预约演示
更新于:2025-08-20
4-octyl itaconate
更新于:2025-08-20
概要
基本信息
药物类型 小分子化药 |
别名 4-OI |
作用方式 抑制剂、刺激剂 |
作用机制 NLRP3抑制剂(含 NACHT, LRR 和PYD 结构域蛋白-3抑制剂)、Nrf2刺激剂(核转录因子的激活红细胞2相关因子刺激剂) |
在研适应症 |
非在研适应症- |
原研机构 |
非在研机构- |
权益机构- |
最高研发阶段临床前 |
首次获批日期- |
最高研发阶段(中国)临床前 |
特殊审评- |
关联
100 项与 4-octyl itaconate 相关的临床结果
登录后查看更多信息
100 项与 4-octyl itaconate 相关的转化医学
登录后查看更多信息
100 项与 4-octyl itaconate 相关的专利(医药)
登录后查看更多信息
115
项与 4-octyl itaconate 相关的文献(医药)2026-02-01·BIOMATERIALS
Charge-reversal nanoassembly for rheumatoid arthritis therapy via cell-free DNA scavenging and microenvironment reprogramming
Article
作者: Peng, Chang ; Fang, Ting ; Li, Ji ; Wang, Dongkai ; Sun, Hanjie
The clearance of cell-free DNA (cfDNA) in rheumatoid arthritis (RA) represents a promising therapeutic approach for inflammation. While cationic materials are widely utilized for cfDNA capture, their safety during in vivo delivery remains a critical concern. Additionally, macrophage-mediated inflammatory responses exacerbate disease progression. Here, we propose a charge-reversal and enhanced nanoassembly responsive to the inflammatory microenvironment, composed of a block polymer termed polycaprolactone-poly (N, N-dimethylacrylamide)-thioketal-polyethylene glycol (PCL-PDMA-TK-PEG, PPTP), a copolymer methoxy poly (ethylene glycol)-poly-l-lysine-2,3-dimethylmaleic anhydride (mPEG-PLL-DMA, PLM), and 4-octyl itaconate (4-OI). Charge reversal in acidic inflammatory microenvironments and ROS-responsive enhancement of positive surface charge, significantly improving cfDNA capture efficiency within inflammatory sites. Mitochondrial targeting through electrostatic interactions, promoting 4-OI release to inhibit macrophage-driven inflammation. Reduced protein shielding during systemic circulation, enabling precise accumulation in inflamed joints. The 4-OI@PPTP/PLM nanoassembly effectively suppresses inflammatory cytokine production, mitigates synovial hyperplasia, and attenuates bone erosion in collagen-induced arthritis models. This strategy integrates cfDNA scavenging with microenvironment reprogramming, offering a dual-action therapeutic platform for RA management.
2025-11-01·BIOMATERIALS
Reprogramming mitochondrial metabolism to enhance macrophages polarization by ROS-responsive nanoparticles for osteoarthritis
Article
作者: Li, Hui-Yun ; Li, Gui-Cheng ; Lu, Hao ; Xu, Hai-Lin ; Yuan, Yu-Song ; Cao, Zheng ; Xu, Chun ; Zhang, Ling-Pu ; Xiao, Hai-Hua
Osteoarthritis (OA) is a chronic low-grade inflammatory joint disease closely related to the inflammatory pathological microenvironment caused by synovial M1 macrophages. In contrast to the proinflammatory role of M1 macrophages, M2 macrophages contribute to anti-inflammatory responses and tissue repair. Therefore, shifting the M2/M1 phenotype ratio in favor of M2 macrophages has become a promising therapeutic strategy for OA. However, current therapeutics cannot penetrate the synovium and only show limited drug retention time. Herein, we developed an OA microenvironment-responsive nanocarrier with thioketal bonds in the main chain and β-1,3-d-glucan and triphenylphosphine units in the side chain, which can respond to reactive oxygen species (ROS) and target macrophages and mitochondrial aggregation. For OA treatment, 4-octyl itaconate and dexamethasone were encapsulated within the nanocarrier, forming HBPTG@OD that effectively eliminated mitochondrial ROS and inducible nitric oxide synthase in M1 macrophages. HBPTG@OD significantly suppressed the release of inflammatory factors by macrophages and thereby reducing chondrocyte death. In vivo studies in a destabilized medial meniscus (DMM)-induced OA model showed that HBPTG@OD effectively converted M1 synovial macrophages to M2 macrophages, consequently delaying chondrogenic apoptosis. This study presents a nanocarrier-based strategy that effectively repolarizes M1 macrophages, demonstrating great promise for the treatment of OA.
