预约演示
更新于:2025-07-31
siRNA(Regeneron)
更新于:2025-07-31
概要
基本信息
原研机构- |
非在研机构- |
权益机构- |
最高研发阶段临床前 |
首次获批日期- |
最高研发阶段(中国)- |
特殊审评- |
关联
100 项与 siRNA(Regeneron) 相关的临床结果
登录后查看更多信息
100 项与 siRNA(Regeneron) 相关的转化医学
登录后查看更多信息
100 项与 siRNA(Regeneron) 相关的专利(医药)
登录后查看更多信息
4
项与 siRNA(Regeneron) 相关的文献(医药)2025-02-07·CURRENT CANCER DRUG TARGETS
Enhanced Efficacy of Radiation Therapy against Glioblastoma by Attenuated Salmonella Carrying Co-Expression Plasmids with siRNA-PD-L1 and Endostatin
Article
作者: Zhao, Tiesuo ; Ji, Yinghua ; Wang, Yu ; Guo, Jiaming ; Ren, Weiwei ; Lu, Chengbiao ; Jiang, Hanyu ; Dang, Peiyuan ; Jia, Huijie ; Chen, Xin ; Lei, Mengyu ; Yang, Jin ; Li, Jiahang ; Geng, Jiaxin
Background::
Glioblastoma (GBM), a common type of brain tumor, is currently treatable through radiation therapy. However, there is room for improvement in the effec-tiveness of treatment. Radiation can lead to an increase in the expression of PD-L1 and VEGF, which might reduce the responsiveness of the tumor to the therapy. This situation underlines the necessity for innovative treatment strategies.
Objectives::
In this study, we investigated the potential of attenuated Salmonella carrying the co-expressing plasmid siPD-L1-Endo to effectively inhibit PD-L1 and VEGF expres-sion, thereby enhancing the anti-tumor effects of radiation therapy in GBM-bearing mice.
Methods::
The regulatory mechanisms responsible for the treatment effect were detected by Flow cytometry, Immunohistochemistry, TUNEL, Immunofluorescence, H&E staining, and Western blot assays.
Results::
Upon administration of attenuated Salmonella carrying siRNA-PD-L1 and co-expressing endostatin plasmids, the results exhibited significant suppression of tumor growth and tumor cell proliferation, as well as a concurrent decrease in PD-L1 and VEGF expression in tumor tissues. Moreover, the treatment led to reduced expression levels of tumor-related proteins p-Stat3, MMP2, Cyclin D1, and PCNA, an increase in the expres-sion of the apoptosis-related protein cleaved-caspase3, facilitated infiltration of CD4+ and CD8+ T cells within tumor tissues, and an elevation of the ratios of CD4+, CD8+ T cells, and NK cells in the spleen of tumor-bearing mice.
Conclusion::
These findings highlight the ability of attenuated Salmonella carrying siR-NA-PD-L1 and co-expressing endostatin plasmids to effectively modulate PD-L1 and VEGF expression, thus strengthening the anti-tumor immune response in GBM-bearing mice subjected to radiation therapy. This combination therapy approach holds promise as a potential avenue for improving the efficacy of radiation therapy in the treatment of glio-blastoma.
2023-08-01·Small (Weinheim an der Bergstrasse, Germany)
M2 Macrophage Membrane-Mediated Biomimetic-Nanoparticle Carrying COX-siRNA Targeted Delivery for Prevention of Tendon Adhesions by Inhibiting Inflammation.
Article
作者: Zhou, You Lang ; Tan, Jun ; Sun, Yu Cheng ; Jin, Jing ; Wang, Hao Liang ; Yang, Qian Qian ; Li, Zhi Jie ; Sun, Jie ; Chen, Qing Zhong ; Ju, Fei
Tendon adhesion is the most common outcome of tendon or tendon-to-bone healing after injury. Our group developed a hydrogel-nanoparticle sustained-release system previously to inhibit cyclooxygenases (COXs) expression and consequently prevent tendon adhesion and achieved satisfactory results. However, effective treatment of multiple tendon adhesions is always a challenge in research on the prevention of tendon adhesion. In the present study, an M2M@PLGA/COX-siRNA delivery system is successfully constructed using the cell membranes of M2 macrophages and poly (lactic-co-glycolic acid) (PLGA) nanoparticles. Targeting properties and therapeutic effects are observed in mice or rat models of flexor digitorum longus (FDL) tendon injury combined with rotator cuff injury. The results showed that the M2M@PLGA/COX-siRNA delivery system has low toxicity and remarkable targeting properties to the injured areas. Treatment with the M2M@PLGA/COX-siRNA delivery system reduced the inflammatory reaction and significantly improved tendon adhesion in both the FDL tendon and rotator cuff tissues. These findings indicate that the M2M@PLGA delivery system can provide an effective biological strategy for preventing multiple tendon adhesions.
