更新于:2024-05-01
ACR
acrosin
更新于:2024-05-01
基本信息
别名 ACR、Acrosin、Acrosin heavy chain + [4] |
简介 Acrosin is the major protease of mammalian spermatozoa. It is a serine protease of trypsin-like cleavage specificity, it is synthesized in a zymogen form, proacrosin and stored in the acrosome. |
关联
100 项与 ACR 相关的临床结果
登录后查看更多信息
100 项与 ACR 相关的转化医学
登录后查看更多信息
0 项与 ACR 相关的专利(医药)
登录后查看更多信息
2,153
项与 ACR 相关的文献(医药)2024-03-04·The Journal of cell biology
Rab32 family proteins regulate autophagosomal components recycling.
Article
作者: Zhe Wu ; Huilin Que ; Chuangpeng Li ; Li Yan ; Shixuan Wang ; Yueguang Rong
In autophagy, autophagosomes deliver the lumenal contents to lysosomes for degradation via autophagosome-lysosome fusion. In contrast, autophagosome outer membrane components were recycled via autophagosomal components recycling (ACR), which is mediated by the recycler complex. The recycler complex, composed of SNX4, SNX5, and SNX17, cooperate with the dynein-dynactin complex to mediate ACR. However, how ACR is regulated remains unknown. Here, we found that Rab32 family proteins localize to autolysosomes and are required for ACR, rather than other autophagosomal or lysosomal Rab proteins. The GTPase activity of Rab32 family proteins, governed by their guanine nucleotide exchange factor and GTPase-activating protein, plays a key role in regulating ACR. This regulation occurs through the control of recycler complex formation, as well as the connection between the recycler-cargo and dynactin complex. Together, our study reveals an unidentified Rab32 family-dependent regulatory mechanism for ACR.
2024-02-21·Kidney & blood pressure research
The association between urinary sodium-potassium ratio, kidney function, and blood pressure in a cohort from the general population.
Article
作者: Karl Marius Brobak ; Toralf Melsom ; Bjørn Odvar Eriksen ; Aud Høieggen ; Jon Viljar Norvik ; Marit Dahl Solbu
Introduction Subclinical kidney dysfunction may contribute to salt sensitive hypertension. We assessed the association between the urinary sodium-potassium ratio (Na/K-ratio) and blood pressure (BP) in a general population cohort without diabetes, chronic kidney disease, cardiovascular disease or treated hypertension. We investigated whether any such association was mediated by the kidney function markers measured glomerular filtration rate (mGFR), urinary albumin creatinine ratio (ACR) and epidermal growth factor - creatinine ratio (EGF-Cr). Methods The Tromsø Study is a population-based study of inhabitants of the municipality of Tromsø, Northern Norway. Participants aged 50-62 years, without diabetes, chronic kidney disease or cardiovascular disease, were invited to the substudy Renal Iohexol Clearance Survey in Tromsø 6 (RENIS-T6; 2007-09). For the present study we excluded participants reporting the use of 1 or more antihypertensive agents, leaving 1311 RENIS-T6 participants for a cross-sectional analysis. We measured office BP, 24-hour ambulatory blood pressure (ABP) and mGFR using iohexol-clearance. Na/K-ratio, ACR, and EGF-Cr were measured in morning urine samples. Results Urinary Na/K-ratio was significantly associated with systolic office BP and ABP independently of cardiovascular risk factors and kidney function markers. A one standard deviation unit increase in the Na/K-ratio was associated with increased systolic ABP by 1.0 (0.3-1.6) mmHg. Urinary Na/K-ratio showed a stronger association with office BP than ABP. EGF-Cr, ACR and mGFR did not mediate the relationship between urinary Na/K-ratio and systolic BP. Conclusions In a representative sample of the middle-aged North-European population without diabetes, chronic kidney disease, cardiovascular disease or treated hypertension, there was a consistent association between urinary Na/K-ratio and BP. The association with BP was not mediated through kidney function measures, suggesting a relationship between a diet with high sodium and low potassium and higher BP regardless of kidney function.
2024-02-15·Journal of fungi (Basel, Switzerland)
Processes Controlling the Contractile Ring during Cytokinesis in Fission Yeast, Including the Role of ESCRT Proteins.