2025-07-01·Clinical and Translational Medicine
Itaconate suppresses neonatal intestinal inflammation via metabolic reprogramming of M1 macrophage.
Article
作者: Zhong, Limei ; Li, Sitao ; Shi, Yongyan ; Yang, Yuling ; Wang, Huijuan ; Mu, Yide ; Lan, Chaoting ; Liu, Yufeng ; Zhao, Peizhi ; Zhong, Wei ; Huangfu, Shuchen ; Wang, Yijia ; Tian, Yan ; Tian, Bowen ; Yan, Chun
BACKGROUND:
Necrotizing enterocolitis (NEC) is a rapidly progressive and severe gastrointestinal disorder in neonates that is marked by an inflammatory cascade initiated by mechanisms that remain incompletely understood, resulting in intestinal necrosis and systemic infections. This study demonstrated that itaconate (ITA) exerts a protective effect in NEC by regulating macrophage reprogramming.
METHODS:
Changes in ITA expression were investigated using immunofluorescence staining and liquid chromatography-mass spectrometry, and their effect on immune cell differentiation was verified through single-cell sequencing. In vivo experiments were performed using ACOD1-/- and ACOD1fl/flLysMcre NEC mouse models.
RESULTS:
We detected changes in ITA expression in clinical NEC samples and confirmed the effect of these changes on immune cell differentiation. In vivo experiments confirmed the therapeutic role of ITA in regulating macrophage differentiation in NEC, and we further investigated the mechanism by which ITA regulates macrophage metabolic reprogramming. The depletion of ITA in NEC correlates with an increased frequency of pro-inflammatory macrophage polarization, thereby exacerbating intestinal inflammatory injury. Importantly, our in vivo experiments revealed that treatment with 4-octyl itaconate (4OI) significantly mitigated intestinal symptoms associated with NEC in murine models. Mechanistic investigations showed that 4OI effectively suppressed M1 macrophage polarization by rescuing mitochondrial function and upregulating oxidative phosphorylation in macrophages.
CONCLUSIONS:
Our results highlight ITA as a metabolic checkpoint of macrophage differentiation in NEC and suggest the therapeutic efficacy of 4OI in NEC.
KEY POINTS:
Itaconate alleviates NEC by reprogramming M1 macrophage metabolism ACOD1 deficiency exacerbates NEC severity 4OI maintains intestinal barrier integrity. 4OI rescues NEC by regulating macrophage mitochondrial activity.
