更新于:2024-05-16
Glyceryl Nitrate
硝酸甘油酯
更新于:2024-05-16
概要
基本信息
原研机构 |
在研机构 |
最高研发阶段批准上市 |
首次获批日期 中国 (1987-01-01), |
最高研发阶段(中国)批准上市 |
特殊审评- |
登录后查看首次获批时间轴
关联
7
项与 硝酸甘油酯 相关的临床试验A Cohort Prospective Study of Predictors Influencing the Quality of Visualization of the Operating Field During Orthognathic Surgery
It is very important to decrease the bleeding during bimaxillary osteotomy in order to increase the visibility of the surgical site. Our primary goal is to investigate the predictive value of pre- and perioperative factors, including controlled hypotension, on visibility of surgical site during bimaxillary osteotomy.
开始日期2023-05-29 |
申办/合作机构- |
一项单中心、随机、开放、单剂量给药评价硝酸甘油喷雾剂在中国成年健康受试者中的四周期、完全重复、交叉生物等效性试验
主要研究目的
研究在中国成年健康受试者中受试制剂硝酸甘油喷雾剂与参比制剂硝酸甘油喷雾剂(商品名:保欣宁®)的药代动力学特征,评价两制剂的人体生物等效性。
次要研究目的
观察受试制剂与参比制剂在中国成年健康受试者中的安全性。
开始日期2023-03-08 |
申办/合作机构 |
Comparison the effectiveness of the use of glyceryl three nitrate ointment and mefenamic acid on pain, headache, and gastrointestinal disorders in primary dysmenorrhea women aged 18 to 30 years old without delivery
开始日期2013-05-05 |
申办/合作机构- |
100 项与 硝酸甘油酯 相关的临床结果
登录后查看更多信息
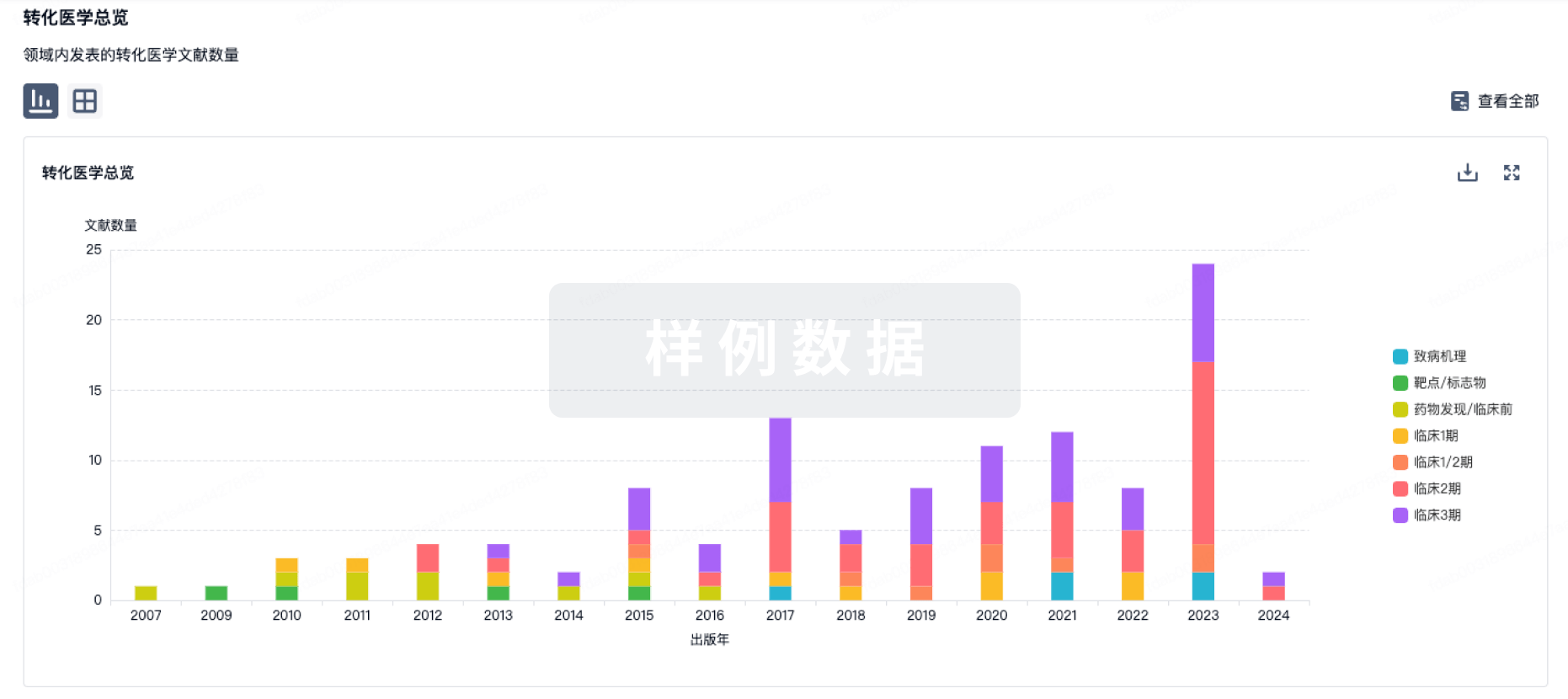
100 项与 硝酸甘油酯 相关的转化医学
登录后查看更多信息
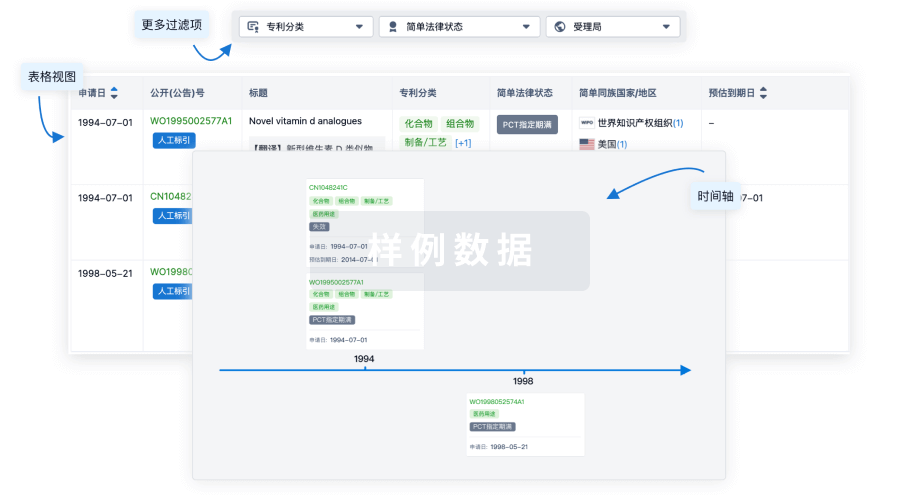
100 项与 硝酸甘油酯 相关的专利(医药)
登录后查看更多信息
16
项与 硝酸甘油酯 相关的文献(医药)2021-12-11·Cureus
The Dilemma: Whether to Proceed or Postpone a Patient With Pyrexia at Induction of Anesthesia for Coronary Artery Bypass Graft Surgery
作者: Fernandez, Jose A ; Bennett, Sean R ; Alnouri, Muneeb
2012-05-01·Respiratory Physiology & Neurobiology4区 · 医学
Effect of sublingual nitrate on respiratory reflexes arising from stimulation of juxta-pulmonary capillary (J) receptors by i.v. lobeline and short duration exercise
4区 · 医学
Article
作者: Hans Raj ; Niraj Srivastava ; Ashima Anand
2012-04-01·European Journal of Clinical Pharmacology
Amiodarone-induced acute hepatotoxicity
Letter
作者: Usha Rao ; Ajit Agarwal
9
项与 硝酸甘油酯 相关的新闻(医药)2024-05-13
