预约演示
更新于:2025-05-20
ATYR-0101
更新于:2025-05-20
概要
基本信息
非在研机构- |
权益机构- |
最高研发阶段临床前 |
首次获批日期- |
最高研发阶段(中国)- |
特殊审评- |
关联
100 项与 ATYR-0101 相关的临床结果
登录后查看更多信息
100 项与 ATYR-0101 相关的转化医学
登录后查看更多信息
100 项与 ATYR-0101 相关的专利(医药)
登录后查看更多信息
13
项与 ATYR-0101 相关的文献(医药)2025-06-01·PROTEINS-STRUCTURE FUNCTION AND BIOINFORMATICS
Unraveling the Molecular Architecture of Mosquito D1 ‐Like Dopamine Receptors: Insights Into Ligand Binding and Structural Dynamics for Insecticide Development
Article
作者: Bhaumik, Prasenjit ; Dasgupta, Subrata
ABSTRACT:
Vector‐borne diseases pose a severe threat to human life, contributing significantly to global mortality. Understanding the structure–function relationship of the vector proteins is pivotal for effective insecticide development due to their involvement in drug resistance and disease transmission. This study reports the structural and dynamic features of D1‐like dopamine receptors (DARs) in disease‐causing mosquito species, such as Aedes aegypti, Culex quinquefasciatus, Anopheles gambiae, and Anopheles stephensi. Through molecular modeling and simulations, we describe the common structural fold of mosquito DARs within the G‐protein–coupled receptor family, highlighting the importance of an orthosteric and enlarged binding pocket. The orthosteric binding pocket, resembling a cage‐like structure, is situated ~15 Å deep within the protein, with two serine residues forming the roof and an aspartate residue, along with two conserved water molecules (W1 and W2), forming the floor. The side walls are composed of two phenylalanine residues on one side and a valine residue on the other. The antagonist binding site, an enlarged binding pocket (EBP) near the entrance cavity, can accommodate ligands of varying sizes. The binding energy of dopamine is observed to be ~2–3 kcal/mol higher than that of the antagonist molecules amitriptyline, asenapine, and flupenthixol in mosquito DARs. These antagonist molecules bind to EBP, which obstructs dopamine movement toward the active site, thereby inhibiting signal transduction. Our findings elucidate the molecular architecture of the binding pockets and the versatility of DARs in accommodating diverse ligands, providing a foundational framework for future drug and insecticide development.
2025-02-01·DYSPHAGIA
Association between Swallowing Outcomes and Dose to Critical Swallow Structures in Patients Undergoing Transoral Robotic Surgery and Post-Operative Radiation Therapy
Article
作者: Milross, Chris ; Clark, Jonathan R ; Lawless, Anna ; Wu, Raymond ; Charters, Emma ; Heller, Gillian ; Britton, Rafe ; McCabe, Natalie
Abstract:
Background:
The radiation dose to dysphagia and aspiration-related structures (DARS) for patients undergoing transoral robotic surgery (TORS) and post-operative radiation therapy (PORT) for primary oropharyngeal carcinoma is unknown.
Methods:
This prospective study measured swallowing using the MD Anderson Dysphagia Inventory at baseline and then 12-months after PORT. Dosimetric parameters were collected.
Results:
19 patients were recruited between 2017 and 2019. Worse swallow function at 12-months after PORT was associated with dose-parameters to the oesophageal inlet muscle, superior pharyngeal constrictor muscle and cervical oesophagus. Mean dose, V50Gy, and V60Gy to the base of tongue and pharyngeal constrictors was significantly lower in those receiving PORT to the neck alone.
Conclusion:
Dose to DARS was lower in patients who received PORT to the neck alone. In patients treated with TORS and PORT, poorer swallowing outcomes at 12 months post-treatment were associated with increased dose to oesophageal inlet muscle, superior constrictor muscle, and cervical oesophagus.