3
项与 4-octyl itaconate 相关的新闻(医药)2025-04-02
·奇点网
*仅供医学专业人士阅读参考近年来,免疫检查点抑制剂在很多恶性肿瘤中都表现出了不错的临床疗效,也给很多晚期癌症患者带来了希望。但获得性耐药仍是免疫检查点抑制剂治疗过程中不可避免的问题。既往有研究显示,获得性耐药与肿瘤微环境代谢改变有关。因此,观察并探究在PD-1抑制剂治疗过程中,肿瘤微环境代谢的变化情况以及其对治疗效果的影响,不仅是充分了解获得性耐药机制的关键,也是当前免疫治疗研究的重要方向。近期,华中科技大学同济医学院附属协和医院杨坤禹/万超团队就发表了一项重要研究成果。他们利用代谢组学分析发现,在PD-1抑制剂治疗过程中,巨噬细胞来源的衣康酸是导致免疫治疗耐药的一个重要因素。具体来说,研究发现,PD-1抑制剂治疗后,CD8阳性T细胞产生的IFN-γ可通过JAK-STAT1信号通路上调巨噬细胞中衣康酸合成酶(顺乌头酸脱羧酶1,ACOD1)的表达,促进了衣康酸的生成,这进一步影响了树突状细胞的抗原呈递功能,从而抑制了CD8阳性T细胞的抗肿瘤免疫反应,最终导致免疫治疗耐药。研究发表在Cancer Research上[1]。论文首页截图为了更好地分析PD-1抑制剂治疗过程中肿瘤微环境的代谢变化情况,研究人员构建了肺癌荷瘤小鼠模型,并对其肿瘤组织进行了非靶向代谢组学分析。结果发现,与对照组小鼠肿瘤组织相比,接受PD-1抑制剂治疗的小鼠肿瘤组织中衣康酸及其衍生物4-OI的丰度出现了明显增加的现象。代谢组学分析鉴于ACOD1是目前衣康酸唯一已知的合成酶,研究人员还观察了PD-1抑制剂治疗后,ACOD1在肿瘤组织中的表达情况,结果同样发现,ACOD1表达显著上调的现象。此外,研究还在多个接受免疫检查点抑制剂治疗的临床队列数据集中观察到,ACOD1表达上调与疾病进展和患者不良结局密切相关。以上结果提示,ACOD1表达上调以及衣康酸水平的升高可能是导致PD-1抑制剂耐药的关键因素。多个临床队列中,ACOD1表达上调与疾病进展和患者不良结局密切相关随后通过构建Acod1基因敲除小鼠模型,研究人员发现,Acod1敲除小鼠在PD-1抑制剂治疗后表现出更强的抗肿瘤免疫反应和更好的总生存期。此外,研究人员还观察到,外源性补充或向肿瘤中注射衣康酸及其衍生物4-OI,会显著抑制Acod1敲除小鼠的免疫治疗效果,这进一步证明了ACOD1和衣康酸在免疫治疗耐药中发挥了关键作用。Acod1敲除可提高免疫治疗效果接下来,利用流式细胞术,研究人员还发现,在PD-1抑制剂治疗过程中,Acod1敲除会显著增加树突状细胞的浸润,以及CD8阳性T细胞的抗肿瘤免疫反应(在去除CD8阳性T细胞的情况下,Acod1敲除对PD-1抑制剂治疗的改善效果会完全消失),而补充衣康酸则会抑制树突状细胞的抗原呈递功能(表现为共刺激分子,如CD80、CD86和MHC-II表达减少),并削弱CD8阳性T细胞的抗肿瘤免疫反应。流式细胞术进一步,通过分析人类黑色素瘤和肺腺癌单细胞转录组学研究数据,研究人员发现,ACOD1会在巨噬细胞中高度表达,而随后的免疫荧光分析揭示了,在PD-1抑制剂治疗过程中,衣康酸的合成和分泌主要可归因肿瘤相关巨噬细胞。衣抗酸的合成和分泌主要可归因肿瘤相关巨噬细胞鉴于PD-1抑制剂治疗会增强CD8阳性T细胞的活化,从而产生大量的IFN-γ。研究人员使用公共RNA-seq数据集对598名肺腺癌患者进行了基因表达相关性分析,结果发现,IFNG和ACOD1的表达水平呈显著正相关。提示,PD-1抑制剂治疗后,CD8阳性T细胞产生的IFN-γ可能是ACOD表达上调和随后衣康酸产生的主要驱动因素。IFNG和ACOD1的表达水平呈显著正相关最后,在具体的分子机制上,研究人员发现,PD-1抑制剂治疗后,CD8阳性T细胞产生的IFN-γ可通过JAK-STAT1信号通路上调巨噬细胞中ACOD1的表达,促进了衣康酸的生成,这进一步影响了树突状细胞的抗原呈递功能,从而抑制了CD8阳性T细胞的抗肿瘤免疫反应,最终导致免疫治疗耐药。机制相关研究结果总之,该研究证实,巨噬细胞来源的衣康酸是导致免疫治疗耐药的一个重要因素,并揭示了其背后的分子机制。此外,研究还发现,靶向ACOD1,可通过抑制衣康酸的生成,有效增强免疫治疗效果。这些结果也为免疫治疗的耐药机制,以治疗策略的优化提供了新思路。参考文献:[1]Yang X,Deng Y,Ye Y,et al.Macrophage-Derived Itaconate Suppresses Dendritic Cell Function to Promote Acquired Resistance to Anti-PD-1 Immunotherapy.Cancer Res.Published online March 4,2025.doi:10.1158/0008-5472.CAN-24-2982本文作者丨张金旭
免疫疗法放射疗法临床研究
2024-06-28
Researchers have made a significant breakthrough by discovering that the drug 4-OI can enhance the effectiveness of a cancer-fighting viral agent. This may lead to treatment of cancers that are otherwise resistant to therapies.
