更新于:2024-09-19
13-Valent Pneumococcal Polysaccharide Conjugate Vaccine(Zhejiang Vacin Biomedicine)
13价肺炎球菌多糖结合疫苗(艾美卫信生物)
更新于:2024-09-19
概要
基本信息
原研机构 |
在研机构 |
非在研机构- |
最高研发阶段临床3期 |
首次获批日期- |
最高研发阶段(中国)临床3期 |
特殊审评- |
关联
2
项与 13价肺炎球菌多糖结合疫苗(艾美卫信生物) 相关的临床试验13 价肺炎球菌多糖结合疫苗单中心、随机、盲法、同类疫苗对照的非劣效性比较Ⅲ期临床试验
主要目的:(1) 考察2月龄(最小6周龄)人群,按第0、2、4月各接种1剂,并于12~15月龄加强接种1剂,接种试验疫苗后,其疫苗血清型特异性肺炎球菌IgG抗体水平非劣效于相同免疫程序接种的同类对照疫苗;(2)考察3~6月龄人群,按第0、1、2月各接种1剂,于12~15月龄加强接种1剂的程序,接种试验疫苗后,其疫苗血清型特异性肺炎球菌IgG抗体水平非劣效于按第0、2、4月各接种1剂,于12~15月龄加强免疫接种1剂的2月龄(最小6周龄)健康人群;(3)7~11月龄人群,按第0、2月各接种1剂,于12~15月龄加强免疫接种1剂;12~23月龄人群,按第0、2月各接种1剂;24~71月龄健康人群,按第0月接种1剂。考察以上免疫程序接种试验疫苗后,其疫苗血清型特异性肺炎球菌IgG抗体水平非劣效于相同免疫程序接种的同类对照疫苗
次要目的:(1)评价2~71月龄(最小满6周龄)人群按不同免疫程序接种试验疫苗后疫苗血清型特异性肺炎球菌抗体调理吞噬活性(OPA);(2)评价2~71月龄(最小满6周龄)健康人群接种试验疫苗的安全性;(3)评价2~6月龄(最小满6周龄)人群接种试验疫苗的免疫持久性。
