更新于:2024-05-01
Universite De La Mediterranee
教育|
France
教育|
France
更新于:2024-05-01
概览
关联
100 项与 Universite De La Mediterranee 相关的临床结果
登录后查看更多信息
0 项与 Universite De La Mediterranee 相关的专利(医药)
登录后查看更多信息
1,517
项与 Universite De La Mediterranee 相关的文献(医药)2019-07-31·Nature Protocols
Publisher Correction: Patch clamp recording from enteric neurons in situ
作者: Osorio, Nancy ; Delmas, Patrick
In the HTML version of this article published online, the abstract contains a typo in the first sentence: "key to understanding intestinal motility anGutn of therapeutic strategies" should read "key to understanding intestinal motility and crucial to the design of theraputic strategies." The PDF version of the article is correct.
2018-04-30·Theory in Biosciences
Bijective codon transformations show genetic code symmetries centered on cytosine's coding properties
作者: Seligmann, Herve
Homol. of some RNAs with template DNA requires systematic exchanges between nucleotides. Such exchanges produce 'swinger' RNA along 23 bijective transformations (nine sym., X ↔ Y; and 14 asym., X → Y → Z → X, for example A ↔ C and A → C → G → A, resp.). Here, analyses compare amino acids coded by swinger-transformed codons to those coded by untransformed codons, defining coding invariance after transformations. Swinger transformations cluster according to coding invariance in four groups characterized by transformations into cytosine (C = C, T → C, A → C, and G → C). C's central mutational coding role shows that swinger transformations constrained genetic code genesis. Coding invariance post-transformations correlate pos./neg. with mitochondrial swinger transcription/lepidosaurian body temperature Presumably, low/high temperatures stabilize/revert rare swinger polymerization modes, producing long swinger sequences/point mutations, resp. Coding invariance after swinger transformations might compensate effects of swinger polymerizations in species with low body temperatures Hypothetically, swinger transcription increased coding potential of RNA self-replicating protolife systems under heating/cooling cycles.
2017·Allergy (Oxford, United Kingdom)
Lung function parameters in omalizumab responder patients: An interesting tool?
作者: Paganin, F. ; Mangiapan, G. ; Proust, A. ; Prudhomme, A. ; Attia, J. ; Marchand-Adam, S. ; Pellet, F. ; Milhe, F. ; Melloni, B. ; Bernady, A. ; Raspaud, C. ; Nocent, C. ; Berger, P. ; Guilleminault, L.
Background: Omalizumab, an anti-IgE antibody, is used to treat patients with severe allergic asthma. The evolution of lung function parameters over time and the difference between omalizumab responder and nonresponder patients remain inconclusive. The objective of this real-life study was to compare the changes in forced expiratory volume in 1 s (FEV1) of omalizumab responders and nonresponders at 6 mo. Methods: A multicenter anal. was performed in 10 secondary and tertiary institutions. Lung function parameters (forced vital capacity (FVC), pre- and postbronchodilator FEV1, residual volume (RV), and total lung capacity (TLC)) were determined at baseline and at 6 mo. Omalizumab response was assessed at the 6-mo visit. In the omalizumab responder patients, lung function parameters were also obtained at 12, 18, and 24 mo. Results: Mean prebronchodilator FEV1 showed improvement in responders at 6 mo, while a decrease was observed in nonresponders (+0.2±0.4 L and -0.1±0.4 L, resp., P<.01). After an improvement at 6 mo, pre- and postbronchodilator FEV1 remained stable at 12, 18, and 24 mo. The FEV1/FVC remained unchanged over time, but the proportion of patients with an FEV1/FVC ratio <0.7 decreased at 6, 12, 18, and 24 mo (55.2%, 54.0%, 54.0%, and 44.8%, resp., P<.05). Mean RV values decreased at 6 mo but increased at 12 mo and 24 mo (P<.05). Residual volume/total lung capacity (RV/TLC) ratio decreased at 6 mo and remained unchanged at 24 mo. Conclusion: After omalizumab initiation, FEV1 improved at 6 mo in responder patients and then remained stable for 2 years. RV and RV/TLC improved at 6 mo.