2024-04-14·Cureus Journal of Medical Science
Impact of Radiation on Dysphagia-Related Structures: A Dosimetric and Clinical Comparative Analysis of Three-Dimensional Conformal Radiotherapy (3D-CRT) and Intensity-Modulated Radiation Therapy (IMRT) Techniques in Patients With Head and Neck Cancer
Article
作者: Manam, Surendra ; Azharuddin, S K ; Teja, Ravi ; Pb, Anand Rao
Introduction Head and neck squamous cell carcinoma (HNSCC) is a significant health concern in India, with around one million new cases annually. The prevalence of HNSCC is notably high in Asia, especially in India, due to habits like tobacco chewing, betel nut usage, and alcohol consumption. Treatment typically involves a combination of surgery, radiation, chemotherapy, and biological therapy, aiming for tumor control while preserving function and quality of life. However, survivors often face long-term side effects like difficulty swallowing, leading to complications such as aspiration pneumonia. Intensity-modulated radiotherapy (IMRT) has shown promise in improving outcomes by sparing critical swallowing structures. Efforts to minimize radiation-related dysphagia are crucial for enhancing patients' quality of life post-treatment. Our study focuses on examining dosimetric parameters associated with dysphagia aspiration, alongside evaluating dysphagia grades in both treatment groups using the RTOG scale. Material and methods Patients with histologically confirmed non-metastatic head and neck carcinomas were included in our study in November 2018-April 2020. A total of 56 patients were taken into our study with 28 in each arm. They underwent radical radiotherapy (RT) with a total dose of 66-70 Gy, with or without concurrent chemotherapy, meeting specific inclusion criteria and excluding those receiving reirradiation or with distant metastasis. Patients were divided into two groups: Group I received three-dimensional conformal radiotherapy (3D-CRT), and Group II received IMRT. Treatment planning involved immobilization, CT imaging, delineation of target volumes and organs at risk, and contouring of swallowing structures. Dose-volume histogram parameters (mean dose, maximum dose, V30, V70, V80, D50, and D80) were used to assess mean dose to swallowing structures outside the planning target volume (PTV), with a mean dose constraint of 50 Gy. Dysphagia was evaluated using the RTOG criteria at baseline, during treatment, and six months post-treatment. Statistical analysis was performed using SPSS, with significance set at p < 0.05. Results In our study, the mean age at presentation differed slightly between the IMRT and 3D-CRT arms: 58 years versus 55 years, respectively. A higher proportion of patients in both arms experienced symptoms for three to six months, with 53.6% in 3D-CRT and 42.9% in IMRT. Stage distribution varied, with IV being most common in 3D-CRT and stage II in IMRT. Approximately 56% of patients in both groups had a history of smoking. Significant differences were observed in spinal cord dose between 3DCRT and IMRT techniques (p < 0.001). Similarly, a significant difference was found in the mean dose received by dysphagia aspiration-related structures (DARSs) between the 3D-CRT and IMRT arms (p = 0.04). Patients in the IMRT arm exhibited superior dysphagia grades compared to those in the 3D-CRT arm, with statistical significance observed in the third month (p = 0.008) and sixth month (p = 0.048). Conclusion Our study found a notable decrease in the mean DARS dose and reduced dysphagia severity at three and six months in the IMRT group compared to the 3D-CRT group. However, due to the diverse study population, establishing a definitive correlation between the DARS dose and dysphagia severity was challenging. Future large-scale studies are needed to validate these findings for improved preservation of DARS structures.
6
项与 ATYR-0101 相关的新闻(医药)2025-05-16
Preclinical data demonstrate ATYR0101’s unique anti-fibrotic mechanism through interaction with LTBP-1.
ATYR0101 to be showcased in oral presentation at the American Thoracic Society (ATS) 2025 Respiratory Innovation Summit.
SAN DIEGO, CA, USA I May 14, 2025 I
aTyr Pharma, Inc. (Nasdaq: ATYR) (“aTyr” or the “Company”), a clinical stage biotechnology company engaged in the discovery and development of first-in-class medicines from its proprietary tRNA synthetase platform, today announced that it has advanced its next investigational new drug (IND) candidate, ATYR0101, which has been selected to be showcased in an oral presentation at the American Thoracic Society (ATS) 2025 Respiratory Innovation Summit, which is scheduled to take place May 16 – 17, 2025, in San Francisco, CA.
The presentation will feature preclinical data generated to date for ATYR0101, a fusion protein derived from a proprietary extracellular domain of aspartyl-tRNA synthetase (DARS) that binds to latent transforming growth factor beta binding protein 1 (LTBP-1) to induce cell death of myofibroblasts, which are key cells responsible for driving the progression of fibrosis.
“Fibrosis is a key driver of morbidity and mortality in many diseases, particularly those affecting the lung, where evasion of myofibroblast cell death is a defining feature,” said Leslie A. Nangle, Ph.D., Vice President, Research, at aTyr. “The unique effects observed with ATYR0101 in preclinical models of fibrosis suggest it may have the potential to reverse fibrosis, which could represent a meaningful advancement in the approach to treating pulmonary fibrosis, where current treatments only slow disease progression.”
President and Chief Executive Officer of aTyr, Sanjay S. Shukla, M.D., M.S., added, “Building on the promising clinical results of our lead tRNA synthetase-derived therapy, efzofitimod, in interstitial lung disease, we’re excited to advance ATYR0101 into IND-enabling studies. This next candidate from our pipeline exemplifies the transformative potential of our innovative drug discovery platform and highlights our unwavering commitment to pioneering therapies for inflammatory and fibrotic diseases. We look forward to further exploring this candidate in pulmonary fibrosis and anticipate filing an IND application in the second half of 2026.”
Details of the presentation appear below. The presentation will be available on the aTyr website once presented.