Researchers from Aarhus University have made a significant breakthrough by discovering that the drug 4-OI can enhance the effectiveness of a cancer-fighting viral agent. This may lead to treatment of cancers that are otherwise resistant to therapies.
When a cancer cell doesn't respond to traditional therapies, doctors may turn to a sort of viral biological warfare, by deploying 'troops' in the form of viral agents that are specifically engineered to target and eliminate cancer cells. The mode of attack is to transform the tumor into an immunologically "hot" environment, making it more visible and recognisable to our immune system.
Now, researchers from the Department of Biomedicine at Aarhus University have found a way to make one strain of viral agents even more effective. And the results are groundbreaking says lead researcher, Associate Professor David Olagnier:
"We found that if we administer a specific viral agent called Vesicular Stomatitis Virus (VSVD51) along with a metabolite-drug called 4-Octyl-Itaconate (4-OI), we are able to treat cancers that are considered resistant to viral infections."
In other words, by combining the drug and the viral agent, the researchers have managed to push the door open to possible treatments for cancers that have been immune to nearly all known treatments, including the viral agents. This is because some cancers have antiviral signaling, which enables them to combat the viral agents and resist the treatment.
The results are particularly surprising because the drug 4-OI has, in other combinations, shown to have the completely opposite effect on different types of viruses. 4-OI is normally antiviral -- meaning it would actually stop viruses rather than boost them. But in this specific combination, 4-OI instead helps the cancer fighting viral agents to work better:
"It is the combination of the specific virus and the drug that brings about a completely unique proviral effect, which potentially can have a significant impact on patients affected by cancer that we are currently unable to treat," explains David Olagnier.
The new findings are an important step towards a new form of treatment, and they underline the need for consistently working to find new ways to treat the many forms of cancer we face, says David Olagnier:
"Cancer is not a single disease but rather a hundred diseases with one name, so it is crucial that we develop multiple ways to eradicate the disease. The use of biologically active viral agents can potentially be a gamechanger for some currently incurable cancers. That's why our findings are so exciting and groundbreaking," he explains.
For the research team, the next step is a more extensive pre-clinical testing of the combinational use of VSVD51 and 4-OI.
"We are especially interested in testing this combination on tumours that have metastasised, which is when the cancer has started to spread, but also on liquid types of cancer like lymphomas," explains David Olagnier.