100 项与 Universite De La Mediterranee 相关的药物交易
登录后查看更多信息
100 项与 Universite De La Mediterranee 相关的转化医学
登录后查看更多信息
组织架构
使用我们的机构树数据加速您的研究。
登录
或

管线布局
2024年07月08日管线快照
无数据报导
登录后保持更新
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
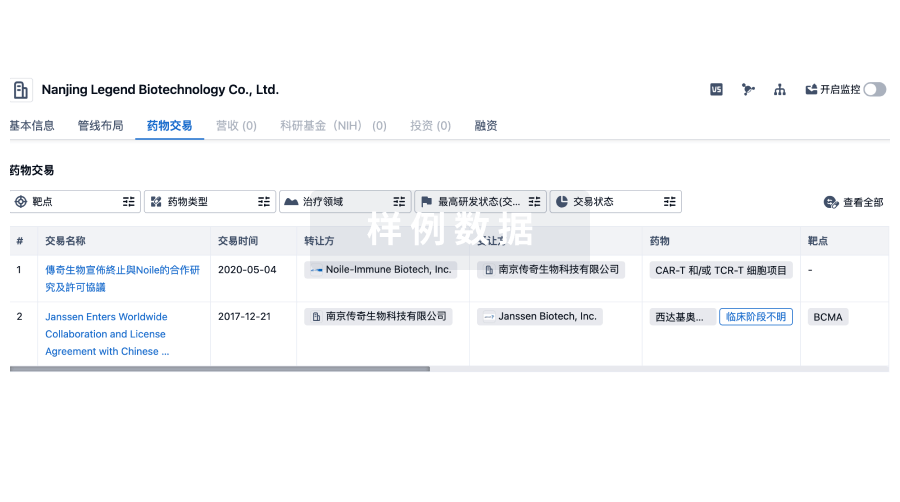