Review
作者: Imane M Rezig ; Wandiahyel G Yaduma ; Christopher J McInerny
Cytokinesis, as the last stage of the cell division cycle, is a tightly controlled process amongst all eukaryotes, with defective division leading to severe cellular consequences and implicated in serious human diseases and conditions such as cancer. Both mammalian cells and the fission yeast Schizosaccharomyces pombe use binary fission to divide into two equally sized daughter cells. Similar to mammalian cells, in S. pombe, cytokinetic division is driven by the assembly of an actomyosin contractile ring (ACR) at the cell equator between the two cell tips. The ACR is composed of a complex network of membrane scaffold proteins, actin filaments, myosin motors and other cytokinesis regulators. The contraction of the ACR leads to the formation of a cleavage furrow which is severed by the endosomal sorting complex required for transport (ESCRT) proteins, leading to the final cell separation during the last stage of cytokinesis, the abscission. This review describes recent findings defining the two phases of cytokinesis in S. pombe: ACR assembly and constriction, and their coordination with septation. In summary, we provide an overview of the current understanding of the mechanisms regulating ACR-mediated cytokinesis in S. pombe and emphasize a potential role of ESCRT proteins in this process.
7
项与 ACR 相关的新闻(医药)2024-01-22
None
Chronic diseases are at an all-time high and are plaguing the U.S. 60% of adults are living with chronic illness, and life expectancy, as a result, is dropping nationally.
Chronic Kidney Disease (CKD) is one of many chronic illnesses that poses a significant threat to public health. About 37 million people in the United States have the condition, and 1 in 3 Americans living with Diabetes are likely to develop CKD. CKD costs Medicare over $130 billion dollars every year—nearly a quarter of all Medicare spending.
There are several reasons contributing to these poor health outcomes, such as a lack of health equity and awareness around these diseases, and disjointed public health strategies.
In response to these significant disparities in CKD management, the National Kidney Foundation (NKF) has outlined several key objectives to address these issues, including removing racial and ethnic barriers, enhancing diagnosis and treatment of CKD to prevent progression to kidney failure, and lowering the financial burden individuals with kidney conditions face.
Here is how these critical suggestions can come to life to improve the overall health of the U.S. and reduce chronic diseases, like CKD.
Evolve Diagnostic Modalities
Clinical recommendations state that Americans at-risk of CKD should be tested yearly by two complementary tests: the estimated glomerular filtration rate (eGFR) and albumin-to-creatinine ratio (ACR). eGFR and ACR are integral to providing indications of CKD at different stages of the disease.
Adherence to the ACR test has been consistently low for decades. Unlike eGFR, which is measured as part of a routine blood test, ACR, a urine test that can importantly identify CKD in earlier stages, is performed significantly less.
With clinical guidelines recommending ACR testing for at-risk populations. There is an urgent need to close the adherence gap and enable better solutions, potentially saving millions of lives and billions in healthcare expenditures.
Dismantle Health Disparities through Data and Collaboration
As reported by the National Kidney Foundation, Black Americans are almost four times more likely and Latinos are 1.3 times more likely to have kidney failure compared to White Americans. Additionally, 60 million Americans live in rural areas where access to healthcare may be low, and rates of mortality and chronic conditions are markedly higher. These populations suffer greatly from a lack of access and health literacy.
Data and digital innovation can help bridge this divide by outlining specific actions, uncover implicit biases and outline a path forward for caregivers.
Power Health Equity through At-Home Testing
Smartphone powered, at-home testing for CKD provides a tangible and scalable solution to this problem offering many benefits, including convenience and accessibility, alongside ease of use. By enabling members to test at home and receive immediate results health plans can increase at scale the compliance rates of previously untested populations.
Minuteful Kidney is a uACR test that is conducted using a smartphone app. The service is compatible with most smartphones and operating systems, making it accessible to virtually anyone with a smartphone.
Today, tens of thousands of health plan members have already used Minuteful Kidney to home test for CKD, improving adherence rates - with 50% test completion and 84% of patients returning to care following a diagnosis.
Expanding Access and Coverage
Further collaboration across the healthcare ecosystem with providers, payors and policymakers can ensure access to new innovations. The key to mitigating the kidney disease crisis in the U.S. is to improve early detection. Together, we can broaden awareness, and enable people at risk to overcome barriers to care – on a national scale.

