更新于:2024-09-19

Myair LLC
更新于:2024-09-19
概览
关联
100 项与 Myair LLC 相关的临床结果
登录后查看更多信息
0 项与 Myair LLC 相关的专利(医药)
登录后查看更多信息
3
项与 Myair LLC 相关的文献(医药)2021-05-03·Sleep
666 Sleep Architecture in the Intensive Care Unit As Revealed via Breathing and Heart Rate Variability
作者: Qader Quadri, Syed Abdul ; Da Silva Cardoso, Madalena ; Kuller, David ; Ye, Elissa ; Thompson, Taylor ; Velpula Krishnamurthy, Parimala ; Tesh, Ryan ; Adra, Noor ; Akeju, Oluwaseun ; Westover, Michael ; Ganglberger, Wolfgang ; Bucklin, Abigail ; Thomas, Robert ; Leone, Michael ; Sun, Haoqi
2021-05-01·TP131. TP131 NOVEL METHODOLOGIES FOR DIAGNOSING SLEEP DISORDERED BREATHING
High Prevalence of Undiagnosed Sleep Apnea in the Intensive Care Unit. Risk Factor Scores Cannot Substitute Objective Measurement
作者: Kuller, D. ; Subapriya, R. ; Paixao, L. ; Da Silva Cardoso, M. ; Ganglberger, W. ; Westover, M.B. ; Ju, Y. ; Panneerselvam, E. ; Thomas, R. ; Akeju, O. ; Higgins, J. ; Hemmige, A.R. ; Tesh, R. ; Thompson, B.T. ; Quadri, S. ; Leone, M. ; Krishnamurthy, P.V. ; Ayub, M.A. ; Sun, H. ; Bucklin, A. ; Adra, N.
Frontiers in Network Physiology
Sleep staging in the ICU with heart rate variability and breathing signals. An exploratory cross-sectional study using deep neural networks
Article
作者: Panneerselvam, Ezhil ; Thompson, B Taylor ; Rajan, Subapriya ; Bucklin, Abigail A ; Higgins, Jasmine ; Sun, Haoqi ; Shao, Yu-Ping ; Westover, M Brandon ; Da Silva Cardoso, Madalena ; Hemmige, Aashritha ; Akeju, Oluwaseun ; Ye, Elissa M ; Ayub, Muhammad Abubakar ; Coughlin, Brian ; Quadri, Syed A ; Ganglberger, Wolfgang ; Paixao, Luis ; Leone, Michael J ; Kuller, David ; Tesh, Ryan A ; Cash, Sydney S ; Adra, Noor ; Krishnamurthy, Parimala Velpula ; Thomas, Robert J
1
项与 Myair LLC 相关的新闻(医药)2024-02-13
The AirCurve 11 is designed to tailor its therapy to a user’s normal breathing patterns.
As Philips reaches a consent decree agreement with the FDA that will temporarily suspend its sales of sleep therapy devices in the U.S., competitor ResMed, meanwhile, is ramping up its product offerings.
ResMed unveiled the latest addition to its slate this week, announcing the launch of a new bi-level respiratory support device that will give doctors another option for treating their patients with sleep apnea beyond the segment-dominating CPAP machines. The AirCurve 11 device, which is compatible with all of ResMed’s masks, is now available in the U.S. with an international rollout on deck.
Bi-level devices like the AirCurve 11 provide two forms of positive airway pressure therapy—with different pressure levels depending on whether a user is inhaling or exhaling—compared to the single-level, continuous positive airway pressure of a CPAP machine.
The AirCurve 11 is also designed to match its therapy to a user’s normal breathing patterns with the help of an algorithm, dubbed ASVAuto, that looks for 13 indicators in the breath cycle 50 times per second to tailor the machine’s output to the length of the user’s inhales and exhales as well as their ventilation needs.
Meanwhile, that nightly output is wirelessly transferred to ResMed’s AirView cloud-based platform, where healthcare providers can monitor their patients’ therapy and remotely adjust it as necessary. The BiPAP machine data also go to the patient-facing myAir app, which they can use to track their progress and conduct regular check-ins about their treatment goals.