2023-08-28
·生物谷
2023年8月24日,清华大学药学院尹航课题组在《Cell Reports》上发表了题为“4-Octyl itaconate restricts STING activation by blocking its palmitoylation”的研究文章。发现衣康酸的衍生物4-辛基衣康酸(4-Octyl itaconate, 4-OI)能够直接烷基化修饰STING的Cys91,从而阻断了STING Cys91位点的棕榈化修饰,抑制了STING的寡聚和下游信号的激活。研究背景天然免疫系统是哺乳动物抵抗外来病原入侵的第一道防线。cGAS-STING信号通路是胞内识别双链DNA的主要天然免疫信号通路。cGAS识别胞质中病毒或者自身来源的双链DNA,以ATP和GTP为底物合成信使分子2’,3’-环状鸟苷酸-腺苷酸 (2’,3’-cGAMP) 激活下游接头蛋白STING。在静息状态下STING以二聚体的形式存在于内质网上,cGAMP和STING结合,STING发生构象变化并寡聚,寡聚后的STING由内质网迁移至反式高尔基体。STING寡聚化可促进与STING结合的TBK1之间的相互磷酸化。磷酸化激活后的TBK1接着可磷酸化STING,STING的磷酸化为IRF3的结合提供锚定,随后IRF3再被TBK1磷酸化。磷酸化的IRF3二聚化并转运至细胞核发挥转录活性,促进I型干扰素等炎症细胞因子的转录产生[1]。cGAS-STING通路主要参与到机体的抗病原微生物尤其是DNA病毒的免疫反应过程中。同时由于cGAS并不能很好区分自身和外源DNA,其异常激活也会造成一些自身免疫疾病。因此对cGAS-STING通路在不同环境下进行精准的调控,不仅可以增强人们对其功能的理解,也便于通过调控该通路去更好的应对感染和相关的自身免疫疾病。研究内容近年来越来越多的研究关注到免疫和代谢之间的相互调控。研究团队通过筛选三羧酸循环常见代谢物或其衍生物对cGAS-STING通路激活的影响,发现衣康酸衍生物4-辛基衣康酸(4-OI)能够明显抑制DNA诱导的cGAS-STING信号通路的激活。