开始日期2022-02-16 |
申办/合作机构 |
13 价肺炎球菌多糖结合疫苗单中心、随机、盲法、同类疫苗对照Ⅰ期临床试验
主要研究目的:评价 13 价肺炎球菌多糖结合疫苗接种于 2~3 月龄(最小满 6 周龄)、7月龄~18 岁及以上健康人群的安全性。
次要研究目的:初步考察 13 价肺炎球菌多糖结合疫苗接种于 2~3 月龄(最小满 6 周龄)、7 月龄~18 岁及以上健康人群的免疫原性。
开始日期2021-02-24 |
申办/合作机构 |
100 项与 13价肺炎球菌多糖结合疫苗(艾美卫信生物) 相关的临床结果
登录后查看更多信息
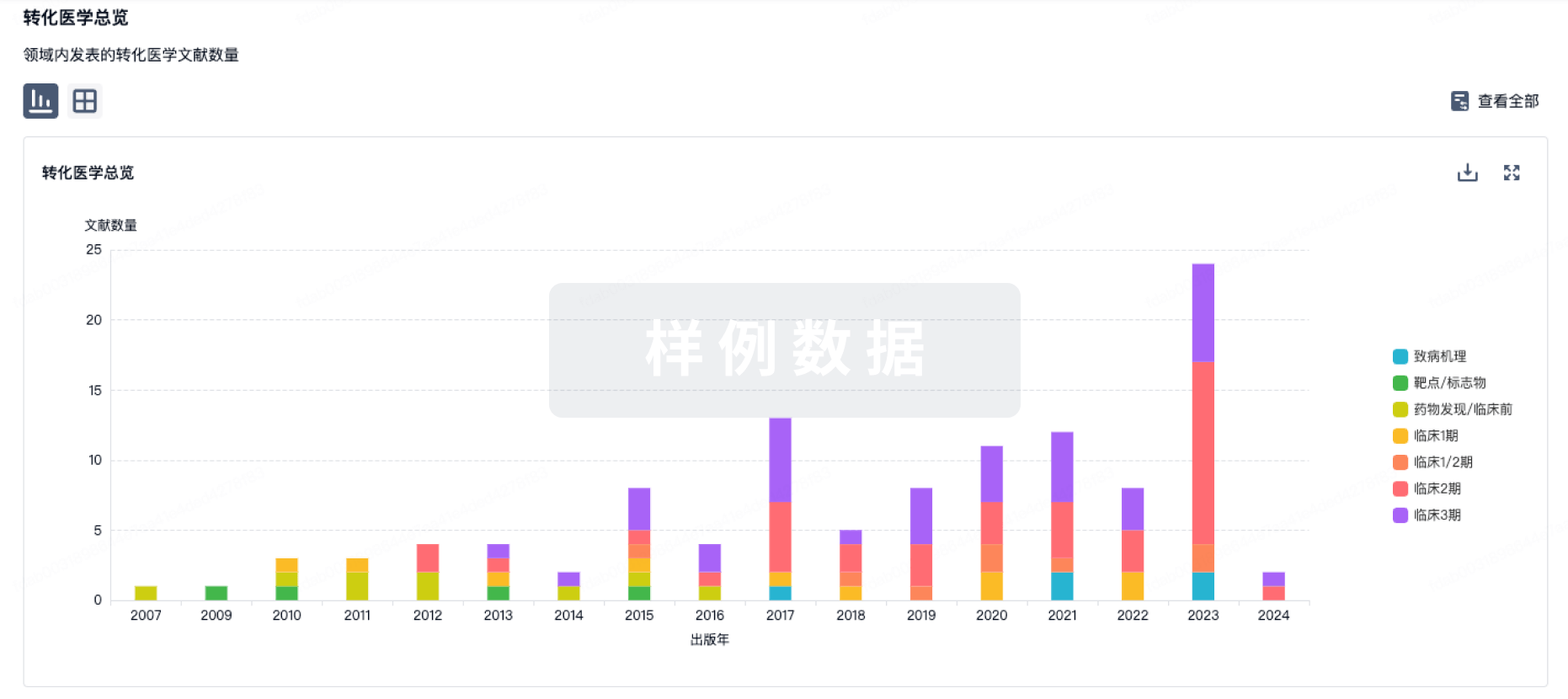
100 项与 13价肺炎球菌多糖结合疫苗(艾美卫信生物) 相关的转化医学
登录后查看更多信息
100 项与 13价肺炎球菌多糖结合疫苗(艾美卫信生物) 相关的专利(医药)
登录后查看更多信息
5
项与 13价肺炎球菌多糖结合疫苗(艾美卫信生物) 相关的文献(医药)2022-01-01·International Journal of Infectious Diseases
Pneumococcal conjugate vaccines in Taiwan: optimizing health gains in children and older adults through constrained optimization modeling
Article
作者: Fu, Tiffany ; Tang, Chao Hsiun ; Ho, Yu-Fan ; Pwu, Raoh-Fang ; Lu, Chun-Yi
2019-05-01·Thorax
Herd protection or herding cats?