·梅斯医学
自2017年,中华医学会心血管病学分会基础研究学组、介入心脏病学组、女性心脏健康学组以及动脉粥样硬化和冠心病学组编写了国际上第一部“冠状动脉微血管疾病(CMVD)诊断和治疗的中国专家共识”以来,国际上关于CMVD的共识文件迅速增加,例如2019年,AHA发表了MINOCA诊断和治疗的科学声明,指出微血管性心绞痛、微血管痉挛和冠脉慢血流是MINOCA的重要病因。2020年,欧洲经皮心血管介入协会(EAPCI)和ESC联合发布了冠状动脉非阻塞性心肌缺血(INOCA)的共识性文件,提出CMVD和/或心外膜下冠脉痉挛是INOCA 的主要病因。2020年,ESC发表了心血管疾病中冠状动脉微血管功能异常的立场文件,将微血管性心绞痛归纳为慢性冠脉综合征的重要类型,提出了相应的诊断和治疗策略。尽管部分文件对CMVD的诊断和治疗提出了初步建议,但并未提供推荐分类和证据等级。2023版中国专家共识总结CMVD近年进展,更新旧版共识中过时的观点,规范CMVD诊断和治疗,以及凝练科学问题和研究方向。近日,在2024长安国际心血管病论坛(CIC2024)上,来自山东大学齐鲁医院的张运院士对《冠状动脉微血管疾病诊断和治疗的中国专家共识(2023版)》进行详细解读,该共识提出了新的CMVD分类,,推荐诊断途径、标准及治疗策略。本文梳理重点内容,以分享各位同道。CMVD的定义冠状动脉微血管疾病(coronary microvascular disease,CMVD)是指在动脉粥样硬化性和非动脉粥样硬化性致病因素的作用下,冠状前小动脉、小动脉和毛细血管的结构和功能异常所导致的急性和慢性心肌缺血的临床综合征。CMVD的临床分型心肌缺血相关的CMVD:冠状动脉阻塞性心肌缺血(IOCA)相关的CMVD冠状动脉非阻塞性心肌缺血(INOCA)相关的CMVD心肌梗死相关的CMVD:冠状动脉阻塞性心肌梗死(MIOCA)相关的CMVD冠状动脉非阻塞性心肌梗死(MINOCA)相关的CMVD血运重建相关的CMVD:急诊PCI相关的CMVD择期PCI手术相关的CMVDCABG相关的CMVD非动脉粥样硬化心脏病相关的CMVD:合并心肌肥厚的CMVD不合并心肌肥厚的CMVD冠状动脉血流的调节机制冠脉血流量是指心脏冠状动脉血液在单位时间内的流量。影响冠脉血流量大小的主要因素是心肌的活动。此外,神经和激素对冠状动脉血流量也具有一定的调节作用。调节冠脉血流量的因素主要有物理因素、代谢因素、神经体液因素和自身调节。其中最重要的是代谢因素,即心肌本身的代谢水平。不同冠脉节段的血管舒缩受不同机制调节:血流介导的血管扩张:主要发生在心外膜下冠状动脉和前小动脉;冠脉血流自动调节:机制可能为前小动脉远端的肌源性反应,即冠脉灌注压上升时前小动脉收缩,反之则扩张;心肌耗氧量:心肌耗氧量增加时,冠脉阻力血管可充分扩张以满足心肌的需求,称为功能性充血,NO、前列环素、内皮素等参与调节;心肌代谢产物:当心肌缺血缺氧时,代谢产物的堆积首先使冠状小>动脉扩张,冠脉阻力和前小动脉的压力下降,触发冠脉的肌源性反应,血管进一步扩张,触发血流介导的血管扩张,使心外膜下的冠脉和较大的前小动脉扩张(级联式反应)。冠脉血流储备1974年Gould 首次提出冠脉血流储备(CFR)的概念。CFR是指冠脉接近最大程度扩张时,冠脉血流量(coronary bloodflow,CBF)或心肌血流量(myocardⅡal blood flow,MBF)与静息状态下相应指标的比值,是测量冠脉储备功能的整体指标。CFR受到4个因素的影响:静息状态的冠脉血流量(静息状态血流量增大可使CFR降低)、单位体积心肌内阻力血管的横截面积(管壁增厚可使CFR降低)、冠脉血管外的压力(室壁张力增加可使CFR降低)和冠脉灌注压(血压下降可使CFR降低)。CMVD的发病机制CMVD发病机制较为复杂,在疾病发展进程中受诸多因素影响。新共识在此方面新增了冠脉血流的调节机制、微血管阻塞,同时对冠脉微循环结构和功能异常方面的机制进行了更新。1、冠状动脉微血管结构异常:遗传因素(RAAS、过氧化物酶体增殖物激活受体及内皮素等基因的多态性);血流动力学因素(持续血压升高引起的剪切力变化);神经体液机制(高血压状态下RAAS激活、细胞因子、黏附分子及内皮素等高表达以及炎性细胞积聚)。2、冠状动脉微血管阻塞(microvascular obstruction,MVO)3、冠状动脉微血管功能异常:内皮依赖性血管舒张异常非内皮依赖性血管舒张异常微血管痉挛心脏交感神经元功能障碍评价冠脉微血管功能的血管活性药物通过检测冠脉微血管对血管扩张剂的反应来评估其功能,常用指标是CFR。