预约演示
更新于:2025-03-20
MULTIPLE SCLEROSIS(Froceth)
更新于:2025-03-20
概要
基本信息
关联
100 项与 MULTIPLE SCLEROSIS(Froceth) 相关的临床结果
登录后查看更多信息
100 项与 MULTIPLE SCLEROSIS(Froceth) 相关的转化医学
登录后查看更多信息
100 项与 MULTIPLE SCLEROSIS(Froceth) 相关的专利(医药)
登录后查看更多信息
16
项与 MULTIPLE SCLEROSIS(Froceth) 相关的文献(医药)2023-09-01·eBioMedicine
Plasma proteomic profiling identifies CD33 as a marker of HIV control in natural infection and after therapeutic vaccination
Article
作者: Llano, Anuska ; Mothe, Beatriz ; Martinez-Picado, Javier ; Clotet, Bonaventura ; Prats, Anna ; Oriol-Tordera, Bruna ; Ruiz-Riol, Marta ; Brander, Christian ; Hanke, Thomas ; Duran-Castells, Clara ; Garcia-Vidal, Edurne ; Galvez, Cristina ; Muñoz-Moreno, Jose A ; Moltó, José ; Ballana, Ester
2023-07-20·Briefings in bioinformatics
IEPAPI: a method for immune epitope prediction by incorporating antigen presentation and immunogenicity.
Article
作者: Tian, Junzhang ; Zhang, Pengyan ; Zhou, Xiao ; Liu, Min ; Deng, Juntao ; Cheng, Weibin
2021-06-01·Computational Biology and Chemistry4区 · 生物学
Evaluation of potential MHC-I allele-specific epitopes in Zika virus proteins and the effects of mutations on peptide-MHC-I interaction studied using in silico approaches
4区 · 生物学
Article
作者: Bello, Murilo Lamim ; da Costa, Aline Silva ; de Souza, Theo Luiz Ferraz ; Fernandes, Tácio Vinício Amorim
100 项与 MULTIPLE SCLEROSIS(Froceth) 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 多发性硬化症 | 临床前 | 立陶宛 | 2024-08-26 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