临床研究
2023-08-04
·生物谷
近日,上海交通大学生命科学技术学院微生物代谢国家重点实验室邓子新团队康前进研究小组于国际权威期刊《自然·通讯》(Nature Communications)杂志上发表题为“Insertion sequence transposition inactivates CRISPR-Cas immunity”的研究论文。上海交大博士研究生盛勇和王珩瑜两位同学为该论文的共同第一作者。上海交大康前进副研究员、白林泉教授与邓子新教授为共同通讯作者。该研究还得到了林双君教授、陶美凤教授、丁伟特别研究员、唐满成特别研究员和上海农业科学院吴莹莹副研究员的大力支持。该工作首先通过综合应用生物信息学、分子生物学、遗传学和基因组学等多种技术手段,揭示了细菌如何利用插入序列(insertion sequences, ISs)在遗传防御与有益外源基因获取之间进化的权衡。在长期的生物进化长河中,CRISPR-Cas免疫系统被认为是广泛存在于细菌和古菌中的一种适应性免疫系统,可以有效保护宿主免受噬菌体和其他可移动元件的入侵。然而,从进化的角度来看,CRISPR-Cas免疫系统却是一把“双刃剑”。一方面,它可以抵御外来遗传物质的入侵,但同时也会限制有益外源基因的获取,在一定程度上阻碍了细菌在胁迫环境中的适应性进化。图1. IS元件转座至CRISPR-Cas系统为了研究细菌如何应对CRISPR-Cas免疫系统所带来的不利影响,通过对CRISPRCasdb数据库中所有的CRISPR-Cas系统进行了系统分析,发现了众多天然的CRISPR-Cas屏障被IS转座所破坏(图1),推测了这一现象可能与有益外源基因的获取相关。随后,研究人员通过一系列分子生物学与遗传学实验在实验室条件下成功模拟了CRISPR-Cas免疫系统与基因水平转移之间的进化权衡关系。实验结果表明,宿主菌株在经历抗生素胁迫的巨大压力下,IS元件通过转座至cas基因,实现宿主菌与带有protospacer序列的外源抗生素耐药质粒的凤凰涅槃以及宿主菌在抗生素存在的环境中得以永生。为了进一步研究IS转座特性,研究人员利用具有单个效应蛋白的type II (SpCas9) 与type V (FnCpf1) CRISPR-Cas系统在大肠杆菌中构建了一套高效的IS元件捕获系统(图2)。该系统能够选择性地捕获和分析转座至cas基因的IS元件,为解析IS转座至CRISPR-Cas系统及其对细菌适应性进化的影响提供了有力工具。为了进一步探索IS元件转座至cas基因的诱因,研究人员对SpCas9-HF1蛋白的RuvC与HNH结构域分别进行了单突变与组合突变,获得了三种具有不同切割能力的蛋白突变体。这些突变体包括对靶标链进行单链切割的SpCas9-HF1 (D10A)、对非靶标链进行单链切割的SpCas9-HF1 (H840A)以及仅结合,不切割的SpCas9-HF1 (D10A & H840A)。通过大量的质粒侵染实验及PCR验证,研究人员发现只有当SpCas9-HF1蛋白对染色体进行双链DNA断裂时,才会诱发IS元件转座至cas基因(图2)。图2. 基于CRISPR-Cas建立高效的IS元件捕获系统接着,研究人员基于密码子的简并性,对Cas核酸酶编码序列进行了三轮的迭代突变,使其DNA序列尽可能地规避IS元件识别的热点motif。然而,令人意想不到的是,即使对核酸酶编码序列进行了重构,仍然以IS1与IS10为主要的转座类型。通过对这两个元件的识别序列进行系统的比较分析,发现了正是由于这两个元件在靶标序列识别上呈现的巨大宽泛性潜能,才使得它们成为破坏CRISPR-Cas免疫系统的主要“武器”。接着,研究人员在IS元件捕获系统中,异源整合了三种修复能力不同的NHEJ(non-homologous end joining)修复系统。他们发现,尽管IS的转座频率有所下降,但转座事件仍然发生。这一结果表明,原核生物可能无法单独依靠NHEJ系统完全修复CRISPR-Cas系统引发的DNA损伤。进一步凸显了IS元件在驱动菌株对环境适应性中的重要地位。最后,研究人员通过组合大量的生物信息学工具对整个NCBI数据库中古菌、细菌与病毒中IS元件的分布进行了系统分析。结果表明,IS元件广泛存在于细菌与古菌中,且各IS家族的拷贝数存在很大差异。IS元件的广泛分布意味着它们在不同宿主中可能发挥着关键功能,通过参与宿主的适应性进化过程,从而推动宿主基因组多样性和适应性演化。为了更深入地理解IS元件在宿主进化中的作用,研究人员还探究了IS元件与其他原核生物防御系统的相互作用。