作者: Whitney, Cynthia G ; van der Linden, Mark
2015-12-01·BMC Infectious Diseases3区 · 医学
Assessing the impact of pneumococcal conjugate vaccines on invasive pneumococcal disease using polymerase chain reaction-based surveillance: an experience from South Africa
3区 · 医学
ArticleOA
作者: Nzenze, Susan ; Cohen, Adam L ; Treurnicht, Florette ; Moyes, Jocelyn ; Tempia, Stefano ; von Gottberg, Anne ; Venter, Marietjie ; de Gouveia, Linda ; von Mollendorf, Claire ; Wolter, Nicole ; Madhi, Shabir A ; Cohen, Cheryl ; Groome, Michelle J ; Walaza, Sibongile
29
项与 13价肺炎球菌多糖结合疫苗(艾美卫信生物) 相关的新闻(医药)2024-06-17
近日,赛诺菲举办了疫苗投资者活动,主要讨论了疫苗产品管线以及公司的疫苗研发是如何支持其药物开发策略的。下面是12条疫苗管线情况,涉及领域包括流感(3个)、脑膜炎(3个)、RSV(3个)、肺炎(1个)、衣原体(1个)和痤疮(1个)。1、Fluzone HDFluzone HD是美国唯一获得许可的高剂量四价流感疫苗,被批准用于65岁及以上人群,在老年人市场中占据主导地位。目前,Fluzone HD正在进行用于小儿流感的2期试验。2、Flu QIV四价流感疫苗Flu QIV的免疫原性数据显示,A菌株与SoC免疫反应相当,B菌株的免疫应答趋势低于SoC;在反应原性方面,与目前获得许可的流感疫苗相比,该疫苗的反应原性更高,但系统严重副作用显著低于Moderna的mRNA-1010(非头对头)。3、Neuraminidase (NA)mNRA NA抗原疫苗免疫原性与Fluzone HD相当;同时其有良好的耐受性和安全性,亦与Fluzone HD相当。4、MenQuadfiMenQuadfi是赛诺菲的一款创新性脑膜炎球菌疫苗。该疫苗可针对4种血清组在多个年龄段人群中产生高免疫应答,并且耐受性良好。据临床数据显示:在10-17岁青少年中,MenQuadfi有更高或与与辉瑞的ACWY相当的免疫反应;在2-12个月的婴幼儿,3剂MenQuadfi比4剂的GSK的ACWY有更高的免疫反应。据了解,目前还没有其他ACWY注射产品可用,这也是MenQuadfi 的一大优势。赛诺菲预计2023年7月向FDA提交MenQuadfi 的上市申请,并于2024年上市销售。在美国,MenQuadfi已被用于超60%以上的MS(多发性硬化症)。