之前有报道4-OI能够通过激活Nrf2抑制炎症因子产生,但研究团队发现Nrf2的敲除并不影响4-OI对cGAS-STING的抑制,因此4-OI对cGAS-STING通路的抑制并不依赖于Nrf2。进一步研究发现4-OI并不影响通路中cGAS, TBK1和IRF3的活性,4-OI直接抑制STING的激活。图1 衣康酸(Itaconate)和4-OI的结构衣康酸以及4-OI都含有一个亲电子的不饱和双键,能和蛋白质半胱氨酸巯基发生加成反应,共价修饰蛋白质来调控蛋白的功能(图1)。因此接下来,研究人员探究4-OI是否能够通过直接共价修饰STING发挥抑制作用。通过4-OI的化学生物学探针点击化学标记实验,以及LC-MS/MS蛋白质质谱研究分析,研究团队发现4-OI能够直接修饰STING的Cys91位点,同时4-OI对Cys91位点突变体STING丧失了抑制活性,进一步证明了4-OI是通过靶向STING的Cys91位点发挥抑制作用的。STING Cys91位点的棕榈酰化对于其寡聚激活起到重要作用。进一步利用棕榈酰化Click探针标记实验,发现4-OI能够抑制STING的棕榈酰化修饰,同时利用Native PAGE实验也发现4-OI能够抑制激活诱导的STING寡聚。随后,在双链DNA病毒单纯疱疹病毒HSV-1感染模型以及cGAS-STING相关自身免疫炎症模型中,研究团队也证明了4-OI对cGAS-STING激活的抑制作用。4-OI作为衣康酸的衍生物,先前的研究大多将其视为衣康酸的替代物,认为4-OI相比衣康酸本身更容易通过细胞膜,同时在细胞内4-OI被能转化为衣康酸发挥免疫调节作用。研究团队接下来便验证内源性衣康酸是否会影响STING的激活。出人意料的是,不管是直接的高浓度衣康酸处理或者是将衣康酸生成的酶IRG1敲除都不会影响cGAS-STING的激活,这表明衣康酸并不影响cGAS-STING的激活,4-OI和衣康酸并不能被简单的等同,4-OI在胞内并没有被完全降解为衣康酸从而发挥其独特的免疫调节功能。 