有趣的是,通过系统的筛查,发现IS1与IS10转座到除了CRISPR-Cas系统以外的12种不同的防御系统中,例如限制性修饰系统与基于环状寡核苷酸的抗噬菌体信号系统等(图3)。这意味着IS元件可能通过干扰宿主的遗传防御系统,从而增加宿主获取外源有益基因的能力,并促进其自身的适应性进化。图3. IS1与IS10元件转座至多种不同的原核生物遗传防御系统迄今为止,主要发现了两种可以失活CRISPR-Cas免疫系统的机制:一类是Acr蛋白(Anti-CRISPR proteins),通过直接结合Cas蛋白来抑制Cas蛋白和crRNA组装成活性复合物,或对crRNA进行降解。另一类是噬菌体利用编码的整合酶,通过自身的attP位点与宿主基因组中的attB位点发生位点特异性重组,将基因组序列整合至宿主的CRISPR array区域,从而干扰crRNA的转录与成熟。该研究揭示了另一种高效失活CRISPR-Cas系统的机制—IS元件转座拆除的CRISPR-Cas免疫系统(图4)。这一重要发现进一步拓宽了我们对CRISPR-Cas失活机制的认知范围。图4. anti-CRISPR机制总览综上所述,这项研究表明,IS元件通过破坏宿主免疫系统,促使细菌更容易获得有益外源基因,介导了细菌遗传防御和有益外源基因获取之间的进化权衡关系,揭示了IS元件如何与宿主免疫系统相互作用,导致适应性基因的获取和整合。通过深入了解IS元件在不同环境中转座的诱因和影响因素,我们可以更好地理解细菌的遗传多样性以及其在不同环境下的定殖、生存和进化策略,并为微生物学、生物技术等相关领域的研究和应用提供重要的指导和启示。论文链接:https://www-nature-com.libproxy1.nus.edu.sg/articles/s41467-023-39964-7会议推荐大会信息 会议名称 | 2023(第九届)肠道微生态与健康研讨会会议时间 | 2023年11月会议形式 | 线下会议地点 | 上海(定向通知)大会规模 | 800人主办单位 | 生物谷、梅斯医学联合主办 | 复旦大学微生物组中心上海交通大学生命科学技术学院上海究本科技有限公司扫码立即报名
基因疗法微生物疗法临床研究
2023-01-30
·生物谷
基于印迹基因的QCIGISH检测在区分甲状腺结节良恶性上具有很高的诊断效能,其对恶性结节很高的阴性预测值证明其在排除恶性肿瘤上非常有效,同时,很高的阳性预测值可使得其作为一种有效的检测方法
甲状腺结节的患病率很高,在成人群体中以超声检查方式统计的患病率为70%,其中约5%的结节是恶性的[1],而良恶性结节的治疗方式及预后差别巨大。因此,准确判断甲状腺结节的良恶性对于其临床管理至关重要。
目前,超声影像学联合细针穿刺(FNA)活检是甲状腺结节诊断的主要方法,但约20%-30%的甲状腺结节仍无法通过这种方法确定性质[2]。因此,急需开发新的检测方法以提高其诊断精确度。
基于生物标志物的肿瘤检测,极大地改变了肿瘤检测的格局,其中基因组印迹作为肿瘤发生过程中的表观遗传标志物,与多种肿瘤的发生关系密切[3],然而这种基因印迹的检测却存在较高的技术壁垒。
近日,由南方科技大学邢明照教授领衔的研究团队在Journal of Clinical Oncology发表了一项重要研究成果。研究发现,基于印记生物标志物的检测可有效区分良恶性甲状腺结节,尤其对于甲状腺恶性结节,敏感性高达100%[4],表明基于印迹基因的新检测方法,在甲状腺结节的临床诊断方面具有很高的潜力。
图1. 文章封面截图
研究人员纳入了中国科学院大学肿瘤医院等8个大型医疗中心550名甲状腺结节患者的病理标本,其中124例(82例恶性结节和42例良性结节)为术后石蜡标本,用于初步诊断模型的构建,32例(8例恶性结节和24例良性结节)为术前甲状腺穿刺标本、用于模型优化,394(117例恶性结节和277例良性结节)例为术后组织病理学的穿刺样本,以进行前瞻性验证研究(图2)。
图2. 研究设计和流程图
由于印迹基因检测存在较高的技术难度,因此,如何完成这550例样本的印迹基因检测就成了研究的核心。
RNA原位杂交(ISH)方法是检测印迹和非印迹基因的转录调控的传统技术[5],为了精确定量印迹基因,研究人员基于这种传统技术,开发出一种更为先进的定量显色印迹基因原位杂交技术(QCIGISH),并鉴定出三个具有癌症诊断潜力的印迹基因:鸟嘌呤核苷酸结合蛋白-α刺激复合物位点(GNAS),生长因子受体结合蛋白(GRB10)和小核核糖核蛋白多肽N(SNRPN)[6]。
那基于QCIGISH检测这些癌症特异性印迹基因,是否可以准确判断出甲状腺结节的良恶性呢?