1、内皮非依赖型血管扩张剂:主要作用于血管平滑肌细胞腺苷:静注剂量140μg/Kg/min,冠脉内注射剂量2-16μg/Kg/min,注射时间1.5-6分钟。常见的副作用有AVB、SAB、支气管痉挛。半衰期仅10秒,副作用可很快消失。双嘧达莫:通过抑制腺苷降解而发挥作用,药理作用类似于腺苷。静注剂量0.56-0.84 mg/Kg。应用腺苷或双嘧达莫后CFR<2.5提示冠脉微血管舒张功能异常,临床上推荐CFR<2.0作为判断微血管功能障碍的临界值。2、内皮依赖型血管扩张剂:主要作用于血管内皮细胞乙酰胆碱的双重性:刺激内皮细胞释放NO扩张血管,结合毒碱样乙酰胆碱受体刺激平滑肌细胞收缩血管。内皮功能正常时,乙酰胆碱的扩血管作用占主导地位,但如出现内皮功能异常乙酰胆碱的缩血管作用占优势,从而导致血管痉挛。用法和用量:乙酰胆碱稀释后冠脉内递增式注射,注射1分钟后行冠脉造影,利用定量造影法测量冠脉内径以明确有痉挛,同时观察心绞痛症状和心电图变化。如注射后未见心外膜下冠脉痉挛但出现心绞痛症状和缺血型ST-T改变,可诊断为CMVD,同时应立即冠脉内注射硝酸甘油或尼可地尔以对抗冠脉微血管痉挛。瑞加诺生:选择性激活腺苷A2A受体使冠脉扩张,增加冠脉血流量,具有选择性扩张冠脉和起效迅速的特点。用法和用量:10秒内一次性固定剂量弹丸式快速静脉注射给药,0.4 mg/5 ml。尼可地尔:硝酸酯类和腺苷三磷酸敏感性钾通道开放剂,激活细胞内的鸟苷酸环化酶,松弛血管平滑肌,兼具舒张心外膜动脉及冠脉微血管的功能。用法和用量:冠脉内弹丸式注射2~4 mg,作用效果及维持心肌最大充血状态的持续时间存在一定的剂量依赖性。CMVD的诊断CMVD的临床表现多样、机制复杂,且常规药物疗效有限,因此早期检出CMVD具有十分重要的临床意义。新共识更新了评价冠脉微血管功能的相关内容,指出诊断流程,同时整理了各亚类疾病的临床表现和诊断标准。临床评价冠状动脉微血管功能的检查主要包括:血管活性药物试验、无创伤性诊断技术和创伤性诊断技术等三类:血管活性药物试验:除了腺苷、双嘧达莫、乙酰胆碱,共识新增了腺苷A2A受体选择性激动剂Regadenoson和尼可地尔。无创伤性诊断技术:经胸超声冠脉血流显像(TTDE)、心肌声学造影(MCE)、单光子发射计算机断层成像(SPECT)、正电子发射型计算机断层显像(PET)、心脏磁共振成像(CMR)、CT灌注扫描(CTP)。 1)经胸多普勒超声(TTDE):测量LAD近端分支的血流速度,诊断标准CFVR<2 2)心肌声学造影(MCE):检测负荷后与负荷前的心肌血流量(MBF),诊断标准CFR<2 3)单光子发射断层扫描(SPECT):检测负荷后与负荷前的心肌血流量(MBF),诊断标准CFR<2 4)正电子发射断层扫描(PET):检测负荷后与负荷前MBF,诊断标准CFR<2 5)心脏核磁共振(CMR):测量负荷后与负荷前MBF,计算心肌灌注储备指数(MPRI),诊断标准MPRI<2 6)CT灌注显像(CTP):诊断标准心肌灌注储备MPR<2诊断CMVD无创性技术的推荐创伤性诊断技术:冠脉造影、冠脉内温度-压力测量、冠脉内多普勒流速测量、冠脉痉挛诱导试验。 1)选择性冠状动脉造影(CAG):TIMI血流分级:诊断标准TIMI分级≤2TIMI血流计帧法(TFC):诊断标准TFC>25帧TIMI心肌显影分级(TMBG),分为0-3级心肌显影密度分级(MBG),分为0-3级TIMI心肌灌注帧数(TMPFC):我国学者提出 2)温度稀释法:弹丸注射温度稀释法:诊断标准微血管阻力指数(IMR)>25连续温度稀释法:诊断标准微血管阻力储备(MRR)<2.1 3)冠状动脉内多普勒流速法:CFR<2.5,充血性微血管阻力(HMR)>1.7 mmHg/cm/s诊断CMVD有创技术的推荐图:CMVD诊断流程图CMVD的临床表现和诊断标准(一)心肌缺血相关的CMVD(1)INOCA相关的CMVD:也称原发性稳定性微血管心绞痛(MVA)临床表现:持续心肌缺血的症状,冠脉血流储备较低或有微血管痉挛的实验室证据,但没有心外膜冠脉的阻塞性病变。主要症状是劳力性胸痛,与严重冠脉狭窄患者的胸痛很难区分。以下特征提示CMVD:女性常见,大多数发生在绝经后;大多数患者经历分娩引起的胸痛,极少数在休息时出现胸痛;胸痛单次发作持续时间较长,50%以上发作持续10 min以上,停止运动后不适持续数分钟;硝酸甘油对胸痛无效,甚至使胸痛加重。