“We’ve seen patient compliance improve from 70% to 87% through the use of coaching features and the ability to track and view their nightly sleep data via MyAir and AirView, so we’ve incorporated these digital health applications into the new AirCurve11 series to enable maximum comfort and support throughout the therapy experience,” said Carlos Nunez, M.D., the company’s chief medical officer.
The new product launch comes shortly after ResMed CEO Mick Farrell touted the company’s ongoing hardware and software growth in its second-quarter earnings presentation.
For the first half of the company’s fiscal year 2024, which began July 1, ResMed reported revenues of more than $2.26 billion, up 14% from where it stood a year prior. Despite that solid revenue growth, however, ResMed’s first-half net income dropped 2%, from $435 million to $428 million, thanks to increased costs from acquisitions, the safety correction for its magnet-equipped masks and an ongoing reorg.
That restructuring began with the fiscal year and saw Farrell announce last fall the layoffs of 5% of ResMed’s 10,000-strong global workforce. It added expenses of just over $64 million in the second quarter, split primarily between employee severance payouts and the costs of winding down certain less profitable areas of the business.

财报
100 项与 Myair LLC 相关的药物交易
登录后查看更多信息
100 项与 Myair LLC 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2024年10月06日管线快照
无数据报导
登录后保持更新
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
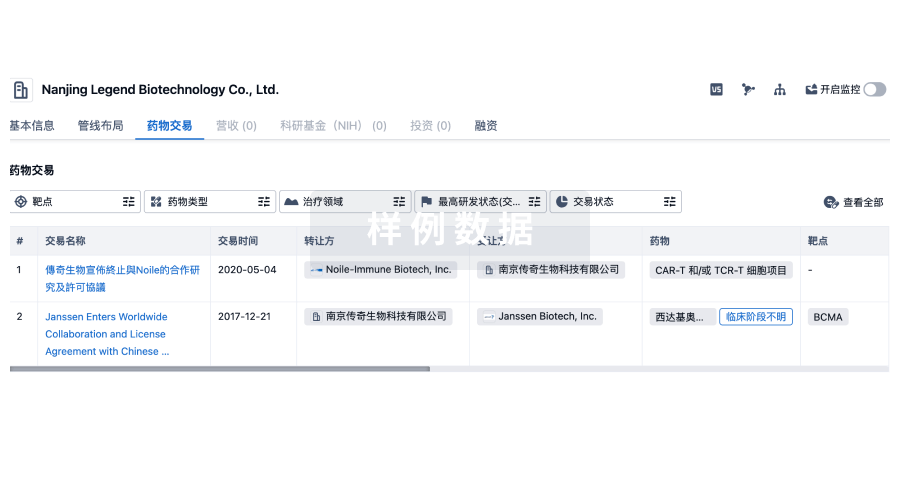
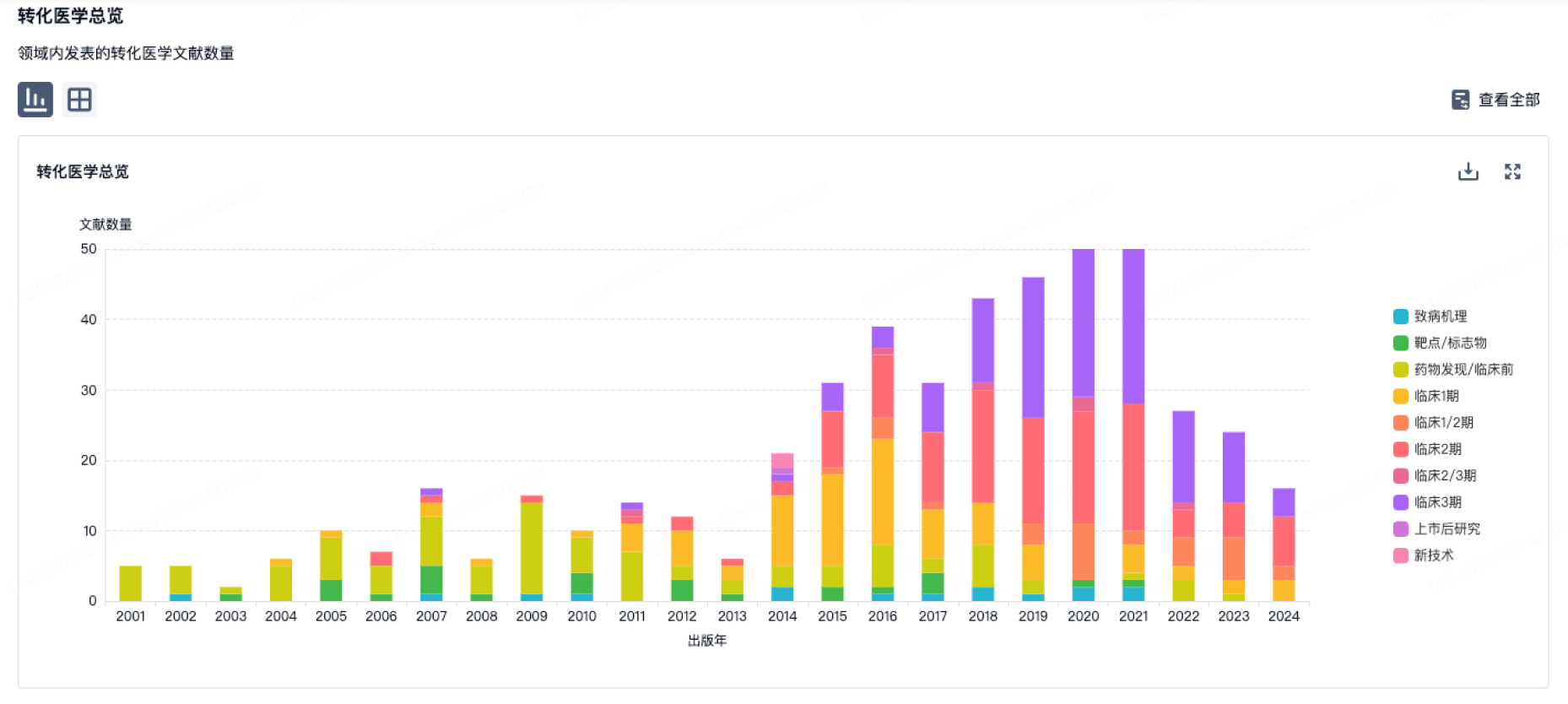
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
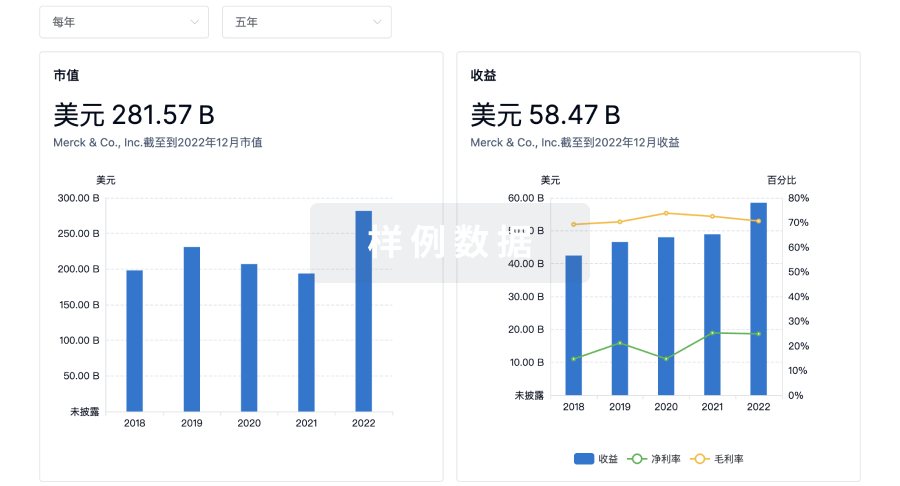
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
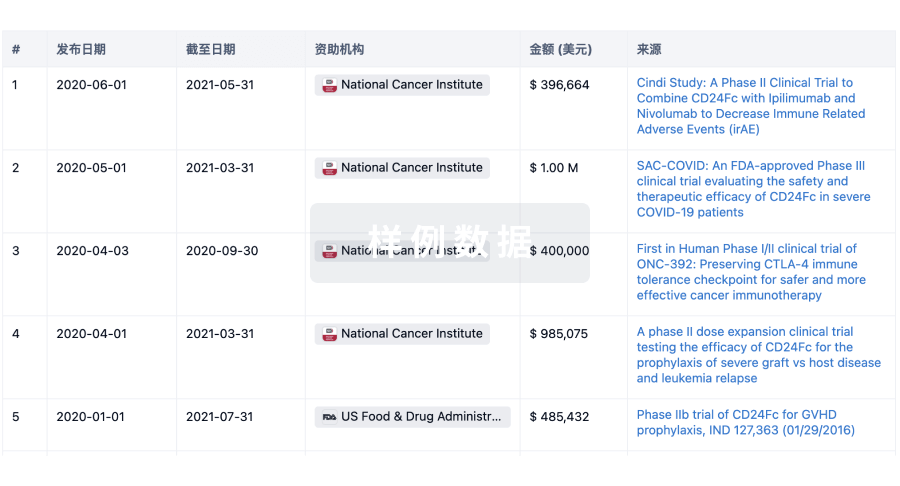
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
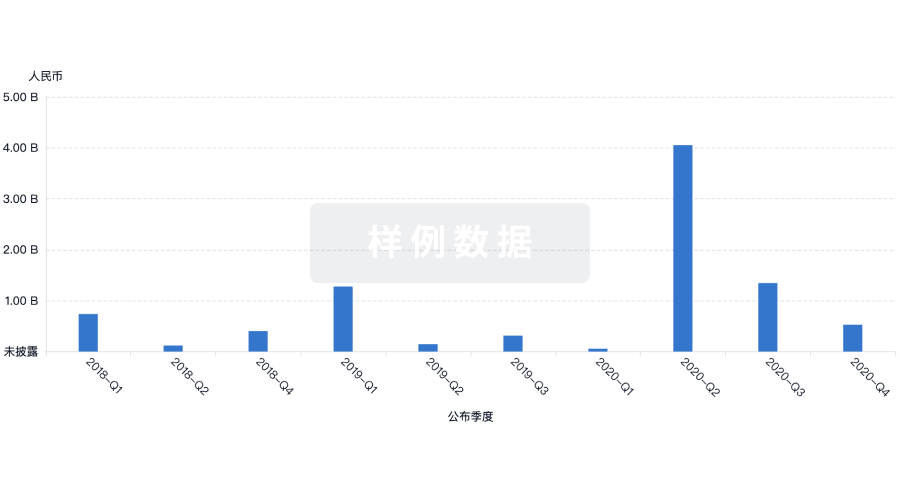
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
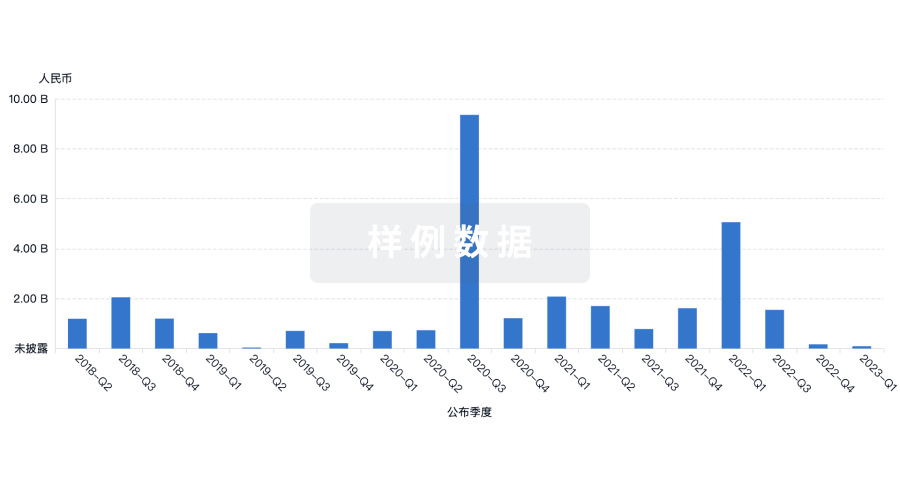
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
标准版
¥16800
元/账号/年
新药情报库 | 省钱又好用!
立即使用
来和芽仔聊天吧
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用