为了巩固市场领导地位,MenQuadfi还在进行国际推广,其目前已经在53个国家注册,且区域范围还在不断扩大中,另外该疫苗在WHO进行资格预审。40份国内人用疫苗申请上市技术审评报告领取方式:关注【药时空】公众号,进入公众号后台,回复关键字“疫苗技术审评资料”,以上资料免费送!PS:后续还会统计汇总CDE上市药品信息中的抗体药物部分,请持续关注本公众号~5、MenB新型MenB配方(SP0230)可提供最佳保护。针对乙型脑膜炎球菌(meningitis B,Men-B)的项目SP0230的1/2期数据显示,赛诺菲配方的耐受性良好、所有抗原都是免疫原性的、防护度也达到了预期水平,可顺利进入下一阶段的研究。值得注意的是,MenB制剂在B菌株间具有很强的交叉保护潜力。6、MenPentaMenPenta也是脑膜炎候选疫苗之一,目前的临床前数据支持MenPenta项目在2023H2时推进到临床1/2阶段研究,并预计2027年在美国提交申请。7、Beyfortus(nirsevimab)Beyfortus是全球首个且唯一可广泛应用于婴儿人群的RSV预防用长效单克隆抗体,由赛诺菲和阿斯利康联合开发,通过结合表达于病毒粒子和受染细胞表面的RSV融合(F)蛋白达到中和RSV的目的,用于预防由RSV引起的下呼吸道疾病。此次赛诺菲公布了Beyfortus的3b期临床试验HARMONIE的数据:该疫苗接种新生儿可以将RSV相关下呼吸道症状住院率降低83%,预计比孕妇接种RSV疫苗有效率高出3倍。2022年11月,Beyfortus获欧盟委员会批准,作为单剂量被动免疫疗法,用于所有新生儿和婴儿,在其第一个RSV季节预防RSV下呼吸道疾病(LRTI)。今年1月,FDA接受Beyfortus的生物制品许可申请(BLA),预计在2023年第3季度公布审查结果;4月,该疫苗在加拿大获批上市;最近该疫苗在国内的上市申请也被CDE纳入了优先审评。8、RSV toddler(SP0125)SP0125为一款减毒活疫苗,也是首个被设计可用于保护所有幼儿的的RSV疫苗。据SP0125的1/2期数据显示,在安全性方面,SP0125与安慰剂类似;在疫苗应答方面,两次使用高剂量配方后,SP0125的疫苗反应强烈(93%),另外,低剂量和高剂量配方之间存在边际差异。赛诺菲预计该疫苗将于2024年上半年进入3期临床。9、RSV older adult (OA,SP0256)SP0256是一款同类第一的RSV-hMPV-PIV三联mRNA疫苗,主要用于老年人。据SP0256的1/2期试验结果显示,RSV OA mRNA疫苗耐受性良好,且显著提高了RSV中和抗体应答。该阳性结果表明SP0256可作为赛诺菲组合呼吸道疫苗的支柱产品。10、PCV21(SP0202)PCV21是由SK bioscience与赛诺菲联合研发的21价肺炎球菌结合候选疫苗,其将特定蛋白与肺炎链球菌的多糖荚膜相结合。该疫苗覆盖21种血清型,高于目前市场上使用的PCV/13/15/20疫苗。此次赛诺菲公布了PCV21疫苗的临床2期试验情况,安全性和免疫原性表现积极:PCV21在儿童人群中耐受性良好,所有4种剂量的安全性均与PCV13相当;与PCV20相比,PCV21的免疫反应良好。