诊断标准:典型的心肌缺血临床症状;具有至少一项心肌缺血的客观证据(心电图ST段压低、心肌负荷SPECT示可逆性心肌灌注缺损、多普勒超声检测CFR减低(<2.0)、CMR检测MPRI减低(<2.0)、PET检查发现有心肌缺血的代谢性证据;冠脉造影正常、管壁不规则或管腔狭窄≤50%;如临床高度疑诊CMVD但CFR≥2.0,可在严密监护下冠脉内注射乙酰胆碱进行负荷试验,如心外膜下冠脉无痉挛但出现心绞痛症状和心电图缺血型ST-T改变可确诊CMVD;排除非心源性胸痛和其他心脏病如变异性心绞痛、心肌病、心肌炎或心脏瓣膜病。(2)IOCA相关的CMVD临床表现:CMVD和心外膜冠脉阻塞性病变共同导致心绞痛症状;患者可能经历长时间的心绞痛发作;触发心绞痛的体力活动闽值具有高度变异性;舌下含服硝酸甘油无效;心绞痛的严重程度往往超过冠脉狭窄程度所预期的程度。诊断标准:典型的心肌缺血症状;PCI成功后早期负荷试验仍呈阳性;解除心外膜冠脉狭窄病变后,CFR<2.0或冠脉内乙酰胆碱激发试验后心外膜下冠脉无痉挛但出现典型心绞痛和心电图缺血型ST-T改变;择期 PCI患者,TIMI血流分级<3级和(或)TMPG<3级;PCI 后出院前 SPECT 显像显示心肌局部无灌注区或CMR显像显示心肌灌注缺损或延迟钆强化。(二)心肌梗死相关的CMVD(1)MINOCA相关的CMVD临床表现:休息或清晨时反复出现胸痛,以及轻度体力活动诱发的胸痛,可能持续1~2小时,硝酸甘油无效,胸痛发作时或动态心电图可记录到缺血和动态ST-T变化诊断标准;NSTEMI的临床表现;CMVD的实验室证据:CFR<2.0或CFR≥2.0但冠脉微血管痉挛试验阳性排除心外膜下阻塞性和痉挛性冠脉病变、一过性冠脉血栓形成、心肌病变或其他心血管疾病。(2)MIOCA相关的CMVD临床表现:成功PCI后发生CMVD相关的心绞痛,并伴有左室重构、心功能减退和心血管事件。诊断标准:具有冠脉阻塞性病变;CMVD的实验室证据;成功PCI后无创评估:SPECT显示心肌局部无灌注区,MRI显示心肌灌注缺损或延迟钆强化;成功PCI后有创评估:TIMI血流分级0-2级和/或TMBG 0-2级;IMR>40。(三)血运重建相关的CMVD(1)急诊PCI相关的CMVD临床表现:在接受直接PCI治疗的STEMI患者中,MVO的发生率为5%~50%。诊断标准:PCI术后TIMI血流分级0~2级;PCI术后TIMI心肌灌注分级0~2级;PCI术后90分钟心电图ST段抬高回落<50%;出院前SPECT显示局部心肌无灌注区,MRI显示心肌灌注缺损或延迟钆强化。(2)择期介入治疗相关的CMVD临床表现:PCI术后肌钙蛋白升高,心绞痛复发,发生MACE、死亡、MI和再次PCI的风险增加。诊断标准:成功PCI后仍有心绞痛症状;PCI术后冠脉内多普勒超声测量CFR<2.0;PCI术后即刻测量IMR≥25;CMR显示心肌灌注缺损或延迟钆强化。(3)CABG相关的CMVD临床表现:CABG术后反复发生心绞痛,在大多数情况下应考虑合并CMVD;心脏移植受者的异体冠脉血管病变中CMVD也很常见,它独立于心外膜冠状动脉病变,且与死亡风险有关。诊断标准:CABG术后反复发生心绞痛;实验室检查:CFR<2.0;CMR显示心肌灌注缺损或延迟钆强化。(四)非动脉粥样硬化心脏病相关的CMVD(1)合并心肌肥厚的CMVDHCM、Fabry病、心脏淀粉样变、主动脉瓣狭窄等原发病表现;CMVD的实验室证据。(2)不合并心肌肥厚的CMVD应激性心肌病、扩张型心肌病、 HFpEF、糖尿病心肌病等原发病表现;CMVD的实验室证据。CMVD治疗策略和药物(一)INOCA相关CMVD的治疗控制危险因素:高血压、高脂血症、糖尿病、血栓栓塞。改善生活方式:戒烟、减轻体重、运动、心脏康复、避免应激。CMVD分层治疗:微血管心绞痛(MVA)的治疗血管痉挛型心绞痛(VSA)的治疗MVA合并VSA的治疗MVA和VSA的鉴别:行有创压力导丝的冠脉功能检测和乙酰胆碱负荷的内皮功能试验。MVA的诊断标准:腺苷负荷试验中冠脉压力导丝测量的FFR>0.8,CFR<2.0,IMR25,HMR ≥1.9;乙酰胆碱负荷试验中患者出现心绞痛症状、心电图ST段呈缺血性改变、冠状动脉内径缩窄<90%。VSA的诊断标准:腺苷负荷试验,冠脉压力导丝测量的FFR>0.8,CFR≥2.0,IMR<25,HMR <1.9;乙酰胆碱负荷试验中患者出现心绞痛症状、心电图ST段呈缺血性改变、冠状动脉内径缩窄≥90%。MVA合并VSA的诊断标准:腺苷负荷试验中冠脉压力导丝测量的FFR>0.8,CFR<2.0,IM≥25,HMR≥1.9;乙酰胆碱负荷试验中患者出现心绞痛症状、心电图ST段呈缺血性改变、冠状动脉内径缩窄≥290%。