Title:
ATYR0101: A New Approach to Fibrosis
Presenter:
Ryan Adams, Ph.D., Senior Director, In Vitro Biology
Session:
Showcase Three: ILD/Fibrosis
Date and Time:
Saturday, May 17, 2025 at 11:30 AM PT
Location:
San Francisco Marriott Marquis, San Francisco, CA
About ATYR0101
ATYR0101 is a fusion protein derived from a proprietary extracellular domain of aspartyl-tRNA synthetase (DARS) that binds to latent transforming growth factor beta binding protein 1 (LTBP-1) to induce myofibroblast apoptosis. ATYR0101 interacts with LTBP-1 through a unique way that presents a differentiated approach to targeting fibrosis. ATYR0101 has demonstrated anti-fibrotic effects in models of lung and kidney fibrosis suggesting it may have broad therapeutic potential in multiple fibrotic diseases. ATYR0101 is currently undergoing IND-enabling studies.
About aTyr
aTyr is a clinical stage biotechnology company leveraging evolutionary intelligence to translate tRNA synthetase biology into new therapies for fibrosis and inflammation. tRNA synthetases are ancient, essential proteins that have evolved novel domains that regulate diverse pathways extracellularly in humans. aTyr’s discovery platform is focused on unlocking hidden therapeutic intervention points by uncovering signaling pathways driven by its proprietary library of domains derived from all 20 tRNA synthetases. aTyr’s lead therapeutic candidate is efzofitimod, a first-in-class biologic immunomodulator in clinical development for the treatment of interstitial lung disease, a group of immune-mediated disorders that can cause inflammation and progressive fibrosis, or scarring, of the lungs. For more information, please visit
www.atyrpharma.com
.
SOURCE: aTyr
临床研究免疫疗法
2025-05-14
Preclinical data demonstrate ATYR0101’s unique anti-fibrotic mechanism through interaction with LTBP-1.
ATYR0101 to be showcased in oral presentation at the American Thoracic Society (ATS) 2025 Respiratory Innovation Summit.
SAN DIEGO, May 14, 2025 (GLOBE NEWSWIRE) -- aTyr Pharma, Inc. (Nasdaq: ATYR) (“aTyr” or the “Company”), a clinical stage biotechnology company engaged in the discovery and development of first-in-class medicines from its proprietary tRNA synthetase platform, today announced that it has advanced its next investigational new drug (IND) candidate, ATYR0101, which has been selected to be showcased in an oral presentation at the American Thoracic Society (ATS) 2025 Respiratory Innovation Summit, which is scheduled to take place May 16 – 17, 2025, in San Francisco, CA.
The presentation will feature preclinical data generated to date for ATYR0101, a fusion protein derived from a proprietary extracellular domain of aspartyl-tRNA synthetase (DARS) that binds to latent transforming growth factor beta binding protein 1 (LTBP-1) to induce cell death of myofibroblasts, which are key cells responsible for driving the progression of fibrosis.
“Fibrosis is a key driver of morbidity and mortality in many diseases, particularly those affecting the lung, where evasion of myofibroblast cell death is a defining feature,” said Leslie A. Nangle, Ph.D., Vice President, Research, at aTyr. “The unique effects observed with ATYR0101 in preclinical models of fibrosis suggest it may have the potential to reverse fibrosis, which could represent a meaningful advancement in the approach to treating pulmonary fibrosis, where current treatments only slow disease progression.”
President and Chief Executive Officer of aTyr, Sanjay S. Shukla, M.D., M.S., added, “Building on the promising clinical results of our lead tRNA synthetase-derived therapy, efzofitimod, in interstitial lung disease, we’re excited to advance ATYR0101 into IND-enabling studies. This next candidate from our pipeline exemplifies the transformative potential of our innovative drug discovery platform and highlights our unwavering commitment to pioneering therapies for inflammatory and fibrotic diseases. We look forward to further exploring this candidate in pulmonary fibrosis and anticipate filing an IND application in the second half of 2026.”
Details of the presentation appear below. The presentation will be available on the aTyr website once presented.
Title: ATYR0101: A New Approach to Fibrosis Presenter: Ryan Adams, Ph.D., Senior Director, In Vitro Biology Session: Showcase Three: ILD/Fibrosis Date and Time: Saturday, May 17, 2025 at 11:30 AM PT Location: San Francisco Marriott Marquis, San Francisco, CA
About ATYR0101 ATYR0101 is a fusion protein derived from a proprietary extracellular domain of aspartyl-tRNA synthetase (DARS) that binds to latent transforming growth factor beta binding protein 1 (LTBP-1) to induce myofibroblast apoptosis. ATYR0101 interacts with LTBP-1 through a unique way that presents a differentiated approach to targeting fibrosis. ATYR0101 has demonstrated anti-fibrotic effects in models of lung and kidney fibrosis suggesting it may have broad therapeutic potential in multiple fibrotic diseases. ATYR0101 is currently undergoing IND-enabling studies.