另外值得一提的是,Cell Reports在2023年3月份发表了一篇类似的文章,发现4-OI能够烷基化修饰STING的Cys147抑制STING的二聚从而抑制STING激活,且衣康酸也能够抑制STING的激活[2]。而本研究发现4-OI是通过烷基化修饰STING的Cys91位点阻断STING棕榈酰化,从而抑制STING的寡聚和激活,同时内源性衣康酸的作用和4-OI并不相同。图2 4-OI烷基化修饰STING抑制STING棕榈酰化和寡聚激活研究结论总之,本研究发现衣康酸衍生物4-OI能够通过烷基化修饰STING,抑制了STING的棕榈酰化从而抑制了STING的激活,展现了STING不同翻译后修饰之间存在相互影响(图2)。同时本研究也表明4-OI能够抑制cGAS-STING介导的免疫炎症,或可为相关自身免疫疾病的治疗提供新的策略。原文链接:https://www-cell-com.libproxy1.nus.edu.sg/cell-reports/fulltext/S2211-1247(23)01051-3会议推荐会议详情会议名称:2023(第14届)细胞与基因治疗研讨会暨抗体工程与创新免疫治疗技术论坛主办单位:生物谷、梅斯医学、同济大学附属同济医院、南京可缘大会时间:9月22-23日大会地点:上海 大会规模:1500人2010年至今,生物谷联合各合作单位已经顺利召开了13届细胞与基因治疗研讨会,与全球致力于细胞治疗行业同仁们一同成长沉淀,在提供行业信息交流平台的同时,也为基础研究提供了技术/产品等产业化的孵化平台。基于此,本届会议将继续以转化医学为切入点,以基础研究与临床应用相结合,针对细胞治疗的临床前沿研究、临床监管、治疗规范、细胞治疗安全性,免疫细胞新型疗法、实体瘤治疗、干细胞与癌症、抗体药物、核酸药物、基因编辑、肿瘤免疫治疗等热门议题进行讨论,诚邀国内外产学研医专家共聚,共绘产业发展新蓝图!长按识别二维码立即报名参会
免疫疗法