另外,PCV21不会干扰共同接种的推荐儿科疫苗(例如破伤风、白喉、百日咳、脊髓灰质炎和B型流感嗜血杆菌疫苗)的免疫原性和安全性。预计该疫苗将于2024年上半年启动临床3期试验,并于2027年提交上市申请。11、Chlamydia(衣原体候选疫苗)创新的多抗原衣原体候选疫苗实现了靶向免疫特性,预计将于2024年进入临床1/2期。12、Acne(青春痘疫苗)痤疮是一种慢性炎症性皮肤病,是全球第8大常见疾病。用于痤疮的治疗性mRNA候选疫苗临床前结果良好,预计该疫苗将于2023年下半年进入临床1/2期。总结:赛诺菲通过BIC/FIC疫苗管道推动创新,自2021年12月疫苗投资者事件以来,赛诺菲有3个新产品获批;领先的mRNA平台提高了其流感护理标准;预计2022/2023年将有6条新的候选疫苗管线进行1/2期试验;预计到2025年,赛诺菲在不同的预防和治疗领域至少启动5个创新疫苗项目的3期试验。另外,在销售额方面,赛诺菲预计到2030年疫苗年销售额将超过100亿欧元。注:文中图片均来自于赛诺菲的Vaccines Investor Event,June 29, 2023。
疫苗临床3期临床2期信使RNA申请上市
2024-01-06
肺炎链球菌是一种常见于上呼吸道的定植菌,是造成致死性感染的常见病原体之一,也是造成细菌性肺炎和脑膜炎的最常见病原菌。而多糖荚膜是造成侵袭性肺炎球菌疾病的主要毒力因素,根据多糖组分的不同,肺炎球菌可分为约90种不同的血清型。通过对不同血清型的肺炎球菌多糖荚膜进行纯化,可制成含有不同抗原组分的多价肺炎球菌多糖疫苗。PS:扫码下方二维码加小编微信,备注“2023肺炎疫苗批签发”,即可获取完整的161批次肺炎球菌疫苗批签发详情表格文件。相关阅读:2023年我国HPV疫苗批签发情况汇总:共574批次,同比增长29%目前,我国上市的肺炎球菌疫苗包13价肺炎球菌多糖结合疫苗(PCV13)和23价肺炎球菌多糖疫苗(PPSV23)。13价肺炎疫苗覆盖了88.7%的肺炎球菌血清型,23价的覆盖率则为90.2%。从适用人群看,PCV13主要用于5岁以下儿童,PPSV23主要用于2岁以上,特别是老年人和免疫功能低下等对肺炎球菌性疾病易感的人群。据中检院披露的生物制品批签发情况显示,2023年国内肺炎疫苗批签发161批次,同比增长5.23%(2022为153批次)。从获批企业来看,涉及6家企业,包括沃森生物批签发86批次、民海生物批签发30批次、成都所批签发18批次、辉瑞批签发13批次、默沙东批签发7批次、科兴生物批签发7批次。与其他家相比,沃森生物的肺炎疫苗批签发批次量约占今年该类疫苗批次总量的一半。(文末附详细的肺炎疫苗批签发信息表)图1:2023年国内肺炎球菌疫苗各企业批签发批次份额,2023年批签发数据统计时间段为2023.01.02-2023.12.31(来源:中检院,药时空制图)其中,PCV13批签发97批次,同比减少10.19%;PPV23批签发64批次,同比增长42.22%。