About aTyr aTyr is a clinical stage biotechnology company leveraging evolutionary intelligence to translate tRNA synthetase biology into new therapies for fibrosis and inflammation. tRNA synthetases are ancient, essential proteins that have evolved novel domains that regulate diverse pathways extracellularly in humans. aTyr’s discovery platform is focused on unlocking hidden therapeutic intervention points by uncovering signaling pathways driven by its proprietary library of domains derived from all 20 tRNA synthetases. aTyr’s lead therapeutic candidate is efzofitimod, a first-in-class biologic immunomodulator in clinical development for the treatment of interstitial lung disease, a group of immune-mediated disorders that can cause inflammation and progressive fibrosis, or scarring, of the lungs. For more information, please visit www.atyrpharma.com.
Forward-Looking Statements This press release contains forward-looking statements within the meaning of the Private Securities Litigation Reform Act of 1995. Forward-looking statements are usually identified by the use of words such as "anticipate," “believes,” “could,” “can,” “designed,” “expects,” “intends,” “may,” “plans,” “potential,” “suggest,” “will,” and variations of such words or similar expressions. We intend these forward-looking statements to be covered by such safe harbor provisions for forward-looking statements and are making this statement for purposes of complying with those safe harbor provisions. These forward-looking statements include, among others, statements regarding the development of ATYR0101; the potential therapeutic benefits and applications of ATYR0101; and timelines and plans with respect to certain development activities and development goals, including our expectation of the potential filing of an IND application for ATYR0101 in the second half of 2026. These forward-looking statements also reflect our current views about our plans, intentions, expectations, strategies and prospects, which are based on the information currently available to us and on assumptions we have made. Although we believe that our plans, intentions, expectations, strategies and prospects, as reflected in or suggested by these forward-looking statements, are reasonable, we can give no assurance that the plans, intentions, expectations, strategies or prospects will be attained or achieved. All forward-looking statements are based on estimates and assumptions by our management that, although we believe to be reasonable, are inherently uncertain. Furthermore, actual results may differ materially from those described in these forward-looking statements and will be affected by a variety of risks and factors that are beyond our control including, without limitation, uncertainty regarding geopolitical and macroeconomic events, risks associated with the discovery, development and regulation of ATYR0101 (including the risk that future findings do not support the findings described in the presentation), the risk that we or our partners may cease or delay preclinical development activities for ATYR0101 for a variety of reasons, the possibility that existing collaborations could be terminated early, and the risk that we may not be able to raise the additional funding required for our business and product development plans, as well as those risks set forth in our most recent Annual Report on Form 10-K, Quarterly Reports on Form 10-Q and in our other SEC filings. Except as required by law, we assume no obligation to update publicly any forward-looking statements, whether as a result of new information, future events or otherwise.
Contact: Ashlee Dunston Sr. Director, Investor Relations and Public Affairs adunston@atyrpharma.com
Source: aTyr Pharma, Inc.
临床研究
2025-03-13
Topline data from Phase 3 EFZO-FIT™ study of efzofitimod in pulmonary sarcoidosis expected in the third quarter of 2025.
Fourth positive DSMB review for efzofitimod in Phase 3 EFZO-FIT™ study reinforces its favorable safety profile.
Publication in Science Translational Medicine validates efzofitimod’s mechanism of action.
Company to host conference call and webcast today, March 13th at 5:00 p.m. EDT / 2:00 p.m. PDT.
SAN DIEGO, March 13, 2025 (GLOBE NEWSWIRE) -- aTyr Pharma, Inc. (Nasdaq: ATYR) (“aTyr” or the “Company”), a clinical stage biotechnology company engaged in the discovery and development of first-in-class medicines from its proprietary tRNA synthetase platform, today announced fourth quarter and full year 2024 results and provided a corporate update.
“2024 was an important year for aTyr, as we completed enrollment in our global pivotal Phase 3 EFZO-FIT™ study, which is the largest interventional study ever to be conducted in pulmonary sarcoidosis, a disease where incidence and prevalence are rising yet there are still limited treatment options,” said Sanjay S. Shukla, M.D., M.S., President and Chief Executive Officer of aTyr. “The stage is set for 2025 to be a potential milestone year as we look toward reporting topline data for EFZO-FIT™ in the third quarter. Leading into this pivotal readout, we are very pleased with the execution of the study to date and the continued favorable safety profile demonstrated for efzofitimod, including our most recent positive DSMB review, which recommended the study continue as designed. Efzofitimod is poised to potentially become a safe and effective alternative to the current standard of care and improve patients’ lives.”