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
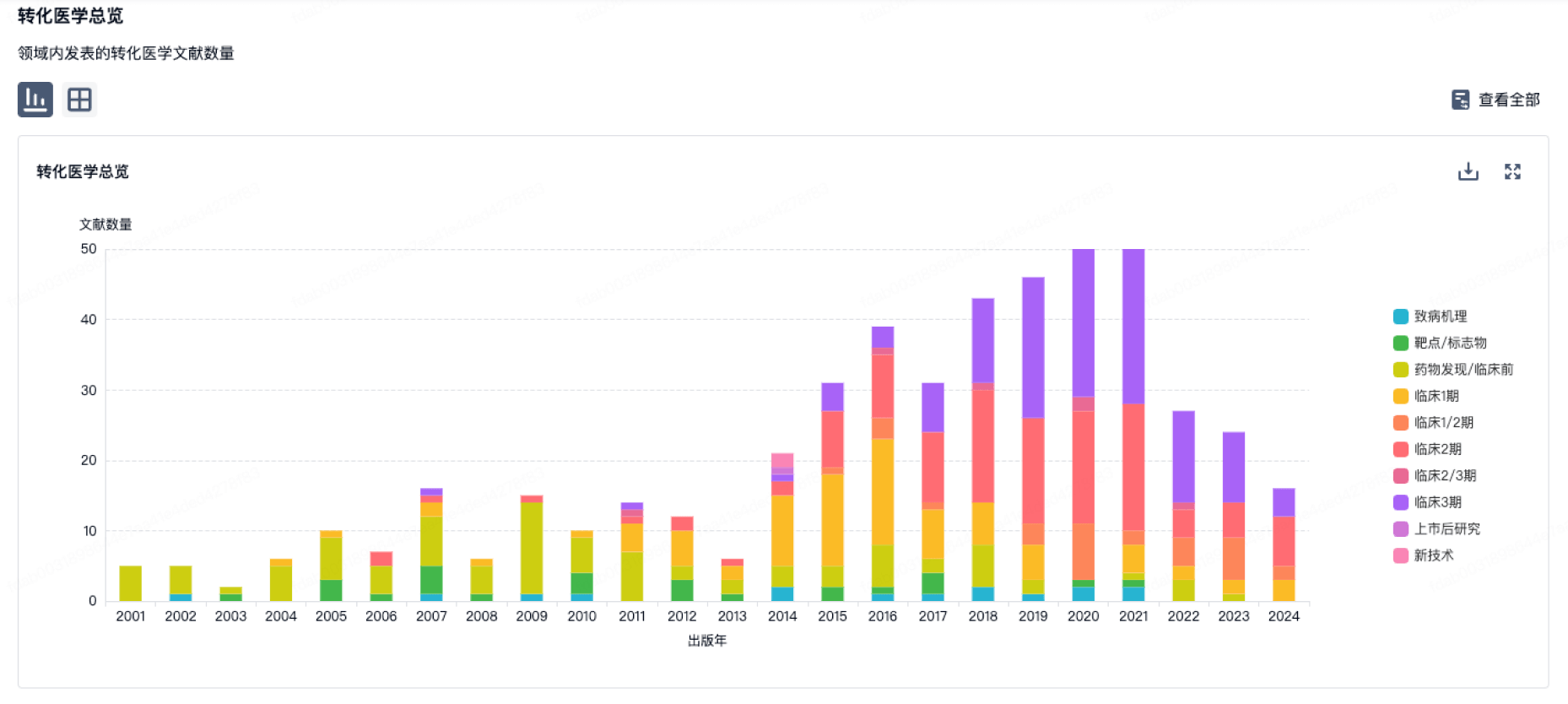
营收
使用 Synapse 探索超过 36 万个组织的财务状况。
登录
或
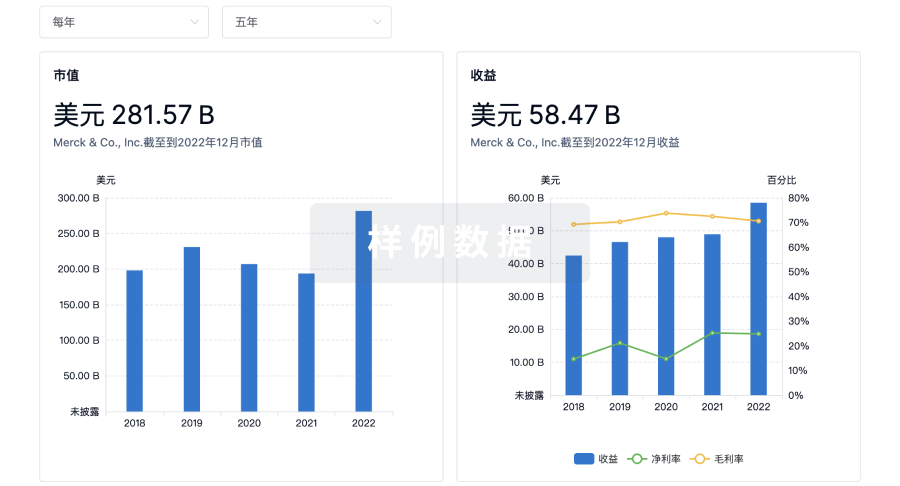
科研基金(NIH)
访问超过 200 万项资助和基金信息,以提升您的研究之旅。
登录
或
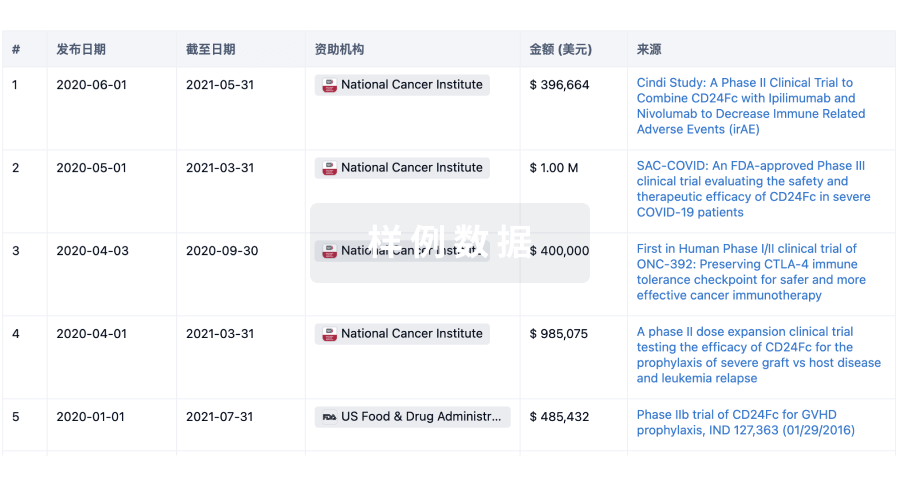