这可能是由于PPV23适用的接种人群范围更大,且国家政策在推进免疫力下降的老年人中接种,所以PPV23的市场空间增长。从研发格局来看,除了以上提及的企业布局了肺炎球菌疫苗外,国内还有兰州所、康希诺、艾美疫苗、安特金、智飞绿竹等企业有相关的在研产品。其中,2023年3月,兰州生物递交了13价肺炎球菌多糖结合疫苗的上市申请,但审批未通过。据西南证券预计,这与数据关系较大,其预计国内未来疫苗行业临床试验要求更加讲究同类优效产品。10月,艾美疫苗宣布,其自主研发的13价肺炎球菌结合疫苗(PCV13)III期临床试验已完成基础免疫MOPA血清检测,即将进入统计揭盲工作。公司在2023年投资者开放日活动中表示,其13价肺炎结合疫苗、23价肺炎多糖疫苗预计于2024年申请注册上市。另外,公司还还率先开发了迭代升级换代产品20价肺炎结合疫苗和24价肺炎结合疫苗,目前20价肺炎结合疫苗已处于CDE预沟通阶段。康希诺则在近期投资者关系记录表中表示,公司13价肺炎结合疫苗正在按计划进行新药申报注册前的必要准备工作,预计在2024年正式申报注册。PS:扫码下方二维码加小编微信,备注“2023肺炎疫苗批签发”,即可获取完整的161批次肺炎球菌疫苗批签发详情表格文件。附:2023年我国肺炎球菌疫苗批签发情况部分截图(来源:中检院,药时空整理)参考资料:[1]2017—2021年中国13价肺炎球菌多糖结合疫苗接种覆盖水平分析.中华预防医学杂志.2023-12-04.[2]市场夹击战下,辉瑞中国裁撤明星肺炎疫苗产品团队.华夏时报.2023-12-09.[3]医药行业2024年投资策略:医药结构性行情,聚焦三大方向.西南证券.20231211.[4]中国食品药品检定研究院.生物制品批签发产品公示情况汇总.[5]艾美疫苗、康希诺等公司公告.识别微信二维码,添加生物制品圈小编,符合条件者即可加入生物制品微信群!请注明:姓名+研究方向!版权声明本公众号所有转载文章系出于传递更多信息之目的,且明确注明来源和作者,不希望被转载的媒体或个人可与我们联系(cbplib@163.com),我们将立即进行删除处理。所有文章仅代表作者观点,不代表本站立场。
疫苗上市批准临床3期
2023-08-31
·药创客
点击上方图片报名参会 艾美疫苗宣布,旗下23价肺炎球菌多糖疫苗启动III期随机、盲法、同类疫苗对照设计临床试验。该临床试验计划入组1920例2岁及以上健康受试者。 艾美疫苗旗下23价肺炎球菌多糖疫苗适用于2岁以上人群(特别是60岁以上老年人群)侵袭性肺炎球菌疾病的预防。该疫苗中含有23种肺炎球菌血清型多糖抗原,可以预防肺炎球菌感染引起的肺炎、脑膜炎、中耳炎及菌血症等,覆盖了最常报道的引起肺炎球菌疾病的近90%的血清型。该款疫苗已于2021年12月开展I期临床试验,截至目前已获得的安全性和免疫原性分析结果显示其安全性良好,且具有较好的免疫原性。而艾美的13价肺炎球菌多糖结合疫苗(PCV13)是全球使用最为广泛的肺炎球菌多糖结合疫苗、也是唯一一款用于全年龄组人群注射的肺炎疫苗,有着全球“疫苗销售之王”的称号。2020年辉瑞PCV13全球销售额高达58.5亿美元,预计国内PCV13市场规模有望达到108亿元。