Fourth Quarter 2024 and Subsequent Period Highlights
Enrollment complete in the global pivotal Phase 3 EFZO-FIT™ study to evaluate the efficacy and safety of efzofitimod in patients with pulmonary sarcoidosis. This is a randomized, double-blind, placebo-controlled, 52-week study consisting of three parallel cohorts randomized equally to either 3.0 mg/kg or 5.0 mg/kg of efzofitimod or placebo dosed intravenously monthly for a total of 12 doses. The study enrolled 268 patients with pulmonary sarcoidosis at 85 centers in nine countries. The trial design incorporates a forced steroid taper. The primary endpoint of the study is steroid reduction. Secondary endpoints include measures of sarcoidosis symptoms and lung function. Topline data from the study are expected in the third quarter of 2025. Patients who complete the study and wish to receive treatment with efzofitimod outside of the clinical trial are eligible to participate in an Individual Patient Expanded Access Program. Held a Type C meeting with the U.S. Food and Drug Administration (FDA) to discuss the statistical analysis plan (SAP) for the Phase 3 EFZO-FIT™ study. The main objective of the meeting was to finalize the way in which the study endpoints are assessed from a statistical standpoint. Based on FDA feedback, steroid reduction will be measured as the absolute change from baseline to week 48. Announced the fourth positive data and safety monitoring board (DSMB) review for the Phase 3 EFZO-FIT™ study. The independent DSMB recommended that the study continue without modifications based on the pre-planned analysis. Enrollment ongoing in the Phase 2 EFZO-CONNECT™ study to evaluate the efficacy, safety and tolerability of efzofitimod in patients with limited and diffuse systemic sclerosis (SSc, or scleroderma)-related interstitial lung disease (SSc-ILD). This proof-of-concept study is a randomized, double-blind, placebo-controlled, 28-week study consisting of three parallel cohorts randomized 2:2:1 to either 270 mg or 450 mg of efzofitimod or placebo dosed intravenously monthly for a total of six doses. The study intends to enroll up to 25 patients at multiple centers in the United States. Patients who complete the study are eligible to participate in a 24-week open-label extension. Interim data from the study are expected in the second quarter of 2025 and will focus on skin assessments measured at baseline and week 12 in approximately 8 patients, including patients on drug and placebo. The data will include skin histopathology, including immune biomarkers, and the modified Rodnan skin score. Manuscript demonstrating the immunomodulatory activity for efzofitimod in lung inflammation and fibrosis published in the peer-reviewed journal Science Translational Medicine. The publication describes efzofitimod’s unique anti-inflammatory effect on macrophages through neuropiln-2 (NRP2) and details the preclinical data supporting its development. The publication, which is entitled, “A human histidyl-tRNA synthetase splice variant therapeutic targets NRP2 to resolve lung inflammation and fibrosis,” is available on the journal’s website and at: https://www-science-org.libproxy1.nus.edu.sg/doi/10.1126/scitranslmed.adp4754. Posters for efzofitimod accepted for presentation at the upcoming American Thoracic Society (ATS) 2025 International Conference. The conference is scheduled to take place May 16 – 21, 2025, in San Francisco, CA. Poster 9320 – Real-World Treatment Patterns Among Pulmonary Sarcoidosis Patients with Parenchymal Involvement in the US on Sunday May 18, 2025, at 11:30 a.m. PDT. Poster 6808 – EFZO-FIT, Largest Placebo-Controlled Trial in Pulmonary Sarcoidosis – Trial Design and Patient Characteristics on Monday, May 19, 2025, at 11:30 a.m. PDT. Poster 9092 – Incidence, Prevalence, and Mortality of Pulmonary Sarcoidosis with Parenchymal Involvement in the US on Tuesday May 20, 2025, at 11:30 a.m. PDT. Presented preclinical research demonstrating anti-fibrotic effects of ATYR0101 in lung and kidney fibrosis in two posters at the Keystone Symposia on Fibrosis: Inflammation, Drivers, and Therapeutic Resolution. The findings demonstrated that ATYR0101 interacts with LTBP-1 to induce myofibroblast apoptosis through a novel anti-fibrotic mechanism and suggest that ATYR0101 has the potential to be a next generation anti-fibrotic drug for lung and kidney fibrosis. Appointed Eric Benevich to the Company’s Board of Directors. Mr. Benevich currently serves as Chief Commercial Officer at Neurocrine Biosciences, Inc., where he is responsible for all aspects of commercial development, marketing, and sales of the Neurocrine product portfolio.
Poster 9320 – Real-World Treatment Patterns Among Pulmonary Sarcoidosis Patients with Parenchymal Involvement in the US on Sunday May 18, 2025, at 11:30 a.m. PDT. Poster 6808 – EFZO-FIT, Largest Placebo-Controlled Trial in Pulmonary Sarcoidosis – Trial Design and Patient Characteristics on Monday, May 19, 2025, at 11:30 a.m. PDT. Poster 9092 – Incidence, Prevalence, and Mortality of Pulmonary Sarcoidosis with Parenchymal Involvement in the US on Tuesday May 20, 2025, at 11:30 a.m. PDT.