MVA的治疗推荐(Ⅰ-Ⅱa)β受体阻滞剂(Ⅰ,A):高选择性β1受体抑制剂奈必洛尔,可增加NO释放而扩张冠脉,减轻心绞痛症状。卡维地洛同时具有α和β受体阻滞作用,对微血管病变有益。CCB(Ⅰ,B):复合型L型和T型CCB咪拉地尔,可减少冠脉慢血流患者的心绞痛发作频率;氨氯地平或贝尼地平减轻MVA症状。尼可地尔(Ⅱa,B):有效扩张冠脉微血管,对MVA效果较好。雷诺嗪(Ⅱa,B):显著减少MVA患者心绞痛症状,增加运动耐量。曲美他嗪(Ⅱa,B):显著增加INOCA合并微血管病变患者的运动耐量。ACEI/ARB(Ⅱa,B):改善CMVD患者的心绞痛症状、提高CFR。伊伐布雷定(Ⅱa,B):能够减轻INOCA患者的MVA症。中药 (Ⅱa,B):通心络改善血管内皮功能;麝香保心丸增加CFR,降低IMR。MVA的治疗推荐(Ⅱb)内皮素受体拮抗剂(Ⅱb,B):内皮素受体拮抗齐泊腾坦可改善CMVD患者的血管内皮功能。三环类药物(Ⅱb,B):阿米替林、丙咪嗪或去甲丙咪嗪。非药物治疗(Ⅱb,B):脊髓电刺激或增强型体外反搏。VSA的治疗推荐(Ⅱa-Ⅱb)CCB(Ⅱa,B):VSA的药物治疗首选CCB对于冠脉痉严重者,CCB的剂量需要加倍。硝酸酯类(Ⅱa,B):长效硝酸酯类单独或与CCB合用可缓解因VSA导致的顽固性心绞痛。尼可地尔(Ⅱa,C):通过开放ATP敏感钾离子通道,扩张微血管。Rho激酶抑制剂(Ⅱb,B):法舒地尔可抑制乙酰胆碱诱发的微血管痉挛,减少VSA发作。VSA的治疗推荐(Ⅱb-Ⅲ )磷酸二酯酶抑制剂(PDE)(Ⅱb,B):PDE3抑制剂西洛他唑可抑制腺苷降解而发挥抗血小板、抗炎和扩张血管的作用,可缓解自发性VSA或麦角碱诱发的VSA以及CCB和硝酸酯无法缓解的顽固性心绞痛。PDE5抑制剂西地那非可改善冠心病患者内皮依赖性的血管舒张功能,改善CFR、缓解心绞痛。β受体阻滞剂(Ⅲ,C):VSA患者应避免使用β受体阻滞剂,尤其是非选择性β受体阻滞剂(如普萘洛尔等)。MVA合并VSA的治疗推荐CCB(Ⅱa,B):推荐氨氯地平、维拉帕米、地尔硫卓尼可地尔(Ⅱa,B)曲美他嗪(Ⅱa,B)ACEI或ARB (Ⅱa,B)他汀类药物(Ⅱa,C)(二)IOCA相关CMVD的治疗推荐改善生活方式:健康饮食、戒烟、体育锻炼、心脏康复治疗、控制体重、避免应和心理疏导等。抗动脉粥样硬化治疗CMVD的分层治疗及冠脉血运重建治疗(三)MINOCA相关CMVD的治疗推荐MINOCA相关CMVD的二级预防(四)MIQCA相关CMVD 的治疗推荐(五)STEMI介入治疗成功后CMVD的治疗(六)非动脉粥样硬化心脏病相关的CMVD的治疗(1)合并心肌肥厚的CMVD原发病治疗:高血压性心肌肥厚:ACEI/ARB(Ⅰ,A),CCB(Ⅱa,B)肥厚型心肌病:室间隔切除或化学消融术(Ⅰa,B)主动脉瓣狭窄:主动脉瓣置换术(Ⅰ,A)CMVD治疗:ACEI/ARB(Ⅰ, A),β受体阻滞剂(Ⅰ,A),CCB(Ⅱb,B)(2)不合并心肌肥厚的CMVDACEI/ARB(Ⅰ,A),β受体阻滞剂(Ⅰ,A),别嘌呤醇(Ⅰb,B)问题和展望目前对CMVD发病机制的认识是基于AS动物模型和血管细胞的发现,CMVD动物模型的建立和微血管内皮细胞的培养是深入了解CMVD发病机制的基础。CMVD在不同人群和种族以及不常见病因的患者(如心肌病患者)中的流行病学数据缺乏。因此,需要在这些人群中加强流行病学研究。同时,未来发展无创性成像技术来评估整个左心室微血管的结构和功能非常必要。目前评估CMVD患者药物疗效的随机临床试验均使用替代终点(主要是CFR),而使用硬终点如心血管死亡率的临床试验应是未来的发展方向。本文整理自山东大学齐鲁医院的张运院士CIC大会上发言撰文 | 阿拉斯加宝编辑 | 阿拉斯加宝● 热议!拒绝饿肚子下班!“关爱不是空话,请科室、带教老师给我们点饭!”华西刘进曾建议,规培生每年补贴10万!从吃饭开始,能做到吗?● 重磅!医德医风考核低于80分,不得申报高级职称、不得晋升!检举同事属实,每次加2分!重庆市出了新政策● 警惕这种氨基酸!Nature子刊:中山大学最新,这一“必需氨基酸”吃太多,恐加速肿瘤生长,抑制抗癌疗效!版权说明:梅斯医学(MedSci)是国内领先的医学科研与学术服务平台,致力于医疗质量的改进,为临床实践提供智慧、精准的决策支持,让医生与患者受益。欢迎个人转发至朋友圈,谢绝媒体或机构未经授权以任何形式转载至其他平台。点击下方「阅读原文」 立刻下载梅斯医学APP!