作为公司的重磅大品种之一,艾美疫苗的PCV13疫苗三期临床即将结束、制造技术已经验证,预计于2024年年底获批。受益于公司全产业链、大平台的优势,产品一经获批上市后即可实现大规模产能放量,快速抢占市场份额:据悉,目前艾美疫苗全资子公司艾美卫信已完成肺炎球菌疫苗生产线的重建和升级,设计年产能达4700万剂。 由于流行性脑脊髓膜炎(流脑)具有起病急、进展快、传染性强、病死率与致残率高等特点,且流脑菌群一直在发生变化,相比过往疫苗,四价流脑结合疫苗(MCV4)具有预防A群、C群、Y群和W135群四种血清型的多价优势。而在国内市场,脑膜炎球菌疫苗长期被纳入国家免疫规划,而MCV4市场长期由进口厂商主导,潜在国产替代化机会明显。 目前艾美疫苗的四价流脑结合疫苗(MCV4)已启动I期单中心、开放性临床试验,受试者已经开始入组,本试验计划入组120例。市场需求缺口叠加MCV4单支价格高、利润空间大的特点,上市后预计将为公司贡献充沛的现金流。 手足口病是由肠道病毒引起的自限性疾病,属于儿童常见传染病,2009-2019年我国手足口病报告发病总体呈波动上升趋势。目前市面上获批的单价手足口病疫苗存在仅能针对EV71这一种病毒株的劣势,因此更为创新的的EV71-CA16二价手足口病疫苗已成为技术发展的必然趋势。 目前,艾美疫苗全球首研的EV71-CA16二价手足口病疫苗已进入临床阶段。这也是我国首个获得临床批件的二价手足口病疫苗,上市后有望填补国内市场空白。 预计2023年下半年和2024-2025年间,艾美疫苗将有至少四款产品发布上市,商业化产品数量提升至两位数;同时,市场所关注的二价手足口病疫苗、冻干人用狂犬疫苗(人二倍体细胞)、四价结合流脑疫苗、破伤风疫苗等产品均预计在5年内上市。产品进入密集收获期,无疑将为公司业绩增添强劲的成长动能。作为国内起步较早、深耕疫苗赛道多年的公司,艾美疫苗有着病毒疫苗平台、细菌疫苗平台、mRNA疫苗平台、基因工程疫苗平台、联合疫苗平台这五大技术平台强力支撑研发,目前已经完成针对14种疾病领域23款在研疫苗的布局,且目前已有9个品种取得共计14个临床批件。作为国内首款针对奥密克戎株BA.5的二价广谱mRNA疫苗,已有的试验数据表明其不仅具有良好的防感染效果,期中分析最高保护率达到80.68%,远高于新冠疫苗保护效力的国际标准;还具有广谱作用,对XBB变异株反而表现出更高的保护效力。随着国内“二阳”、甚至“三阳”“四阳”的病例人数逐渐增多,预计该款mRNA新冠疫苗上市后亦将贡献显著业绩增量。根据艾美疫苗发布的2023年中期业绩公告,在研二价Delta-Omicron BA.5 mRNA新冠疫苗海外III期临床正处于收尾阶段。未来公司将使用该款疫苗在国内的I、II期临床数据,结合在巴基斯坦的III期临床数据,申请该款疫苗在国内注册上市。此外,公司研发的人用狂犬病mRNA疫苗是国内首款申报临床获得受理的非新冠mRNA疫苗,目前临床试验申请已获受理。从收入结构来看,乙肝疫苗与人用狂犬病疫苗是公司主要的收入来源,在市场一直占据领先地位,保障了公司现金流。