基于QCIGISH检测技术,研究人员使用靶向GNAS、GRB10、SNRPN和HM13非编码内含子序列的探针进行印迹基因检测,并测量其双等位基因表达(BAE)、多等位基因表达(MAE)和总表达(TE)来对印迹基因的灵敏性和特异性进行客观定量(图3A)。随后,研究人员通过结节组织连续切片进行QCIGISH检测和HE染色,以分析这四种印迹基因表达与甲状腺结节良恶性的相关性(图3B)。
图3. QCIGISH的原理-印迹基因等位基因表达状态的可视化、定量和病理确认
完成初始化模型构建和模型优化后,研究人员对394例用于前瞻性验证的临床样本进行了QCIGISH临床适用性的测试,发现超声检查ACR TI-RADS分类中3-5级结节中组织病理恶性肿瘤率随级别增加逐渐升高,Bethesda分型也发现级别越高恶性肿瘤率也越高。
随后,研究人员以组织病理学诊断作为标准,评估了QCIGISH分级模型的诊断效能:QCIGISH诊断甲状腺恶性结节的总体敏感性为100%,良性结节的特异性为91.5%,总体阳性预测值(PPV)为96.5%,恶性肿瘤的阴性预测值(NPV)为100%(图4),相应的总体诊断准确率为97.5%(384/394)。
图4. QCIGISH诊断甲状腺结节的诊断效能
接下来,研究人员评估了QCIGISH在不同Bethesda分型患者中的诊断效能:
对于Bethesda II型甲状腺结节,100%(83/83)的QCIGISH阴性病例为组织病理学良性,而42.9%(6/14)的QCIGISH阳性病例为组织病理学恶性(图5D);
对于Bethesda III和IV型甲状腺结节,QCIGISH阴性病例中100%(23/23)为组织病理学良性结节,QCIGISH阳性病例中96.6%(56/58)为组织病理学恶性结节,PPV为96.6%,NPV为100%(图5E),诊断恶性甲状腺结节的总体准确率为97.5%(79/81);
对于Bethesda V型甲状腺结节,仅一例为QCIGISH阴性且为组织病理学良性结节,而100%(31/31)的QCIGISH阳性病例为组织病理学恶性结节(图5F);
对于Bethesda VI型甲状腺结节,100%(184/184)的QCIGISH阳性病例为组织病理学恶性结节(图5G)。
图5. QCIGISH诊断不同Bethesda分型甲状腺结节的诊断效能
综上所述,基于印迹基因的QCIGISH检测在区分甲状腺结节良恶性上具有很高的诊断效能,其对恶性结节很高的阴性预测值证明其在排除恶性肿瘤上非常有效,同时,很高的阳性预测值可使得其作为一种有效的检测方法,以辨别细胞学上不确定的甲状腺结节。这项研究提供了一种新的甲状腺分子诊断检测方法,或可改变甲状腺临床诊断的格局。
参考文献:
[1] Guth S, Theune U, Aberle J, et al. Very high prevalence of thyroid nodules detected by high frequency (13 MHz) ultrasound examination. Eur J Clin Invest. 2009 Aug;39(8):699-706. doi: 10.1111/j.1365-2362.2009.02162.x.
[2] Wang CC, Friedman L, Kennedy GC, et al. A large multicenter correlation study of thyroid nodule cytopathology and histopathology. Thyroid. 2011 Mar;21(3):243-51. doi: 10.1089/thy.2010.0243.
[3] Jelinic P, Shaw P. Loss of imprinting and cancer. J Pathol. 2007 Feb;211(3):261-8. doi: 10.1002/path.2116.
[4] Xu H, Zhang Y, Wu H, et al. High Diagnostic Accuracy of Epigenetic Imprinting Biomarkers in Thyroid Nodules. J Clin Oncol. 2022 Nov 15:JCO2200232. doi: 10.1200/JCO.22.00232.
[5] Kohda A, Taguchi H, Okumura K. Visualization of biallelic expression of the imprinted SNRPN gene induced by inhibitors of DNA methylation and histone deacetylation. Biosci Biotechnol Biochem. 2001 May;65(5):1236-9. doi: 10.1271/bbb.65.
