GSK. Amgen and AstraZeneca won FDA approval for an anti-TSLP antibody, Tezspire, late in 2021. Novartis hung a 'for sale' sign on its midphase TSLP prospect, CSJ117, months after the FDA authorized Tezspire.
GSK has weighed up the competition and bet up to $1.4 billion on AIO-001. In a statement, Tony Wood, chief scientific officer at GSK, called AIO-001 a potentially best-in-class medicine that could expand the company’s biologics portfolio to the 40% of severe asthma patients with low T2 inflammation.
Post-hoc analyses of phase 2/3 trials of Tezspire linked the antibody to reductions in exacerbations in T2 low asthmas, a subgroup that other drugs, including GSK’s Nucala and phase 3 prospect depemokimab, aren’t designed to treat. Tezspire’s broad efficacy led the FDA to make it the first asthma drug approved for severe asthma without phenotypic limitations, such as eosinophilic, or biomarker restrictions.
The belief that AIO-001 can improve on Tezspire rests, in part, on its dosing schedule. Tezspire is given subcutaneously once a month. GSK believes the “enhanced potency and half-life extension technology” of AIO-001 could support dosing every six months. The Big Pharma’s work on the HIV drugs Cabenuva and Apretude has shown how longer-lasting medicines can win market share.
GSK, which will acquire rights to AIO-001 outside of Greater China, plans to run a phase 2 trial in adults with asthma and is assessing whether to expand development into other indications, including chronic rhinosinusitis with nasal polyps. Amgen and AstraZeneca are running phase 3 trials of Tezspire in people with chronic rhinosinusitis and eosinophilic esophagitis.
The deal represents another successful exit for Aiolos CEO Khurem Farooq, who co-founded the biotech with Tony Adamis, M.D., after leading Gyroscope Therapeutics to an $800 million takeover by Novartis.

上市批准临床3期并购临床2期免疫疗法
100 项与 Ecleralimab 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 哮喘 | 药物发现 | 美国 | 2020-09-09 | |
| 哮喘 | 药物发现 | 加拿大 | 2020-09-09 | |
| 哮喘 | 药物发现 | 匈牙利 | 2020-09-09 | |
| 哮喘 | 药物发现 | 波兰 | 2020-09-09 | |
| 哮喘 | 药物发现 | 拉脱维亚 | 2020-09-09 | |
| 哮喘 | 药物发现 | 日本 | 2020-09-09 | |
| 哮喘 | 药物发现 | 斯洛伐克 | 2020-09-09 | |
| 哮喘 | 药物发现 | 俄罗斯 | 2020-09-09 | |
| 哮喘 | 药物发现 | 阿根廷 | 2020-09-09 | |
| 哮喘 | 药物发现 | 比利时 | 2020-09-09 |
登录后查看更多信息
临床结果
临床结果
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
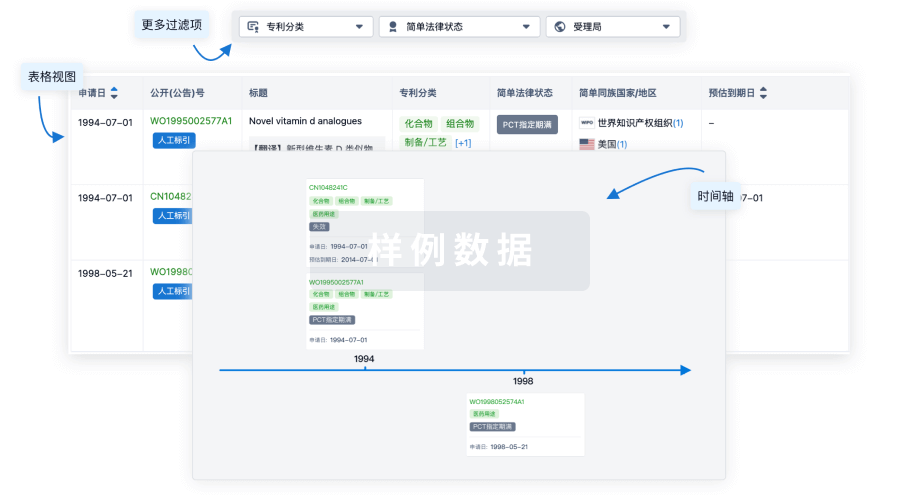
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
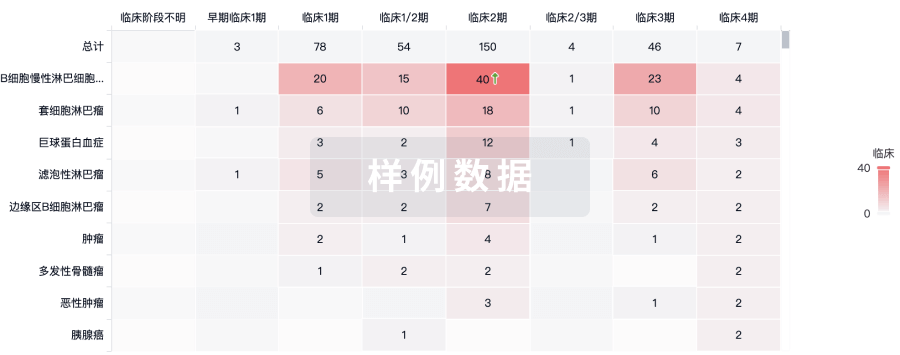
批准
利用最新的监管批准信息加速您的研究。
登录
或
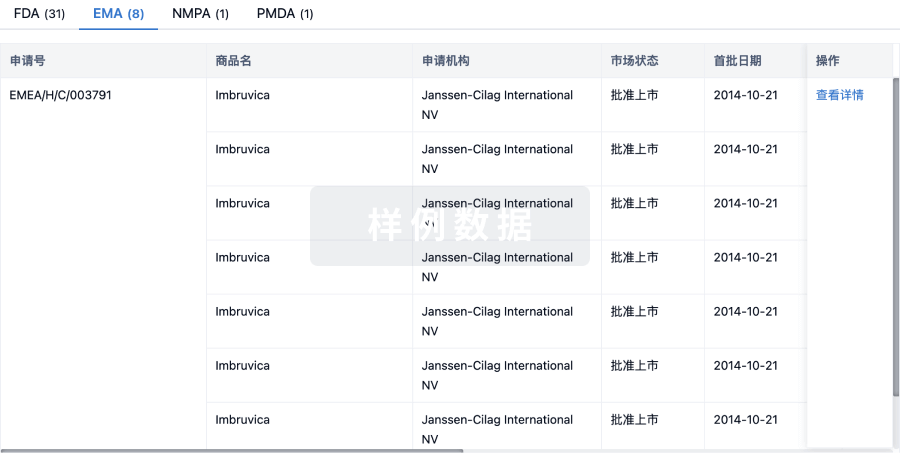
生物类似药
生物类似药在不同国家/地区的竞争态势。请注意临床1/2期并入临床2期,临床2/3期并入临床3期
登录
或
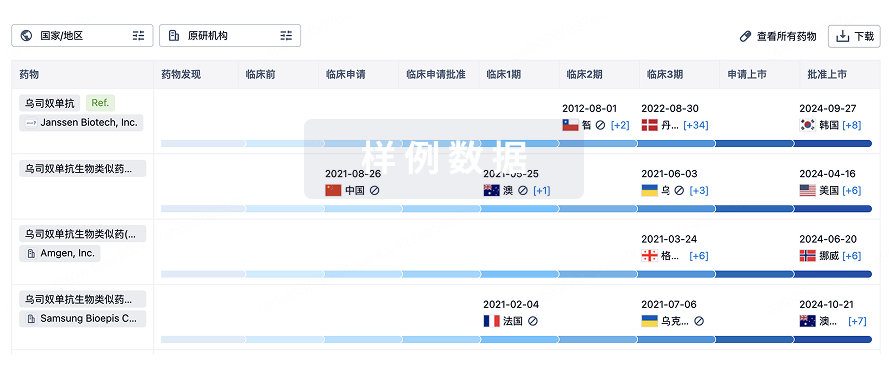
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
Eureka LS:
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用