2018-03-27·Current drug delivery4区 · 医学
Chemotherapy with si-RNA and Anti-Cancer Drugs
4区 · 医学
Review
作者: Chandra, Saket ; Singh, Ranjit ; Rath, Goutam ; Goyal, Amit Kumar ; Kaur, Kamaljeet
BACKGROUND:
To treat cancer, chemotherapy is a key therapeutic approach which is associated with several limitations. This chemotherapeutical agent exhibits multi drug resistance coupled with undesirable side effects. This multidrug resistance is exhibited by tumor cell due to actuation of drug out flow mechanism, programmed cell death and protection mechanisms etc. One of the therapeutic approaches to cure cancer is RNA interference (RNAi). Small interfering RNA (si-RNA) is considered as a major therapeutic tool used to control expression of a particular gene. It is a well known fact that intake of more drugs can lead to cancer chemo resistance, thus siRNA based therapeutic approach is under scrutiny to cure cancer.
METHODS:
This review article gives an overview of various combination approaches for si-RNA with chemotherapeutics. Further, article highlights the potential of nanotechnology to improve bioavailability of drug and bio-therapeutics at the site of action.
RESULTS:
Combination chemotherapy is employed in clinics as a main cancer treatment tool to suppress multidrug resistance in cancer. On the other hand, suitable protective carrier is needed due to the stability issues and small size of si-RNA. To overcome these drawbacks associated with siRNA currently, nanotechnology based approaches have been widely used.
CONCLUSION:
Delivery of anti-cancer drugs with si-RNA will be one of important intermingled approach to reduce duration of chemotherapy and improve therapeutic outcomes in cancer patient.