[6] Shen R, Cheng T, Xu C, et al Novel visualized quantitative epigenetic imprinted gene biomarkers diagnose the malignancy of ten cancer types. Clin Epigenetics. 2020 May 24;12(1):71. doi: 10.1186/s13148-020-00861-1.

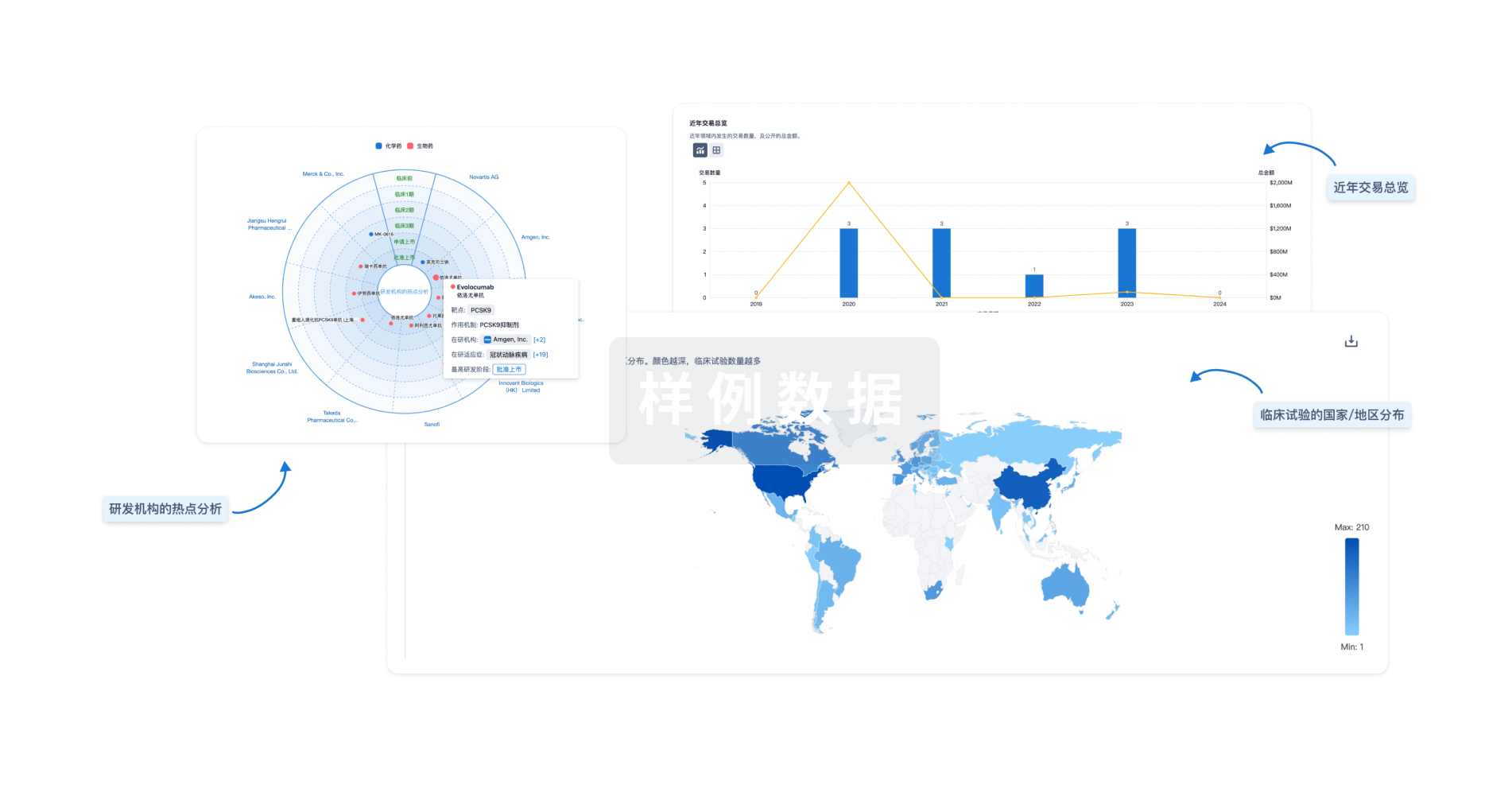
分析
对领域进行一次全面的分析。
登录
或
标准版
¥16800
元/账号/年
新药情报库 | 省钱又好用!
立即使用
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用