Year Ended 2024 Financial Highlights and Cash Position
Cash & Investment Position: Cash, cash equivalents, restricted cash and available-for-sale investments as of December 31, 2024, were $75.1 million. Subsequent to the end of the fourth quarter 2024, the Company raised approximately $18.8 million in gross proceeds from its at-the-market (ATM) offering with Jefferies LLC. Financial Guidance: The Company updated its prior guidance and believes its cash runway will be sufficient to fund its operations for a period of one year following the Phase 3 EFZO-FIT™ readout, which includes the potential filing of a Biologics License Application (BLA) for efzofitimod in pulmonary sarcoidosis. R&D Expenses: Research and development expenses were $54.4 million for the year ended 2024, which consisted primarily of clinical trial costs for the Phase 3 EFZO-FIT™ and Phase 2 EFZO-CONNECT™ studies, manufacturing costs for the efzofitimod program and research and development costs for the efzofitimod and discovery programs. G&A Expenses: General and administrative expenses were $13.8 million for the year ended 2024. Collaboration and License Revenue: Collaboration and license revenue related to the Kyorin Agreement was $0.2 million for the year ended 2024, which consisted of drug product material sold to Kyorin for the Japan portion of the EFZO-FIT™ study.
Conference Call and Webcast Details
aTyr will host a conference call and webcast today at 5:00 p.m. EDT / 2:00 p.m. PDT to discuss its financial results and provide a corporate update. Interested parties may access the call by registering here in order to obtain a dial in, personalized passcode and webcast information. Links to a live audio webcast and replay may be accessed on the aTyr website Events page at: https://investors.atyrpharma.com/events-and-webcasts. An audio replay will be available for at least 90 days following the event.
About Efzofitimod
Efzofitimod is a first-in-class biologic immunomodulator in clinical development for the treatment of interstitial lung disease (ILD), a group of immune-mediated disorders that can cause inflammation and fibrosis, or scarring, of the lungs. Efzofitimod is a tRNA synthetase derived therapy that selectively modulates activated myeloid cells through neuropilin-2 to resolve inflammation without immune suppression and potentially prevent the progression of fibrosis. aTyr is currently investigating efzofitimod in the global Phase 3 EFZO-FIT™ study in patients with pulmonary sarcoidosis, a major form of ILD, and in the Phase 2 EFZO-CONNECT™ study in patients with systemic sclerosis (SSc, or scleroderma)-related ILD. These forms of ILD have limited therapeutic options and there is a need for safer and more effective, disease-modifying treatments that improve outcomes.
About aTyr
aTyr is a clinical stage biotechnology company leveraging evolutionary intelligence to translate tRNA synthetase biology into new therapies for fibrosis and inflammation. tRNA synthetases are ancient, essential proteins that have evolved novel domains that regulate diverse pathways extracellularly in humans. aTyr’s discovery platform is focused on unlocking hidden therapeutic intervention points by uncovering signaling pathways driven by its proprietary library of domains derived from all 20 tRNA synthetases. aTyr’s lead therapeutic candidate is efzofitimod, a first-in-class biologic immunomodulator in clinical development for the treatment of interstitial lung disease, a group of immune-mediated disorders that can cause inflammation and progressive fibrosis, or scarring, of the lungs. For more information, please visit www.atyrpharma.com.