100 项与 siRNA(Regeneron) 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 青光眼 | 临床前 | 美国 | 2022-05-01 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
No Data | |||||||
登录后查看更多信息
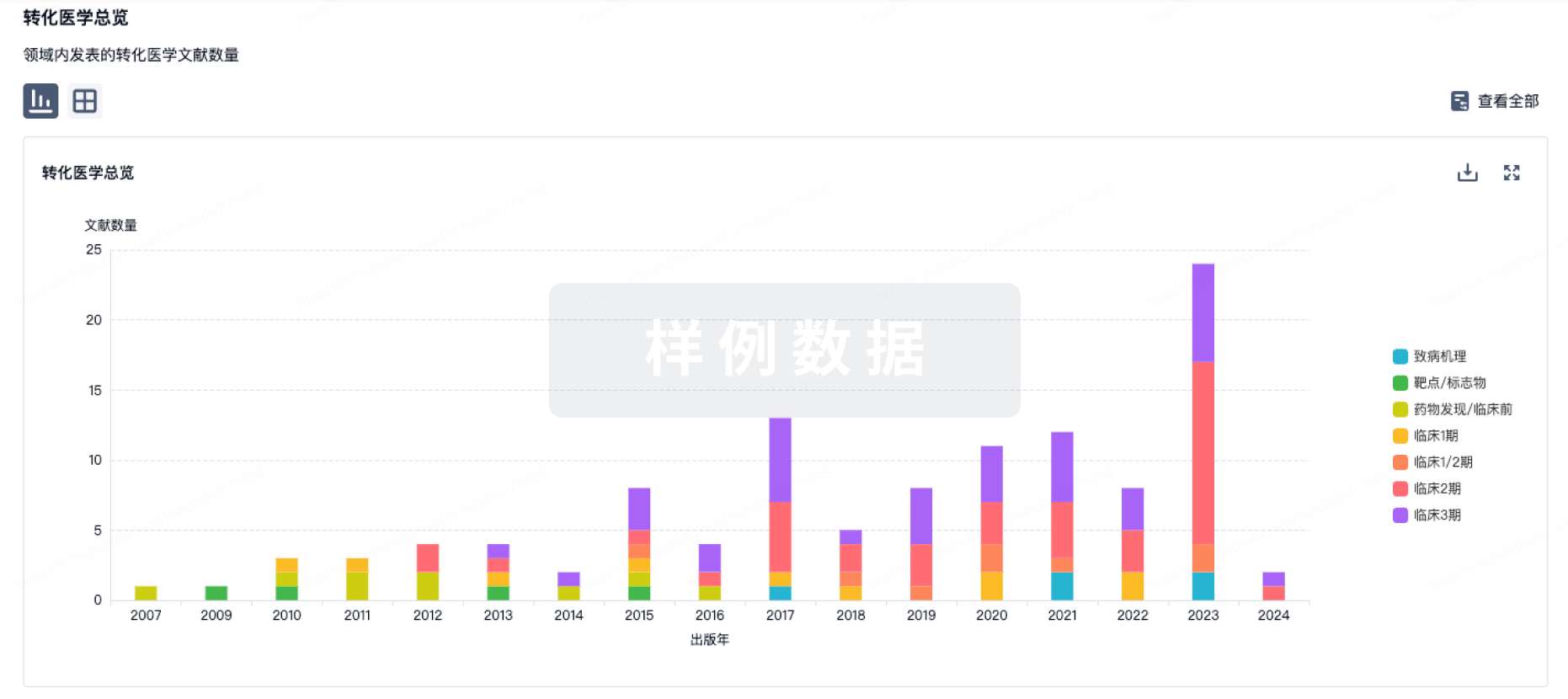
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
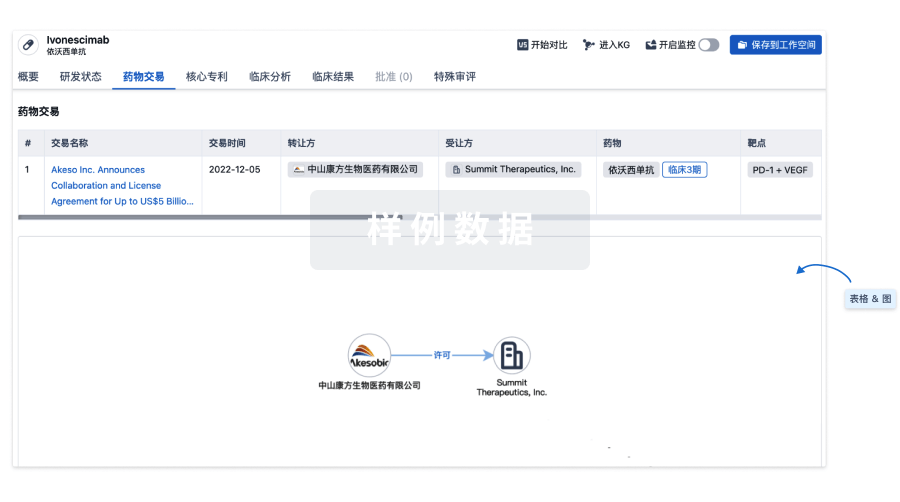
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
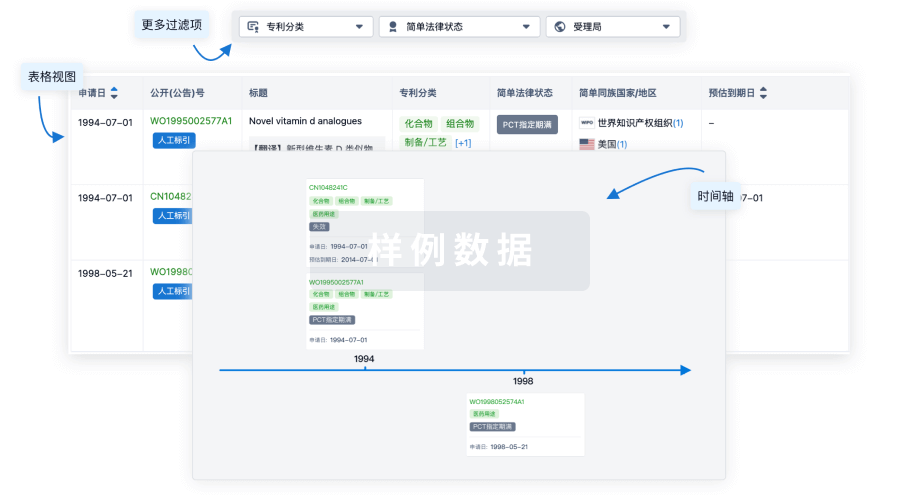
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
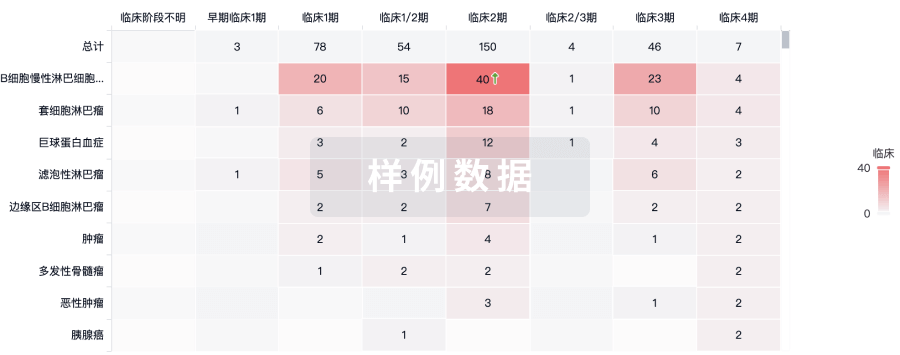
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
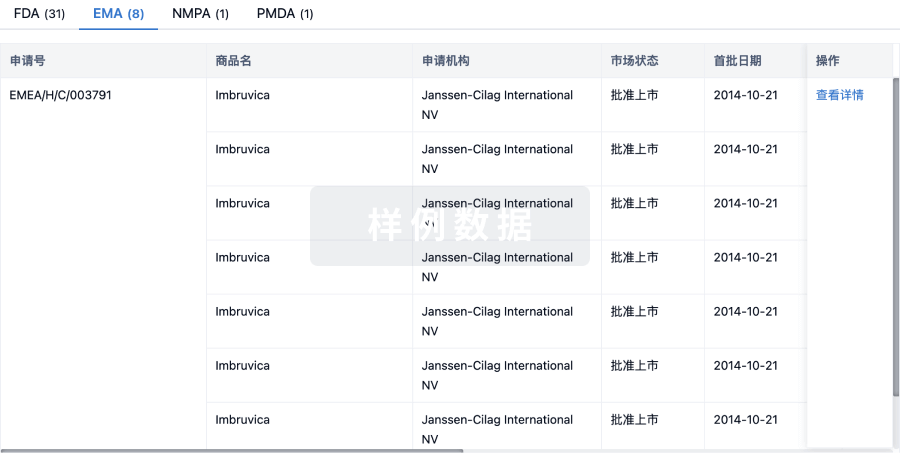
批准
利用最新的监管批准信息加速您的研究。
登录
或
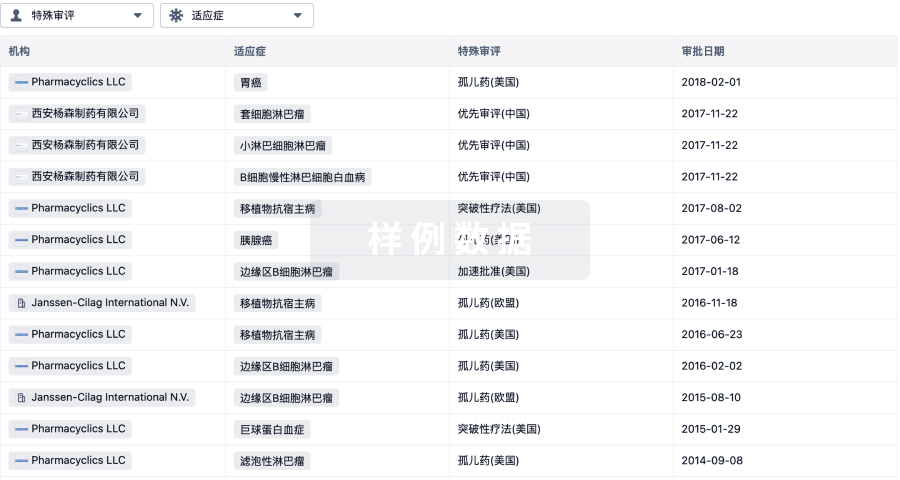
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
Eureka LS:
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