No Data | |||||||
登录后查看更多信息
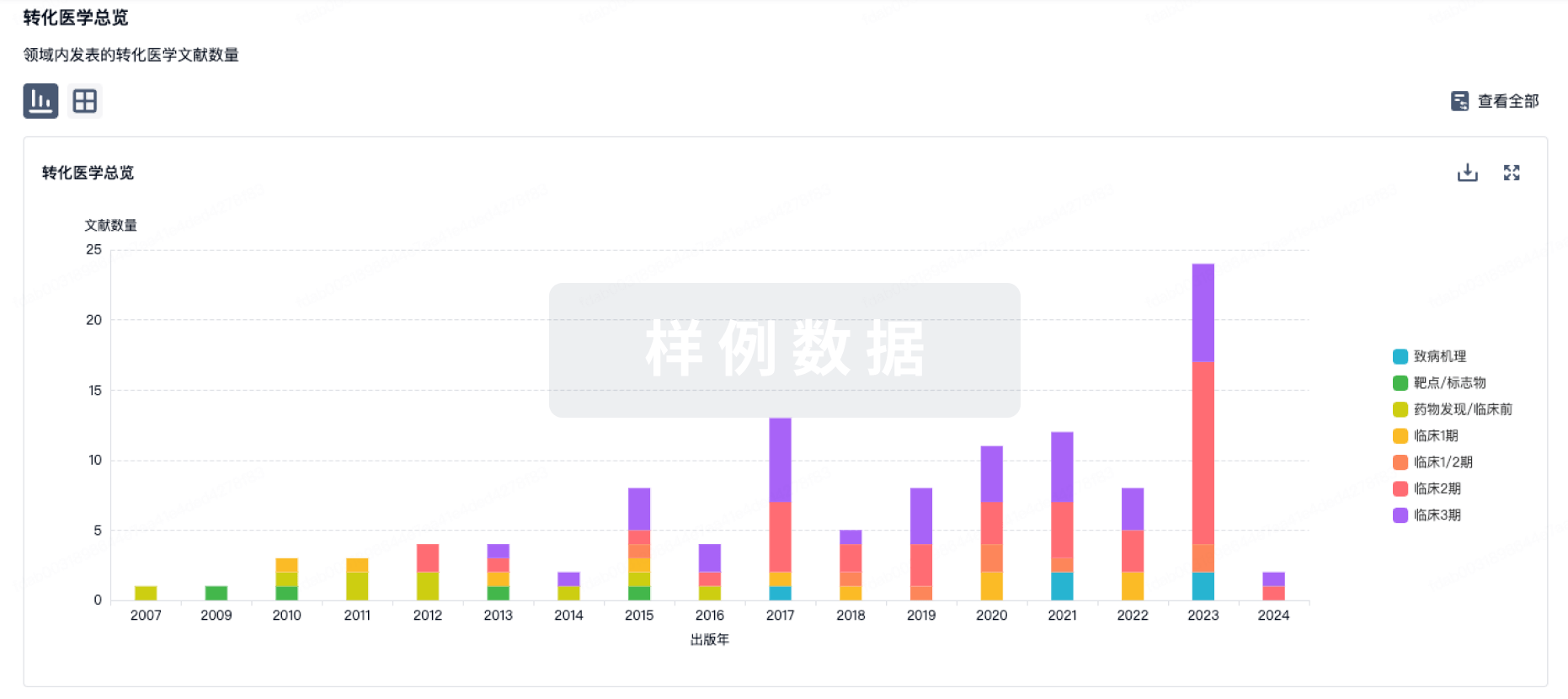
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
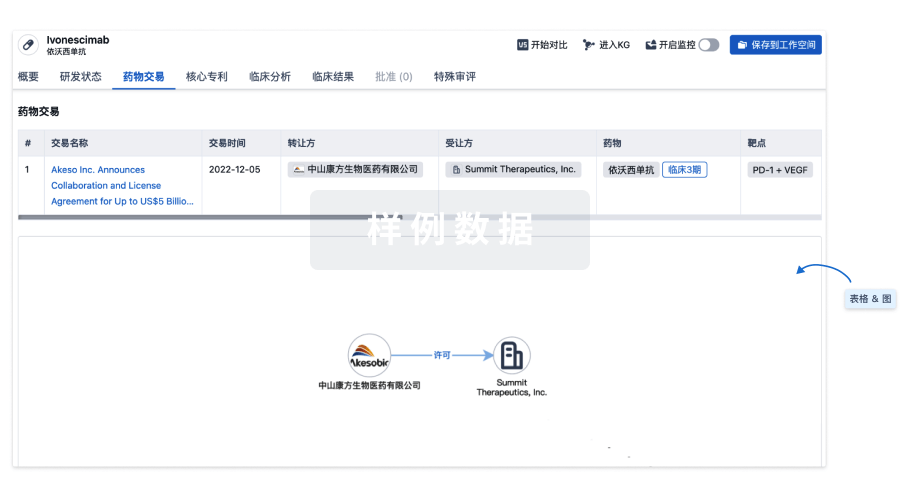
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
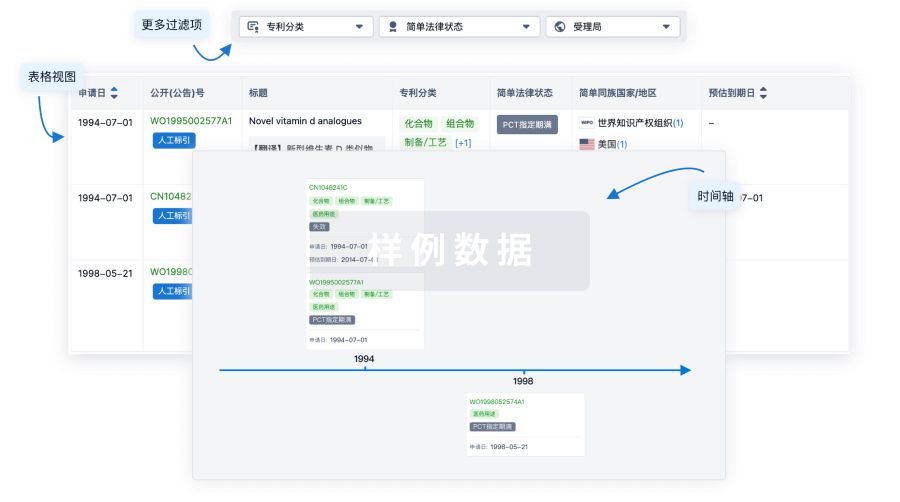
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
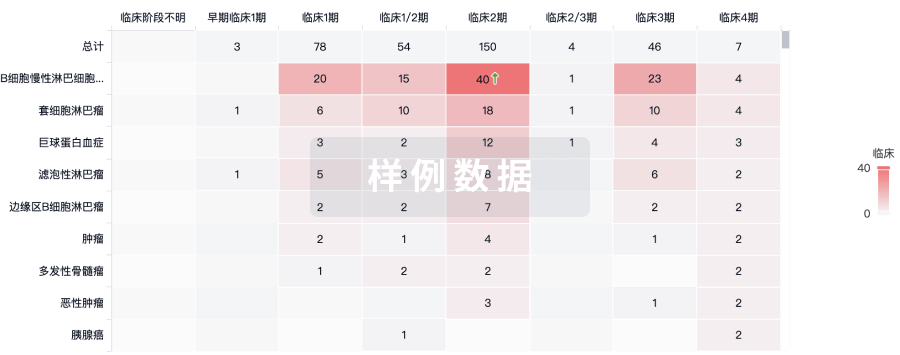
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
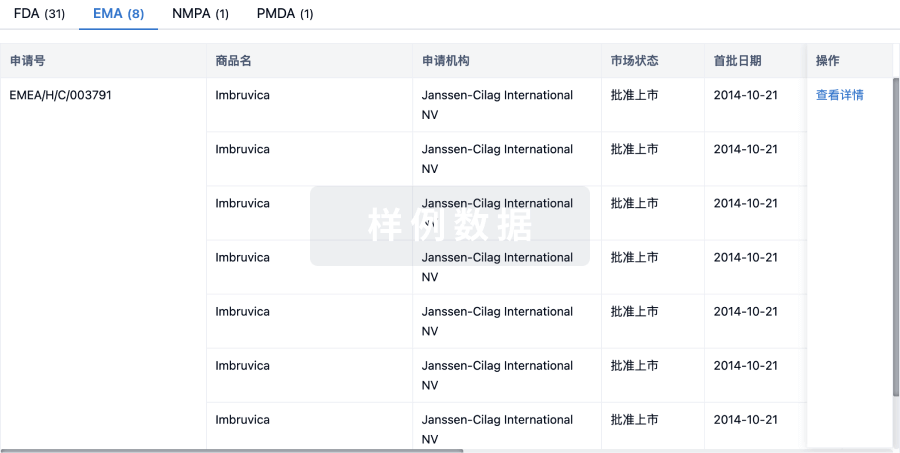
批准
利用最新的监管批准信息加速您的研究。
登录
或
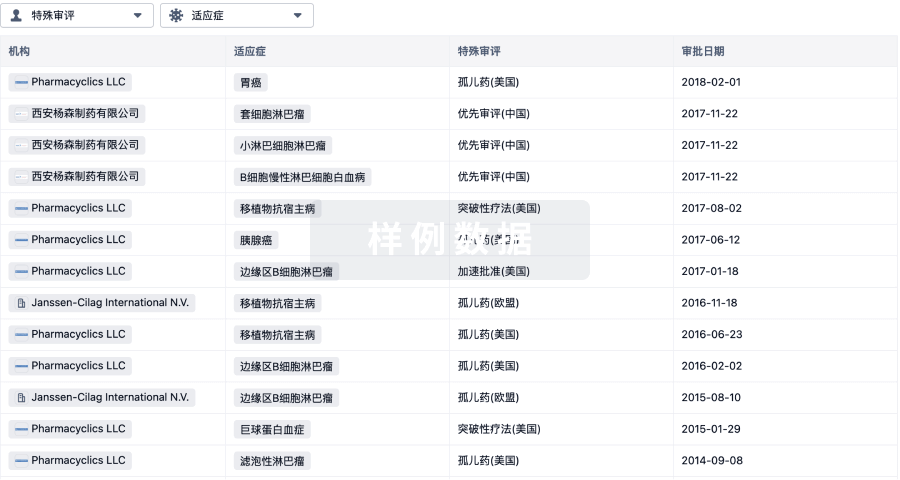
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
来和芽仔聊天吧
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