深入探究公司业务就会发现,即使不考虑未来新产品上市,在现有的狂犬疫苗与乙肝疫苗上公司亦早有布局。展望后续研发路线,公司在狂犬疫苗上亦有着完善的迭代升级规划,包括已获临床批件的无血清Vero细胞狂犬病疫苗、人二倍体细胞狂犬病疫苗以及mRNA狂犬病疫苗。其中,公司所研发的人用狂犬病mRNA疫苗是国内首款申报临床的狂犬病mRNA疫苗,目前临床试验申请已获受理。在乙肝疫苗方面,艾美是中国第一家也是唯一一家实现使用汉逊酵母进行抗原表达的乙型肝炎疫苗稳定生产和批签发量的疫苗公司。在所有可用的三种制造技术(汉逊酵母、酿酒酵母及CHO细胞)中,汉逊酵母被公认为是乙型肝炎疫苗的最佳制造技术路线,具有更好的遗传稳定性、更高的纯度及更强的抗原表达能力。识别微信二维码,添加小编,符合条件者即可申请加入微信群!请注明:姓名+单位!声明:本文旨在传递更多信息,版权归原作者所有。原创文章转载均需经过授权并注明来源,如涉及内容、版权或其他问题请时联系小编删除!文章仅代表作者个人观点,并不代表公众号立场。本公众号拥有对此声明的最终解释权!投稿邮箱:yck19876@163.com
临床3期疫苗临床1期
100 项与 13价肺炎球菌多糖结合疫苗(艾美卫信生物) 相关的药物交易
登录后查看更多信息
研发状态
10 条进展最快的记录, 后查看更多信息
登录
| 适应症 | 最高研发状态 | 国家/地区 | 公司 | 日期 |
|---|---|---|---|---|
| 肺炎球菌感染 | 临床3期 | 中国 | - |
登录后查看更多信息
临床结果
临床结果
适应症
分期
评价
查看全部结果
| 研究 | 分期 | 人群特征 | 评价人数 | 分组 | 结果 | 评价 | 发布日期 |
|---|
No Data | |||||||
登录后查看更多信息
转化医学
使用我们的转化医学数据加速您的研究。
登录
或
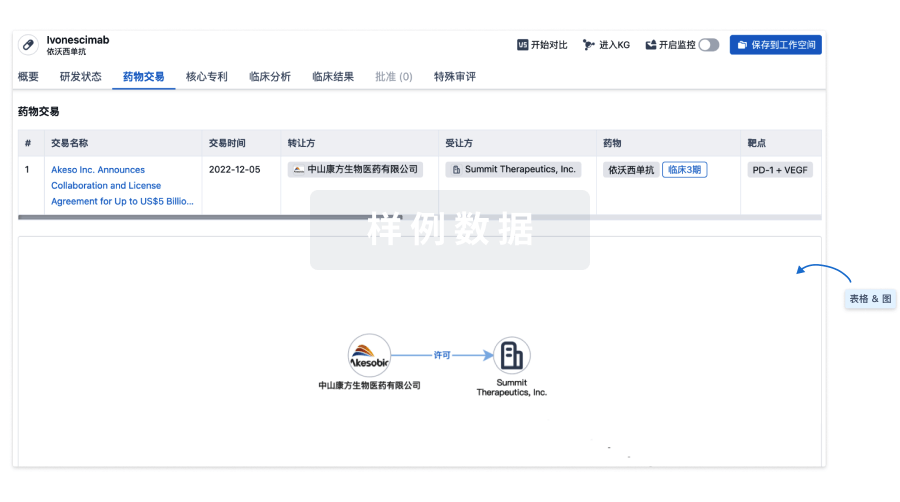
药物交易
使用我们的药物交易数据加速您的研究。
登录
或
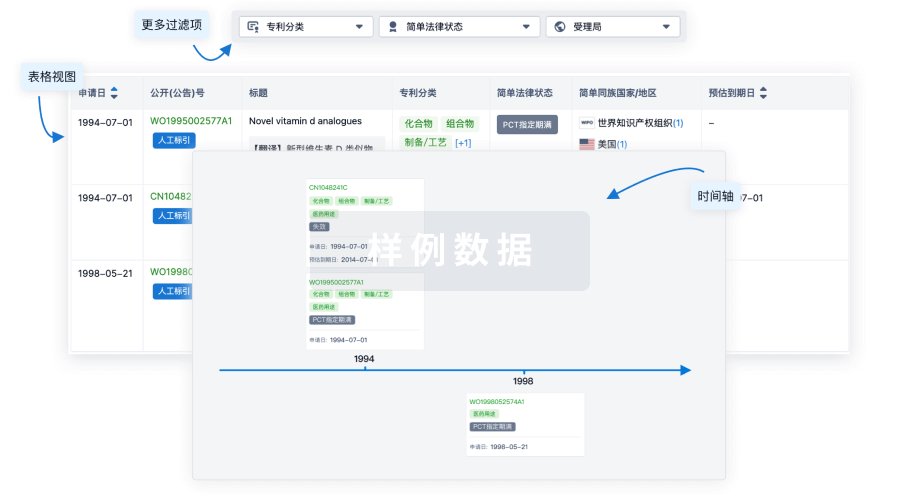
核心专利
使用我们的核心专利数据促进您的研究。
登录
或
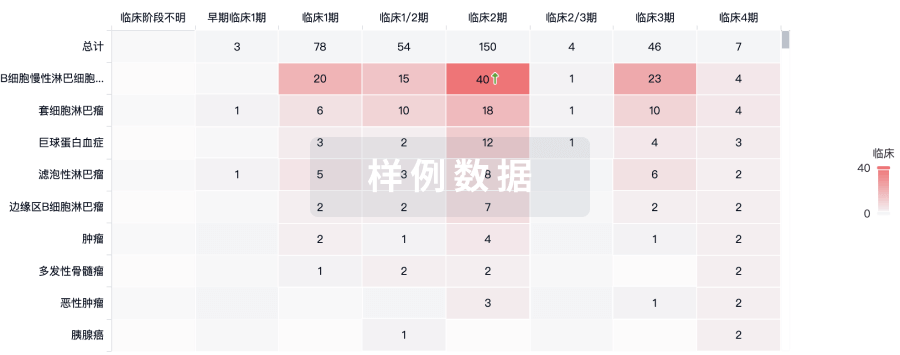
临床分析
紧跟全球注册中心的最新临床试验。
登录
或
批准
利用最新的监管批准信息加速您的研究。
登录
或
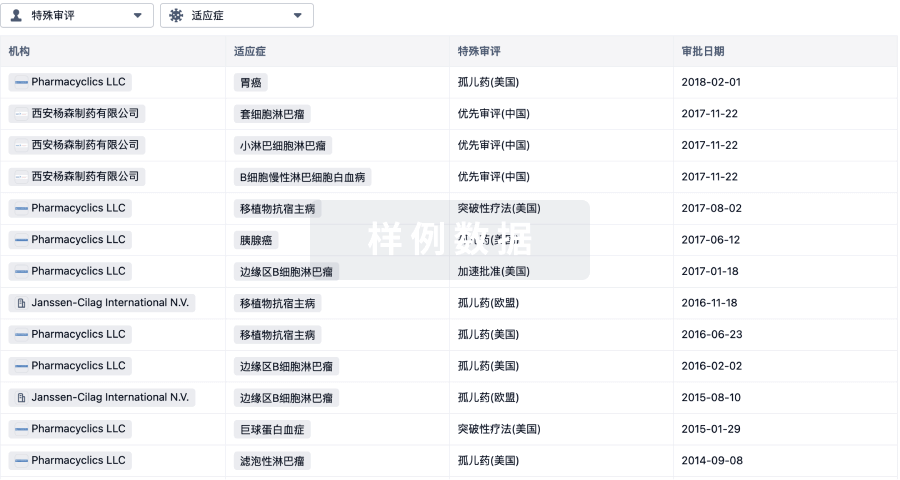
特殊审评
只需点击几下即可了解关键药物信息。
登录
或
标准版
¥16800
元/账号/年
新药情报库 | 省钱又好用!
立即使用
来和芽仔聊天吧
立即开始免费试用!
智慧芽新药情报库是智慧芽专为生命科学人士构建的基于AI的创新药情报平台,助您全方位提升您的研发与决策效率。
立即开始数据试用!
智慧芽新药库数据也通过智慧芽数据服务平台,以API或者数据包形式对外开放,助您更加充分利用智慧芽新药情报信息。
生物序列数据库
生物药研发创新
免费使用
化学结构数据库
小分子化药研发创新
免费使用