Forward-Looking Statements
This press release contains forward-looking statements within the meaning of the Private Securities Litigation Reform Act of 1995. Forward-looking statements are usually identified by the use of words such as “aims” “anticipates,” “believes,” “can,” “designed,” “expects,” “intends,” “look toward,” “may,” “plans,” “potential,” “project,” “will,” and variations of such words or similar expressions. We intend these forward-looking statements to be covered by such safe harbor provisions for forward-looking statements and are making this statement for purposes of complying with those safe harbor provisions. These forward-looking statements include, among others, statements regarding interactions with the FDA relating to the SAP for the Phase 3 EFZO-FIT™ study, including the measurement of steroid reduction; the expected size of, and number of patients to be enrolled in, the EFZO-CONNECT™ study; the skin assessments and expected number of patients to be included in the interim data for the EFZO-CONNECT™ study; the potential therapeutic benefits and applications of efzofitimod; expectations regarding our financial guidance and the sufficiency of our cash runway; and timelines and plans with respect to certain development activities and development goals, including the potential filing of a BLA for efzofitimod in pulmonary sarcoidosis and our expectation that our Phase 3 EFZO-FIT™ study of efzofitimod in patients with pulmonary sarcoidosis will report topline data in the third quarter of 2025 and expectation that our Phase 2 EFZO-CONNECT™ study will report interim data in the second quarter of 2025. These forward-looking statements also reflect our current views about our plans, intentions, expectations, strategies and prospects, which are based on the information currently available to us and on assumptions we have made. Although we believe that our plans, intentions, expectations, strategies and prospects, as reflected in or suggested by these forward-looking statements, are reasonable, we can give no assurance that the plans, intentions, expectations, strategies or prospects will be attained or achieved. All forward-looking statements are based on estimates and assumptions by our management that, although we believe to be reasonable, are inherently uncertain. Furthermore, actual