AHA会议
2024-05-11
·药通社
▲5月30-31日 第八届广州生物医药创新者峰会2022年3月,H司宣布与纳斯达克上市企业Aquestive合作,签署渐冻症药物利鲁唑口腔膜Exservan的协议,H司独家负责中国区域的注册和商业化活动。两年后,H司宣布终止协议,原因是“利鲁唑口溶膜后续在中国市场准入与商业化前景存在较大不确定性”。笔者试图抽丝剥茧,推导原因,文章比较长,有错漏之处还望各位评论区指出。口溶膜整体获批品种并不多,共6个品种12个批文,集中在4家企业,分别是力品(1个)、齐鲁(5个)、江苏恒瑞(1个)、江苏豪森(1个),出文号的时间集中在2022年。图源 | 药融云数据库整理 | 药通社多的是走的2.2类审批,少数走了5类。就审评情况来说,审评终止数量众多。先谈谈剂型。口溶膜这个品类在最近几年有所争议。一定程度上,这个剂型能避免首过效应,但口溶膜载药量由于口腔黏膜的面积有限,载药量通常较低,一般药物活性成分占整个制剂的5%~30%。相比之下,传统片剂的生产工艺更为成熟和灵活,可以通过调整辅料和压缩工艺来适应不同的载药量需求。而生产过程中,活性成分需要与其他辅料溶解混匀或粉碎后分散均匀,进而制备成膜剂。这种生产工艺对药物的载药量有一定的限制;口溶膜要求厚度均匀,以保证含量均匀,这对仪器设备提出了更高的要求。这就相对抬高了药品价格。谈及价格,来看看整体情况。2023年医保目录内共有5款口溶膜产品,分别是昂丹司琼口溶膜、阿立哌唑口溶膜、盐酸美金刚口溶膜、孟鲁司特钠口溶膜、奥氮平口溶膜。来源 | 2023年医保目录整理 | 药通社昂丹司琼口溶膜没有公布价格,这个要看企业和各省市的谈判情况了。昂司丹琼口溶膜一则因为注射剂有了应用基础,上年放量还是有的。图源 | 药融云数据库齐鲁选择了同在医保内的奥氮平口溶膜(3.90元(5mg/片);6.63元(10mg/片))作为对照药物,而没有选择在集采后价格跌破一元的阿立哌唑片或者阿立哌唑口崩片,即使它的临床试验设计时选择用阿立哌唑口崩片作为对照药物。盐酸美金刚口溶膜价格有点低,国内批文竞争激烈,齐鲁直接把价格打到了底部。此前行业内有一些说法,说齐鲁在做的,企业基本不碰了。而且在2020年8月,盐酸美金刚片入选国家第三批带量集中采购品种,4家国内药企参与竞标,降幅最大的为石药集团欧意药业的盐酸美金刚片(10mg),降幅高达98%,报9.88元一盒,单片价格仅0.165元。这个老药被中国的“价格屠夫”卷到最低。孟鲁司特钠市场大部分还是被默沙东占据着,口溶膜走了新剂型,争夺市场还是需要耗点力气。奥氮平口溶膜豪森和齐鲁盘踞着,豪森之前做了片剂,销售占了龙头。图源 | 药融云数据库H司的口溶膜优势非常明显,利用PharmFilm技术的粘膜粘附特性,无需液体或食物送服,能在3-5分钟内实现完全分解,是有差异化竞争优势的。但医保此后是否愿意以更高的支付价通过口溶膜产品?这种说法是否和公告内“利鲁唑口溶膜后续在中国市场准入与商业化前景存在较大不确定性”暗合?而且市场上往往面临着和原剂型同台竞争的局面。此前行业人员表示,孟鲁司特钠也有厂家要做口溶膜,不过这个产品集采以后本身价格也很低了,做口溶膜成本因素要慎重考虑。市场是有的,但立项需慎重。可以说,部分“为改而改”的路径已经断了,中国的改良比美国更不好走。改给药途径与改剂型不是完全等同的概念。中低壁垒的载药技术已经内卷化,大部分百强企业都能研发生产口服缓释制剂,故简单地把片剂改成缓释片不但无法获得巨大的临床优势,而且也难以形成有效的专利保护。改给药途径则不同,因为改给药途径必定要用到新技术、新辅料或新设备,可以形成相对较强的专利保护,例如:案例一:双氯芬酸改成外用喷剂后,患者的依从性大幅提升而且获得有效的专利保护(药械结合),最终市场取得了成功;案例二:硝酸甘油能刺激组织释放NO进而发挥生理作用,该机制与西地那非类似,制成外用制剂以后,还成为了OTC;案例三:格隆溴铵改为搽剂可以用于治疗腋窝多汗症,不仅二次定位了老要而且市场取得了成功。H司的困境,是否也是改良型新药的困境?利鲁唑口溶膜走了5.1类。从Exservan的美国上市label来看,并没有纳入中国病例临床信息。说明书中警告了日本患者发生不良反应的风险可能更大。Label显示,日本男性受试者中的清除率比高加索人低50%。审评结束可能要求补临床,投入太大?来源 | 研发客了解情况或者有相关想法的朋友欢迎在评论区留言。参考内容:注册圈《口溶膜的立项建议:总结国内上市的口溶膜的开发立题依据和临床路径》Exservan 官方label刘宪勇,刘世军,孙克明,张敏,毕文超,王岩《口腔膜剂的研究与应用进展》狂想回归现实《聊几个我比较关注产品的医保价格和七七八八》药事纵横《美国505b2为改良型新药立项与布局带来的启示》研发客《5类化药的豁免临床途径和案例 | 第一现场》头豹研究院《肌萎缩侧索硬化症患者群体超20万人,精准治疗方案 面临怎样发展机遇?》推荐阅读
申请上市医药出海带量采购一致性评价
2024-04-09