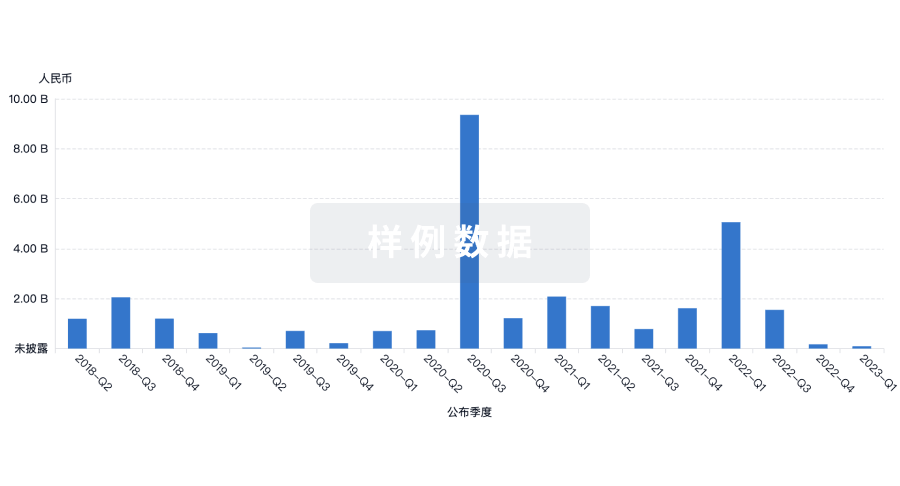
投资
深入了解从初创企业到成熟企业的最新公司投资动态。
登录
或
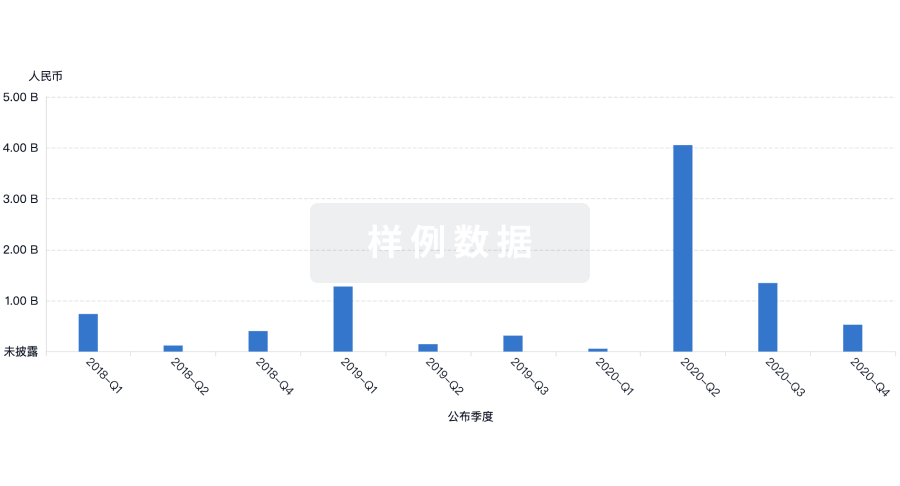
融资
发掘融资趋势以验证和推进您的投资机会。
登录
或
标准版
¥16800
元/账号/年
新药情报库 | 省钱又好用!
立即使用
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用