results may differ materially from those described in these forward-looking statements and will be affected by a variety of risks and factors that are beyond our control including, without limitation, risks related to our reliance on third-party partners and the potential that such partners may not perform as anticipated, the fact that NRP2 and tRNA synthetase biology is not fully understood, uncertainty regarding the ultimate long-term impact of evolving macroeconomic and geopolitical conditions, the risk of delays in our clinical trials, risks associated with the discovery, development and regulation of our product candidates, including the uncertainty of related costs and regulatory filings and the risk that results from clinical trials or other studies may not support further development, the risk that we may cease or delay preclinical or clinical development activities for any of our existing or future product candidates for a variety of reasons, the fact that our collaboration agreements are subject to early termination, and the risk that we may not be able to raise the additional funding required for our business and product development plans, as well as those risks set forth in our most recent Annual Report on Form 10-K, Quarterly Reports on form 10-Q and in our other SEC filings. Except as required by law, we assume no obligation to update publicly any forward-looking statements, whether as a result of new information, future events or otherwise.
Source: aTyr Pharma, Inc.
临床3期临床2期临床结果高管变更财报
100 项与 ATYR-0101 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 纤维化 | 临床前 | 美国 | 2024-04-17 |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
No Data | |||||||
登录后查看更多信息
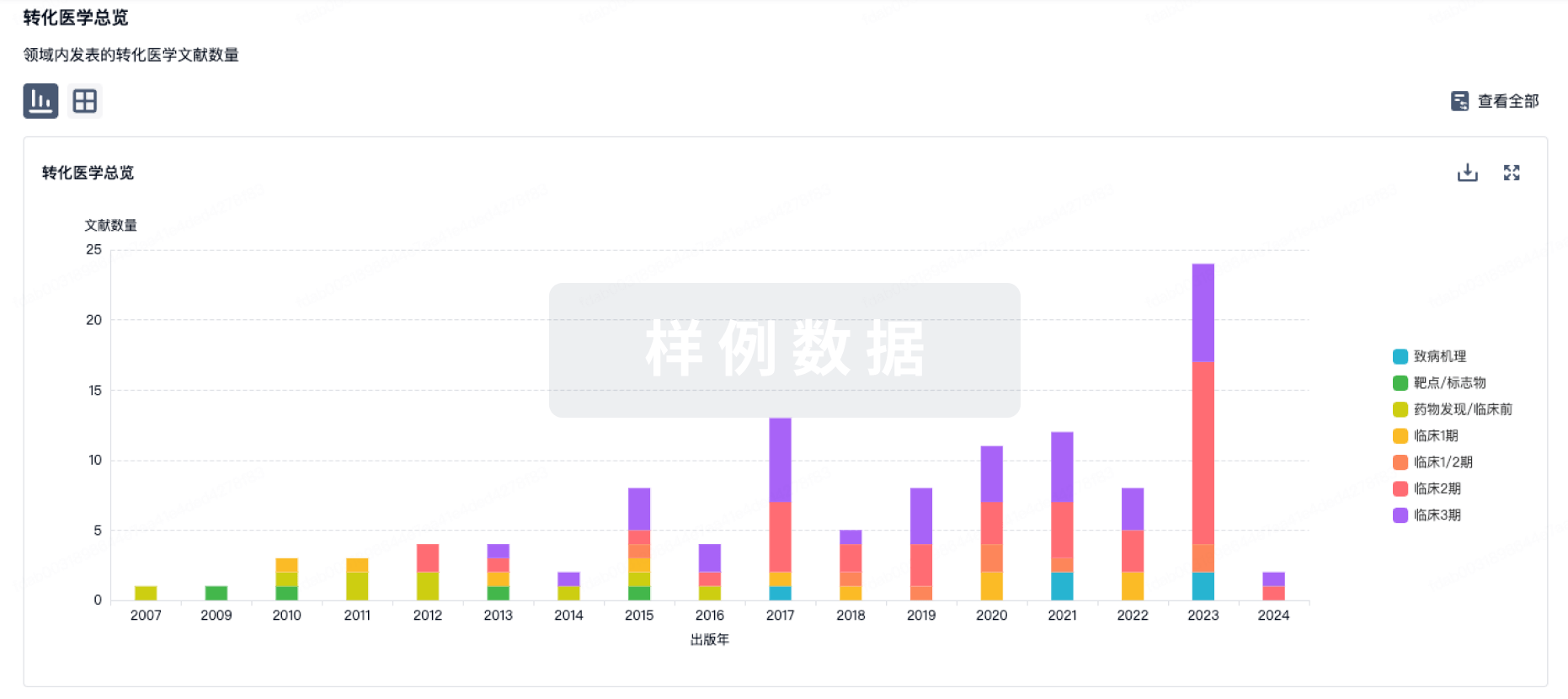
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
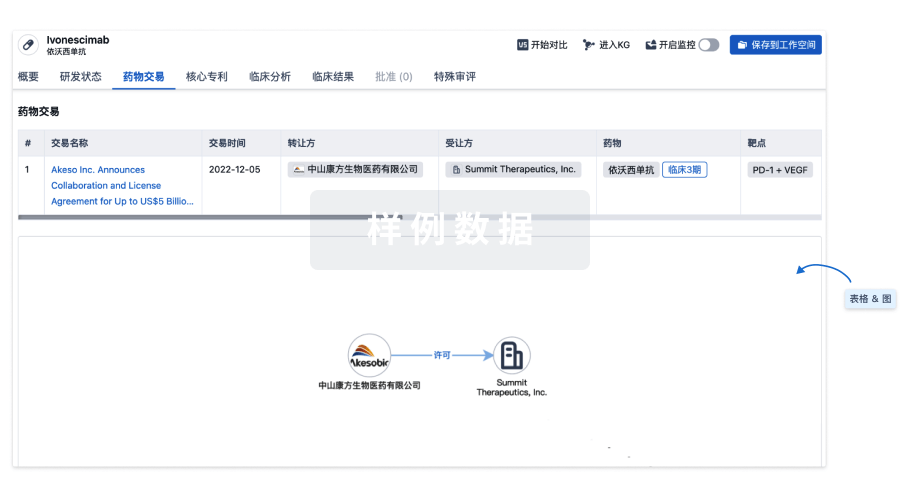
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
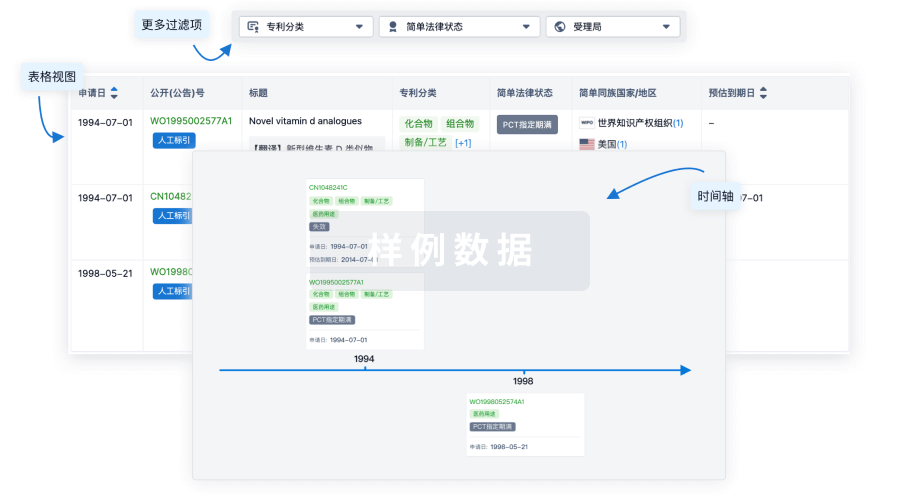
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
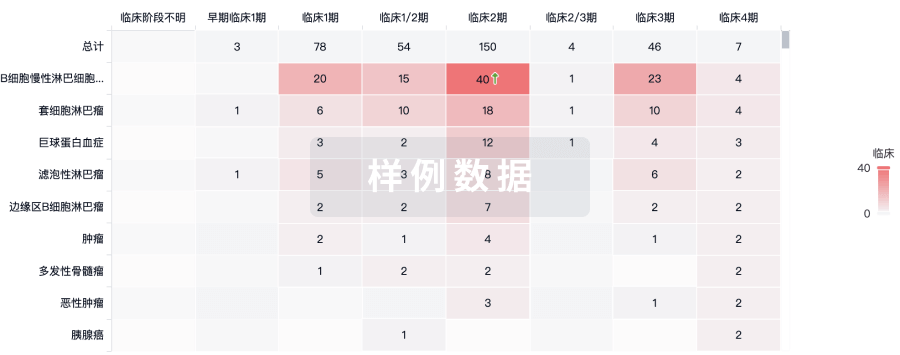
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
批准
利用最新的监管批准信息加速您的研究。
登录
或
生物类似药
生物类似药在不同国家/地区的竞争态势。请注意临床1/2期并入临床2期,临床2/3期并入临床3期
登录
或
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
生物医药百科问答
全新生物医药AI Agent 覆盖科研全链路,让突破性发现快人一步
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用