100 项与 4-octyl itaconate 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 脓毒症 | 临床前 | 中国 | 2025-06-16 | |
| Cryopyrin相关周期性综合征 | 临床前 | 西班牙 | 2025-05-23 | |
| 术后认知功能障碍 | 临床前 | 中国 | 2024-04-22 | |
| 系统性红斑狼疮 | 临床前 | 中国 | 2018-11-22 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
No Data | |||||||
登录后查看更多信息
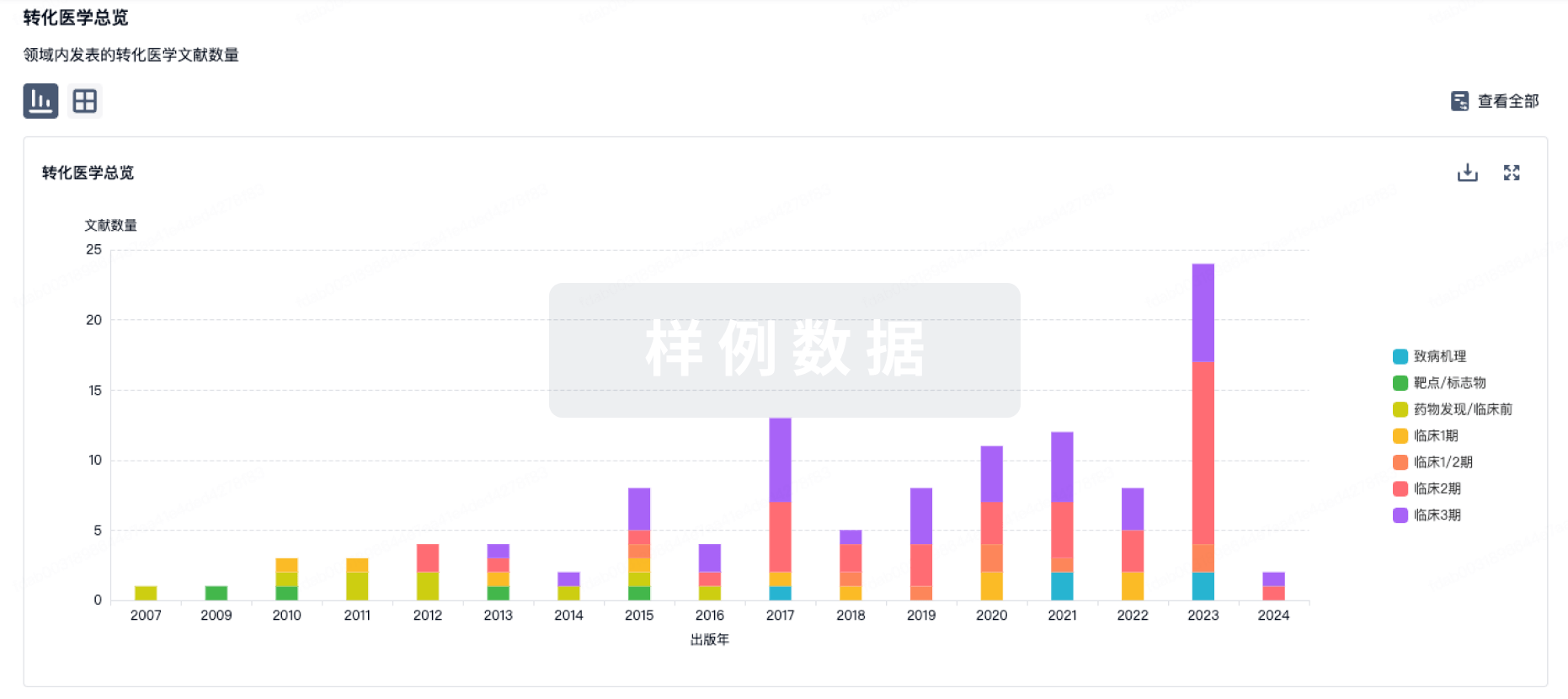
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
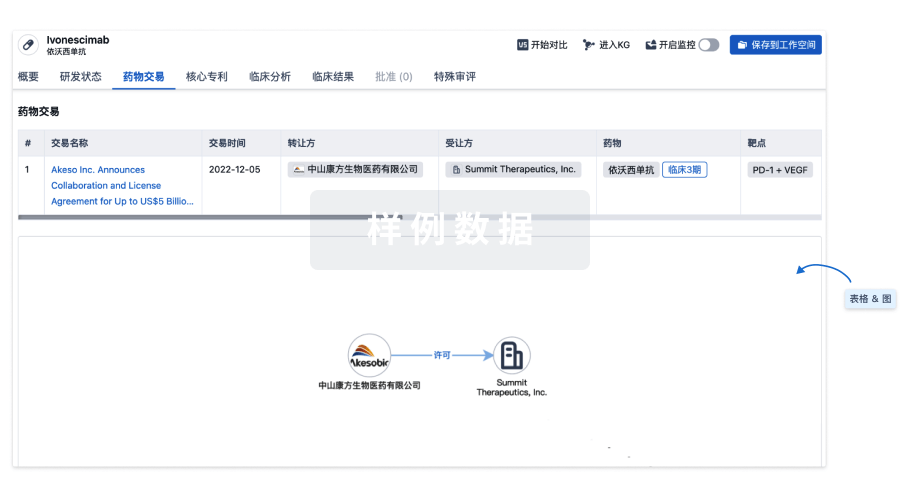
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
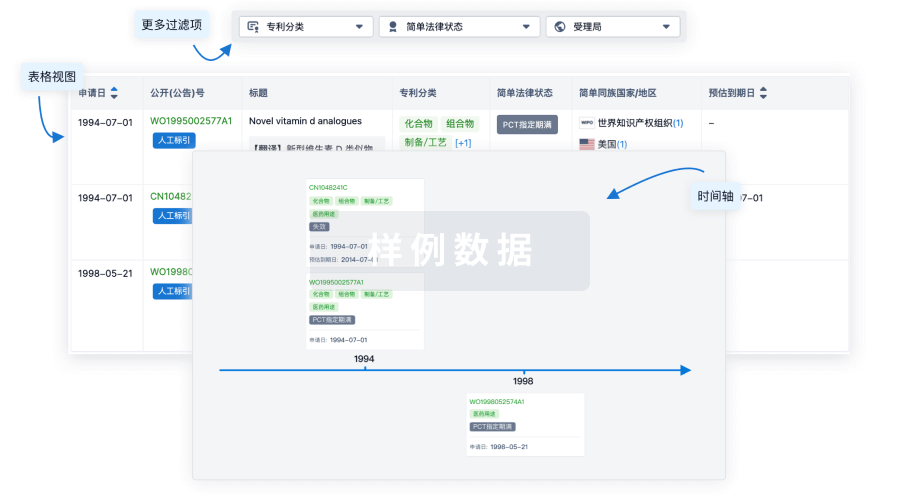
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
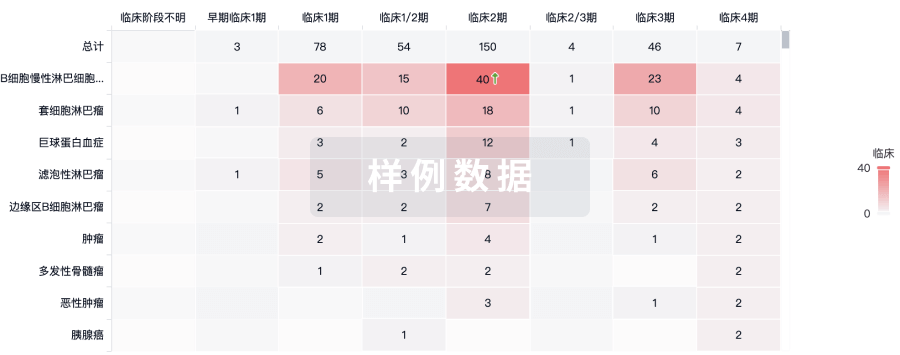
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
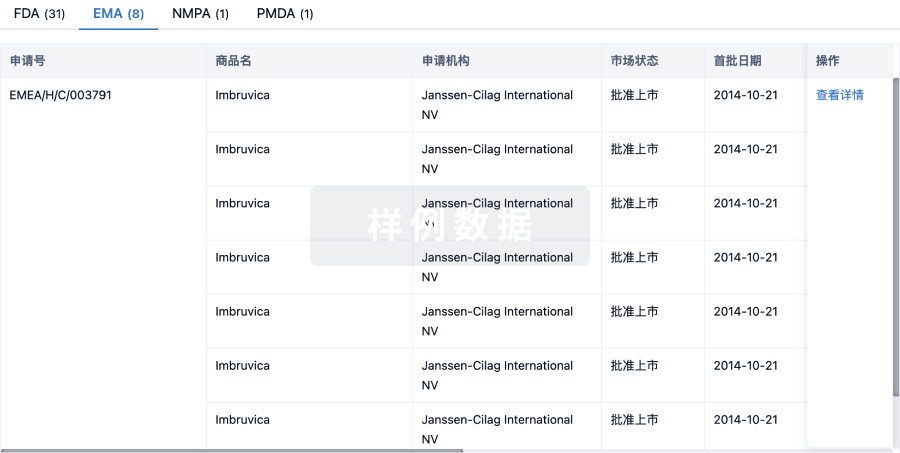
批准
利用最新的监管批准信息加速您的研究。
登录
或
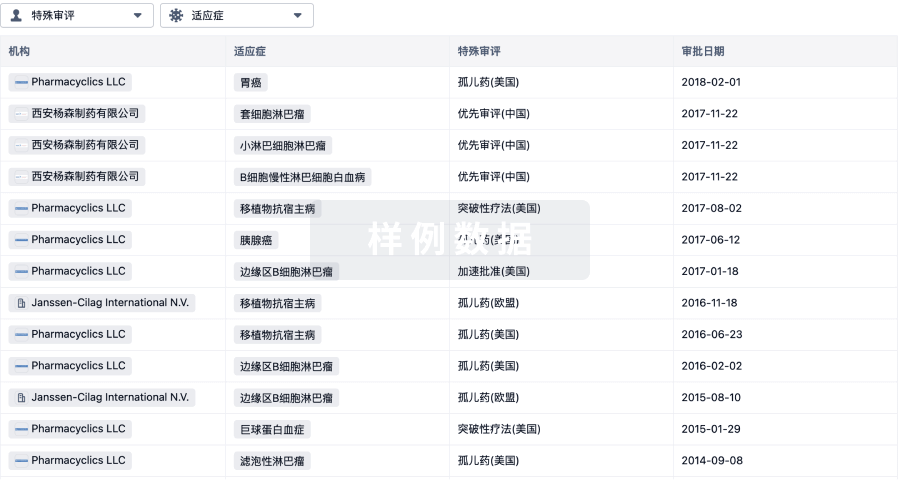
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用