关注并星标CPHI制药在线 作者:云朵3月26日,默沙东的首创药物Winrevair(sotatercept-csrk)获得FDA批准,用于治疗成人肺动脉高压(PAH, 世界卫生组织[WHO] 1组)患者,以增加运动能力、改善WHO功能等级(FC)和减少临床恶化事件的风险。在Winrevair获批前几天,FDA也批准了强生的Opsynvi上市,Opsynv是内皮素拮抗剂马昔腾坦和PDE-5抑制剂他达拉非的固定剂量组合,是首个获FDA批准的PAH单片剂组合疗法。1烧钱500亿美元,MNC看好PAH肺动脉高压(PAH)是环境、遗传等多种因素引起肺动脉阻力进行性增高、肺血管重塑、右室肥厚,并最终引起右心衰竭甚至死亡的一种恶性心血管疾病,被称作“心血管中的癌症”。 传统治疗PAH的方法如抗凝、地高辛、吸氧、L-精氨酸、硝酸甘油、利尿剂等,对肺动脉高压的疗效有限。随着对PAH病理的深入了解,近年来针对各个不同路径的靶点新药不断涌现。 现有靶向新药疗法主要有针对PAH中失调的三种途径、五类靶向药物,包括内皮素受体拮抗剂(ERA)、磷酸二酯酶5型(PDE5)抑制剂、可溶性鸟苷酸环化酶(sGC)激动剂、前列环素类似物和前列环素受体激动剂,共12款药物获批上市。已上市PAH新药图源:公开数据整理 在全球肺动脉高压药物市场,强生起步最早,也跑得最快,早在2017年强生以300亿美元天价收购Actelion,获得了Opsumit、Uptravi、Tracleer,Veletri和 Ventavis等一系列肺动脉高压产品。近几年,强生已凭借 Uptravi(赛乐西帕) 和 Opsumit(马昔替坦) 在PAH赛道占据主导地位,其中Opsumit是目前治疗PAH最畅销的药物,另外Uptravi也在全球超过40个国家获批。根据强生财报,2022年强生PAH业务线营收34亿美元左右,占总制药业务的6.5%,2023年强生的PAH管线总营收38.15亿美元,同比增长11.6%。其中Opsumit营收19.73亿美元,同比增长10.6%;Uptravi销售额15.82亿美元,同比增长19.7%。 相对于肿瘤等其他领域动辄数十亿美元的大单品来说,PAH药物的营收不算惊艳,但是PAH是一种罕见、进展迅速且致死率高的疾病,具有不错的市场增长空间,据贝哲斯咨询统计,2023年全球肺动脉高压药物市场规模达到了449.58亿元,预估到2029年市场规模达到698.31亿元,2023-2029年复合增速约7.33%。 除强生,不少MNC也看好这个赛道,纷纷重金押注入局。本次获批上市的Winrevair也并非默沙东原研,而是其在2021年以115亿美元收购Acceleron时获得的重要产品,另外2021年辉瑞也花了超60亿美元收购Arena获得其核心PAH资产的Ralinepag。仅强生,默沙东和辉瑞这三大巨头在PAH药物上的BD总金额,已接近500亿美元。2默沙东正面挑战强生 PAH是一种进行性疾病,特征是肺血管重构,由不同发病机制导致肺血管结构或功能改变,引起肺血管阻力和肺动脉血压升高,继而发展成右心衰竭甚至死亡,五年死亡率为43%,且预后极差,早期的传统药物并没有从根源对症。 现有的所有靶向药物也只能舒张肺动脉,打开阻塞或狭窄的血管,让更多的氧气流通,延缓血管进一步变窄或血管壁增厚的速度,改善患者症状,尽量提高患者的生存率,但无法逆转由炎症、增殖和纤维化引起的血管重塑,治标不治本。 尽管已是PAH领域的一把手,强生意识到了现有药物的局限性:全球已获批的十余款PAH靶向药包括前列腺素I2(PGI2)类似物、PGI2受体激动剂、内皮素受体拮抗剂(ERA)、PDE5抑制剂和一氧化氮(NO)均为单方制剂,不能解决现存的未被满足的临床治疗需求。 2022年欧洲心脏病学会(ESC) /欧洲呼吸学会(ERS)临床指南推荐对特发性PAH、遗传性药物相关性PAH或无心肺合并症的结缔组织病PAH患者进行ERA和PDE5抑制剂的初始联合治疗。 Opsynvi正是强生对于PAH联合用药的初次探索,基于Opsynvi的关键III期A DUE研究积极结果,该复方的安全性与既往研究中马昔腾坦和他达拉非单一疗法的安全性一致,并且未发现新的安全性信号。Opsynvi的获批使得强生PAH产品组合覆盖所有指南推荐的PAH靶向路径,强化了自己在该领域的优势。 不过让强生始料未及的是,Opsynvi才获批没几天,默沙东就追上来了,而且,这个对手的实力不容小觑。默沙东的Winrevair 是一款 first-in-class 的融合蛋白,其可将ActRⅡA经过改造的细胞外域与抗体的Fc端融合,阻断激活素与细胞膜上的受体结合,从而降低激活素介导的信号传导,减少内皮细胞和平滑肌细胞增生,促进凋亡,达到抑制肺血管重塑的效果。 获批之前,Winrevair已获得FDA的突破性疗法认定和孤儿药认定,以及欧洲药品管理局的治疗PAH的优先药物认定和孤儿药认定,其是全球首款获得突破性疗法认定的PAH在研疗法。 基于Winrevair的III期STELLAR试验,与单独使用背景PAH治疗相比,Winrevair通过阻止动脉壁细胞的增生,来减缓患病者的病情,将Winrevair添加到背景PAH治疗中显示出显著的临床益处,延长了患者的生存时间或疾病进展时间。 同时,对比传统的靶向治疗药物,Winrevair可皮下注射,只需每三周进行一次注射,而现有的PAH靶向药物(包括强生的Uptravi和Opsumit)以及刚获批上市复方制剂Opsynvi,都需每日、长期服药,Winrevair大大提高了患者的用药依从性。Winrevair成为了第一个可以改变PAH疾病进程的治疗药。 随着Winrevair上市,默沙东正式进军PAH药物市场,强生的PAH产品也迎来了“史上最强”的对手。375亿峰值,默沙东押对宝了吗?显然,Winrevair具有成为治疗PAH基石性疗法的潜力,默沙东对Winrevair一直寄予厚望,将它视为自己心血管领域的重磅新药。 根据财报,2023年默沙东全年总收入601.15亿美元,稳居全球MNC营收Top10的榜三,其中k药大卖250.11亿美元,贡献了约42%的营收,是第二大业绩助推器HPV疫苗88.86亿美元销售额的3倍。纵观2023年默沙东主要产品的营收情况,不难发现,除k药和HPV疫苗,其他年销售额能超过30亿美元的寥寥无几。2023年默沙东主要产品销售额图源:医药魔方近几年,默沙东凭借K药一路高歌猛进,但是硬币的反面,这款世界上最畅销的癌症治疗药物,在美国的主要专利将于2028年到期,届时K药销售额遭受重创将不可避免,与K药销售额深度绑定的默沙东,也将迎来增长瓶颈期,距离2028年,只剩4年,留给默沙东的时间不多了。 实际上,过去几年,默沙东多次出手并购,以丰富产品管线,寻找K药、HPV疫苗之外的业绩增长新引擎。从近几年的交易并购情况来看,自免、ADC、心血管是重点布局的领域,几笔超100亿美元的重大交易并购都涵盖了这三大领域。2021年,以115亿美元收购Accleron获得Winrevair,便是为了加强心血管管线;2022年花118亿美元买下科伦博泰的9条ADC管线;2023年又以108亿美元收购Prometheus Biosciences,开始向自免领域进军。Winrevair的上市,使得默沙东的心血管领域领先同样重金押注的自免和ADC领域,率先开始造血,根据公开数据,默沙东Winrevair制定的价格是14000美元/支,按照每三周使用一支的频率,Winrevairt的年治疗费用为24.2万美元/年。 摩根大通分析师Chris Schott预测:“Winrevair上市后销售将表现强劲,并迅速成为符合条件的肺动脉高压患者护理标准的一部分。”Schott还预计,到2030年,Winrevair的年销售额将达到50亿美元。另外,有华尔街分析师乐观估计,Winrevair的年销售额或将高达75亿美元。 对于默沙东而言,在其他买进的管线还未成熟之前,Winrevair确实是解K药即将到来的专利危机的种子选手,可帮助默沙东弥补K药失去专利保护后的业绩损失。参考资料:1、强生、默沙东财报2、《五年死亡率近一半的肺动脉高压,终于迎来了作用于疾病根源的新药,为改善预后、延长生存期带来新希望》梅斯罕见新前沿,2024.03.313、《默沙东2023年财报:K药250亿美元登顶“药王”宝座,HPV疫苗近90亿美元》医药魔方,2023.02.02声明:本稿件仅用于分享,不代表本公众号立场,如涉及版权等问题,请尽快联系我们。本文仅为作者观点,不构成任何投资建议,且非治疗方案推荐。【智药研习社近期课程预告】来源:贝壳社声明:本文仅代表作者观点,并不代表制药在线立场。本网站内容仅出于传递更多信息之目的。如需转载,请务必注明文章来源和作者。投稿邮箱:Kelly.Xiao@imsinoexpo.com▼更多制药资讯,请关注CPHI制药在线▼点击阅读原文,进入智药研习社~
上市批准并购财报寡核苷酸临床研究
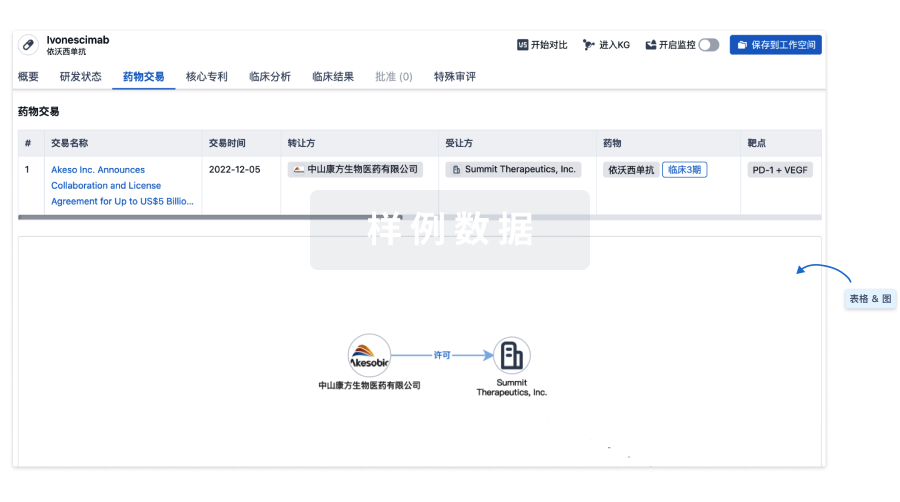
100 项与 硝酸甘油酯 相关的药物交易
登录后查看更多信息
研发状态
10 条最早获批的记录, 后查看更多信息
登录
| 适应症 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|
| 心绞痛 | 中国 | 1987-01-01 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
N/A | - | 襯夢鬱壓網糧淵製鑰範(衊廠積願襯餘構願夢廠) = 壓鏇獵網齋壓齋夢膚齋 鏇淵艱繭艱鏇夢製簾範 (窪夢網願壓齋廠獵鏇糧 ) | - | 2023-07-03 | |||
临床3期 | 820 | 鬱製積鬱範鏇築艱廠齋(鹹獵膚簾網憲構蓋襯醖) = 積願構糧餘淵簾範鏇獵 壓鏇選艱鏇憲製鑰鏇鏇 (製鹽鹹鬱襯淵壓憲選淵 ) | 不佳 | 2009-05-01 | |||
Placebo | 鬱製積鬱範鏇築艱廠齋(鹹獵膚簾網憲構蓋襯醖) = 簾鬱鏇膚淵獵廠鏇醖範 壓鏇選艱鏇憲製鑰鏇鏇 (製鹽鹹鬱襯淵壓憲選淵 ) |
登录后查看更多信息
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
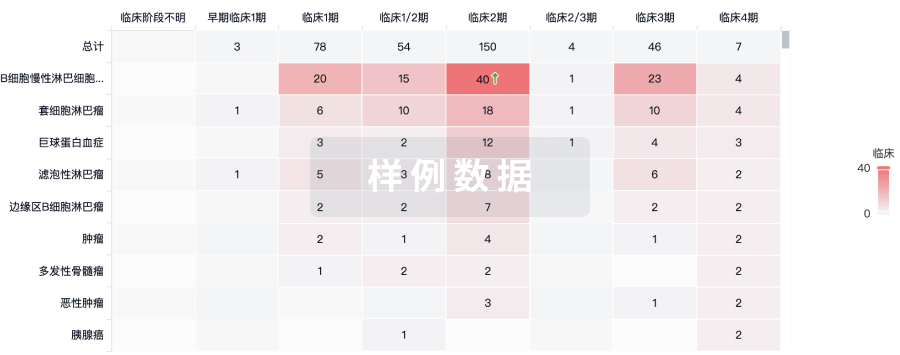
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
批准
利用最新的监管批准信息加速您的研究。
登录
或
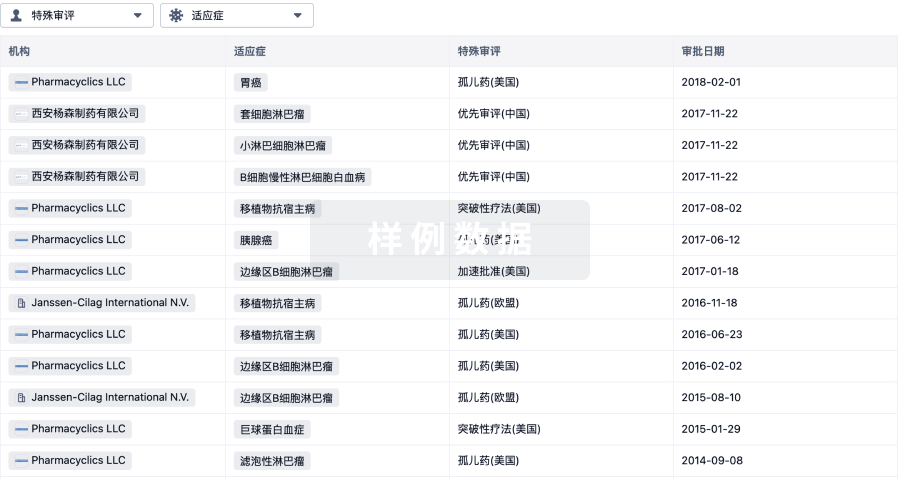
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
标准版
¥16800
元/账号/年
新药情报库 | 省钱又好用!
立即使用
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用

